Abstract
Patients with epilepsy have their authorisation to drive restricted under detailed guidelines, but the rules for those with non-epileptic seizures are far less clear. We surveyed specialist clinicians in Australia and found little agreement as to whether such guidelines existed for non-epileptic seizures or what they might be. A number of possible interpretations of the Australian fitness to drive guidelines are explored, and these are often vague in themselves, as well as uncertain in their scope. This means clinicians making momentous driving decisions for their patients with non-epileptic seizures are doubly challenged, first in interpreting what guidelines exist, and second in what they mean. The International League Against Epilepsy proposed specific guidelines for driving with non-epileptic seizures, which reflect the range of presentations of non-epileptic seizures in a decision-making algorithm. We believe a specific algorithm such as this is essential in removing one level of uncertainty and responsibility for clinicians, and restoring equity for patients with non-epileptic seizures.
Can you drive if you have non-epileptic seizures?
People with epilepsy commonly have their licence to drive restricted. Though this protects the safety of the public and the patient, these restrictions come at a cost to the patient’s liberty and quality of life, particularly in a car-dependent country like Australia (Somerville and Driving Committee of the Epilepsy Society of Australia, 2019). Consequently, the regulations in most countries will attempt to calibrate the degree of restriction to the phenomenology and frequency of the seizures. This balances the safety of the public with the cost to the patient with epilepsy, and discussions around it often form a critical part of the ongoing management of epilepsy. But what about the other primary seizure disorder, non-epileptic seizures (NES)?
The seizures of NES can be as disabling (Karakis et al., 2014) and as frequent (Kemp et al., 2018) as those in epilepsy, though their impact on driver safety is far less clear. Perhaps because of this, and certainly compounding it, the regulations are usually also less clear – to the extent that it may be unclear whether those regulations even exist. This was brought to light for the authors recently when contributing to an international consensus statement (Asadi-Pooya et al., 2020) on what the rules about driving with NES should be: one of us was sure the rules for NES in Australia were the same as for epilepsy, another that there were no rules for NES. We examined how far this confusion extends by an informal survey of our specialist networks – precisely those clinicians who should know what the rules are. We asked 67 clinicians (neurologists, neuropsychiatrists, neuropsychologists, clinical nurse consultants) across Queensland, New South Wales and Victoria, ‘What are the regulations for non-epileptic seizures and driving in Australia?’, of whom 60 replied (90%) with the results in Table 1.
Survey of specialist clinicians on the regulations for driving applicable to NES.
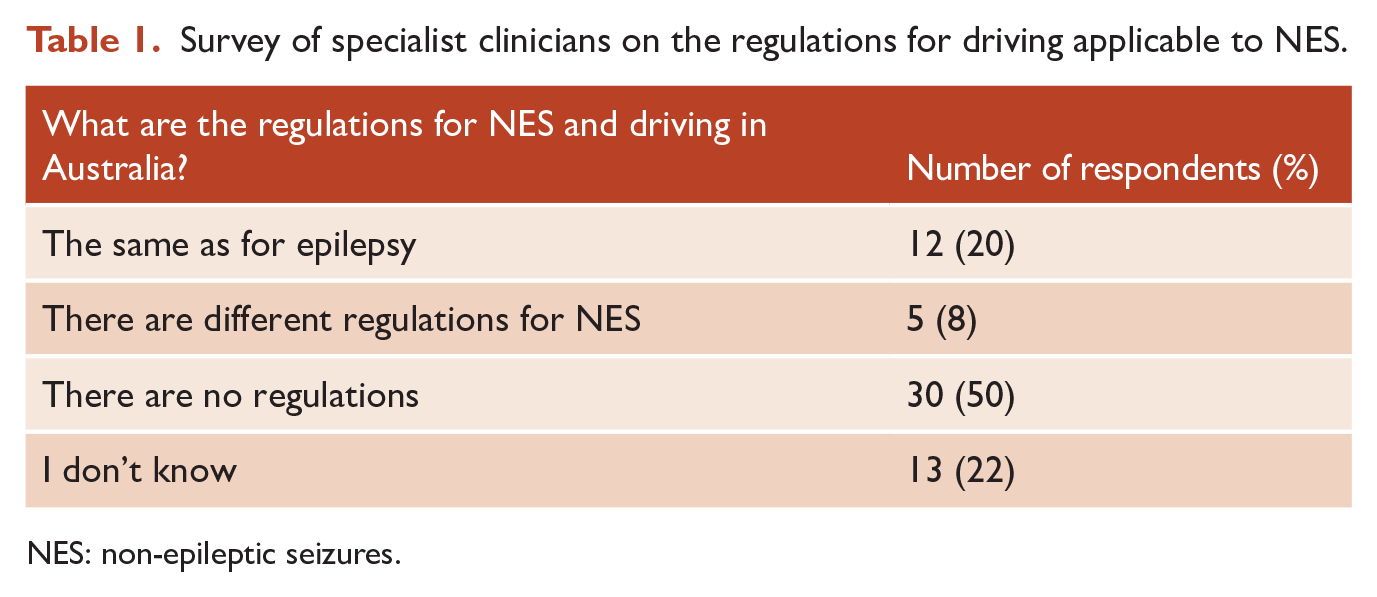
NES: non-epileptic seizures.
What does that mean for this critical management decision? If not exactly arbitrary, it certainly means it would be hard to predict the outcome. For the decision will now rest not only on the clinician’s interpretation of the rules, but also on their interpretation of which rules, if any, apply. We will look briefly at what those rules might be, before outlining what we think should be done.
What might be the rules?
In Australia, as in most countries, it is the responsibility of the driving licencing authorities to decide whether a patient with a health condition should be allowed to drive or not. In clinical practice, however, this responsibility is often delegated to the treating physician (Somerville et al., 2010). Austroads is the peak organisation of road transport and traffic agencies in Australia and New Zealand. Its publication Assessing Fitness to Drive details medical standards for driver licencing purposes for use by health professionals and driver licencing authorities (Austroads and National Transport Commission, 2016). While these guidelines can be quite complex, they give detailed guidance about patients suffering from ‘seizures and epilepsy’. For these patients a ‘default standard’ has been determined, which applies to all drivers who have had a seizure (minimum 1-year seizure-free non-driving period) unless reductions are allowed based on specific types of epilepsy or specific circumstances. For a first seizure, for example, the seizure-free non-driving period can be reduced to 6 months.
The Austroads guidelines make no mention of Functional Neurological Disorders, in general, or NES in particular. Though the psychiatric section explains that assessment should be by the pattern of illness rather than diagnosis, the diagnoses it covers include nothing like NES. It concludes that if the condition is ‘associated with epilepsy’ that section should be referred to as well, and the guidelines on ‘seizures and epilepsy’ are perhaps sufficiently vague to cause the confusion among experts as to whether they can or should be applied to patients suffering from NES (as evidenced by our survey). The Austroads guidelines emphasise that not all conditions and clinical situations that might impair someone’s ability to drive safely are covered. They also mention that other neurological or psychiatric conditions not covered specifically by the guidelines should be assessed individually and that a practical driving assessment may be required. They say that ‘a degree of professional judgement is therefore required in assessing fitness to drive’ in these situations (Austroads and National Transport Commission, 2016).
This advice appears reasonable in theory, but in practice puts the treating physician in a very difficult position. A test of driving ability would not usually be useful for patients with NES, due to the variable and episodic nature of the disorder (patients may go many weeks between seizures), which means the responsibility will devolve almost entirely to the ‘professional judgement’ of the physician. The impact of restricting someone’s driving is huge (Xu et al., 2015) and while the treating doctor has responsibility to the wider community and the public’s safety, he or she also needs to develop and maintain a therapeutic relationship with the patient with trust and honesty between both parties. Yet, in an increasingly litigious world, the fear of potential civil and criminal proceedings may strongly influence doctors’ practice. Some doctors will not wish to cancel their patients’ licences to avoid damaging the doctor–patient relationship, while others might practice defensive medicine, applying overly strict driving criteria over concerns about lawsuits (Jones et al., 2012; Nash et al., 2009). Discussions about driving restrictions are challenging for health professionals at the best of times and doctors find this particularly difficult if guidelines are not clear (Farooq et al., 2018; Jones et al., 2012).
Australia is not alone in grappling with this, of course, and the experience of other countries can be instructive. The United Kingdom had similar issues to Australia in the past. Their Driver and Vehicle Licensing Agency (DVLA) had specific advice for patients with NES, although it was vague: ‘Licence will be issued after medical reports confirm that behavioural disturbances have been satisfactorily controlled’ (DVLA, 2010). It was not specified what ‘satisfactory control’ actually meant and the levels of confusion were similar to those indicated in our Australian survey (Morrison and Razvi, 2011). The DVLA guidelines have been revised more recently and for private vehicles and motorcycles they are now as follows: ‘Licensing may be considered when the driver or applicant has been event free for three months. If episodes have occurred or are considered likely to occur whilst driving, a specialist’s review would also be required prior to licensing’ (DVLA, 2020).
Still a nuanced threshold, clearly, though a notably less restrictive one than for epilepsy, but at least the clinician will know they are on the right page.
What should be done?
The findings of our survey highlight that in the Australian context, the current guidelines provide insufficient guidance for decision-making in relation to driving in patients with NES. This uncertainty about driving regulations in Australia reflects a lack of certainty on this issue both locally and internationally. The risk seems likely to be less than for epilepsy, but opinions differ (Asadi-Pooya et al., 2020), and there is very little systematic evidence. What is clear is that robust research involving a large number of participants with NES will be needed to establish the actual level of risk to both self and others. However, even future research is unlikely to provide a simple answer – a one-size-fits-all solution – because the clinical manifestations of NES have many guises, lie on a spectrum of severity and can change across time and context. While some NES involve clinical symptoms that are likely to interfere with capacity to drive, others do not.
In this context, because of heterogeneity and individual differences across patients, the clinical decision process for assessing fitness to drive is likely to require an algorithm/decision-making tree that includes the broad range of factors that might apply in any particular case regarding any particular patient. The International League Against Epilepsy (ILAE) Report by the Task Force on Psychogenic Nonepileptic Seizures has proposed such an algorithm for assessing whether individuals with NES are safe to drive (Asadi-Pooya et al., 2020). In addition to requiring that the individual be seizure-free for 6 months (a figure determined by a survey of professionals working with NES), the algorithm includes a range of other potential risk and mitigating factors. Factors that were felt to increase risk included a history of seizure-related injuries, or of changes in conscious (‘loss of awareness responsiveness’); factors that were felt to mitigate risk included seizures occurring exclusively in response to defined triggers not related to driving, or antecedent warning signs that give the person ample time to move off the road.
This is clearly too complicated for a simple soundbite of NES driving risk, but it is clearly well within the grasp of clinicians. The use of such algorithms has already been tested in other Australian public departments, such as for clinicians to assess the risks in reporting harms to children (Family and Community Services provides an algorithm that clinicians can use to determine the level of risk of harm for children [NSW Government Communities and Justice, 2019]) and, of course, to assess driving risk for epilepsy (Austroads and National Transport Commission, 2016). It is also appropriate to the importance of the decision. However complex and uncertain those guidelines are, clinicians and patients should have confidence that they are at least the right guidelines for NES, to ease the burden on clinicians, and restore equity to patients.
Footnotes
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: R.A.K. is Chair of the RANZCP Section of Neuropsychiatry. All authors contributed to the ILAE guidelines.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
