Abstract
Objectives:
The aim of this scoping review was to map and synthesise peer-reviewed literature reporting on the Australian National Disability Insurance Scheme and psychosocial disability.
Method:
The review followed the rigorous and systematic protocol of Arksey and O’Malley. Five databases were searched and, using strict inclusion and exclusion criteria, publications were identified for inclusion. Data were extracted from publications, tabulated and graphically presented. A qualitative analysis was also completed.
Results:
Twenty-eight publications were included. While a wide range of issues were covered across this literature, only eight publications specifically focused on the National Disability Insurance Scheme. Almost half of publications were only author commentary without analysis of external data. There were no evaluations and a paucity of publications documenting the lived experiences of people with psychosocial disability or their families. Qualitative analysis identified 59 separate themes. These were grouped using a modified strengths, weakness, opportunities and threats framework. While it was acknowledged that the Scheme has the capacity to enrich people’s lives and enhance service integration, themes relating to weakness and threats dominated within this literature. These included a variety of existing or predicted problems such as poor integration of a recovery philosophy into the National Disability Insurance Scheme, complex application processes creating barriers to access, concern for those ineligible or not accessing the National Disability Insurance Scheme, the need to ensure National Disability Insurance Scheme plans address specific, changing participant needs and that services will be available to provide required supports.
Conclusion:
Given the significant impact of the National Disability Insurance Scheme on the lives of individuals and the wider mental health service system, there continues to be surprisingly limited peer-reviewed literature reporting on experiences and outcomes of the Scheme for people living with psychosocial disability. Future research examining outcomes and shedding light on National Disability Insurance Scheme experiences of people with psychosocial disability and their families are particularly important for ongoing development and evaluation of the Scheme.
Keywords
Background
Since the inception of the first ‘National Mental Health Plan’ (Australian Health Ministers, 1992), the mental health system in Australia has undergone a series of important changes (Grace et al., 2017). One of the most profound changes to impact the lives of people with severe and persistent mental illness and the mental health service system across Australia occurred when Parliament passed the National Disability Insurance Scheme Act (Australian Government, 2013).
The National Disability Insurance Scheme (NDIS) is designed to provide no fault insurance cover for Australians living with ‘permanent disability’ including those with disability stemming from severe and persistent mental illness (Australian Government, 2013). The National Disability Insurance Agency (NDIA) is charged with development and oversight of the Scheme. NDIS represents a major paradigm shift in the organisation, planning, funding and delivery of services. The NDIS is described as a ‘person-centred’ approach where participants, people with disability, can control their own service plans and budgets, directly seeking and purchasing the services they choose (Bonyhady, 2014).
The Scheme was initially designed without the inclusion of people with a psychosocial disability in mind (Williams and Smith, 2014). Psychosocial disability was the last major disability group to ‘join’ the NDIS (Smith-Merry et al., 2018). Funding for the Scheme was drawn, in part, from the termination of previous national psychosocial programmes delivered through the non-government or community-managed sector: Partners in Recovery (PIR), Personal Helpers and Mentors (PHaMs) and Day to Day Living (D2DL) (Hancock et al., 2019). Concerns have been raised regarding the termination of these programmes given that: (a) psychosocial services delivered through the non-government sector were such a small proportion of the mental health budget to start with (Department of Health and Ageing, 2013) and (b) only a small proportion of people (approximately 10%) with severe and persistent mental illness will be eligible for the Scheme and therefore fewer services would be available for the majority (National Mental Health Commission, 2017; Smith-Merry et al., 2018).
To gain access to the NDIS, people living with severe mental illness need to gather and submit evidence to prove that their mental illness results in a disability, that is, that their illness has a long-term impact upon their ability to do everyday activities. The NDIA, responsible for development and oversight of the Scheme, estimated that at full roll out (2019–2020) the NDIS will support 460,000 Australians living with disability, with 13.9% or 64,000 of these people expected to have a primary psychosocial disability (National Disability Insurance Agency, 2018).
Given that the Scheme has been rolling out for greater than 6 years and is anticipated to reach full roll out by the end of 2020, it was deemed timely to survey, collate and synthesise the peer-reviewed literature on the NDIS for people with a psychosocial disability. To achieve this, a systematic scoping review was undertaken.
Methods
A scoping review is designed to survey and ‘map’ literature that has been written about a topic in a systematic reproducible manner (Peters et al., 2015). Unlike a ‘systematic review’, quality of the evidence is not assessed but rather a detailed, broad overview is sought. Five methodological stages developed by Arksey and O’Malley (2005) were used to ensure a robust and comprehensive overview of the literature was achieved.
Stage 1: identifying the research question
It is important to keep the research question broad enough to capture all relevant literature but specific enough to be systematically rigorous in its application. The question asked was: What does the breadth and focus of literature published to date within peer-reviewed literature tell us about the Australian NDIS and psychosocial disability?
Stage 2: identifying relevant publications
To identify relevant publications, five electronic databases were searched: CINAHL, Medline, Web of Science, PsychINFO and Scopus. The primary search was undertaken in July 2019 with a ‘top up’ search completed in February 2020. In the first four databases, searches were undertaken using the terms NDIS OR National Disability Insurance Scheme OR NDIA OR National Disability Insurance Agency AND Psychosocial OR Psychiatry* OR Mental OR depress* OR schizophren* OR affective disorder* OR psychosis OR mood disorder* OR psycho* OR dissociat* OR personality disorder* OR obsessive compulsive disorder* OR trauma*. Scopus was searched using the keywords NDIS OR National Disability Insurance Scheme OR NDIA OR National Disability Insurance Agency AND psychosocial OR psychiatry OR mental.
The ‘grey literature’ was not included in the search, but it is acknowledged that there have been several non-peer-reviewed reports published on the NDIS and psychosocial disability (e.g. ‘People Making Choices’ (Brophy et al., 2014), ‘Choice Control and the NDIS’ (Warr et al., 2017), ‘National Disability Insurance Scheme: Psychosocial Disability Pathway’ (Mental Health Australia, 2018), ‘Mind the Gap’ (Smith-Merry et al., 2018) and a recent evaluation by Tune (2019)).
Stage 3: study selection
Inclusion and exclusion criteria were developed by the authors. Publications were excluded if they were about children or focused solely on overseas schemes without specific comment about Australia. If publications mentioned psychosocial disability and the NDIS they were included, but those exclusively focused on other disabilities and the NDIS were excluded. Publications that focused on ‘psychosocial disability’ with no mention of the NDIS were similarly excluded.
Two authors (D.H. + J.N.S.) independently reviewed all included publications. This commenced with a review of titles, then abstracts and finally full texts. At each stage, the two authors compared their assessments and where discrepancies existed, these were resolved through discussion.
Finally, reference lists and citations of the included publications were then searched by hand to identify any other relevant publications.
Stage 4: charting the data
The data charting process involved extracting several data points from each publication. First, the journal name, year of publication and methods used were extracted. Second, the ‘primary focus’ of the publication was recorded. This was to identify where NDIS was the main focus of the publication and where it was mentioned in a secondary or peripheral way in the discussion section for example. Finally, the ‘perspective(s) presented’ was extracted, listing whether the publication reported on perspectives of consumers, carers/families, service providers or predominantly the opinions of the authors themselves.
Stage 5: collating, summarising and reporting data
Information from the data charting process was summarised and graphed to give an overview of the literature. Included publications were then subjected to a rigorous process of qualitative thematic analysis. The first step involved two authors (D.H. and N.H.) independently coding four publications. Each publication was read line by line and any data relating to NDIS and psychosocial disability were then coded using inductive constant comparative methods (Charmaz, 2014). Authors then met to compare coding decisions and reach consensus. D.H. then continued the analysis of remaining publications meeting regularly with the team to discuss and ensure coding remained true to original meanings. At these team meetings, authors also discussed initial codes and drew together those that the team agreed to be conceptually similar.
As a final step, a modified qualitative SWOT (strengths, weakness, opportunities and threats) analysis was undertaken. SWOT is described in detail elsewhere (Gürel and Tat, 2017). This step involved deductively aligning each code to one of the four SWOT domains – strengths, weaknesses, opportunities and threats. Modified slightly from the original SWOT definitions, ‘strengths’ and ‘weaknesses’ were those expressed as currently occurring whereas the ‘opportunities’ and ‘threats’ were those anticipated as future possibilities at the time they were written.
Results
The initial search yielded a total of 206 publication and an additional 25 publications were identified in the top-up search. A total of 23 publications were retained from the initial search and 4 from the top-up search. One additional publication was identified in the hand searches of citations and reference lists, giving a total of 28 publications included in the final review. The overall process is summarised in Figure 1. Charted data from the 28 included publications are available as Supplemental File 1.
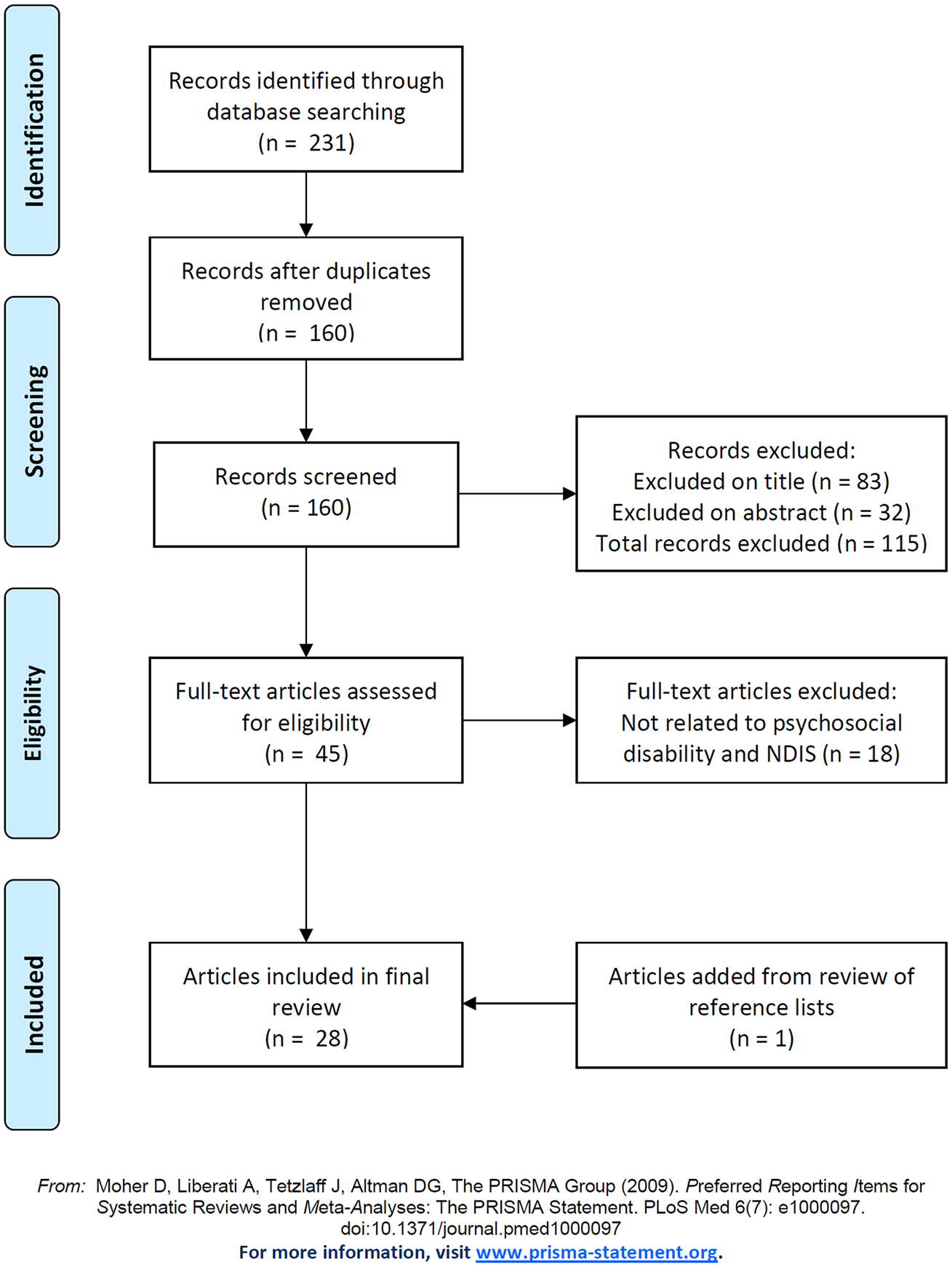
Publication selection diagram (based on the PRISMA flow chart).
The primary sources for publications about psychosocial disability and the NDIS were Australian and New Zealand Journal of Psychiatry (5/28; 18%) and its sister journal Australasian Psychiatry (3/28; 11%), representing a total of 29% (8/28) of publications. Other journals to include more than one publication included Australian Occupational Therapy Journal (two publications); Health and Social Care in the Community (two publications) and Public Health Research and Practice (two publications). Most (22/28; 79%) were published since 2017 with the remainder published in 2014 (n = 4) and 2016 (n = 2).
Figure 2 reports information about the methods used and identifies whether NDIS was the primary or peripheral focus of each publication. A range of data collection methods were used with almost half of all publications (13/28; 46%) being commentaries rather than analyses of empirical data. Only eight publications (29%) were primarily focused on the NDIS itself. Other publications focused on a breadth of topics such as intellectual disability, employment, housing and other mental health initiatives and peripherally discussed their findings in relation to the NDIS and people with psychosocial disability.
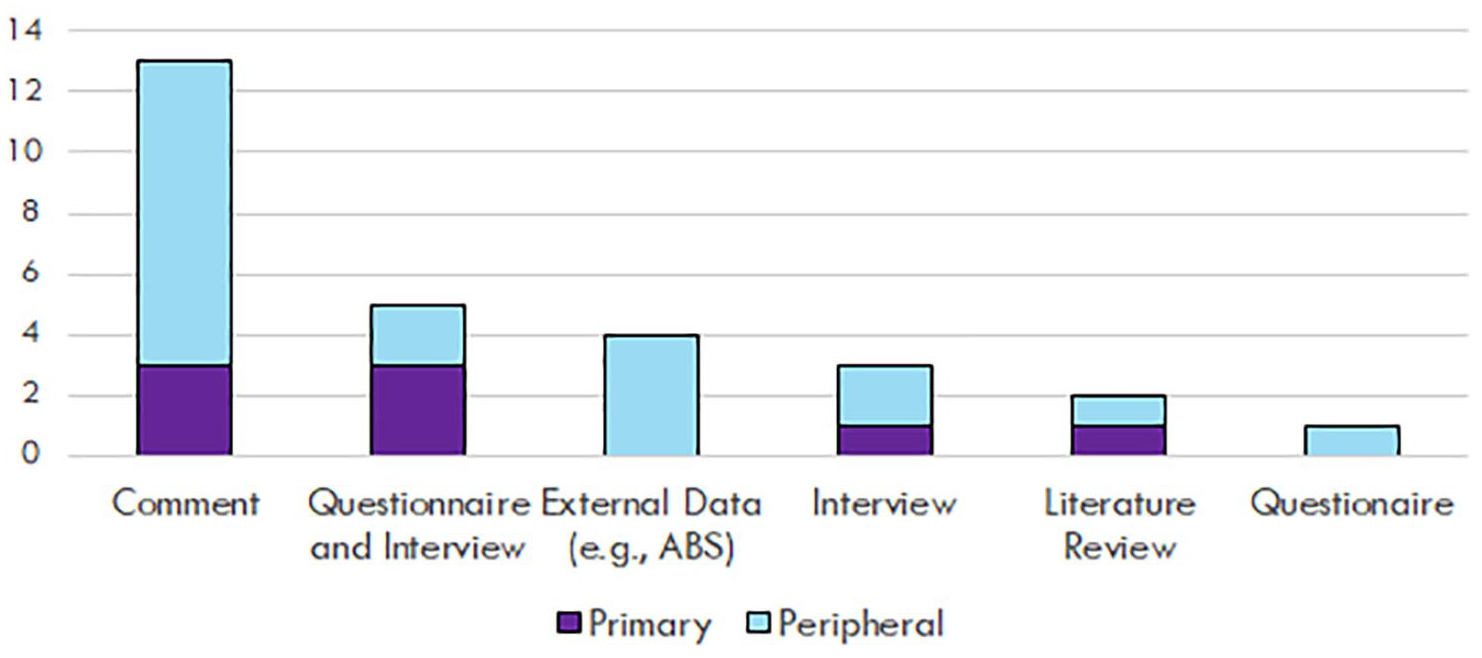
Methods used in publications and focus of publication.
Figure 3 summarises the perspectives examined or presented in each publication. Where comments about the NDIS and psychosocial disability were not based on empirical data, the perspective was deemed to be the authors. Author’s perspective rather than data-driven insights comprised 61% (17/28) of the included publications.
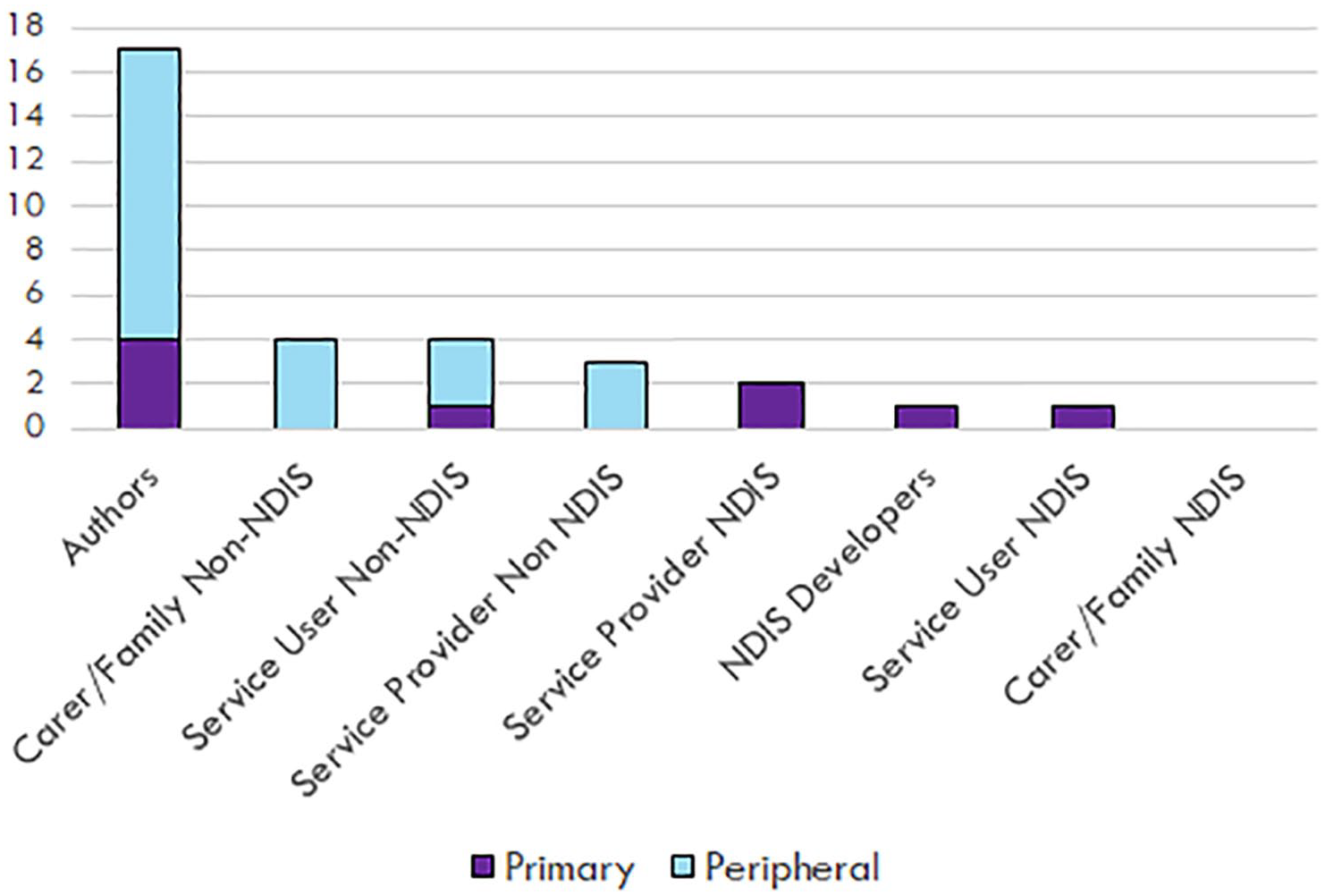
Perspective presented in the publication.
Table 1 presents the results of the qualitative analysis which resulted in 59 separate codes or themes. These were grouped into current strengths of the Scheme for people living with psychosocial disability (n = 2), current weaknesses (n = 10), potential opportunities (n = 20) and potential threats (n = 27).
Thematic analysis of literature (SWOT: strengths, weaknesses, opportunities and threats).
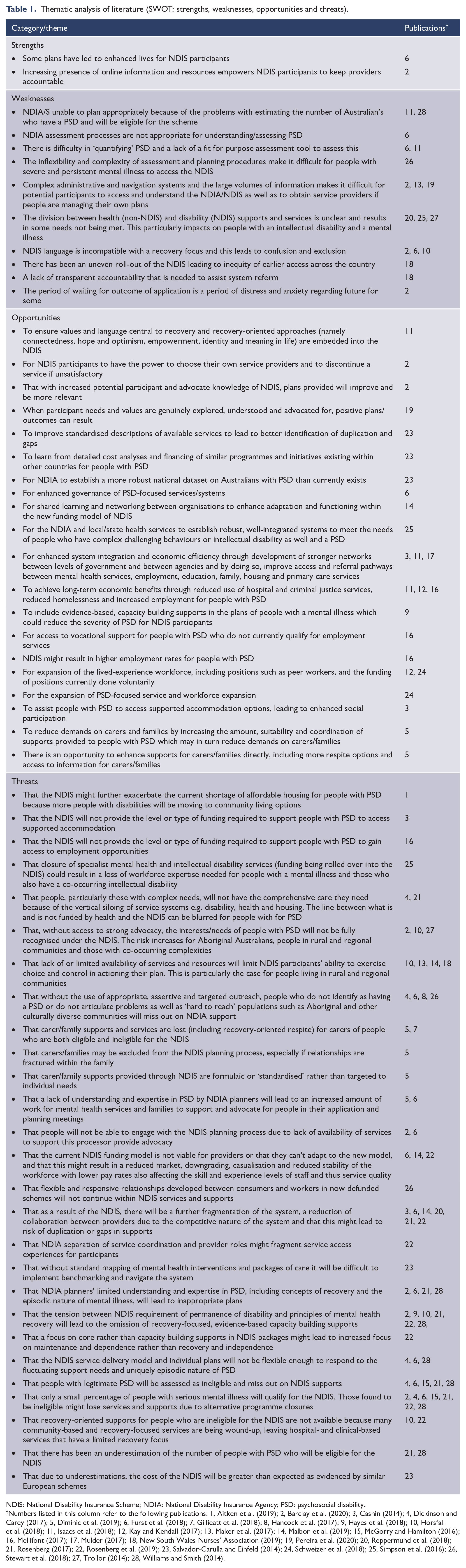
NDIS: National Disability Insurance Scheme; NDIA: National Disability Insurance Agency; PSD: psychosocial disability.
Numbers listed in this column refer to the following publications: 1, Aitken et al. (2019); 2, Barclay et al. (2020); 3, Cashin (2014); 4, Dickinson and Carey (2017); 5, Diminic et al. (2019); 6, Furst et al. (2018); 7, Gillieatt et al. (2018); 8, Hancock et al. (2017); 9, Hayes et al. (2018); 10, Horsfall et al. (2018); 11, Isaacs et al. (2018); 12, Kay and Kendall (2017); 13, Maker et al. (2017); 14, Malbon et al. (2019); 15, McGorry and Hamilton (2016); 16, Mellifont (2017); 17, Mulder (2017); 18, New South Wales Nurses’ Association (2019); 19, Pereira et al. (2020); 20, Reppermund et al. (2018); 21, Rosenberg (2017); 22, Rosenberg et al. (2019); 23, Salvador-Carulla and Einfeld (2014); 24, Schweizer et al. (2018); 25, Simpson et al. (2016); 26, Stewart et al. (2018); 27, Trollor (2014); 28, Williams and Smith (2014).
Discussion
This scoping review was undertaken to map the current peer-reviewed literature about the NDIS and people with psychosocial disability. A total of 28 publications were identified.
Peripheral comments about the NDIS and people living with psychosocial disability were found across a diversity of literature, reflecting the wide, substantial impact NDIS is already having and is predicted to have across the mental health service system and beyond. However, the current study evidences a poverty of peer-reviewed literature focused specifically on NDIS for people living with psychosocial disability and an absence of peer-reviewed empirical evaluations of NDIS for this population.
Of the eight publications focused specifically on the NDIS, only one publication (Barclay et al., 2020) explored the experiences of NDIS participants themselves and only two of these participants had a psychosocial disability. Equally, there was an absence of exploration of family member experiences or perspectives. There was a noteworthy absence of literature representing the lived experiences of those in rural/regional/remote settings, Aboriginal and Torres Strait Islander, LGBTQIA and linguistically diverse people, despite the unique and additional needs of these communities (Heneker et al., 2017; Kaplan and McGrath, 2018; Smith-Merry et al., 2018; Somerville et al., 2017).
In 2015, the NDIA published its ‘Co-design framework’ (National Disability Insurance Agency, 2015) heralding its commitment to co-designing the scheme and evaluating NDIS in genuine partnership with service users and their families. If people with a psychosocial disability are playing an authentic and meaningful role in contributing to the design and evaluation of NDIS, and if the Scheme is to develop in line with their needs, it would be expected that the evidence and perspectives of participants and their families would be more prevalent in the peer-reviewed literature.
There was no reporting of empirical evaluations of the impacts and outcomes of NDIS. Although still recent, the NDIS is a major financial investment that has now been operating for 6 years and is anticipated to be at full ‘rollout’ this year. Rather than NDIS focused publications reporting on evaluations of population or Scheme specific data, the most dominant perspective or ‘voice’ across this literature was the opinion of authors themselves. While there are a number of commissioned reports on the NDIS that do focus in varying degrees on psychosocial disability (e.g. Kaplan and McGrath, 2018; Smith-Merry et al., 2018; Tune, 2019), these have not been subjected to the rigour of peer review. The absence of an independent and robust examination of this major mental health initiative parallels other Australian investments in large psychosocial programmes such as the Better Access Scheme introduced in 2006 that was based on limited evidence and poorly evaluated (Jorm, 2011, 2018). The National Mental Health Commission (2014) described the mental health system’s ‘failure to harness knowledge, as well as [learn] from previous reform attempts’ (p. 14).
When robust evaluations of psychosocial initiatives have been funded, and positive evidence harnessed, that evidence has not always be used to inform practice. A national evaluation of PIR (Wallace et al., 2015: 1) found emerging evidence that it was an ‘effective … innovative model … delivering transformational change for many clients with severe and persistent mental illness’. Nonetheless, the programme was discontinued in order to allocate funding to the NDIS.
Future lines of inquiry should be informed by the themes drawn from the qualitative analysis completed in this project and reported in Table 1. While current strengths and weaknesses were identified, the literature predominantly focused on the future opportunities the Scheme could provide for improving economic, social and health outcomes (Isaacs et al., 2018; Kay and Kendall, 2017; Mellifont, 2017) and the possible threats to the Scheme working effectively for people with psychosocial disability.
Major themes emerging from the analysis related to the flow on impact of the NDIS on the broader health and social service systems. While some highlighted the opportunities for enhanced integration of the service system (Cashin, 2014; Isaacs et al., 2018; Mulder, 2017), many spoke of the inherent weaknesses associated with a lack of clear distinction between what was to be provided through existing services and what was to be provided through the NDIS, especially for people with complex needs and co-occurring conditions (Bonyhady, 2014; Reppermund et al., 2018; Simpson et al., 2016; Trollor, 2014). Additionally, many publications spoke of a multitude of threats to the community-managed mental health system, including loss of qualified staff, casualisation, threats to financial viability, lack of access to services for rural and remote communities and loss of services for individuals not eligible for NDIS (Furst et al., 2018; Malbon et al., 2019; Rosenberg et al., 2019). Commissioned reports evidence that some established services have not survived, and others have adapted by changing business models and reducing services (Smith-Merry et al., 2018) but the broader aim of achieving an integrated services system goes beyond the NDIA and requires cooperation between NDIA, NDIS-funded services and various government and non-government services to enable seamless referral pathways between mental health services, employment, family, education, housing and primary care services.
Other themes related to the NDIS itself. An inherent weakness of the NDIS was the disconnect between the language of ‘recovery’ and ‘hope’ promoted within the mental health system (Leamy et al., 2011) and the language of ‘disability’ and ‘permanence’ used within the Scheme (Barclay et al., 2020; Furst et al., 2018; Horsfall et al., 2018). This was described as potentially distressing and considered an obstacle to Scheme access, as many individuals do not view their conditions as ‘permanent’ or a ‘disability’.
The arduous system for application and meeting eligibility requirements of the Scheme was identified as a weakness. Limited NDIA understanding of psychosocial disability and a lack of support and advocacy services to assist with the application process threaten equity of access to the Scheme (Dickinson and Carey, 2017; Furst et al., 2018; McGorry and Hamilton, 2016; Rosenberg, 2017; Williams and Smith, 2014).
Threats were also identified for people with psychosocial disability once they had been accepted into NDIS. These included inappropriate plans developed by planners with limited understanding of psychosocial disability; lack of flexibility within plans that failed to recognise the episodic nature of severe and persistent mental illness; a focus on core supports (i.e. ‘maintenance’) rather than capacity building (i.e. growth and recovery); and a potential lack of access to appropriate services that could provide required supports, especially for regional and remote communities, Aboriginal Australians and people with co-occurring conditions (Barclay et al., 2020; Furst et al., 2018; Horsfall et al., 2018; Maker et al., 2017; Rosenberg, 2017; Simpson et al., 2016; Williams and Smith, 2014).
Significant work is currently being undertaken by the NDIA in attempt to address some of these issues or threats. For example, they have developed an information sheet articulating an alignment between recovery and the NDIS (National Disability Insurance Scheme, 2019d) and are currently developing an NDIS Recovery Framework and establishing the role of ‘Recovery Coaches’ (National Disability Insurance Scheme, 2020). User-friendly resources are now available attempting to demystify the application process, and templates have been developed to support professionals to more easily document NDIA required evidence of ‘psychosocial disability’ (National Disability Insurance Scheme, 2019b). Other recent initiatives include appointments of NDIS assessment and planning staff with specialist psychosocial expertise, intentions to increase flexibility of people’s personalised plans (Fletcher and Henderson, 2018) and revisions to pricing schedules with the aim to enable and support access to remote and regional services (National Disability Insurance Scheme, 2019a). The new NDIS Quality and Safeguards Commission is charged with monitoring service quality. However, there is no apparent plan for the evaluation of the effectiveness or impact of these many new initiatives.
The multitude of themes detailed in Table 1, some of which are discussed above, are a synthesis of expressed hopes for the potential of the NDIS and warnings about the risks of the Scheme to fail to meet or align with the needs of people living with psychosocial disability. These themes align with issues raised in other reports into the NDIS in relation to individuals with severe and persistent mental illness. Collectively they provide a rich foundation from which to focus future lines of critical enquiry.
The NDIS is a very major national investment and, if operating as promised, could improve people’s capacity to live a full and valued life with hope, meaning and recovery (Isaacs et al., 2018). Outcomes for people with psychosocial disability may be enhanced such as increasing employment and reducing hospital admissions, homelessness and involvement with the criminal justice system (Isaacs et al., 2018; Kay and Kendall, 2017; Mellifont, 2017). However, more research is urgently required. To date, there is no comprehensive evaluation of outcomes achieved by NDIS participants with a psychosocial disability. While some data on participant outcomes are available (National Disability Insurance Scheme, 2019c), the following steps would help to address the gaps identified in this review: (a) development of a national psychosocial disability and NDIS research agenda, (b) discrete funding set aside for independent research activity, (c) national NDIS data made available for independent interrogation and (d) ensure the dataset is able to be linked with data from other sectors (e.g. health and housing) so that the broader impact of NDIS can be evaluated. Finally, NDIA needs to continue to seek out evidence from, and be responsive to, the needs and values of people with psychosocial disability and those who support them. While the individualised nature of each person’s needs and thus their NDIS plans makes research and evaluation challenging, it is essential that we understand whether NDIS plans ultimately have an impact on the lives of programme participants and to ensure this very large investment is delivering value for money.
Conclusion
The role of a scoping review is to synthesise a body of literature, identify areas where further research is needed and to consider implications for policy and practice (Tricco et al., 2016).
This scoping study revealed a paucity of research into the NDIS for people living with psychosocial disability and has highlighted some key research priorities, such as the need for more in-depth exploration of the lived experiences of participants of the NDIS with a psychosocial disability and their families. It identified internal problems with the Scheme that are yet to be rectified. While new initiatives have been proposed or recently implemented to address these problems, they are yet to be evaluated.
This review also identified systemic problems beyond the NDIS that can only be tackled with social, health, housing and employment sectors and the NDIA all working together in an integrated and coordinated manner. This will require the NDIA to provide researcher access to data and support data linkage with other service sectors such as health and housing. There is a need for a clear research agenda, access to quality data from NDIA and funding to facilitate robust independent research.
Rigorous, independent research and reporting is needed to ensure NDIS improves and delivers on its vision to enhance the lives of all Australians with disability, including people living with psychosocial disability as well as to examine the impact of NDIS on the overall mental health service landscape.
Supplemental Material
Supplemental_Table_-_Charted_data_(1) – Supplemental material for The National Disability Insurance Scheme and people with severe and persistent mental illness/psychosocial disability: A review, analysis and synthesis of published literature
Supplemental material, Supplemental_Table_-_Charted_data_(1) for The National Disability Insurance Scheme and people with severe and persistent mental illness/psychosocial disability: A review, analysis and synthesis of published literature by Debra Hamilton, Nicola Hancock, Justin Newton Scanlan and Michelle Banfield in Australian & New Zealand Journal of Psychiatry
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
