Abstract

To the Editor
Clozapine is the medication of choice for treatment-resistant schizophrenia. Clozapine has multiple serious side effects, including slowed gastrointestinal transit in up to 80% of patients as it has significant anticholinergic effect and serotonin receptor antagonism (Every-Palmer et al., 2017). Slowed gastrointestinal transit can potentially result in severe constipation, paralytic ileus and bowel obstruction, the latter being associated with a high mortality rate (De Hert et al., 2011). The usual management of clozapine-induced gastrointestinal hypomotility (CIGH) is administration of multiple laxatives although there is little evidence of their efficacy (Every-Palmer et al., 2017).
Prucalopride is an agonist of the serotonin 5HT4 receptors and its administration increases gut motility without causing QTc interval prolongation or significant cardiac ischemia (Quigley et al., 2009). In Australia, prucalopride can be prescribed for adults with chronic functional constipation, who have not responded to at least two laxatives for at least 6 months. Cisapride is also a 5HT4 agonist and was used in the past but was removed because of severe cardiovascular adverse effects.
Here, we report two successful responses to prucalopride in patients with severe CIGH who did not respond to multiple laxatives and who regularly required enemas. Patient A was a 48-year-old male with schizophrenia since 1996 who was on a combination of clozapine, amisulpride, lamotrigine, clonazepam and allopurinol. Patient B was a 56-year-old male with a 40-year history of schizophrenia and who was on a combination clozapine and paliperidone. It was noted that their mental state deteriorates rapidly when they are constipated.
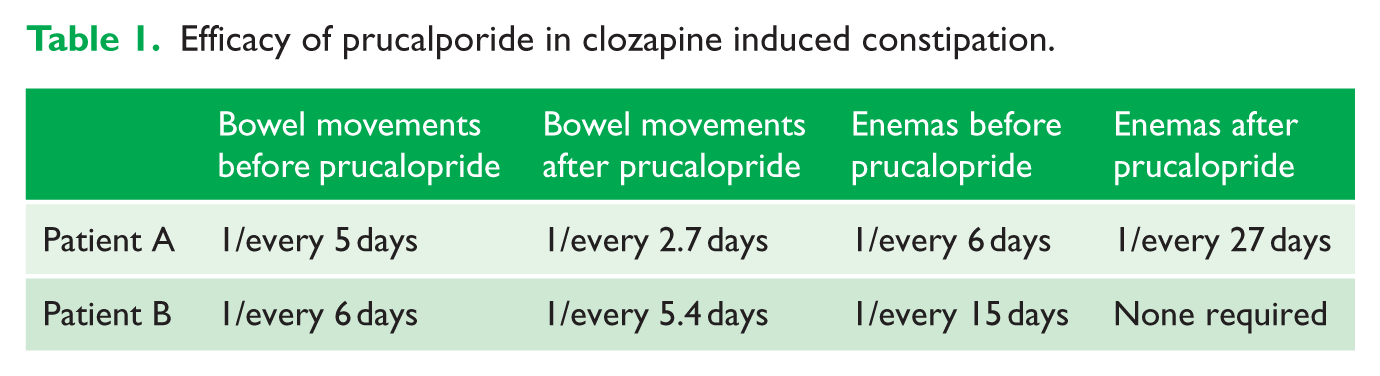
Considering these scenarios, and after discussion with a colorectal surgeon (J.M.C.Y.), the treatment team considered using cardiac safe prokinetic medication, prucalopride. Both patients were commenced on prucalopride 2 mg once daily in addition to the regular laxatives. Daily bowel movements were charted. After trial of prucalopride, there was a significant improvement in constipation for both patients (Table 1) and no side effects were reported. A considerable improvement in the mental state in these patients was also noted.
Efficacy of prucalporide in clozapine induced constipation.
The use of prucalopride for management of CIGH is promising, and future clinical trials assessing its efficacy and tolerability would be valuable.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
