Abstract

To the Editor
Niemann–Pick type C (NPC) is a genetic neurodegenerative lysosomal storage disorder with highly variable symptoms and age at onset. Although rare, it is of relevance to psychiatrists, as highly frequent symptoms in adolescents and adults include psychiatric symptomatology (e.g. psychosis in 62%), altered behaviour (52%) and cognitive symptoms (90%) (Bonnot et al., 2018). Many of these, despite often having features atypical for primary psychiatric illness, are non-specific and challenging to assess in the context of psychosis and behavioural disturbance. Therefore, initial misdiagnosis as a primary psychiatric illness does not infrequently occur, with accurate diagnosis coming only after development of frank neurological symptoms such as dystonia or ataxia (although these may also be misattributed to a psychiatric disorder and/or treatment). Misdiagnosis and diagnostic delay have significant negative implications, especially since treatments are available for NPC. As for many psychiatric and neurological disorders, there is a need for biomarkers for early diagnosis and to aid in differential diagnosis, prognostication and treatment response. Neurofilament light chain (NfL), as a biomarker of neuronal injury that can be measured in cerebrospinal fluid (CSF) and blood, has shown great promise in diagnosis and differential diagnosis of a range of psychiatric and neurological disorders (Eratne et al., 2019). To our knowledge, NfL has not been explored in NPC.
We report on three patients with genetically confirmed NPC who had CSF NfL measured using commercially available enzyme-linked immunosorbent assay (NF-light; UmanDiagnostics, Umea, Sweden). As demonstrated in Table 1 and Figure 1, patients with NPC had statistically significantly elevated CSF NfL levels compared to (older) healthy controls (HC; Kruskal–Wallis, p = 0.00189) and psychiatric disorders (PSY; most with schizophrenia, bipolar and major depressive disorders, p = 0.00768). NfL perfectly distinguished NPC from HC and NPC with areas under the curve of 1 (695 pg/mL cut-off for NPC vs HC, 1234 pg/mL for NPC vs PSY). One patient with severe psychotic symptoms, ataxia and multiple falls had a follow-up level at 9 months after commencing intrathecal cyclodextrin treatment. She had a significant clinical response with dramatic improvements in her psychosis and ataxia, with no further falls. Her CSF NfL level also significantly decreased over this period, essentially halving and returning to levels similar to those of HC.
Demographics.
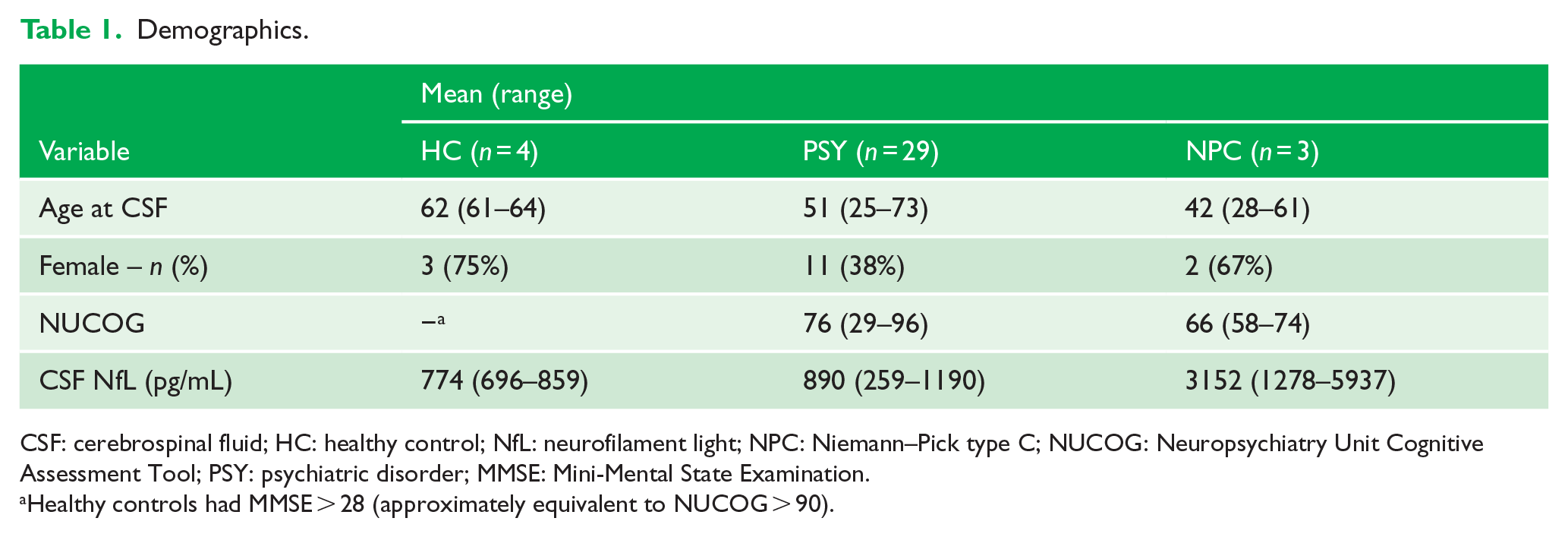
CSF: cerebrospinal fluid; HC: healthy control; NfL: neurofilament light; NPC: Niemann–Pick type C; NUCOG: Neuropsychiatry Unit Cognitive Assessment Tool; PSY: psychiatric disorder; MMSE: Mini-Mental State Examination.
Healthy controls had MMSE > 28 (approximately equivalent to NUCOG > 90).
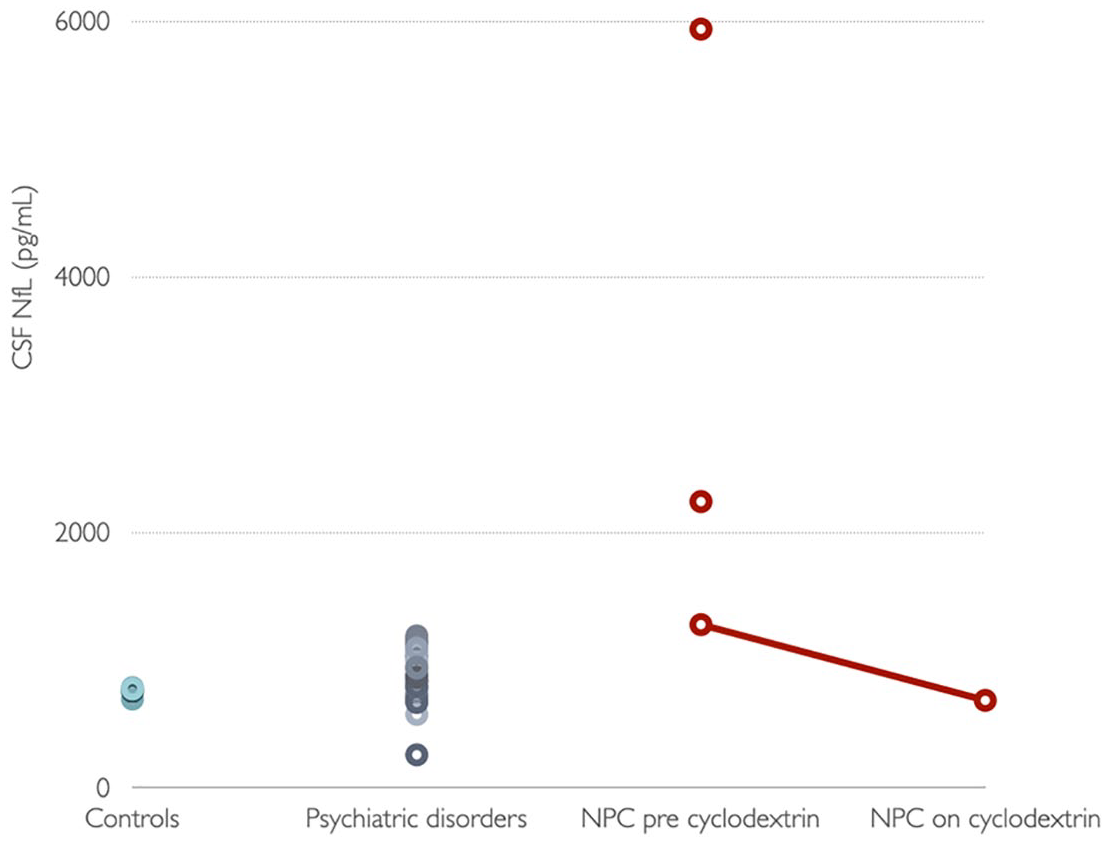
Cerebrospinal fluid neurofilament levels in healthy controls, psychiatric disorders, Niemann–Pick type C precyclodextrin and on cyclodextrin.
These preliminary data suggest diagnostic utility of CSF NfL in differentiating PSY from NPC. Furthermore, data from one patient may also point to NfL as a marker of treatment response in NPC. A significantly elevated NfL level in a patient with a primary psychiatric diagnosis should prompt a quick review of symptoms and consideration of neurological and neurodegenerative differential diagnoses. Although NfL is a non-specific marker of neuronal injury, this is a strength for a potential screening test for broad neurological/neurodegenerative differential diagnoses, thus allowing for precision medicine approaches to further, more specific and costly investigations, leading to reduced misdiagnosis, diagnostic delay and improved outcomes. For example, more specific biomarkers for NPC such as oxysterols are unlikely to be feasible or cost-effective as broad screening tests in psychiatric settings for a rare disorder like NPC; however, following an abnormal NfL and review of symptoms that in a new light raises suspicions for NPC, a more precise use of specific testing such as oxysterols would then be indicated (Patterson et al., 2017). Further studies are warranted of NfL, particularly in blood, which may lead to a simple screening blood test of high utility to psychiatrists, neurologists and general practitioners.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by NorthWestern Mental Health Research Seed Grants. The role of this funding was solely to purchase UmanDiagnosHcs NF-Light ELISA kits, and had no role in the study design, collecHon, analysis or interpretaHon of data, or wriHng of the report.
