Abstract
Objective:
Current nosology conceptualises body dysmorphic disorder as being related to obsessive-compulsive disorder, but the direct evidence to support this conceptualisation is mixed. In this systematic review, we aimed to provide an integrated overview of research that has directly compared body dysmorphic disorder and obsessive-compulsive disorder.
Method:
The PubMed database was searched for empirical studies which had directly compared body dysmorphic disorder and obsessive-compulsive disorder groups across any subject matter. Of 379 records, 31 met inclusion criteria and were reviewed.
Results:
Evidence of similarities between body dysmorphic disorder and obsessive-compulsive disorder was identified for broad illness features, including age of onset, illness course, symptom severity and level of functional impairment, as well as high perfectionism and high fear of negative evaluation. However, insight was clearly worse in body dysmorphic disorder than obsessive-compulsive disorder, and preliminary data also suggested unique visual processing features, impaired facial affect recognition, increased social anxiety severity and overall greater social-affective dysregulation in body dysmorphic disorder relative to obsessive-compulsive disorder.
Conclusion:
Limitations included a restricted number of studies overall, an absence of studies comparing biological parameters (e.g. neuroimaging), and the frequent inclusion of participants with comorbid body dysmorphic disorder and obsessive-compulsive disorder. Risks of interpreting common features as indications of shared underlying mechanisms are explored, and evidence of differences between the disorders are placed in the context of broader research findings. Overall, this review suggests that the current nosological status of body dysmorphic disorder is somewhat tenuous and requires further investigation, with particular focus on dimensional, biological and aetiological elements.
Keywords
The conceptualisation of body dysmorphic disorder (BDD) is an area of increasing research interest, given the recent and controversial classification of BDD within the new chapter of Obsessive Compulsive and Related Disorders in the fifth edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM-5; American Psychiatric Association, 2013). BDD is defined by a distressing preoccupation with a perceived defect in one’s appearance, and performance of excessive or repetitive behaviours or mental acts in response to this preoccupation such as mirror checking and gazing, disproportionate grooming, modification or camouflaging of appearance, and mentally comparing appearance to that of others (American Psychiatric Association, 2013). Despite being relatively common (prevalence of 1.7–2.4% in population estimates; Buhlmann et al., 2010; Koran et al., 2008; Schneider et al., 2017), BDD is often under-recognised (Zimmerman and Mattia, 1998). As such, improving our conceptualisation of the condition might assist in improving clinical awareness and treatment decision-making, and enhance research developments in understanding underlying aetiology.
The currently dominant conceptualisation of BDD as related to obsessive-compulsive disorder (OCD) within an ‘obsessive-compulsive spectrum’ formed the basis for the classification of BDD and OCD in DSM-5 (Hollander et al., 2010). This classification decision was based on assertions of overlap between BDD and OCD in areas of symptom presentation, comorbidity patterns, illness course, familiality, neurobiology, biomarkers, temporal antecedents, and responsiveness to serotonin reuptake inhibitors (Hollander et al., 2008; Phillips et al., 2010). As such, it was hoped that the classification of BDD alongside OCD in DSM-5 would improve clinical awareness and understanding of BDD in accordance with the ‘obsessive-compulsive spectrum’ conceptualisation of the condition (Phillips et al., 2010).
However, the classification of BDD as an Obsessive-Compulsive and Related Disorder has attracted critical debate. In particular, the strength and legitimacy of evidence to indicate a meaningful relationship between BDD and OCD has been questioned, as claims of similarity relied heavily on indirect comparisons with only a handful of direct comparative investigations having been published at the time (Castle and Phillips, 2006; Chosak et al., 2008). In addition, theoretical and empirical problems have been identified in the arguments used to support claims of relatedness between BDD and OCD (Abramowitz and Jacoby, 2015; Castle and Phillips, 2006; Frias et al., 2015). Beyond these concerns, it has been highlighted that BDD has been relatively understudied and that there is a lack of knowledge regarding specific aetiological mechanisms of the disorder.
Since the publication of the DSM-5, there have been considerably more direct comparative investigations of BDD and OCD. These investigations not only contribute to nosological conceptions of BDD, but importantly help elucidate both the core and transdiagnostic features of the disorder. Knowledge of such features is essential for advancing future research into aetiological illness mechanisms and potential treatment pathways (Cuthbert, 2014). As such, this systematic review seeks to synthesise research which has directly compared BDD and OCD, with the goal of delineating unique and shared features of the disorders. This delineation is additionally essential for clarifying the evidence which underpins the current classification of BDD as an Obsessive Compulsive Related Disorder in the DSM-5.
Method
A systematic search of the literature was conducted through the PubMed database, using the search terms: (body dysmorphic disorder OR dysmorphophobia OR dysmorphobia OR muscle dysmorphia) AND (obsessive compulsive disorder OR obsessive-compulsive disorder). Publication dates were inclusive from inception to 29 January 2018. In addition, hand searches through reference lists of included articles and relevant review articles were conducted. Article selection and reporting was conducted according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) protocol (Moher et al., 2009). Eligible articles were required to meet the following criteria: (1) Report original empirical research of direct comparisons between discrete BDD and OCD groups, wherein all participants had a current, confirmed clinical diagnosis. Review articles, meta-analyses, case studies, editorials, and opinion or correspondence letters were excluded. Furthermore, studies of non-clinical participants, sub-clinical BDD and OCD, or unconfirmed BDD or OCD (e.g. self-reported only) were excluded. (2) Written in English language and be published in a peer-reviewed journal (or accepted for publication/in-press, provided the accepted full-text manuscript was available). Article abstracts were screened for relevance, with full-text inspection used to confirm eligibility.
Results
Study selection
The search strategy yielded 379 articles after removal of duplicates. After determining eligibility, 31 articles were selected for inclusion in the review (see Figure 1). A summary of each included article’s sample characteristics, key findings, and methodological strengths and weaknesses is presented in Table 1. As noted in Table 1, several articles appear to have shared a participant sample, but addressed different research questions. Specifically, Didie et al. (2007) and Phillips et al. (2007) appear to have reported on the same participants, as did the three publications of Reese et al. (2010, 2011a, 2011b) and six articles by Toh et al. (2015a, 2015b, 2017a, 2017b, 2017c, 2017d). Where the same information was repeatedly reported across articles with shared samples, only the first mentioning article was cited. After accounting for these duplicate participant groups, we estimate that the selected articles collectively encompass up to 795 unique individuals with BDD and up to 1334 unique individuals with OCD. Several studies also included a third group of individuals with comorbid BDD and OCD (referred to as BDD-OCD hereafter). These comparisons are not reported here, as the results did not contribute to our aims of identifying clear overlaps and differences between the independent diagnostic entities of BDD and OCD. In addition, several studies included individuals with BDD-OCD within BDD and OCD groups. We have noted these studies in the text, as this inclusion may obscure delineation of differences between BDD and OCD.
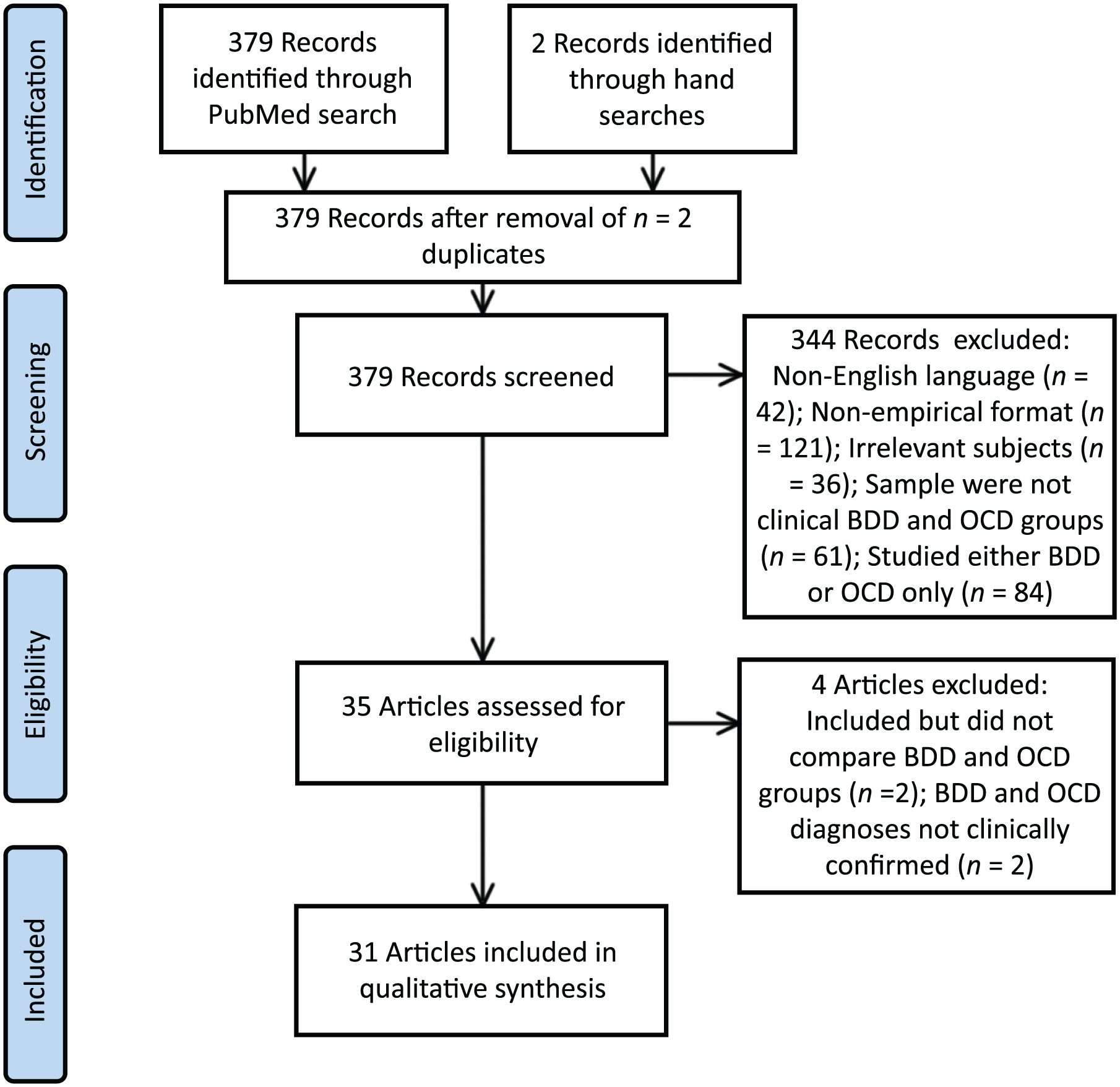
PRISMA flow diagram of systematic search and article screening.
Summary of study groups, key findings, and study strengths and weaknesses for the reviewed studies.
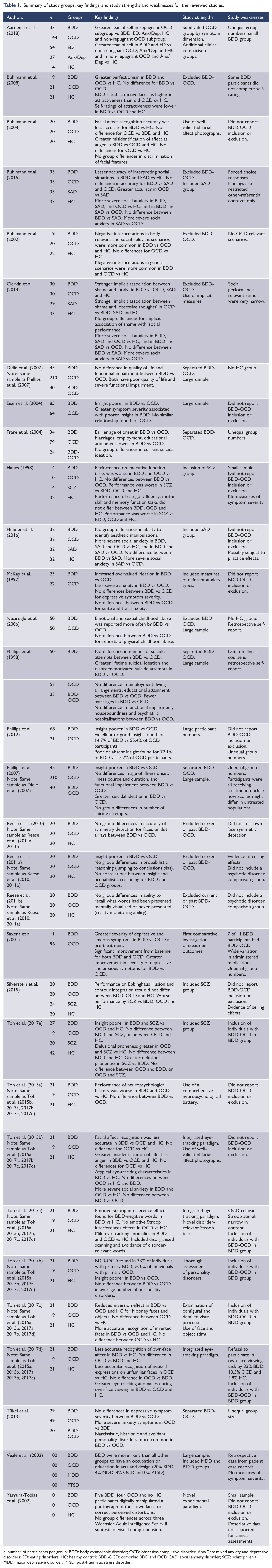
n: number of participants per group; BDD: body dysmorphic disorder; OCD: obsessive-compulsive disorder; Anx/Dep: mixed anxiety and depressive disorders; ED: eating disorders; HC: healthy control; BDD-OCD: comorbid BDD and OCD; SAD: social anxiety disorder; SCZ: schizophrenia; MDD: major depressive disorder; PTSD: post-traumatic stress disorder.
In reporting the results, the data were synthesised into subcategories under the headings of Clinical Characteristics, Phenomenology, and Cognitive Function in accordance with the available evidence. In addition, we calculated and reported Cohen’s d effect sizes for results of group comparisons using reported means and standard deviations, where possible.
Clinical characteristics
Sociodemographics
Of the 22 studies which reported comparisons in one or more sociodemographic areas including marital status, employment status, educational attainment and estimated IQ, most found broad similarities between BDD and OCD, despite some mixed findings (Aardema et al., 2018; Buhlmann et al., 2002, 2004, 2008, 2015; Clerkin et al., 2014; Didie et al., 2007; Frare et al., 2004; Hanes, 1998; Hübner et al., 2016; McKay et al., 1997; Neziroglu et al., 2006; Phillips et al., 1998, 2007, 2012; Reese et al., 2010, 2011b; Toh et al., 2015a, 2017b, 2017e; Tükel et al., 2013; Veale et al., 2002). Findings of difference included fewer marriages in BDD than in OCD in two of six studies (Frare et al., 2004; Phillips et al., 1998). Mixed results were also reported in two of five comparisons of employment status (Frare et al., 2004; Toh et al., 2017e) and in two of 13 comparisons of educational attainment (Frare et al., 2004; Tükel et al., 2013). In addition, one of four studies reported a higher IQ in BDD relative to OCD (Toh et al., 2017e). Finally, one study found that significantly more BDD participants had an occupation or education in arts and design, relative to OCD, major depression and post-traumatic stress disorder (PTSD) participants; this was interpreted as signalling BDD is associated with a predisposition towards aesthetic occupations (Veale et al., 2002).
Age of onset
Across six studies, the mean age of illness onset ranged between 16 and 18.3 years for BDD and between 14 and 21.2 years for OCD. While one of these studies reported a significantly earlier mean age of onset for BDD relative to OCD (d = 0.52; Frare et al., 2004), the remaining five found no significant differences in the mean age of illness onset between the two disorders (d range = 0.06–0.40; Neziroglu et al., 2006; Phillips et al., 1998, 2007, 2012; Tükel et al., 2013). In addition, one study found no significant differences in mean age of subclinical BDD and OCD symptom onset (d = 0.17), which was reported as 11.9 years (standard deviation [SD] = 8.2) in BDD and 13.1 years (SD = 5.2) in OCD (Phillips et al., 2007). Overall, these results demonstrate strong similarity in the mean ages of BDD and OCD onset.
Illness course
A retrospective study of illness course found generally similar patterns between BDD and OCD participants (free of BDD-OCD), with some exceptions (Phillips et al., 1998). Gradual illness onset was predominant in both groups (76% BDD, 71% OCD), while acute onset was reported by approximately a quarter of each group. Both groups also largely exhibited a chronic, continuous illness course (92% BDD, 96% OCD) rather than episodicity. However, individuals with BDD were significantly more likely than those with OCD to report their illness had worsened with time (62% BDD, 36% OCD), while a significantly higher proportion of the OCD group reported a stable illness course (16% BDD, 51% OCD).
Treatment response
Only one study has reported on treatment response in BDD and OCD groups (Saxena et al., 2001). No significant differences were present in pre-treatment illness severity (d = 0.38), but depressive and anxious symptoms were significantly more severe in the BDD group than in the OCD group (d = 0.98, 0.92). After a 6-week multimodal treatment intervention, both groups had improved significantly across all baseline measures, with no significant group differences in post-treatment illness severity (d = 0.20) and depressive and anxious symptom severity (d = 0.13, 0.17). However, the findings of this study may be more relevant to the treatment of OCD and BDD-OCD than BDD, as 7 of the 11 BDD participants had BDD-OCD. Furthermore, the BDD group (n = 11) was relatively small compared to the OCD group (n = 96).
Primary symptom severity
Across eight studies which compared BDD and OCD symptom severity using disorder-specific measures, none reported significant between-group differences (d range = 0.01–0.05), with qualitative inspection revealing mean scores in the moderate-to-severe range for both groups across all studies (Didie et al., 2007; Eisen et al., 2004; Frare et al., 2004; Phillips et al., 1998, 2007, 2012; Toh et al., 2015a, 2017e). All studies used the analogous Yale Brown Obsessive Compulsive Scale (YBOCS) for OCD participants and the YBOCS Modified for BDD (BDD-YBOCS) for BDD participants. Severity scores on the thought and behaviour subscales of the YBOCS and BDD-YBOCS were further examined in two studies, both of which found no difference between BDD and OCD in the severity of symptomatic behaviours (d = 0.16, 0.19; Eisen et al., 2004; Phillips et al., 2012). However, Phillips et al. (2012) reported significantly greater severity of symptomatic thoughts in OCD than BDD (d = 0.50), while Eisen et al. (2004) found no group differences in this respect (d = 0.21).
Insight
All eight studies which examined illness insight found significantly poorer insight in BDD than in OCD, with very large effect sizes (d range = 1.45–3.86; Eisen et al., 2004; Phillips et al., 2007, 2012; Reese et al., 2011a; Silverstein et al., 2015; Toh et al., 2017c, 2017e). All but one of these studies used the well-validated Brown Assessment of Beliefs Scale (BABS; Eisen et al., 1998) to measure insight, with McKay et al. (1997) employing the Overvalued Ideas Scale (McKay et al., 1997; Neziroglu et al., 1999). Phillips et al. (2012) also demonstrated significant group differences in the distribution of insight scores, with the majority of BDD participants demonstrating poor or absent insight (72% BDD, 16% OCD), and the majority of OCD participants demonstrating good or excellent insight (55% OCD, 15% BDD). Interestingly, Toh et al. (2017e) further found similar levels of insight among BDD participants and a schizophrenia/schizoaffective disorders group (d = 0.24) and significantly better insight in OCD relative to the schizophrenia/schizoaffective group (d = 1.38).
Propensity for delusional thinking styles
Two studies found no significant differences between BDD and OCD for propensity to engage in broadly unusual thinking styles (d range = 0.31–0.58; Silverstein et al., 2015; Toh et al., 2017e), as measured by the Peters Delusional Inventory (Peters et al., 1999). Toh et al. (2017e) additionally found significantly higher scores for unusual thinking style in OCD relative to healthy controls (d = 1.40), with no difference between OCD participants and a schizophrenia/schizoaffective group (d = 0.40; Toh et al., 2017e). Conversely, similar scores were found for BDD relative to controls (d = 0.68), with BDD demonstrating significantly lower scores than the schizophrenia/schizoaffective group (d = 0.94). These results suggest BDD and OCD may have similar, yet differently graded positions on a continuum of propensity for unusual thinking styles.
Depressive symptoms
Depressive symptoms appear to be broadly comparable across BDD and OCD, as 10 of 14 studies reported no significant differences in depressive symptom severity between BDD and OCD groups (d range = 0.20–0.50; d could not be calculated for one study; Buhlmann et al., 2015; Clerkin et al., 2014; Hanes, 1998; Hübner et al., 2016; McKay et al., 1997; Phillips et al., 2007; Reese et al., 2011b; Toh et al., 2015b; Tükel et al., 2013; Yaryura-Tobias et al., 2002). However, the remaining four studies reported significantly more severe depressive symptoms in BDD than in OCD, with large effect sizes (d range = 0.92–1.16; Buhlmann et al., 2002, 2004, 2008; Saxena et al., 2001); although it should be noted that one of these studies included seven BDD-OCD participants in the small BDD group (n = 11), which may have contributed to findings of elevated depressive symptoms in the BDD group (Saxena et al., 2001). Qualitative inspection of group means reported by all 14 studies demonstrated that depressive symptoms were generally of mild-to-moderate clinical severity for both BDD and OCD groups.
Generalised anxiety symptoms
Mixed findings were reported across the four studies which compared generalised anxiety symptoms. The largest of the four studies reported no significant differences between BDD and OCD for severity of anxiety symptoms (d = 0.61; Tükel et al., 2013). Two smaller studies reported significantly more severe anxiety in OCD than in BDD (d = 0.41, unable to calculate d for one study; McKay et al., 1997; Yaryura-Tobias et al., 2002). By contrast, Saxena et al. (2001) reported significantly more severe anxiety in BDD than in OCD (d = 0.98; although high rates of BDD-OCD in the BDD group may have influenced this finding). Qualitative inspection of group means across all four studies revealed that anxiety symptoms were in the mild-to-severe ranges for both groups. In sum, the results might support somewhat elevated generalised anxiety symptoms in OCD versus BDD but are inconclusive at present.
Two investigations of fluctuating and dispositional anxiety using the State-Trait Anxiety Inventory (Spielberger et al., 1983) also demonstrated mixed results. The larger study (n = 30 per group) of participants free of BDD-OCD manifested significantly greater state (d = 0.68) and trait (d = 0.48) anxiety in BDD than in OCD (Clerkin et al., 2014). However, the smaller study of McKay et al. (1997) reported no BDD versus OCD differences in state (d = 0.39) or trait (d = 0.29) anxiety. Across both of these studies, symptom scores fell within moderate-to-severe severity ranges for both groups.
Social anxiety symptoms
Although mixed findings were reported across four studies of social anxiety severity, the overall data indicate greater severity of social anxiety symptoms in BDD than in OCD. Two of the four studies found significantly more severe social anxiety in BDD than in OCD, with medium-to-very large effect sizes (d = 0.57, 1.08; Buhlmann et al., 2015; Clerkin et al., 2014), while the remaining two studies reported no significant differences between BDD and OCD groups (d = 0.24, 0.57; Hübner et al., 2016; Toh et al., 2015b). In all four studies, comparisons to controls demonstrated significantly greater social anxiety severity in both BDD (d range = 1.05–2.48) and OCD (d range = 0.81–1.37). However, further comparisons to a primary social anxiety disorder (SAD) group in three of these studies showed no significant differences between BDD and SAD (d range = 0.36–0.39; Buhlmann et al., 2015; Clerkin et al., 2014; Hübner et al., 2016). By contrast, social anxiety severity was significantly lessened in OCD relative to the SAD group across all three of these studies (d range = 0.95–1.54).
Childhood maltreatment
A single study of 50 BDD and 50 OCD participants free of lifetime BDD-OCD found that those with BDD made significantly more reports of childhood sexual (22% vs 6%) and emotional (28% vs 2%) abuse than OCD participants (Neziroglu et al., 2006). Conversely, similar proportions of both groups (14% BDD vs 8% OCD) reported childhood physical abuse. However, the absence of a healthy control group in this study prevents comparison of these abuse rates to those of a non-clinical population, thus rendering these findings inconclusive.
Functional impairment
The largest and most comprehensive of five studies of functional impairment reported that both BDD and OCD were associated with significant functional impairment and poor quality of life across many domains, including interpersonal, recreational, academic, occupational, role functioning, and psychological and physical health (Didie et al., 2007). Similarly, the remaining four studies variously demonstrated that both disorders encompass similarly high rates of global functional impairment, psychiatric hospitalisations (e.g. 58% BDD, 51% OCD), being housebound (e.g. 31% BDD, 32% OCD) and mental health disability status (17.8% BDD, 15.7% OCD; Neziroglu et al., 2006; Phillips et al., 1998, 2007; Saxena et al., 2001).
Suicidality
Data from four studies demonstrated mixed findings regarding levels of suicidal ideation and history of suicide attempts between BDD and OCD. Lifetime generalised suicidal ideation (i.e. ideation not specifically linked to BDD/OCD symptoms) was more often reported by BDD than OCD participants in one study (78% BDD, 55% OCD; Phillips et al., 2007). Conversely, a second study reported no differences between BDD and OCD for severity of current generalised suicidal ideation (27% BDD, 20% OCD; Frare et al., 2004). Regarding suicidal ideation specifically linked to BDD and OCD symptoms, one study found that significantly more BDD than OCD participants reported suicidal ideation (70% BDD, 47% OCD; Phillips et al., 1998), while another study found no group differences in this respect (62% BDD, 44% OCD; Phillips et al., 2007). In terms of suicide attempts, two studies found no significant differences in the proportion of BDD (13–29%) and OCD (16–19%) participants who reported prior suicide attempts (Phillips et al., 1998, 2007). However, Phillips et al. (1998) reported that significantly more BDD (22%) than OCD (8%) participants cited their disorder as the primary impetus for having attempted suicide.
Comorbidities
Studies of comorbidity have found that BDD and OCD are similar in the overall number of comorbid psychiatric conditions. Toh et al. (2015a) reported no significant differences for the average number of any current comorbid psychiatric disorder per participant between BDD and OCD groups (BDD M = 2.8, SD = 1.6, OCD M = 1.7, SD = 1.1), nor for the average number of personality disorders per participant between BDD and OCD groups (BDD M = 1.4, SD = 1.4, OCD M = 1.1, SD = 1.6). Similarly, Neziroglu et al. (2006) reported no differences in the proportion of BDD and OCD patients who had at least one currently comorbid psychiatric disorder (78% BDD, 62% OCD).
The prevalence of specific comorbid disorders within BDD and OCD groups has been statistically examined across four studies, with mixed findings (Frare et al., 2004; Phillips et al., 1998, 2007; Tükel et al., 2013). The surveyed disorders included major depressive disorder (MDD), bipolar I and II, dysthymic disorder, SAD, panic disorder, generalised anxiety disorder, specific phobia, anorexia nervosa (AN) or bulimia nervosa, alcohol or substance use disorder, and somatoform disorders. While results were generally mixed across these studies, a higher prevalence of MDD in BDD than in OCD was found in two studies, as were higher rates of alcohol and substance use disorders (Frare et al., 2004; Phillips et al., 1998, 2007). One study further reported higher rates of SAD and psychotic disorders in BDD than in OCD, although the elevated rate of psychotic disorders may be explained by the outmoded Diagnostic and Statistical Manual of Mental Disorders (4th ed.; DSM-IV) method of double-coding delusional BDD as a psychotic disorder (Phillips et al., 1998). Generalised anxiety disorder was more common in OCD than in BDD in one study (Frare et al., 2004), and conflicting results were found across two studies for the prevalence of dysthymic disorder. However, the remaining comparisons variously demonstrated no significant differences between BDD and OCD across these disorders. In terms of comorbid personality disorders, Tükel et al. (2013) found a significantly greater prevalence of narcissistic, histrionic and avoidant personality disorders in BDD than in OCD. In addition, Tükel et al. (2013) further reported that individuals with BDD were more likely than those with OCD to have a personality disorder, especially Cluster B personality disorders. Phillips et al. (2007) reported a significantly greater prevalence of paranoid personality disorder in BDD than in OCD, but no further differences. In sum, the available data regarding the prevalence of specific comorbidities among BDD and OCD provide no conclusive evidence of similarity or difference in terms of comorbidity patterns between the disorders.
Finally, results from one study indicate that there is a higher rate of comorbid OCD within primary BDD, than vice versa. Toh et al. (2017b) found comorbid lifetime and current OCD in 33% and 23.8% of the primary BDD group, respectively. Conversely, there was no incidence (0%) of lifetime or current BDD in the OCD group.
Phenomenology
Fear of self
A recent investigation of feared self-perceptions using the Fear of Self Questionnaire (Aardema et al., 2013) demonstrated complex positioning of BDD relative to specific subtypes of OCD (Aardema et al., 2018). Initial assessment of OCD participants in this study found significantly greater fear of self in individuals with personally repugnant obsessions (e.g. moral, sexual, religious, aggressive) than in those with personally non-repugnant concerns (e.g. contamination, checking, ordering and arranging, somatic, or other, d = 1.05). Comparison of the repugnant and non-repugnant OCD subgroups to the BDD group revealed significantly greater fear of self in repugnant-OCD versus BDD (d = 0.58), and in BDD versus non-repugnant OCD (d = 0.52). Interestingly, a mixed eating disorders (ED) group demonstrated the same patterns as BDD; that is the ED group and BDD did not significantly differ (d = 0.15), and the ED group shared the same pattern of significant differences as BDD relative to both OCD subgroups. Finally, fear of self was significantly greater in all clinical groups relative to healthy controls, with very large effect sizes (d range = 1.01–2.1).
Facial attractiveness judgements
The only published study of facial attractiveness judgements found significant differences between BDD and OCD in ratings of attractive faces and in ratings of own attractiveness (Buhlmann et al., 2008). While BDD, OCD and control participants each gave similar classifications of faces as ‘average’, ‘attractive’ or ‘unattractive’, BDD participants gave significantly higher ratings of attractiveness to the attractive faces than did OCD (d = 1.04) or control participants (d = 1.19). Furthermore, BDD participants gave themselves significantly lower ratings of attractiveness than did the OCD (d = 0.81) and control participants (d = 0.89), despite all three groups placing themselves within an ‘average’ attractiveness range. In a subset of participants who allowed their image to be rated by independent evaluators (n = 13/19 BDD, 16/21 OCD and 19/21 controls), only the BDD participants’ ratings were significantly lower than those of independent evaluators. Importantly, the independent evaluators gave similar mean ratings to all three groups (d range = 0.00–0.07), which suggests BDD participants’ low self-ratings were attributable to their own self biases rather than any objective unattractiveness.
Perfectionism
A single study reported no significant differences between BDD and OCD in overall perfectionism scores (d = 0.11), with both groups demonstrating significantly higher scores than controls (d = 0.92–0.96; Buhlmann et al., 2008). In sub-dimensions of perfectionism, both clinical groups demonstrated significantly higher scores than controls for ‘doubting of actions’ (OCD d = 2.19; BDD d = 1.15) and ‘concern over mistakes’ (d = 1.35 for both groups). While BDD and OCD did not differ in scores for ‘concern over mistakes’ (d = 0.03), the OCD group scored significantly higher than the BDD group for ‘doubting of actions’ (d = 0.88). No further group differences were found across the remaining sub-dimensions of ‘personal standards’, ‘parental expectations’, ‘parental criticism’ and ‘organisation’.
Shame
A single study investigated implicit associations of shame with the body, intrusive thoughts, and public speaking performance (Clerkin et al., 2014). The BDD group demonstrated significantly stronger implicit associations of shame with the body as compared to OCD, SAD and healthy control participants. Moreover, the OCD group demonstrated significantly stronger implicit associations of shame with intrusive thoughts as compared to all other groups. No group differences were found in the strength of implicit associations between shame and public speaking performance.
Fear of negative evaluation
Of the three studies which compared BDD and OCD using the Brief Fear of Negative Evaluation scale (Carleton et al., 2006), two reported no significant differences between BDD and OCD groups (d = 0.18, 0.70; Buhlmann et al., 2004; Toh et al., 2015a). The third found significantly higher fear of negative evaluation scores in BDD relative to OCD, with a large effect size (d = 0.93; Buhlmann et al., 2002). However, all three studies found that both BDD and OCD demonstrated significantly higher scores than healthy controls, with very large effect sizes (d range = 1.29–2.90). As such, fear of negative evaluation appears to be a prominent concern in both disorders.
Interpretive biases
One study found that BDD participants were significantly more likely than OCD and healthy control participants to interpret ambiguous social and body-focused situations as being personally relevant and threatening (e.g. ‘Others are negatively judging my social performance/bodily appearance’; Buhlmann et al., 2002). However, both the BDD and OCD groups made significantly more negative interpretations of general situations (not involving socialisation or body focus) than did healthy controls, suggesting both clinical groups share a tendency to interpret ambiguous information as threatening (Buhlmann et al., 2002).
Cognitive function
Social cognition
Results from a single study suggested that BDD and OCD overlap yet may subtly differ in social cognitive functioning (Buhlmann et al., 2015). Using the Movie for the Assessment of Social Cognition, this study found no significant differences between BDD and OCD for overall accuracy of social inferences (d = 0.55). However, additional comparisons revealed similarly poor accuracy of social inferences scores in BDD and a group with SAD (d = 0.37), such that both BDD and SAD had significantly poorer scores than healthy controls, with large effect sizes (d = 0.72 and 1.06, respectively). Conversely, no difference was found between OCD and healthy controls (d = 0.14), with significantly greater accuracy scores in OCD than in SAD (d = 0.89).
Attentional biases
A single study found no differences between BDD and OCD in behavioural performance on a disorder-relevant emotional Stroop task, or in eye-tracking data for visual scan strategies used during task performance (Toh et al., 2017a). However, BDD participants demonstrated significant interference effects for BDD-negative words (e.g., ‘ugly’) relative to healthy controls, while no differences were observed between OCD and control participants. Furthermore, eye-tracking analysis showed subtle anomalies in both clinical groups relative to controls, including increased fixations in OCD and decreased visual attention in BDD for BDD-negative and OCD-washing words. Qualitative inspection additionally found disorganised viewing strategies in both clinical groups, which included avoidance of disorder-relevant words. Of note, the OCD-relevant stimuli in this study were restricted to washing and checking words, and therefore these stimuli may have been too narrow to elicit attentional biases from all OCD participants, as not all had washing or checking concerns.
Facial affect recognition
Despite some inconsistencies, data from three studies suggest fine-grained differences in facial affect recognition between BDD and OCD, particularly in relation to healthy controls (Buhlmann et al., 2004; Toh et al., 2015b, 2017d). While Toh et al. (2015b) found significantly impaired affect recognition in BDD relative to OCD using unfamiliar faces (unable to calculate d for this study), no significant group differences were reported by Buhlmann et al. (2004) for the same task (d = 0.41). However, both studies reported significant impairment in BDD relative to healthy controls (d = 0.95), with no differences between OCD and control participants (d = 0.58). Moreover, both studies found that the BDD group misidentified expressions as anger significantly more often than both the OCD (d = 0.59) and control groups (d = 1.12). Using a subset of the same participant sample as Toh et al. (2015b; n = 14/21 BDD, 17/19 OCD, 20/21 control participants), Toh et al. (2017d) further found that accuracy of own-face affect recognition was not significantly different between BDD and OCD participants (d = 0.39). However, comparison to controls demonstrated significantly poorer affect recognition in BDD (d = 0.96), with no differences between OCD and control participants (d = 0.56).
Visual processing of faces
Mixed results were found across four studies of facial visual processing, with some data suggesting abnormal visual scan strategies in BDD relative to OCD. Toh et al. (2015b) found no significant differences between BDD and OCD for visual scan strategies used during the viewing of unfamiliar faces. However, the BDD group demonstrated significantly more disorganised scan strategies than controls, while OCD and controls did not differ. Within a subset of the same sample, Toh et al. (2017d) identified significantly greater anomalies in visual scanning strategies during own-face viewing in BDD relative to both OCD and healthy controls. Conversely, OCD and controls did not differ. In addition, scan strategies of BDD participants with facial preoccupations were qualitatively distinguishable by excess fixation, avoidance or intermittent checking of preoccupying features (Toh et al., 2017d).
Other research found no significant differences between BDD, OCD and healthy control participants on the Benton Facial Recognition Test (d range = 0.08–0.15), indicating no measurable deficits in the foundational processing of facial features (Buhlmann et al., 2004). Finally, another small study (n per group = 10) found five BDD and four OCD participants reported perceived distortions in their own facial photographs when misled by the researchers to believe the images may have been altered (Yaryura-Tobias et al., 2002).
General visual processing
Five studies examined various aspects of visual processing. Of these, one found evidence of greater detailed visual processing in BDD versus OCD (Toh et al., 2017c), while the remainder variously demonstrated no differences between BDD and OCD in aesthetic detection (Hübner et al., 2016; Reese et al., 2010), visual organisation (Silverstein et al., 2015) or visual comprehension (Yaryura-Tobias et al., 2002). In the most recent study, Toh et al. (2017c) investigated configural and detailed (i.e. piecemeal) visual processing using inverted Mooney faces and objects. A significantly reduced inversion effect was found for BDD relative to OCD (d = 0.62) and healthy controls (d = 0.83) for both face and object stimuli, while no significant difference was observed between OCD and controls (d = 0.18). Furthermore, the BDD group was significantly more accurate than the OCD (d = 0.66) and control (d = 0.77) groups in recognising inverted faces, while no difference was found between OCD and controls (d = 0.11). Overall, these findings indicate a greater use of detailed visual processing in BDD than in OCD or controls.
Of two studies of aesthetic awareness, one found no differences between BDD, OCD and healthy control participants for detection of facial symmetry (d range = 0.11–0.22) and dot array symmetry (d = 0.15–0.40; Reese et al., 2010). Similarly, the second study reported no differences between BDD, OCD, SAD and healthy control participants in the detection of subtle aesthetic changes to facial features (d range = 0.13–0.50; Hübner et al., 2016). In terms of visual organisation, Silverstein et al. (2015) found no significant differences between BDD, OCD and healthy control participants in performance on the Ebbinghaus illusion and a contour integration test, with all groups significantly outperforming a schizophrenia group. However, ceiling effects may have occurred in the BDD, OCD and healthy control groups, which could have prevented detection of differences. Finally, the smallest study (n per group = 10) reported no differences between BDD, OCD and healthy control participants on the Picture Completion, Block Design and Matrix Reasoning subtests of the Wechsler Adult Intelligence Scale III, indicating no measurable visual comprehension deficits in BDD or OCD (Yaryura-Tobias et al., 2002). Overall, these studies demonstrate similarity between BDD and OCD in visual processing areas of aesthetic detection, visual organisation and visual comprehension, but clearly indicate enhanced detailed visual processing in BDD versus OCD.
Other neuropsychological domains
Five studies of neuropsychological function indicated broadly similar neurocognitive profiles between BDD and OCD, particularly in domains of executive function. The most comprehensive of these studies utilised the Repeated Battery for the Assessment of Neuropsychological Status (Toh et al., 2015a). This study found similar, significant impairment in both BDD and OCD relative to healthy controls across domains of immediate memory and attention, but the three groups did not differ across domains of visuospatial construction, language and delayed memory. In individual tasks, the BDD group was significantly impaired compared to both the OCD and control groups for digit span and story recall, while both the BDD and OCD groups were impaired relative to controls on story memory.
A further study of executive function found similar impairment in BDD and OCD groups relative to healthy controls in performance on the Tower of London Task and the Stroop Interference task, indicating executive dysfunction in both disorders (Hanes, 1998). However, no group differences were found in additional tasks of category fluency, motor skill and memory function. Third, a small study (n = 10 per group) reported no differences between BDD, OCD and healthy control participants in performance of the Wisconsin Card Sorting Test, a measure of set-shifting abilities (Yaryura-Tobias et al., 2002). Finally, two studies of cognitive reasoning found no differences between BDD, OCD and healthy control participants in reality monitoring (Reese et al., 2011b) or in the presence of a ‘jumping to conclusions’ bias for probabilistic reasoning tasks (Reese et al., 2011a).
Discussion
The objective of this review was to provide a summary of the research to date which has directly compared BDD and OCD, to delineate areas of overlap or divergence between the conditions. The 31 reviewed studies together demonstrated a broad array of findings of various strength, and highlighted areas of overlap, areas of difference, and mixed or unclear findings, as depicted visually in Figure 2. These interpretations were based on consistency of results across studies, calculated effect sizes for available comparisons and consideration of study strengths and weaknesses. However, given the small number of reviewed studies and other limitations of the review, these interpretations are necessarily tentative.
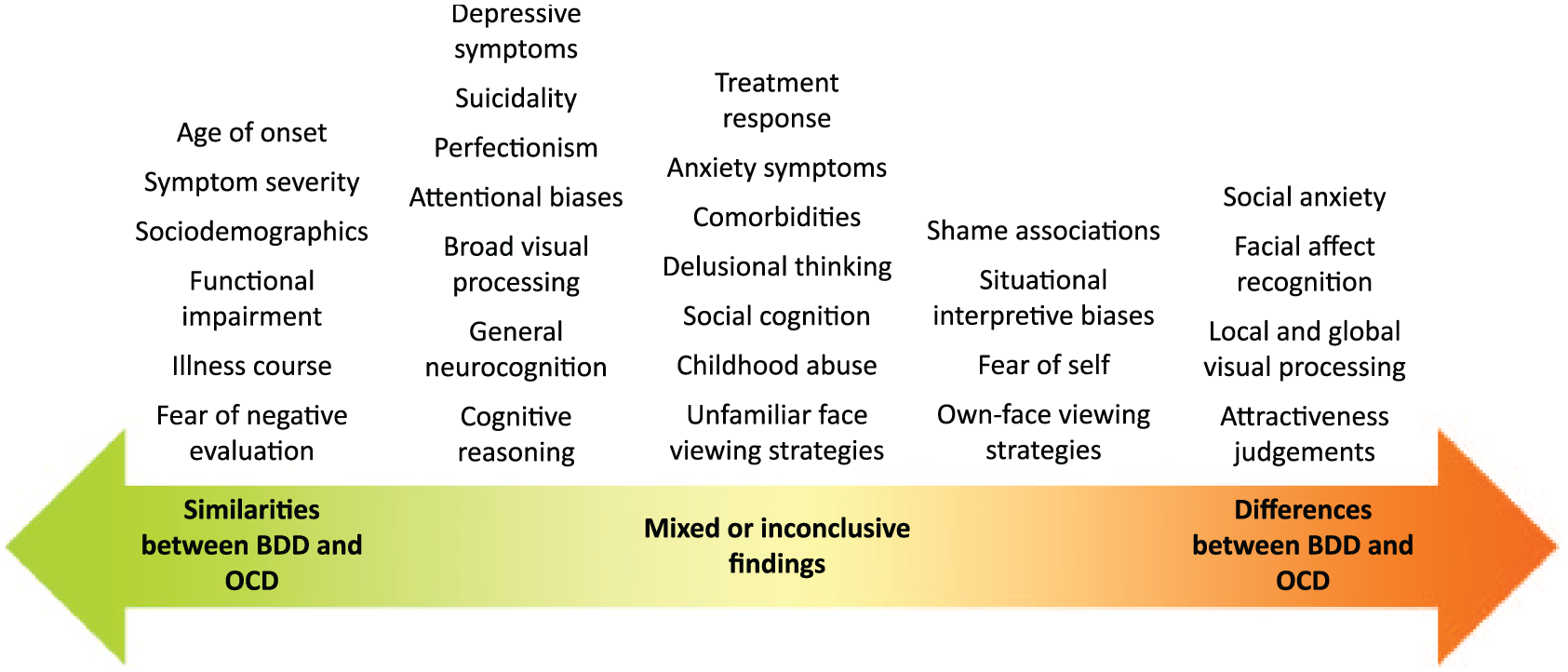
A visual depiction of conclusions regarding similarities and differences between BDD and OCD, and areas of mixed or inconclusive findings. Conclusions were made on the basis of author agreement after taking into account the consistency of findings across studies, individual study strengths and weaknesses, and calculated effect sizes for group comparisons (where available).
Areas of convincing overlap between BDD and OCD as supported by convergent findings include sociodemographic features (e.g. marital status, employment status and educational attainment), average age of onset and illness course, severity of primary symptoms, functional impairment and fear of negative evaluation. Possible overlaps, as indicated either by single studies or partially inconsistent findings across multiple studies, include the severity of depressive symptoms, perfectionism, disorder-relevant attentional biases, normal general visual processing and similarly broad yet mild impairments in neuropsychological function.
Conversely, poor illness insight in BDD relative to OCD emerged as the starkest and most well-supported area of difference. Further probable differences, although supported by fewer studies or partially inconsistent findings, included association of BDD with greater social anxiety severity, biased facial affect recognition, greater detailed visual processing, unique facial attractiveness judgements, shame associations and interpretive biases, and disorganised visual scan strategies used during own-face viewing. In addition, mixed evidence of finely gradated differences within broader similarities between BDD and OCD emerged in areas of proneness to delusional thinking, fear of self, social cognition and visual scan strategies for unfamiliar faces. Finally, some research areas had a paucity of findings or mixed results and thus are inconclusive at present. These areas include treatment response, anxiety symptom severity, suicidality, childhood experiences of abuse and patterns of comorbidities between BDD and OCD.
Overlaps between BDD and OCD
The strongest evidence of similarity between BDD and OCD suggests that the conditions share a general illness template of severe and intractable mental illness, as characterised by moderate-to-severe symptom severity, illness onset in adolescence or young adulthood, a chronic and continuous illness course, and substantial functional impairment with poor quality of life. Similarities in these features may indicate broad overlaps in patterns of illness manifestation between BDD and OCD, but they do not necessarily signify analogous underlying mechanisms are present in both disorders. For example, despite similarity in the overall mean age of BDD and OCD onset, significant sex differences in the mean age of OCD onset have been identified (i.e. significantly earlier for males than females; Ruscio et al., 2010). Conversely, the mean age of BDD onset appears similar across the sexes (Phillips et al., 2006), possibly indicating differential biological mechanisms (e.g. sex hormone influenced) may be linked to the development of each disorder. Moreover, contextualisation of these overlaps between BDD and OCD within wider psychopathology demonstrates that a variety of theoretically distinct conditions also share similar symptom severity, age of onset, illness course and associated impairment as BDD and OCD (e.g. dysthymia, SAD, panic disorder, AN and bulimia nervosa, several personality disorders; American Psychiatric Association, 2013). As such, overlaps between BDD and OCD in these areas may not signal a particularly unique relationship between the two disorders, but may reflect similarities across a large cluster of conditions. Study of the mechanisms underlying development of similar general illness features may instead provide clarity in determining meaningful linkages across disorders.
The finding of similar symptom severity scores between BDD and OCD indicates that disorder-specific symptomatic thoughts and behaviours in both disorders are associated with similar experiences of time depletion, distress, interference, irresistibility and involuntariness, as per the parallel nature of YBOCS and BDD-YBOCS items. As such, BDD may share with OCD a fundamental symptom structure characterised by persistent and powerfully compelling thoughts and behavioural urges, although with differing foci regarding cognitions and behaviours. However, a better understanding of the functional elements within this symptom structure is necessary to provide meaningful insights into the disorders, which may be of use in treatment. For instance, empirical identification of a key functional relationship between obsessions and compulsions in OCD (i.e. obsessions trigger anxiety and compulsive urges, compulsions provide anxiety relief) has been instrumental in forming effective cognitive-behavioural treatment models of the disorder (Hodgson and Rachman, 1972; Steven et al., 2011). However, BDD appears to differ from OCD in that symptomatic behaviours (e.g. mirror checking) do not provide distress relief (Veale and Riley, 2001). In addition, burgeoning neurobiological data regarding BDD thus far indicates important differences from OCD in terms of symptom correlates, particularly in alterations of visual system regions and pathways involved in the transfer and integration of cognitive, emotional and visual information in BDD (Beilharz et al., 2017; Grace et al., 2017). As such, further investigation of symptom function and aetiology, rather than form, is essential to enhance our understanding of BDD.
Other overlaps between BDD and OCD were found for perfectionism, fear of negative evaluation and social anxiety severity, though these findings are based on few studies. Although perfectionism is a transdiagnostic feature which contributes to the development and maintenance of a variety of disorders, including depression, anxiety and eating disorders (Egan et al., 2011), it has been identified as a key construct in the cognitive processes of OCD and is theorised to involve similar significance in BDD (Obsessive Compulsive Cognitions Working Group, 1997; Veale, 2004). Perfectionism relating to idealised self-standards may further contribute to a fear of negative evaluation and social anxiousness in both disorders, as well as disorder-specific (i.e. differential) experiences of shame and fear of self. In addition, elevated scores for BDD and OCD in perfectionism sub-dimensions of ‘concern over mistakes’ and ‘doubting of actions’ may further reflect a meaningful overlap between the disorders, as higher scores in these domains have been linked to increasingly severe ‘not just right’ experiences (NJREs; Coles et al., 2003). Elevated NJREs have been found in both BDD and OCD, with more severe NJREs being predictive of greater obsessional tendencies in OCD and non-clinical samples (Belloch et al., 2016; Summers et al., 2017). As such, future comparisons might find that BDD and OCD share similar patterns of interrelationships between these features.
Finally, both BDD and OCD appear to share similar, mild impairments in broad neurocognitive functioning, particularly in executive function. Modest impairments in executive function, processing speed and attention have been previously established in OCD, but questions remain as to whether these alterations have an aetiological role or are sequelae of the condition (Abramovitch et al., 2013; Snyder et al., 2015). The neuropsychological profile of BDD has yet to be clearly established due to a paucity of investigations, therefore comparisons to OCD in this respect may be premature. Indeed, the relevant studies reviewed here were few in number, often narrow in scope and possibly underpowered, warranting cautious interpretation of their findings. Nevertheless, findings suggest similar dysregulation of prefrontal regions in both disorders, although a lack of impairment in other functions such as verbal fluency and set-shifting ability is consistent with a more complex interplay of dysfunctionality across wider brain networks in both conditions (Grace et al., 2017; Menzies et al., 2008).
Divergences between BDD and OCD
Regarding differences between BDD and OCD, our findings most prominently demonstrated worse illness insight in BDD than in OCD. We speculate that worse insight in BDD might relate to the highly perceptual (i.e. appearance based) nature of BDD beliefs, while the often abstract nature of OCD beliefs may permit more ‘malleable’ insight. For BDD, disturbances in visual processes might contribute to distortions of body image, which could reinforce disordered beliefs relating to appearance defects (Beilharz et al., 2017; Grace et al., 2017). In this sense, people with BDD may perceptually ‘see’ what they believe to be true with respect to their appearance – which in turn may act as an especially convincing reinforcer of reduced insight.
Concordantly, one study in this review demonstrated greater use of detailed visual processing in BDD than OCD. This result is consistent with previous findings of a behavioural bias towards detailed visual processing and hyperactivity of detailed-oriented visual systems in BDD (Beilharz et al., 2017). A bias for detailed visual processing in BDD may also partly explain the finding of more disorganised visual scan strategies in BDD versus OCD during own-face viewing. Reduced coherency of own-face scan strategies in BDD has been previously linked to intensive selective attention towards and/or avoidance of preoccupying facial features (Greenberg et al., 2014; Grocholewski et al., 2012). Although speculative, we suggest that a bias for detailed visual processing combined with selective attention towards disliked appearance features might magnify distortions of body image in BDD and might be an aetiologically important distinguishing feature of BDD relative to OCD.
Although supported by less consistent results, the review also demonstrated some support for impaired facial affect recognition in BDD versus OCD, especially for the misinterpretation of expressions of others, as anger. These results align with those of previous studies of facial affect recognition in BDD (Buhlmann et al., 2011; Jefferies et al., 2012; Labuschagne et al., 2011), as well evidence of mild yet specific affect recognition impairments in OCD (Daros et al., 2014). For BDD, affect recognition impairment might relate to visual processing disturbances, or overriding appearance preoccupations may divert visual attention away from features germane to affect identification (Toh et al., 2015b). In addition, misinterpretation of expressions as anger in BDD may stem from negative expectations that others will be rejecting or hostile in response to perceived flaws in one’s appearance (Buhlmann et al., 2006; Kollei et al., 2012). As such, this anger misinterpretation bias could relate to high social anxiety or problems with social cognition in BDD.
While both BDD and OCD clearly involve clinically elevated social anxiety, careful interpretation of mixed comparative findings suggests there is more severe social anxiety in BDD than in OCD. With this, BDD appears indistinguishable from SAD in the severity of social anxiety symptoms (albeit with differing cognitions; that is, body related in BDD, social performance in SAD), while social anxiety in OCD appears not to reach the same intensity. Furthermore, results from one study suggested that BDD may place relatively higher than OCD on a continuum of social cognitive impairment, again with close overlap between BDD and SAD. Finally, BDD was also associated with increased negative, self-focused interpretative biases of social situations relative to OCD in one study. Although based on limited findings, we suggest that these studies (along with evidence of facial affect recognition impairment in BDD) support a significant role of social-affective dysregulation in BDD as compared to OCD. Other work has demonstrated that self-evaluative concerns in BDD are frequently accompanied by equally important and anxiety-provoking socio-evaluative concerns (Anson et al., 2012) and that individuals with BDD endorse strong fear of social consequences such as rejection, humiliation and isolation contingent on other’s evaluations of their appearance (Veale et al., 1996). As such, greater attention to social-affective dysregulation in the clinical treatment of BDD may enhance treatment outcomes. In particular, treatment strategies for SAD may have translational value in addressing social-affective aspects of BDD concerns. However, there is a need for fine-grained investigations of the operative role of social-affective dysregulations in both BDD and OCD, as both conditions present with clinically significant social anxiety, and a minority of individuals with BDD have no socio-evaluative concerns (Veale, 2004).
Finally, the review findings indicate subtle differentiation between reduced insight and proneness to cognitive styles associated with psychotic delusions in both BDD and OCD. First, OCD appeared to place higher than BDD on a continuum of proneness to delusional thinking styles when compared to controls and schizophrenia patients (i.e. OCD indistinguishable from schizophrenia). This subtle difference in continuum placement may reflect the predominance of unusual beliefs or magical thinking styles than often underpin OCD obsessions, while disordered beliefs in BDD appear circumscribed to appearance-based concerns which involve less broad magical thinking styles. Second, two studies found that neither BDD nor OCD demonstrate cognitive reasoning biases, which are often associated with psychosis. Together, these findings contrast with strong evidence of poorer illness insight in BDD than in OCD. As such, the current evidence seems to suggest that poor/absent insight in BDD and OCD may be best conceptualised separately from (psychotic) delusionality and that magical thinking may have a differential role in OCD than in BDD.
Limitations
Although this review provides a comprehensive overview of the comparative research between BDD and OCD to date, there are limitations which must be considered in interpretation of the findings. The relatively small number of studies, few replications and predominance of potentially underpowered studies in this review necessitate cautious interpretation and highlight the need for increased comparative studies. Adding to this concern is the frequent inclusion of individuals with BDD-OCD within BDD and OCD groups, which may have obscured delineation of differences between the disorders. Similarly, efforts to match study samples across core demographic features may have obviated population-level differences in these features. In addition, the absence of biological comparisons in this review represents a significant gap in our understanding of possible interrelationships or divergences between BDD and OCD, as these investigations are essential in forming a nuanced understanding of the links between clinical presentation features and underlying biological aetiological mechanisms (Cuthbert, 2014). Finally, the lack of treatment research included in this review represents a significant limitation, as such studies are essential for establishing the relative efficacy of certain interventions (e.g. cognitive-behavioural therapy, medications) across BDD and OCD. In particular, the current classification of BDD as an Obsessive Compulsive Related Disorder may lead clinicians to apply similar treatment models to both OCD and BDD, but the utility of shared approaches remains to be investigated. Given these limitations, there is a clear need for further comparative investigation of BDD and OCD, particularly in biological domains, treatment and other areas (e.g. phenomenology and cognition) which may uncover core and transdiagnostic features in the disorders. Importantly, this work should be well-powered, replicative and expansive upon current studies and rigorous in accounting for the presence of BDD-OCD within sample groups.
Future research and conclusion
This review demonstrates a need for further theoretical and empirical evaluation of current models of BDD, and the nosological standing of BDD as belonging within the Obsessive-Compulsive and Related Disorders category. While the reviewed evidence corroborates some claims of similarity between BDD and OCD as made by research groups involved in development of the DSM-5, particularly in the areas of symptom severity, average age of onset and illness course, there was no clear comparative evidence to support claims of similarity in several other listed areas, including familiality, neurobiology, biomarkers, temporal antecedents and responsiveness to serotonin reuptake inhibitors (Phillips et al., 2010). As such, our review findings lead us to suggest that the current classification of BDD within the Obsessive-Compulsive and Related Disorders category may not be the most appropriate. Other evidence has indicated that BDD shares many dimensional similarities with other conditions such as SAD and AN, but these linkages have been much less studied (Fang and Hofmann, 2010; Hartmann et al., 2013). As such, it is possible that the conceptualisation of BDD as an Obsessive-Compulsive and Related Disorder is in part a product of intensive research focus on links between BDD and OCD, to the exclusion of other possible linkages. For example, BDD and AN share core psychological components of distorted body image, poor illness insight, intense overvaluation of appearance and body-focused behaviours specifically intended to check, change or hide disliked bodily features (Hartmann et al., 2013). The disorders also share abnormalities in visual system functioning, particularly regarding detail-oriented visual systems, which has been theorised to link in to body image preoccupations in both disorders (Li et al., 2015a, 2015b). As such, BDD might be better classified as a ‘body image disorder’, closely related to AN (Haliburn, 2018; Phillipou et al., 2017). In particular, the muscle dysmorphia subtype of BDD has been hotly contested in this respect (dos Santos Filho et al., 2016; Murray and Touyz, 2013; Phillipou et al., 2016). In addition, BDD and SAD share many overlaps in clinical features, including severe social anxiety, avoidant and safety-seeking behaviours, threat-based interpretations of ambiguous information and responsiveness to very similar modalities of cognitive-behavioural therapy (Fang and Hofmann, 2010). As such, BDD might also be conceptualised as an anxiety disorder, just as OCD had been up until publication of DSM-5. Indeed, some researchers have suggested that overlaps between BDD and OCD reflect shared anxiety-driven pathology (Abramowitz and Jacoby, 2015; Stein et al., 2010). Regardless, it is clear that further research is required to better inform any future classification of BDD. Thus, future research should investigate relationships between BDD and OCD, and disorders other than OCD (e.g. AN, SAD) in areas that may relate to core pathology, such as underlying psychological, cognitive and neurobiological features. Data from such research will determine the specificity of observed similarities between BDD and OCD, and between BDD and other disorders, thus providing broad and balanced information in the development of better theoretical models of BDD.
Furthermore, the review highlighted numerous areas of both overlap and difference between BDD and OCD (e.g. social cognition, fear of self and proneness to unusual thinking). These findings demonstrate the need for a dimensional approach in the study of overlaps between disorders, rather than simple identification of categorical similarities or differences. While the current categorical approach of the DSM has had pragmatic success in providing a framework for research, treatment and management of psychological conditions, the system inherently dissuades a multidimensional approach in the understanding of psychopathology. BDD is quite clearly a distinct yet multidimensional disorder involving strong overlaps with multiple other conditions, and as such is not simple to categorise within the DSM hierarchy (Schneider et al., 2018). Alternate approaches such as the Research Domain Criteria system, which emphasises a cross-diagnostic dimensional approach to psychiatric research, may be better suited to improving our understanding of complex conditions (Cuthbert and Insel, 2013). Elucidation of the relative positioning of BDD and other disorders along various illness dimensions within such an approach can help to clarify the complexity of BDD and more accurately crystallise our conceptualisations of the condition. Furthermore, this intuitive dimensional approach is essential in advancement towards precision medicine, which is anticipated to provide improved treatment outcomes for complex conditions such as BDD (Cuthbert, 2014).
In sum, the present review provides limited support for conceptualisation of BDD as belonging within the Obsessive-Compulsive and Related Disorders category, as adapted in the current DSM-5. Evidence of shared features between BDD and OCD appear to largely reflect a broad template of severe, intractable mental illness, and the presence of transdiagnostic features which may be common to many psychopathologies. Several areas of difference between BDD and OCD were identified which may reflect divergences in aetiopathogenesis between the disorders. In particular, BDD appears associated with poorer illness insight, increased detail-oriented visual processing, impaired and anger-biased facial affect recognition, elevated social anxiety and possibly broader social-affective dysregulation. As such, we suggest that the current nosological standing of BDD within the Obsessive-Compulsive and Related Disorders category deserves further research investigation and re-evaluation in future. Specifically, research which elucidates underlying illness mechanisms in BDD and their connections to clinical presentation, and clarifies complex dimensional linkages between BDD and other disorders, will be essential in improving our understanding and treatment of BDD.
Footnotes
Acknowledgements
A.M. would like to acknowledge the support of the Australian Government Research Training Program Scholarship during preparation of this publication. P.G.R. would like to acknowledge support of an Australian Catholic University Research Fund Program Grant during his contribution to this publication.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
