Abstract
Objectives:
Low cholesterol has been linked with violent and suicidal behaviour in people with schizophrenia. This association, if consistently present, may be a promising biological marker that could assist clinicians in decision making regarding risk and treatment. We conducted a systematic review to assess whether there is a reliable association between lipid profile (total cholesterol, high- and low-density lipoprotein cholesterol, and triglycerides) and aggression, self-harm or suicide in people with schizophrenia, and whether effects are similar in males and females.
Method:
Relevant databases were searched to identify primary research studies (up to November 2020) that (1) involved adults (some samples also included 16- to 18-year olds) with a confirmed diagnosis of schizophrenia, schizoaffective disorder or psychosis; and (2) included a standardised assessment of verbal aggression, physical aggression against objects, physical aggression against self (including suicide) or others. The search yielded 23 studies eligible for inclusion following a quality appraisal.
Results:
Suicidality was the most commonly assessed subtype of aggression (20 studies). For suicidality, about half the studies, including the study with the largest sample size, found a link with total cholesterol. An association between low total cholesterol and violence towards others was found in six of nine studies that investigated this. The evidence for a link with violence was the strongest for total cholesterol, followed by low-density lipoprotein cholesterol and high-density lipoprotein cholesterol, and the weakest for triglycerides. Only a few studies investigated sex differences and yielded mixed evidence. Studies focussed on self-harm as well as involving females in forensic settings were lacking.
Conclusion:
There is encouraging evidence of an association between low total cholesterol and aggression towards others as well as suicidality in schizophrenia. Future studies should systematically explore this association in people with schizophrenia who have a significant history of violence, suicidality and self-harm, both inpatients and community, and also investigate underlying mechanisms.
Introduction
The majority of patients in forensic psychiatric services have schizophrenia (Fleischman et al., 2014; Silverstein et al., 2015) or personality disorder (PD), often presenting co-morbidly (Arseneault et al., 2000). There is considerable evidence of an association between interpersonal violence and schizophrenia (Fleischman et al., 2014; Silverstein et al., 2015; Walsh et al., 2002). Violent crime has been shown to be up to 10 times more common in people with schizophrenia than matched populations (Fazel et al., 2009). A growing body of evidence (review, Sedgwick et al., 2016) suggests that several neurobiological measures are aberrant in forensic psychiatric populations. Some of these aberrations, if reliably associated with risk or outcomes, could assist clinicians to make decisions about treatment planning, risk and discharge (Sedgwick et al., 2016). One such promising biological marker could be the lipid profile, particularly serum cholesterol.
A link between low levels of cholesterol and violent behaviour in forensic psychiatric populations has been suggested for over 25 years (Boston et al., 1996; Douglas and Nasrallah, 2019; Sedgwick et al., 2016). Low cholesterol may also be linked to suicidality (Asellus et al., 2010; Lee and Kim, 2003; Wu et al., 2016). Low cholesterol has been discussed as a biomarker for suicide since the early 1990s when meta-analytic evidence associated the use of statins (cholesterol-lowering drugs) with an elevated risk of death by suicide, despite these drugs lowering the risk of death by coronary events (Muldoon et al., 1990). A significant relationship between low serum cholesterol levels and suicide in psychiatric disorders, including psychosis, has also been reported (Kułak-Bejda et al., 2021). Furthermore, low cholesterol has been linked to inpatient suicidal and violent behaviour, and with 3-month post-discharge violent behaviour in non-forensic patient populations (Roaldset et al., 2011), as well as with criminal violence in the general population (Golomb et al., 2000). However, some studies indicate that low cholesterol-aggression association may be true only for men (Tomson-Johanson and Harro, 2018), and a few studies failed to observe this association (Deisenhammer et al., 2004; Roy et al., 2001). To what extent this association is influenced by sex or reliably present in people with schizophrenia remains unclear.
The main aim of this review, therefore, was to systematically investigate possible associations between lipid profile, as indexed by the levels of total cholesterol (TC), high-density lipoprotein cholesterol (HDL), low-density lipoprotein cholesterol (LDL) and triglycerides (TG), and specific dimensions of aggression and violence in adult patients with schizophrenia. For the purpose of this review, aggression was defined as any behaviour falling under verbal aggression, physical aggression against objects, physical aggression against self (including suicide) or physical aggression against others, in line with the Modified Overt Modified Overt Aggression Scale (MOAS) (Sorgi et al., 1991). Our secondary aim was to consider potential sex differences in these associations wherever possible.
Methods
Information sources and search
We followed the guidelines detailed in the Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA) (Moher et al., 2009) for literature search. An extensive search of PubMed, PsycINFO, Academic Search Complete, CINAHL Plus, MEDLINE, Scopus and Web of Science databases was carried out in the first week of December 2020. A combination of the following search terms was used: (cholester* OR high density lipoprotein OR HDL OR low density lipoprotein OR LDL OR triglycerides OR lipid profile) AND (schizoph* OR psychosis OR psychotic OR schizoaffective*) AND (violen* OR aggress* OR assault OR suicide* OR self-harm* OR self-mutilation). Other studies were located through hand searching of relevant publications and reference lists.
Screening and selection
Articles were selected using the following pre-formed inclusion and exclusion criteria: (1) patients must have a diagnosis of schizophrenia, schizoaffective disorder or psychosis stated through either a DSM (Diagnostic and Statistical Manual of Mental Disorders) or ICD (International Classification of Diseases) classification; (2) participants must be adults, aged 18 years and over, unless unavoidable (i.e. studies where the vast majority of participants were over 18, but included some participants between 16 and 18 years, were included); (3) aggressive behaviour described must fall under at least one type stated in the MOAS – verbal, physical against objects, physical against self, physical against others; (4) level of cholesterol must be specified with units; (5) access to full published text and methodology must be available (excluding review articles, editorials and data from conference publications); and (6) articles must be available in English. Two blinded reviewers (P.S. and D.A.) independently made the study selection according to these criteria. Both reviewers had to agree with the articles selected.
Quality appraisal and data extraction
The quality of the selected studies was then assessed using The Joanna Briggs Institute (JBI) Critical Appraisal Tools for cross-sectional, case–control and case series studies (Zeng et al., 2015). One point was granted for meeting each of the criteria. Articles scoring less than 80% were excluded. Each criterion was graded as ‘yes’, ‘no’, ‘unclear’ or ‘not applicable’. One point was granted for scoring ‘yes’ on each of the criteria, and then all points added to derive the total score, expressed in percentage, for each study. Studies assessed ranged in score from 71.4% to 100% (Tables 1–3). Articles scoring less than 80% were excluded. The mean score of papers included in the review following quality appraisal was 94.2%.
The Joanna Briggs Institute (JBI) quality appraisal ratings for included and excluded studies: case–control studies.
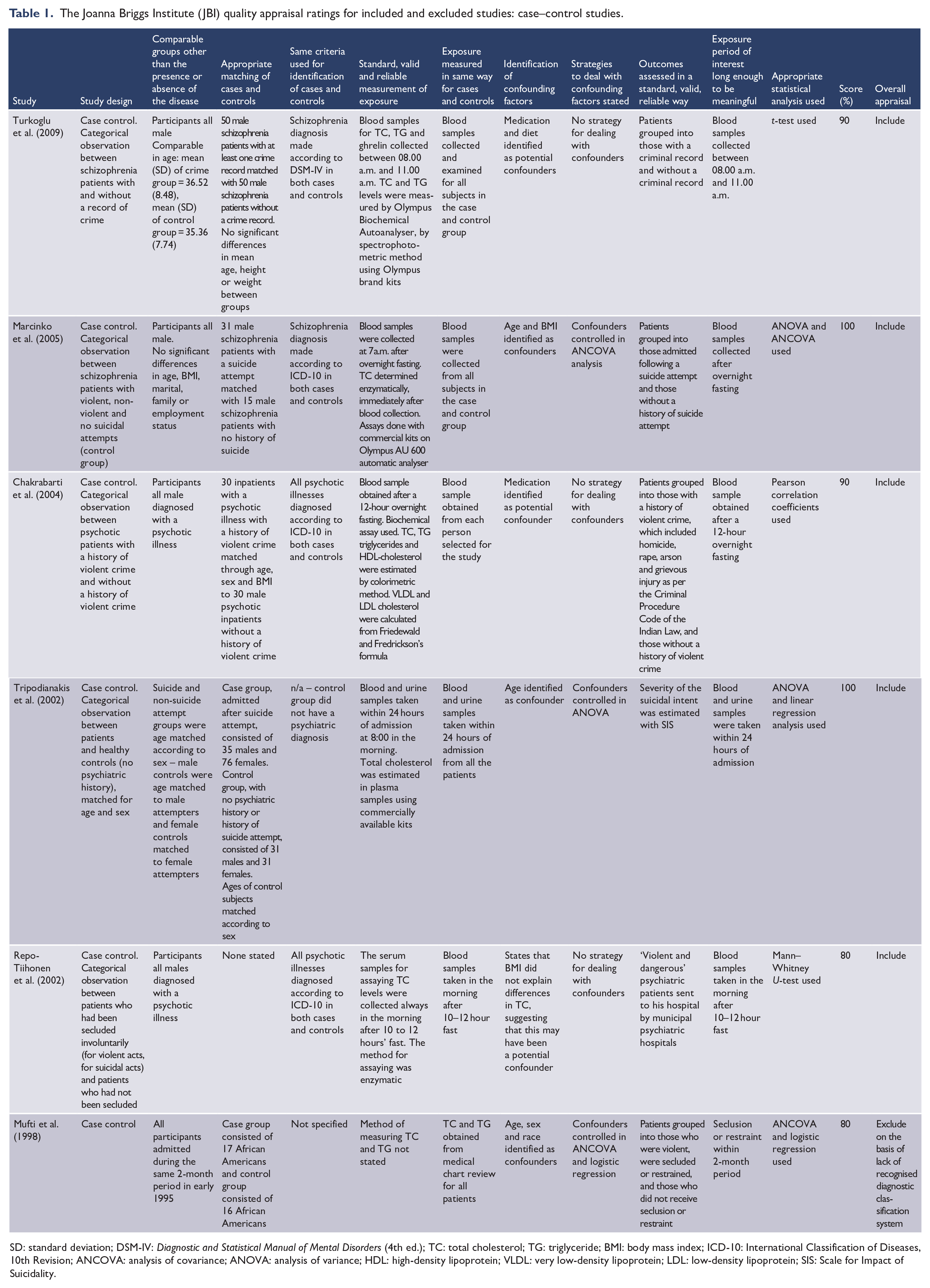
SD: standard deviation; DSM-IV: Diagnostic and Statistical Manual of Mental Disorders (4th ed.); TC: total cholesterol; TG: triglyceride; BMI: body mass index; ICD-10: International Classification of Diseases, 10th Revision; ANCOVA: analysis of covariance; ANOVA: analysis of variance; HDL: high-density lipoprotein; VLDL: very low-density lipoprotein; LDL: low-density lipoprotein; SIS: Scale for Impact of Suicidality.
The Joanna Briggs Institute (JBI) quality appraisal ratings for included and excluded studies: Case series studies.
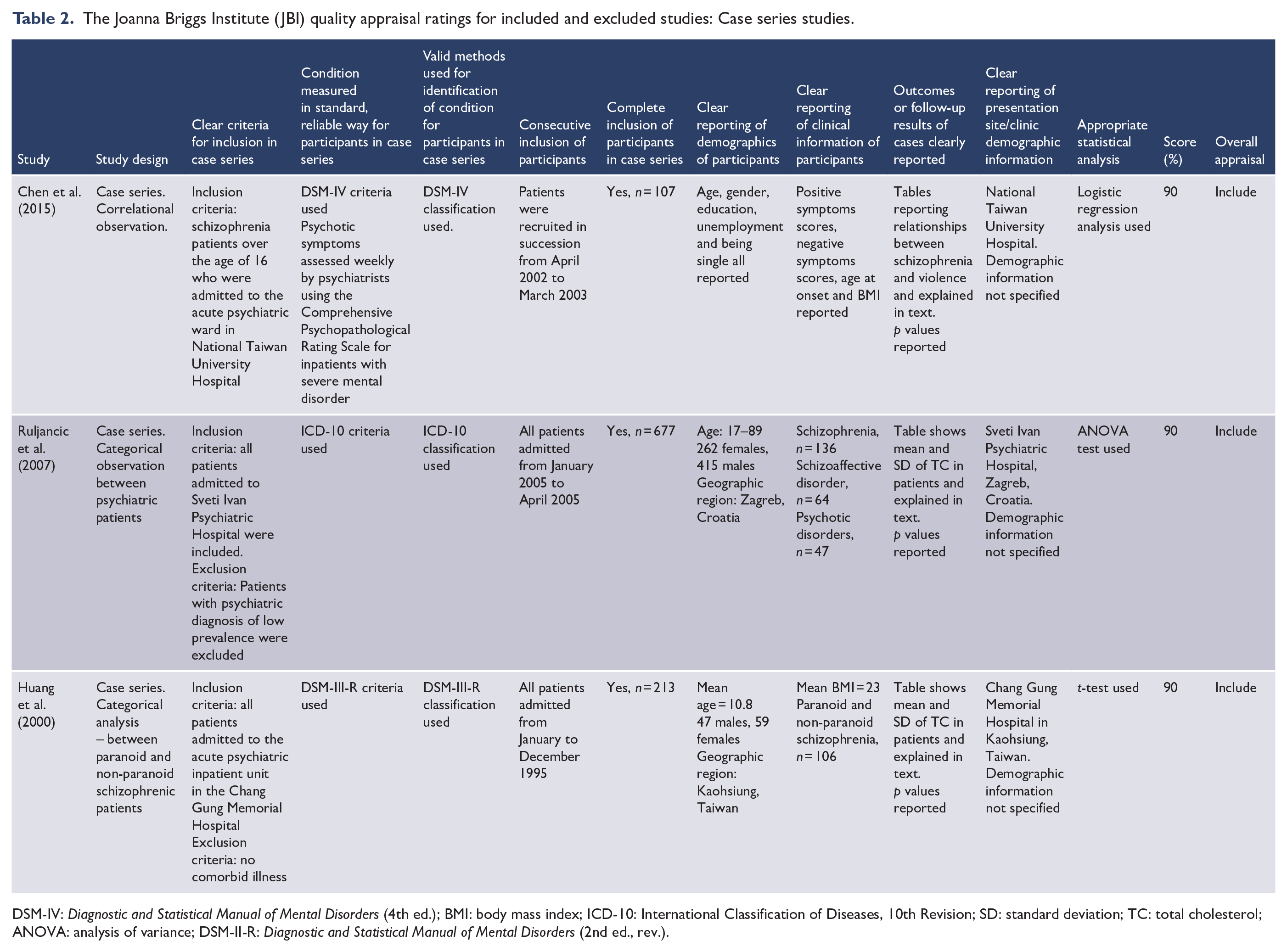
DSM-IV: Diagnostic and Statistical Manual of Mental Disorders (4th ed.); BMI: body mass index; ICD-10: International Classification of Diseases, 10th Revision; SD: standard deviation; TC: total cholesterol; ANOVA: analysis of variance; DSM-II-R: Diagnostic and Statistical Manual of Mental Disorders (2nd ed., rev.).
The Joanna Briggs Institute (JBI) quality appraisal ratings for included and excluded studies: cross-sectional studies.
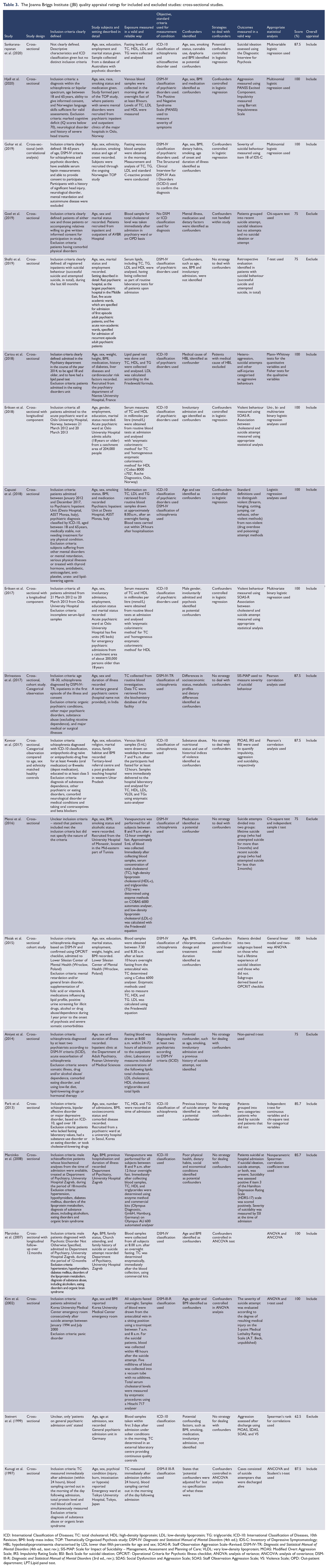
ICD: International Classification of Diseases; TC: total cholesterol; HDL: high-density lipoprotein; LDL: low-density lipoprotein; TG: triglyceride; ICD-10: International Classification of Diseases, 10th Revision; BMI: body mass index; TOP: Thematically Organised Psychosis study; DSM-IV: Diagnostic and Statistical Manual of Mental Disorders (4th ed.); IDS-C: Inventory of Depressive Symptomatology; HBL: hypobetalipoproteinaemia characterised by LDL lower than fifth percentile for age and sex; SOAS-R: Staff Observation Aggression Scale–Revised; DSM-IV-TR: Diagnostic and Statistical Manual of Mental Disorders (4th ed., text rev.); SIS-MAP: Scale for Impact of Suicidality – Management, Assessment and Planning of Care; VLDL: very low-density lipoprotein; MOAS: Modified Overt Aggression Scale; IRS: Impulsivity Rating Scale; BSI: Beck Scale for suicidal ideation; OPCRIT: Operational Criteria for Psychotic Illness checklist; ANOVA: analysis of variance; ANCOVA: analysis of covariance; DSM-III-R: Diagnostic and Statistical Manual of Mental Disorders (3rd ed., rev.); SDAS: Social Dysfunction and Aggression Scale; SOAS: Staff Observation Aggression Scale; VS: Violence Scale; OPD: Out-patient department; LPT:Lipid panel test.
Case–control studies were scored out of 10, based on the following criteria: were the groups comparable, other than the presence of disease in cases or the absence of disease in controls; were cases and controls matched appropriately; were the same criteria used for identification of cases and controls; was exposure measured in a standard, valid and reliable way; was exposure measured in the same way for cases and controls; whether confounding factors were identified; whether strategies to deal with confounding factors were stated; whether outcomes were assessed in a standard, valid and reliable way for cases and controls; was the exposure period of interest long enough to be meaningful; and whether appropriate statistical analyses were used.
Similarly, case series studies were scored out of 10. A point was given if: there were clear criteria for inclusion in the case series; the condition was measured in a standard, reliable way for all participants included; valid methods were used for identification of the condition for all participants included; the case series had consecutive inclusion of participants; the case series had complete inclusion of participants; there was clear reporting of the demographics of the participants in the study; there was clear reporting of clinical information of the participants; the outcomes or follow-up results of cases were clearly reported; there was clear reporting of the presenting site/clinic demographic information; and statistical analysis chosen was appropriate.
Finally, cross-sectional studies were scored out of 8, based on criteria assessing whether: the inclusion criteria were clearly defined; the study subjects and setting were described in detail; the exposure was measured in a valid and reliable way; objective, standard criteria was used for measurement of the condition; confounding factors were identified; strategies to deal with confounding factors were stated; the outcomes were measured in a valid and reliable way and appropriate statistical analysis was chosen. Studies excluded at this stage consistently lacked the identification of confounding factors and strategies to handle them appropriately. A list of articles with reasons for exclusion following quality appraisal is provided in Tables 1–3.
A data extraction table was created with the final selection of articles (Table 4), compiling data on: the first author’s name, year of publication, location of the study, study design, psychiatric conditions included in the study, the diagnostic classification used, sample size (and sex distribution), the number of schizophrenia, schizoaffective and psychotic patients included (and sex distribution), details of the case and control groups, form of cholesterol examined (TC, LDL, HDL, TG), findings classified by each aggression type (physical against self, physical against others, physical against objects, verbal) and any other findings (see Table 4).
Details of the included studies and key findings.
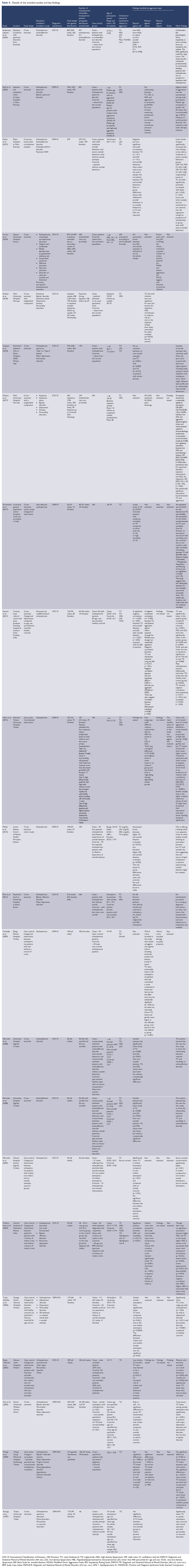
ICD-10: International Classification of Diseases, 10th Revision; TC: total cholesterol; TG: triglyceride; HDL: high-density lipoprotein; OR: odds ratio; CI: confidence interval; DSM-IV: Diagnostic and Statistical Manual of Mental Disorders (4th ed.); LDL: low-density lipoprotein; HBL: Hypobetalipoproteinaemia characterised by LDL lower than fifth percentile for age and sex; VLDL: very low-density lipoprotein; BSI: Beck Scale for suicidal ideation; MOAS: Modified Overt Aggression Scale; IRS: Impulsivity Rating Scale; DSM-IV-TR: Diagnostic and Statistical Manual of Mental Disorders (4th ed., text rev.); BMI: body mass index; DSM-III-R: Diagnostic and Statistical Manual of Mental Disorders (3rd ed., rev.); APA 1: Apolipoprotein A1; PANSS-EC: Positive and Negative Syndrome Scale–Excited Component.
Results
Our literature search produced 29 articles for quality appraisal, of which 23 were deemed eligible for inclusion (Figure 1).
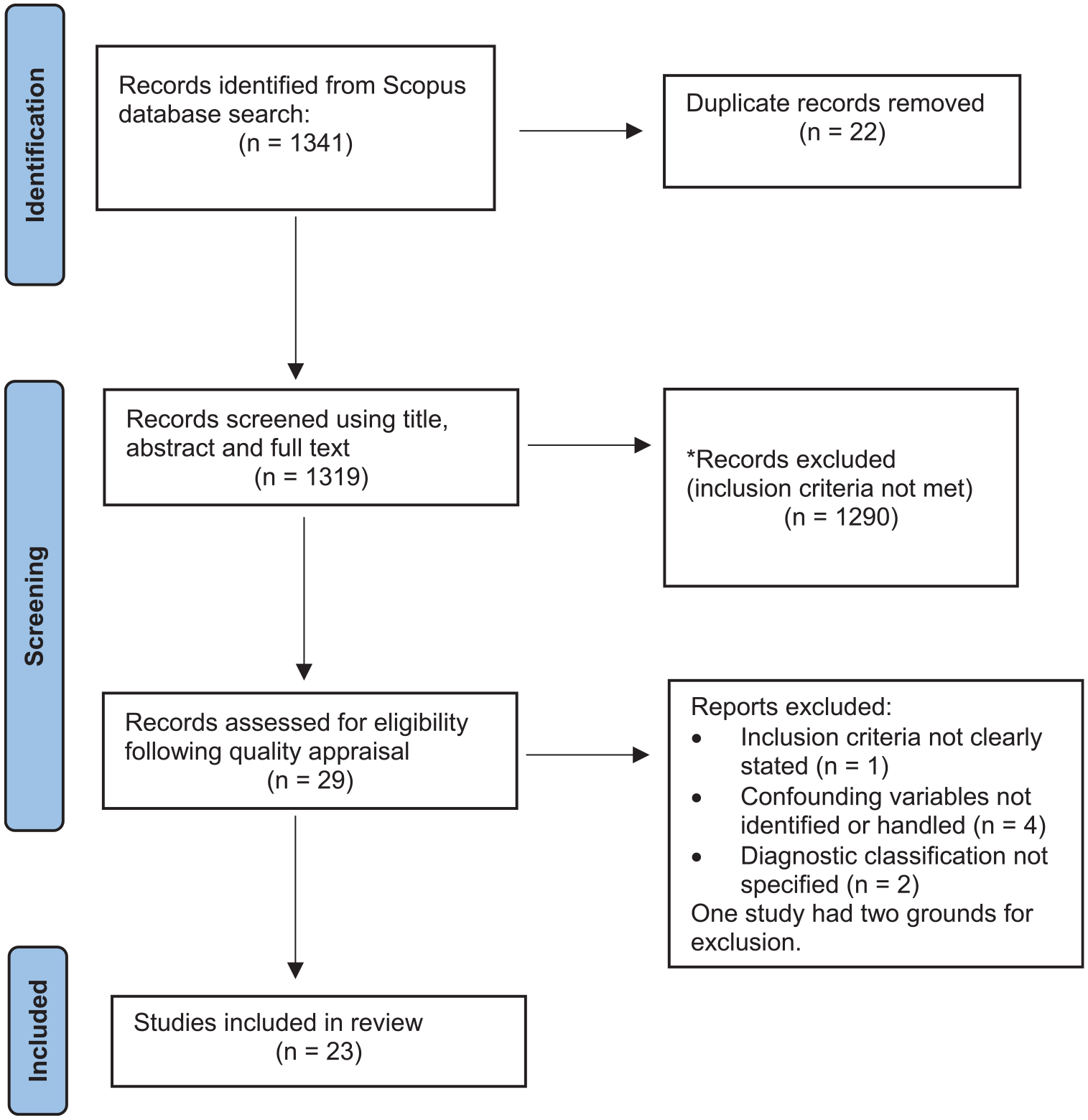
Flow chart of study selection.
Studies on suicide
In total, 20 studies (see Table 4) examined attempted suicide and suicidal behaviour, and some of these studies considered violent suicide attempts in inpatients with schizophrenia.
Eight of these 20 studies (Kavoor et al., 2017; Marcinko et al., 2005, 2007, 2008; Repo-Tiihonen et al., 2002; Ruljancic et al., 2007; Sankaranarayanan et al., 2020; Tripodianakis et al., 2002) concluded that relatively lower levels of cholesterol were associated with suicidality in patients with schizophrenia. Additionally, one of these studies (Repo-Tiihonen et al., 2002) found relatively lower TC (below 5.3 mmol/L) to be a marker of violent and suicidal behaviour. Apart from TC, low levels of HDL were associated with suicidality in three studies (Kavoor et al., 2017; Marcinko et al., 2008; Sankaranarayanan et al., 2020), of which one study was on males with schizoaffective disorder (Marcinko et al., 2008). Two of these studies also showed a link of suicidality with low LDL (Kavoor et al., 2017; Marcinko et al., 2008). Of these eight studies, one small sample study (Marcinko et al., 2005) showed that patients with a violent suicidal attempt had significantly lower TC levels than patients with non-violent attempts and non-suicidal controls but another study (Tripodianakis et al., 2002) with a far larger sample size found no such difference. Yet another study (Ruljancic et al., 2007) found a link between relatively low cholesterol and non-violent suicidal attempts (across several disorders) when compared to those without a suicidal attempt but did not report on such a link specifically for schizophrenia, schizoaffective disorder or psychotic disorder.
A total of seven studies (Capuzzi et al., 2018; Cariou et al., 2018; Gohar et al., 2019; Huang and Wu, 2000; Kunugi et al., 1997; Park et al., 2013; Shrivastava et al., 2017) did not find any link between lipid profile and suicidality in schizophrenia. In addition, one study (Chen et al., 2015) that examined the four types of aggression did not report findings on suicidality. One study (Misiak et al., 2015) found the opposite link, where relatively higher TC was associated with suicidal ideation in females with first-episode schizophrenia, thus demonstrating the complexity of the link. Finally, one study (Kim et al., 2002) found a link between relatively low TC and suicidality for major depressive disorder and personality disorder, but not for schizophrenia.
With regard to TG, seven studies (Capuzzi et al., 2018; Gohar et al., 2019; Kavoor et al., 2017; Marcinko et al., 2007; Misiak et al., 2015; Park et al., 2013; Sankaranarayanan et al., 2020) explored TG and suicidality, and none found an association.
All these studies were spread over a time period of more than two decades between 1997 and 2020. Sample sizes varied widely, from 31 to 802, though the smaller studies targeted patients admitted to hospital following a suicidal attempt. It is interesting to note, however, that the study (Sankaranarayanan et al., 2020) with the largest sample size (n = 802) did find a link between lipid profile and suicidality.
Studies on aggression against others
A total of nine studies (Cariou et al., 2018; Chakrabarti et al., 2004; Chen et al., 2015; Eriksen et al., 2017, 2018; Hjell et al., 2020; Huang and Wu, 2000; Repo-Tiihonen et al., 2002; Turkoglu et al., 2009) explored the link between lipid profile and violence against others, of which six studies found a link. However, there were some variations in the findings. One group of researchers (Eriksen et al., 2018) did not find a link with TC but with HDL, and only for men and not for women. The same authors, while studying violence in the first 3 months after discharge, also found HDL to be inversely associated with violence in men only (Eriksen et al., 2017). One study (Repo-Tiihonen et al., 2002) tried to identify a cut-off point for low TC levels to be a marker for violence, measured by frequency of seclusion, finding the cut-off level to be 5.3 mmol/L. Another researcher group (Kavoor et al., 2017) found a correlation with TC and LDL but not with HDL for measures of psychopathology, impulsivity and aggression (and suicidality).
One study (Cariou et al., 2018) retrospectively evaluated hospitalised patients over the course of a year and found a link between low plasma concentration of LDL and hetero-aggression. The group with low LDL also had a higher frequency of schizophrenia, thus reinforcing the link between low LDL levels, psychiatric disorders and aggression (Cariou et al., 2018).
Serum TG was explored in five studies (Cariou et al., 2018; Chakrabarti et al., 2009; Chen et al., 2015; Kavoor et al., 2017; Turkoglu et al., 2009) involving violence to others, with one finding a clear link between low TG and violence (Cariou et al., 2018), one between high TG and violence (Turkoglu et al., 2009), with the other three studies finding no significant link, but a trend towards a link between low TG and violence (Chakrabarti et al., 2009; Chen et al., 2015; Kavoor et al., 2017).
Two studies (Hjell et al., 2020; Huang and Wu, 2000) did not find a link between measures of serum cholesterol and violence in schizophrenia patients. Of these, the largest and most recent study (Hjell et al., 2020) had a large sample size (n = 1001) and examined all patients with schizophrenia recruited from inpatient and outpatient clinics of major hospitals in Oslo, Norway, between the years 2002 and 2017. It had 601 patients with schizophrenia spectrum disorders, and the measure of aggression was the PANSS Excited Component (PANSS-EC; Kay et al., 1987). This scale has items on excitement, hostility, tension, uncooperativeness and poor impulse control. Impulsivity was measured with the Barratt Impulsiveness Scale (BIS-11; Patton et al., 1995). There were no significant associations between TC, LDL, HDL and aggression or impulsivity in patients with schizophrenia spectrum disorders. The other study (Huang and Wu, 2000) examined paranoid and non-paranoid schizophrenia patients and did not find significant differences in serum cholesterol levels between patients with and without physical violence and patients who had or had not made a suicidal attempt. This study was on an exclusively inpatient sample.
The studies were again spread over a time period of almost two decades, between 2002 and 2020. Sample sizes varied widely, the largest study with a sample size of 1001 (Hjell et al., 2020), medium level studies with sample sizes of 409 and 348 (Eriksen et al., 2018; Repo-Tiihonen et al., 2002) and the smallest with a sample size of 60 patients (Chakrabarti et al., 2009).
Studies assessing sex differences
For the studies on suicidality, there were only three studies and these were exclusively single sex, for males (Marcinko et al., 2005, 2007, 2008). One found a link between low TC, low LDL and low HDL (but not low TG) and suicidality in schizoaffective disorder (Marcinko et al., 2008), one found a link between low TC and suicidality in first-episode psychosis (Marcinko et al., 2007) and the third study found low TC in patients with violent suicidal attempts as opposed to non-violent suicidal attempts and controls (Marcinko et al., 2005).
For the studies exploring link between cholesterol levels and violence, there were three studies exclusively on males (Chakrabarti et al., 2004; Repo-Tiihonen et al., 2002; Turkoglu et al., 2009), all involving forensic populations. These studies all found a significant association between relatively low TC and violence, except one (Turkoglu et al., 2009), where the association did not reach statistical significance. With regard to the studies which found a positive link between low TC and suicidality, one study (Misiak et al., 2015) which had both males and females in it found a link between relatively higher TC and LDL levels with suicidal ideation in female, but not in male first-episode schizophrenia patients. One problem with this study, however, was the relatively low overall prevalence of suicidal ideation. The authors themselves advise caution in the interpretation of the study results.
With regard to the studies examining the link between lipid profile and violence, one study (Eriksen et al., 2018) found low HDL to be contributing significantly to the model for violence risk assessment in males, but not females. In another report from the same group (Eriksen et al., 2017), low HDL level was significantly correlated with violence for males but not females in the first 3 months following discharge. However, another study (Chen et al., 2015), where sex distribution was 33 male and 74 female schizophrenia patients, found female sex and low dichotomised TC levels as two of five variables (others being early onset, higher scores of positive symptoms and lower scores of negative symptoms) which could be used as predictors of violence, with a predictive accuracy of 0.85 (95% CI = [0.72, 0.97]).
The studies which exclusively examined male populations were all in forensic patients and all suggested a link between lower TC and violence (Chakrabarti et al., 2004; Repo-Tiihonen et al., 2002; Turkoglu et al., 2009). However, there have been no recent studies on forensic populations, and none involving female forensic populations.
A study of 41 male and 19 female schizophrenia patients (Shrivastava et al., 2017) observed that females with moderate but not low or high suicidality had lower cholesterol levels to statistical significance, but such a link was not found for males. However, sample sizes were really low (n = 4–9 per subgroup in female participants) in this study.
Overall, the link between lipid profile and violence seems to be slightly stronger for males than females, but that might well be because males have been studied more often than females. There is also some inconclusive evidence to suggest that the relationship might be different for females and males, both for violence and suicidality.
Discussion
There were three main findings in relation to the primary objectives of this systematic review.
First, there were many more studies which reported on a link between low cholesterol and violence to others than those which did not find a link. All researchers investigating forensic samples found such a relationship. However, the relationship was not only with low TC but also with other parameters of the lipid profile, such as low LDL and low HDL. It is thus important not just to collect data on TC, but LDL and HDL as well. The evidence was weaker for the link between TG and violence, with only two studies finding a link, but one with high TG, the other with low TG. It is to be noted that the study with the largest sample size failed to find a link (Hjell et al., 2020). However, one of the issues in this study was the relatively low rate of baseline violence in the study population, thus offering some indication that the link is likely to be more valid in groups where there is a greater prevalence of violence (i.e. forensic populations).
The biological mechanism behind cholesterol–violence association has been hypothesised to involve serotonin. Animal studies have found an increase in violent behaviour in monkeys assigned to a low-cholesterol diet (Kaplan et al., 1991, 1994). Kaplan et al. (1991) suggested that low cholesterol may reduce cell viscosity and reduce serotonergic receptor activity. This may lead to a depressive state (Marcinko et al., 2005), increased impulsivity (Carver and Miller, 2006; Paaver et al., 2007) and aggressive behaviour (Chakrabarti et al., 2004). This finding was observed in Kaplan et al. (1994), where monkeys with experimentally lowered cholesterol had higher concentrations of serotonin metabolites than monkeys given high-cholesterol diets. However, the exact biological mechanism underlying cholesterol–violence (towards self/others) association in humans is still unclear.
Second, there was mixed evidence for a link between low cholesterol and suicidality in schizophrenia, with almost equal number of studies in favour and against such a link. The majority of studies used suicide as the method of assessing aggression. Eight studies found a statistically significant association between low cholesterol and suicide attempts, two of which only found this association in females (Misiak et al., 2015; Shrivastava et al., 2017). Seven studies failed to find a link. However, the study with the largest sample size (Sankaranarayan et al., 2020) did find a link, thus suggesting that methodological flaws, particularly low power, might have contributed to the variation in findings.
The evidence for a specific relationship between lipid profile and violent suicidal attempts was even more mixed. Ruljancic et al. (2007) found a significant association between low cholesterol and non-violent suicide attempts, in contrast to two other studies (Marcinko et al., 2005; Tripodianakis et al., 2002), reporting an association between low cholesterol and violent suicide attempts. While the two studies showing a positive association had smaller sample sizes, such findings are supported by other literature (Garland et al., 2000; Vevera et al., 2003). A meta-analysis found 50% more violent deaths in males with relatively low cholesterol than in participants with higher levels of cholesterol (Jacobs et al., 1992). This meta-analysis also found a higher prevalence of depressive symptoms in males with low serum cholesterol.
An association between low cholesterol and depression has frequently been observed (Grussu et al., 2007; Ploeckinger et al., 1996; Troisi et al., 2002). It is plausible that the causal pathway from low cholesterol to suicidality in schizophrenia patients involves depression. Kunugi et al. (1997) did not find a significant difference in cholesterol level between suicidal and non-suicidal inpatients with schizophrenia spectrum disorders. However, significantly lower cholesterol levels were found in suicide attempters with mood disorders compared with controls. Similarly, Modai et al. (1994) found a significant association between lower cholesterol and suicidality in patients with depression, but not in schizophrenia patients. Around 40% of people with schizophrenia have depression, with depression being the most significant factor in completed suicide (Upthegrove et al., 2016). People with schizophrenia and comorbid depression also have a significantly increased risk of violence and suicidality (Conley et al., 2007) and poorer clinical outcomes (Gardsjord et al., 2016; Upthegrove et al., 2009). The studies included in this systematic review did not control for depressive symptoms in schizophrenia patients. Although findings of low cholesterol and depression are inconsistent, with a number of researchers not finding a significant association (Cepeda et al., 2020; Van Dam et al., 1999), it is plausible that suicidality seen in schizophrenia patients with low cholesterol may be a consequence of depressive symptoms.
Third, most of the studies had similar findings for males and females. However, low HDL was seen in two studies to be a better predictor of violence than low TC for males (Eriksen et al., 2017, 2018). Another study found female sex and low TC levels could be used, in part, as predictors of violence in patients with schizophrenia (Chen et al., 2015). One study found higher TC and LDL levels to be associated with suicidality in females but not males with first-episode schizophrenia, thus suggesting that the link between lipids and violence is somewhat complex (Misiak et al., 2015). Future studies need to be designed to explore the nature of the link separately for females and males. All studies (Chakrabarti et al., 2004; Marcinko et al., 2005, 2007, 2008; Repo-Tiihonen et al., 2002) investigating only male schizophrenia patients found a significant association between low cholesterol and suicidality, except one group (Turkoglu et al., 2009) who did not report a significant association. On the contrary, three study authors observed an association only in female participants: two for suicidality (Misiak et al., 2015; Shrivastava et al., 2017) and one for violence towards others in patients with schizophrenia (Chen et al., 2015). However, one study (Eriksen et al., 2017) did not find this specific correlation in female participants.
Thus, it can be concluded that cholesterol levels could be used, in part, as predictors of violence in patients with schizophrenia. The evidence for a clear link with sex remains inconclusive. This is an important area for further work given that rates of violence in psychiatric patients following discharge tend to be higher in men than in women (Robbins et al., 2003). In addition, the neurobiology of violence, factors like body mass index (BMI), incidence of metabolic syndrome following antipsychotic medication and the effects of cholesterol are different between men and women, suggesting that discrete effects may occur in each sex (Golomb, 1998).
Limitations
There were several limitations regarding the studies reviewed. First, in many of the studies reviewed, the main focus was on suicide and physical aggression to others. As a result, most patients observed were clinically ill enough to warrant inpatient treatment. Few studies evaluated aggression as physical against property and verbal, potentially deemed less severe and more likely to be seen in community or outpatient-based studies. A representative view of schizophrenia patients of all severities, including inpatients and outpatients, was therefore not specifically assessed in this review. Second, confounding factors, including sex, medication and age, may have affected the findings of this review. According to the Gender Paradox in Suicide, men are more likely to die by suicide than women, while women are more likely to engage in suicidal behaviour and deliberate self-harm (Canetto and Sakinofsky, 1998). However, self-harm was not frequently assessed in these studies. There is some indication of a link between low TC, HDL, LDL and impulsivity, which could translate into risk of self-harm, but this link needs to be explored through studies in populations with higher self-harming behaviours, like inpatient female wards. Medication, such as certain antipsychotics like risperidone, stimulate serotonergic output in cortical and subcortical areas more than other antipsychotics (Amato, 2015), and this may contribute to changes in aggressive behaviour independent of cholesterol level. In addition, with age comes a natural variance in cholesterol level, with a tendency of increased serum cholesterol with increasing age (Morgan et al., 2016). Aggressive behaviour may be independent of low cholesterol in younger participants as they, typically, would have a lower cholesterol level when compared to older patients. The effects of age as well as medication were not accounted for in a number of studies. Finally, the lack of statistical analysis using a 95% confidence interval in a number of studies (see Table 4) limited the review by making it difficult to assess precision and risk in data obtained.
In addition, there are limitations to the review itself. First, the review may have been limited by only allowing diagnosis of schizophrenia by a variant of DSM or ICD classifications. This excluded foreign classifications such as T-SCL-90-R. Second, selection bias arose when only considering studies reported in English. The inclusion and exclusion criteria stated that participants must be adults only, unless unavoidable. As a result, three included studies (Chen et al., 2015; Repo-Tiihonen et al., 2002; Ruljancic et al., 2007) had some participants below the age of 18, leading to wide variations in the age range of the study participants.
Conclusion
This systematic review presents encouraging evidence of low cholesterol showing promise as a biomarker of risk in patients with schizophrenia. The majority of studies (around 70%) did find an association between low cholesterol and violence towards others, as well as about half of the studies with suicidal behaviour. However, studies specifically focusing on males and females with schizophrenia were lacking, along with relatively small sample sizes for some studies. Future studies need to be carried out focused exclusively on participants with a diagnosis of schizophrenia, and with histories of violent, self-harming and suicidal behaviours. These studies need to be longitudinal, exploring measures of self-harm, suicidality and aggression in male and female patients, both inpatients and outpatients, while taking age, medication history and any comorbidities into account, to explore patterns of link with lipid profiles including TC, LDL and HDL. Preferably, these studies should also include patients with other diagnoses as comparison groups. Such research would be essential to explore how a relatively commonly assessed measure like serum cholesterol along with high- and low-density lipoprotein could be incorporated into calculations of risk for any patient with schizophrenia, whether it is risk to others or to self.
Footnotes
Acknowledgements
We gratefully acknowledge Joanne McPhie, Librarian at Brunel University, for her assistance with identification of appropriate key words and databases for the literature search.
Author Contributions
P.S. and V.K. contributed to conception of the review; P.S. and D.A. led the literature search, quality appraisal and data extraction from the eligible studies; V.K. contributed to review of data from the eligible studies; P.S. and D.A. wrote first draft of the paper; A.I.B. and V.K. critiqued the output for important intellectual content. All authors contributed to and approved the final version.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship and/or publication of this article: P.S. was supported for some of his research time and for sponsorship of his PhD at Brunel University London by Elysium Healthcare, UK.
Data Accessibility Statement
All data supporting this review will be made available through Brunel University London research repository.
