Abstract
Context:
The relationship between benzodiazepine consumption and subsequent increases in aggressive behaviour in humans is not well understood.
Objectives:
The current study aimed to identify, via a systematic review, whether there is an association between benzodiazepine consumption and aggressive responding in adults.
Method:
A systematic review was conducted and reported in line with the PRISMA statement. English articles within MEDLINE, PsycARTICLES, PsycINFO, Academic Search Complete, and Psychology and Behavioural Sciences Collection databases were searched. Additional studies were identified by searching reference lists of reviewed articles. Only articles that explicitly investigated the relationship between benzodiazepine consumption and subsequent aggressive behaviour, or a lack thereof, in human adults were included.
Results:
Forty-six studies met the inclusion criteria. It was not possible to conduct a meta-analysis due to the heterogeneity of study design and benzodiazepine type and dose. An association between benzodiazepine use and subsequent aggressive behaviour was found in the majority of the more rigorous studies, although there is a paucity of high-quality research with clinical or forensic populations. Diazepam and alprazolam have received the most attention. Dose-related findings are inconsistent: therapeutic doses may be more likely to be associated with aggressive responding when administered as a once-off, whereas higher doses may be more risky following repeated administration. Trait levels of anxiety and hostility may indicate a vulnerability to the experience of benzodiazepine-related aggression.
Conclusions:
There appears to be a moderate association between some benzodiazepines and subsequent aggressive behaviour in humans. The circumstances under which aggressive responding may be more likely to follow benzodiazepine use remain unclear, although some evidence suggests dose and/or personality factors may influence this effect.
Rationale
Benzodiazepines are one of the most commonly prescribed classes of pharmaceuticals in developed countries (Australian Institute of Health and Welfare, 2011; Health and Social Care Information Centre, 2011; Home Office Statistics, 2012; Stephenson et al., 2013; Substance Abuse and Mental Health Services Administration, 2011). They are commonly prescribed for the management of anxiety, sleep disorders, agitation and alcohol withdrawal (Ashton, 2002). Although the most common effects of benzodiazepines include sedation and reduced anxiety, there have been reports of some users experiencing behavioural disinhibition following consumption, which includes aggressive behaviour (Bond, 1998; Fry et al., 2007; Paton, 2002). In fact, it is estimated that anywhere between 1% and 20% of benzodiazepine users experience some form of increased anger or express aggression (Lader, 2011). Furthermore, a number of clinical case studies report that individuals experience aggressive responding following administration of a range of benzodiazepines including diazepam (Gardos, 1980; Lion et al., 1975; Zisook and DeVaul, 1977), clorazepate (Karch, 1979), alprazolam (Rosenbaum et al., 1984), clonazepam (Binder, 1987; Kalachnik et al., 2003), and flunitrazepam (Dåderman et al., 2003). Such incidents occurred at both high and low doses (approximate diazepam (DZM) equivalent doses ranging between 5 mg and 240 mg), and by individuals with (Kalachnik et al., 2003; Lion et al., 1975) and without (Karch, 1979) histories of aggressive behaviour. Despite this accumulating clinical evidence, there has been no systematic review of the existing literature to inform policy or practice.
A complicating factor is the variable definitions of aggression used within the literature. For the purposes of this report, aggressive behaviour is defined as physical behaviour directed toward another person with the goal of harming or injuring that person, who is motivated to avoid such behaviour (Baron and Richardson, 1994). The term ‘violence’ is often used interchangeably with ‘aggression’, although commonly reflects more serious harm (Anderson and Bushman, 2002) and forensic contexts (Anderson and Bokor, 2012). Our definition deliberately describes the behaviour of interest (i.e. physical force against another) without a severity clause, in order to capture these more severe instances of aggression (DeWall et al., 2011). We feel that to exclude research pertaining to ‘violence’ would be to exclude valuable information from individuals involved in the criminal justice system, to whom forensic implications stemming from benzodiazepine-related aggression may directly apply. Our deliberate and sole focus on physical aggression directed toward another person is due to the potential severe medical and legal consequences of such responses for the victim and perpetrator, respectively (i.e. hospitalisation and mortality; legal responsibility, sentencing, and rehabilitation considerations).
This issue has significant implications for judicial decision-making pertaining to violent offending behaviour. For example, a study of 102 injecting drug users (with a range of criminal histories) reported that benzodiazepine use was associated with unprovoked aggressive behaviour (20%), fights (13%) and crime (14%; Smith et al., 2007). Furthermore, self-reported substance use in adult police detainees (n=1884) indicated that 27% of users attributed their current offence to benzodiazepine use (Payne and Gaffney, 2012). Although limited by the use of retrospective self-attributions of behaviour causes and the lack of control for concurrent substance use, these findings do highlight that disentangling these issues via a systematic and critical analysis of the literature is timely.
A number of biological theories have been proposed to explain how benzodiazepines may possibly increase aggressive responding. Neurological theories based on animal models have suggested that certain subunits on GABAA receptors (γ, α) may be implicated (e.g. Lee and Gammie, 2010; Miczek et al., 2003), and others have considered the similar neurological effects between benzodiazepines and alcohol as contributing to aggression (e.g. Miczek et al., 1993). It has also been posited that benzodiazepines disrupt the endogenous anxiety/threat-detection system (Hoaken and Stewart, 2003). However, the very nature of benzodiazepine use contributes additional complexity to understanding benzodiazepine-related aggression. For example, benzodiazepines are regularly consumed with other substances, including those which have been previously associated with aggression (i.e. anabolic steroids and alcohol; Anderson and Bokor, 2012; Lennings et al., 2003; Lundholm et al., 2010). In addition, aggression has been reported following both prescribed doses and considerably higher doses (Hoaken and Stewart, 2003; Paton, 2002), and although anecdotal concern generally rests with short-acting benzodiazepines (i.e. alprazolam; e.g. French, 1989) due to their greater abuse potential, evidence also demonstrates aggressive responses following long-acting benzodiazepines (i.e. diazepam; e.g. Ben-Porath and Taylor, 2002). Taking into account such complexity, Lion and colleagues (1975) suggest an interaction between drug use, personality, and environmental factors, with more recent research highlighting that personality may be as, or more, important than pharmacological factors (Ben-Porath and Taylor, 2002; Hoaken and Stewart, 2003; Paton, 2002; Wilkinson, 1985). Lion and colleagues’ premise aligns with general understandings of aggressive and violent behaviour, in that it is multiply determined, and involves sociological, genetic, biological, and environmental factors (Anderson and Bokor, 2012). The circumstances under which aggressive behaviour is likely to result following benzodiazepine consumption are poorly understood and the literature lacks a systematic review of the empirical research investigating the relationship between benzodiazepine consumption and subsequent aggressive or violent behaviour. This relationship needs to be understood when considering prescribing protocols, and the potential clinical and legal implications of aggressive responses. This paper reports on a systematic review addressing the question: Does benzodiazepine consumption increase aggressive behaviour in adult humans?
Methods
A systematic review was designed and reported according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) statement (Liberati et al., 2009; Moher et al., 2009). The Maryland Scale of Scientific Rigour (Sherman et al., 1998) was applied to assess each study’s internal validity. According to this scale, randomised clinical trials (RCTs) and well-controlled experimental studies provide the strongest level of scientific rigour (Sherman et al., 1998). Although experimental studies can inform the impact of acute doses, they provide limited information on chronic use, and the findings are based on highly contrived circumstances. Therefore, less rigorous designs (i.e. cross-sectional, prospective) were included in this review in order to enhance the ecological and clinical validity of the findings. However, at the lowest level of evidence (Merlin et al., 2009), case studies were excluded from consideration due to their poor generalisability (Evans, 2003). Further information on methods can be found in Supplementary Material Appendix A.
Eligibility criteria
Studies investigating the relationship between benzodiazepines and aggression in adult human populations were located. Inclusion criteria included English language and peer-reviewed journal articles. Exclusion criteria included animal studies, unrelated neurobiological studies, case studies, and clinical trials which did not explicitly measure aggression. Articles were also excluded if they investigated non-benzodiazepine sedatives, hypnotics, or anxiolytics. Synthesis articles (i.e. reviews, meta-analyses) were excluded following examination of their reference lists for original articles meeting the above criteria.
Information sources
The search was applied to Medline Complete, PsycARTICLES, PsycINFO, Academic Search Complete, and the Psychology and Behavioural Sciences Collection electronic databases.
Search terms used were: benzo*, BZD, sedative, hypnotic, anxiolytic, anti-anxiety medication, anti-anxiety drug, tranquilisers, tranquilizers, diazepam, lorazepam, temazepam, alprazolam, flunitrazepam, oxazepam, clonazepam, nitrazepam, aggress*, and violen*.
Study selection
Two authors (BA and PS) independently screened the titles and abstracts of all publications obtained by the search strategy (2492), and assessed the full text of selected articles (64) for inclusion. In questionable cases, the authors discussed the inclusion and exclusion requirements and came to a consensus.
Results
Study selection
The initial database search revealed a total of 2492 articles. Of these, 2428 studies were discarded as duplicates or because they did not meet the criteria (Figure 1). The full text of the remaining 64 citations was examined in more detail. An additional 15 articles were identified by examining the reference lists of these citations and through previous literature searches. Thirty articles did not meet the inclusion criteria as described, including 19 non-systematic reviews, and a review investigating the behavioural side effects of benzodiazepines in individuals with an intellectual disability (Kalachnik et al., 2002). Upon detailed study, two studies were excluded (Cherek et al., 1987; Cowdry and Gardner, 1988) because they reported the same data as a further two (Cherek et al., 1990; Gardner and Cowdry, 1985, respectively); the latter two contained more methodological and statistical detail. One experimental study (Brown, 1978) was excluded as it failed to report details regarding method. Hence, 46 studies met the inclusion criteria.
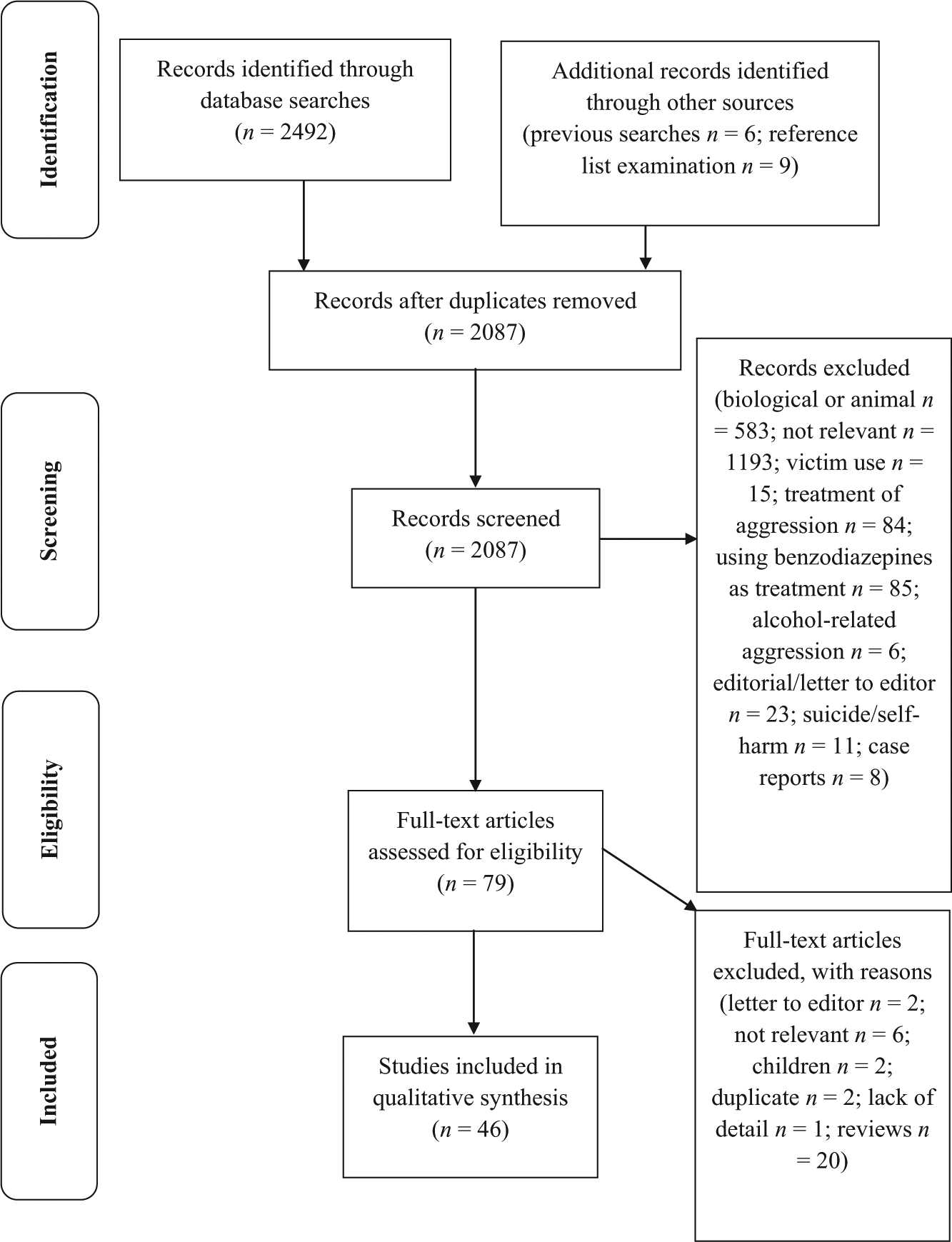
PRISMA flow diagram depicting the flow of information through the stages of the systematic review.
Study characteristics
The 46 studies varied considerably in terms of study design, type of samples, the range of benzodiazepines examined and doses considered. Owing to the heterogeneity of the study design and benzodiazepine type and dose, it was not possible to conduct a meta-analysis on the reviewed data.
Design
The association between benzodiazepine consumption and subsequent aggressive behaviour had been explicitly investigated in two prospective studies, 25 cross-sectional studies, six clinical studies, and 13 experimental studies.
Sample
The studies investigated clinical (n=15), forensic (n=12), and healthy community (n=19) samples.
Drug type
Benzodiazepines investigated across the studies included diazepam, alprazolam, flunitrazepam, triazolam, temazepam, clonazepam, oxazepam, lorazepam, and clorazepate. Diazepam and alprazolam have received the most attention (nine and six studies, respectively), and 43.5% (n=20) explored non-specific benzodiazepine use.
Dose
The included studies investigated both therapeutic and higher doses; approximate DZM equivalent doses for the clinical and experimental studies ranged between 3.3 mg and 100 mg, and 2 mg and 20 mg, respectively. The experimental studies examined acute benzodiazepine administration, whilst the clinical studies explored chronic administration ranging from four days to three months. Cross-sectional and prospective studies did not specify dose. Tables 1 and 2 detail the characteristics of the included studies.
Characteristics of included studies assessing non-specific benzodiazepine-related aggressive behaviour (ordered by year of publication).
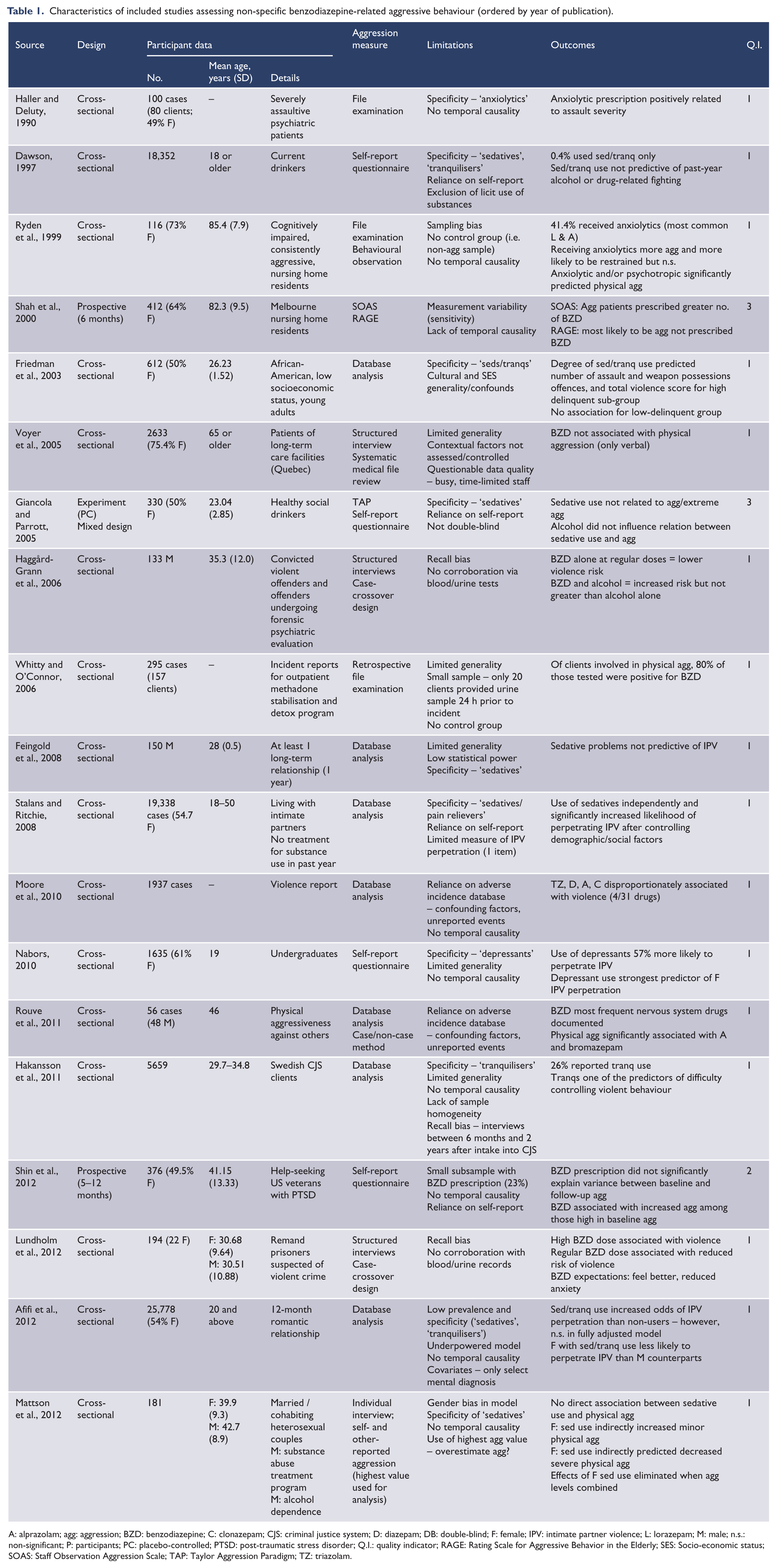
A: alprazolam; agg: aggression; BZD: benzodiazepine; C: clonazepam; CJS: criminal justice system; D: diazepam; DB: double-blind; F: female; IPV: intimate partner violence; L: lorazepam; M: male; n.s.: non-significant; P: participants; PC: placebo-controlled; PTSD: post-traumatic stress disorder; Q.I.: quality indicator; RAGE: Rating Scale for Aggressive Behavior in the Elderly; SES: Socio-economic status; SOAS: Staff Observation Aggression Scale; TAP: Taylor Aggression Paradigm; TZ: triazolam.
Characteristics of included studies assessing benzodiazepine-related aggressive behaviour (ordered by benzodiazepine type and year of publication).
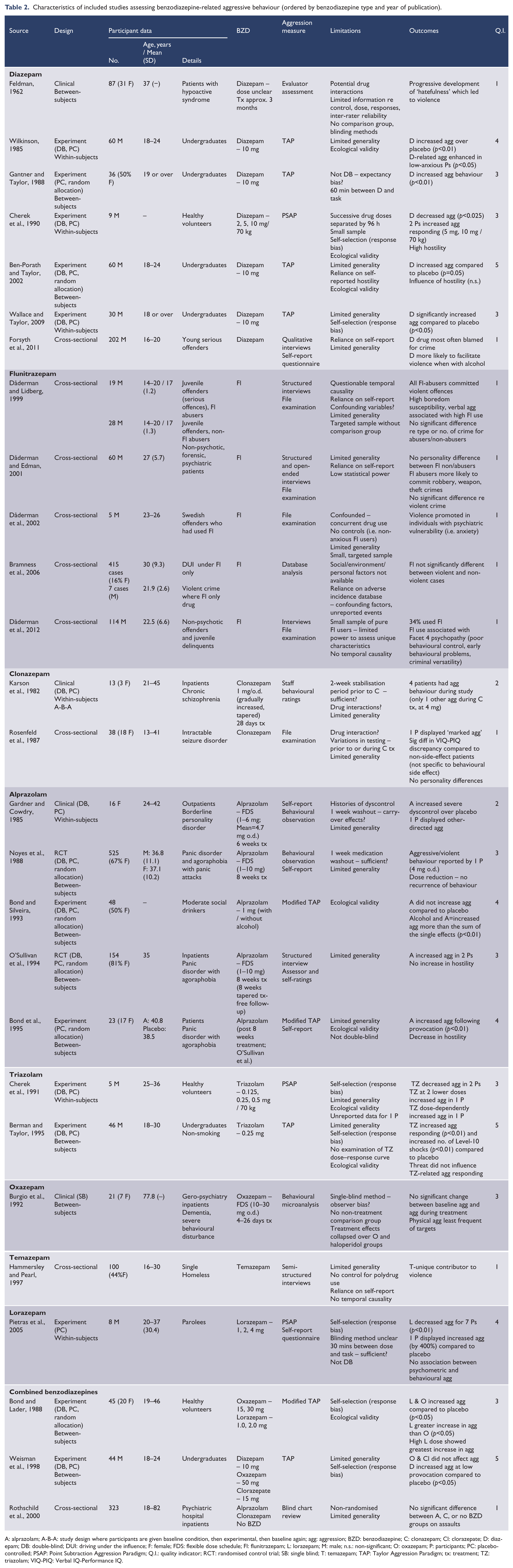
A: alprazolam; A-B-A: study design where participants are given baseline condition, then experimental, then baseline again; agg: aggression; BZD: benzodiazepine; C: clonazepam; Cl: clorazepate; D: diazepam; DB: double-blind; DUI: driving under the influence; F: female; FDS: flexible dose schedule; Fl: flunitrazepam; L: lorazepam; M: male; n.s.: non-significant; O: oxazepam; P: participants; PC: placebo-controlled; PSAP: Point Subtraction Aggression Paradigm; Q.I.: quality indicator; RCT: randomised control trial; SB: single blind; T: temazepam; TAP: Taylor Aggression Paradigm; tx: treatment; TZ: triazolam; VIQ-PIQ: Verbal IQ-Performance IQ.
Risk of bias within studies
There were multiple risks of bias in each article reviewed, ranging from limited generalisability to potential confounding by drug interactions, as detailed in the tables. Application of the Maryland Scale of Scientific Rigour (Sherman et al., 1998) demonstrated that, overall, 56.5% (n=26) of the included studies are of a Level 1 standard, and only 6.5% (n=3) are of a Level 5 standard, indicating that the quality of the evidence base surrounding the benzodiazepine–aggression relationship is poor.
Synthesis of results
Does benzodiazepine consumption increase aggressive behaviour in adult humans?
The reviewed literature demonstrated a moderate relationship (with some inconsistency) between benzodiazepine consumption and subsequent aggression. Diazepam demonstrated the greatest association with increased aggression (n=6 studies; 13.0%), and has been examined in more high-level (Levels 4 and 5; n=3) studies than any other benzodiazepine.
Experimental studies
The 13 experimental studies utilised either the Taylor Aggression Paradigm (TAP; n=10) or the point subtraction aggression paradigm (PSAP; n=3), with the majority utilising placebo-controlled (n=11) and double-blind (n=9) methods. The TAP involves participants administering and receiving electrical shocks under a competitive reaction time task, where the participant’s shock setting for a (fictional) opponent gives a proxy measure of behavioural aggression. Reaction to provocation is also measured, by providing participants with an indication of the shock set per trial by their opponent. Modifications involve using noise instead of shocks (e.g. Bond and Lader, 1988). The PSAP provides participants with a choice between escape responding, non-aggressive monetary-reinforced responding, and a proxy measure of aggression involving the subtraction of money from a (fictional) opponent, following provocation. It is noted that although laboratory proxy measures of aggression have demonstrated some external (Anderson and Bushman, 1997) and construct validity (e.g. Cherek et al., 2000; Giancola and Parrott, 2008; Golomb et al., 2007), debate continues as to the empirical value and external validity of laboratory aggression paradigms (e.g. Ferguson and Rueda, 2009; Ferguson et al., 2008). Eleven studies investigated undergraduate students or community members (18–46 years old), and one study each explored a clinical (28–40 years; Bond et al., 1995) and forensic (20–37 years; Pietras et al., 2005) sample.
Variable effects were reported both within and across benzodiazepine types. Diazepam was found to consistently increase responding, indicative of behavioural aggression in five studies and produce mixed responses in one study; two studies demonstrated increased responding indicative of aggression following alprazolam consumption; lorazepam, oxazepam, and triazolam each demonstrated varied results between two studies; and one study demonstrated clorazepate to have no effect on responding. Study methodology may have influenced these findings, as responding indicative of aggression generally increased in TAP studies and decreased in PSAP studies post-benzodiazepine consumption. Studies that utilised the original or modified TAP demonstrated enhanced aggressive responding following consumption of triazolam (Berman and Taylor, 1995), lorazepam, oxazepam (15 mg, 30 mg; Bond and Lader,1988), alprazolam (Bond et al., 1995), combined alcohol and alprazolam (Bond and Silveira, 1993), and diazepam (Ben-Porath and Taylor, 2002; Gantner and Taylor, 1988; Wallace and Taylor, 2009; Weisman et al., 1998; Wilkinson, 1985), but not clorazepate or oxazepam (50 mg; Weisman et al., 1998), and self-reported ‘sedative’ use in healthy adults did not influence alcohol-related aggressive responding (Giancola and Parrott, 2005). Interestingly, Wilkinson (1985) reported that aggressive responding was enhanced in low-trait anxious participants compared to high-trait anxious participants. The variation concerning oxazepam may reflect a dose effect or an insufficient absorption period by Weisman and colleagues (1998) (90 minutes versus 4 hours), as oxazepam has been found to have a later onset of action (Bond and Lader, 1988). Comparatively, the PSAP studies demonstrated decreased responding indicative of aggression in the majority of participants following lorazepam (n=8; Pietras et al., 2005), triazolam (n=5; Cherek et al., 1991), and diazepam consumption (n=9; Cherek et al., 1990). Response patterns in the latter study indicated increased aggressive responding in high hostile participants (n=2). Personality characteristics were measured in a further four studies (Bond and Lader, 1988; Bond and Silveira, 1993; Bond et al., 1995; Pietras et al., 2005); however, none discussed whether individual differences were related to patterns of responding.
The most common approximate DZM equivalent doses administered acutely were 5 mg and 10 mg (DZM range=2–20 mg), and each produced variable results. Findings of two out of five studies using 5 mg (Berman and Taylor, 1995; Bond and Lader, 1988) and five out of ten studies using 10 mg (Ben-Porath and Taylor, 2002; Bond and Lader, 1988; Gantner and Taylor, 1988; Wallace and Taylor, 2009; Wilkinson, 1985) suggested increased aggression. Higher doses either failed to influence aggressive responding (DZM=16.7 mg; Weisman et al., 1998) or resulted in decreased responding indicative of aggression (DZM=20 mg; Pietras et al., 2005), and only one participant displayed increased aggressive responding following the low equivalent dose of 2.5 mg (Cherek et al., 1991). Only one study considered chronic administration, where participants engaged in the laboratory task following 8 weeks of alprazolam treatment (DZM=10–100 mg) or placebo (Bond et al., 1995). Although the findings indicated alprazolam use increased behaviour indicative of aggression compared to placebo, the flexible dosing schedule precludes consideration of dose effects.
Overall, the experimental studies suggest that acute administration of certain benzodiazepines (i.e. diazepam, alprazolam) can result in an increased aggressive response in adults. However, the use of analogue representations of aggression greatly limits the ecological validity of the findings. Moreover, the studies cannot inform our understanding of chronic benzodiazepine use, and the reliance on healthy community samples reduces their ability to inform clinically pertinent prescribing practices.
Clinical studies
The review identified six clinical studies of varying methodological rigour. In each instance, aggression following benzodiazepine use was a secondary consideration. The clinical populations varied widely, including individuals with panic disorder and agoraphobia (Noyes et al., 1988; O’Sullivan et al., 1994), chronic schizophrenia (Karson et al., 1982), borderline personality disorder (BPD; Gardner and Cowdry, 1985), hypoactive syndromes (Feldman, 1962), and psychogeriatric patients (Burgio et al., 1992). Across the combined samples, aggressive behaviour was reported following benzodiazepine consumption in less than 1% (0.6%) of participants.
Only two of the clinical studies reviewed were RCTs (Noyes et al., 1988; O’Sullivan et al., 1994). Both explored acceptance and side effects of alprazolam treatment over eight weeks in individuals with panic disorder and agoraphobia (n=525, Noyes et al., 1988; n=154, O’Sullivan et al., 1994). Inspection of the data indicates that one (0.19%; Noyes et al., 1988) and two (1.3%; O’Sullivan et al., 1994) patients demonstrated elevated physical aggression during treatment, in one case following a DZM equivalent dose of 40 mg (Noyes et al., 1988). Further interpretation of the role of alprazolam in these events is hampered by inadequate detail regarding dosing schedules and the length of alprazolam treatment prior to the aggressive incidents.
Two studies utilised double-blind and placebo-controlled methods in a within-subjects design to explore the effect of clonazepam on individuals with chronic schizophrenia (n=13; Karson et al., 1982) and alprazolam on behavioural dyscontrol in females with BPD (n=16; Gardner and Cowdry, 1985). Each of the studies reported aggressive responding in a single patient following an equivalent dose of 80 mg (Karson et al., 1982) and 20 days of treatment (Gardner and Cowdry, 1985). Less rigorous designs and poor reporting characterised the final two studies. An unclear number of individuals with hypoactive syndromes demonstrated aggressive responding following an unreported dose of diazepam (Feldman, 1962), and collapsed treatment effects across oxazepam and haloperidol suggested no changes in aggressive behaviour during treatment (4–26 days) in a sample of psychogeriatric patients (n=21; Burgio et al., 1992). It is interesting, and potentially clinically pertinent, that the latter study utilised a substantially lower dose schedule (DZM=3.3–10 mg) than the above studies (DZM=10–100 mg) and reported no changes in aggression. However, any oxazepam-specific results are obscured by the authors’ decision to collapse the treatment effects.
The above findings suggest that instances of aggressive responding to benzodiazepines are rare in the clinical populations investigated. However, poor reporting makes consideration of control methods and dose schedules difficult. Moreover, although the results appear to suggest that higher doses may be more risky, it is difficult to draw conclusions regarding chronic administration of benzodiazepines due to the large variation in treatment periods (i.e. four days to three months; Burgio et al., 1992 and Feldman, 1962, respectively), and the potential of other drug interactions, with medication wash-out periods ranging from one week (Burgio et al., 1992; Gardner and Cowdry, 1985; Noyes et al., 1988) to two weeks (Karson et al., 1982; O’Sullivan et al., 1994).
Prospective studies
Only two prospective studies were identified, and both suggest an association between benzodiazepine consumption and aggressive behaviour. However, due to the associative nature of the studies, neither provides evidence of causality.
The association between benzodiazepine prescription and aggression lacked robustness in both papers, as the associative strength varied according to the operationalisation of aggression. In a 6-month study of nursing home residents, the finding of an association between increased benzodiazepine prescription and heightened levels of aggression depended on the observation rating scale used to classify participants as aggressive (Shah et al., 2000). As residents were assessed using both scales, this variation suggests some issues with scale validity. The second prospective study followed a random sample of help-seeking US veterans with post-traumatic stress disorder (PTSD), of whom 23% were prescribed benzodiazepines over 5–12 months (Shin et al., 2012). The findings demonstrated that although benzodiazepine prescription did not explain the overall variance between baseline and follow-up aggression scores, benzodiazepine prescription was related to increased aggressive behaviour in individuals who were aggressive at baseline. However, as the authors operationalised aggression as the sum of four items adapted from the Conflict Tactics Scale, where only one item referred to other-directed physical aggression, it is unclear which aspect/s of aggressive behaviour increased between baseline and follow-up. Combined, these studies indicate how variable measurement of aggression can affect findings, and, in turn, our understanding of the relationship between benzodiazepine use and subsequent aggression. Tentatively, however, individuals with higher baseline aggression levels may be more likely to experience benzodiazepine-related aggression.
Overall, both studies indicate some level of association between benzodiazepine prescription and aggressive behaviour. However, as neither study can suggest temporal order, the associations may reflect increased benzodiazepine prescriptions to manage aggressive behaviour. Moreover, both studies investigated highly specific samples, limiting generalisability, and neither study explored variations in benzodiazepine type or dose, and therefore fail to inform clinical practice.
Cross-sectional studies
The cross-sectional studies explored a range of sample types, including clinical (i.e. psychiatric, addiction, hospital; n=7), healthy or community (n=7), and forensic (i.e. criminal justice involvement or incidents, forensic psychiatric; n=11). Per sample type, a large proportion of studies suggested an association between benzodiazepine use and aggression (63.6–71.4%).
Overall, 14 (56%) cross-sectional studies demonstrate positive associations between benzodiazepine consumption and aggressive behaviour (Afifi et al., 2012; Dåderman et al., 2002, 2012; Forsyth et al., 2011; Hakansson et al., 2011; Haller and Deluty, 1990; Hammersley and Pearl, 1997; Lundholm et al., 2013; Moore et al., 2010; Nabors, 2010; Rouve et al., 2011; Ryden et al., 1999; Stalans and Ritchie, 2008; Whitty and O’Connor, 2006), and three studies provide mixed findings according to sex and level of aggression (Mattson et al., 2012), delinquent status (Friedman et al., 2003), and unclear differences in cognitive assessment scores (Rosenfeld, 1987). The final eight studies suggest that benzodiazepine use is not associated with physical aggression or violence (Bramness et al., 2006; Dåderman and Edman, 2001; Dåderman and Lidberg, 1999; Dawson, 1997; Feingold et al., 2008; Haggård-Grann et al., 2006; Rothschild et al., 2000; Voyer et al., 2005). It could be posited that levels of aggression do not significantly differ between benzodiazepine users and non-benzodiazepine users due to similar temperament and sensation-seeking scores (Dåderman and Edman, 2001). However, other cross-sectional findings assert the importance of intrapersonal factors in this effect, suggesting that certain personality traits assessed through empirically supported personality inventories (i.e. boredom susceptibility, verbal aggression, Dåderman and Lidberg, 1999; antisocial psychopathy characteristics, Dåderman et al., 2012) and file-based indicators of psychiatric vulnerability (e.g. anxiety, impulsivity; Dåderman et al., 2002) may influence an aggressive response to flunitrazepam.
Operationalisation and measurement of benzodiazepines and aggression varied considerably across studies. Examination of specific benzodiazepines suggested that aggressive behaviour was associated with use of temazepam (Hammersley and Pearl, 1997) and diazepam (Forsyth et al., 2011), but not alprazolam (Rothschild et al., 2000), with mixed results for flunitrazepam (Bramness et al., 2006; Dåderman and Edman, 2001; Dåderman and Lidberg, 1999; Dåderman et al., 2002, 2012) and clonazepam (Rosenfeld et al., 1987; Rothschild et al., 2000). However, nine studies utilised poorly defined terms such as sedatives or tranquilisers (e.g. Afifi et al., 2012; Dawson, 1997; Feingold et al., 2008; Friedman et al., 2003), or grouped benzodiazepines with other substances (e.g. opiates, gamma hydroxybutyrate; Mattson et al., 2012; Nabors, 2010; Stalans and Ritchie, 2008), reducing the specificity of results and attenuating the associative or predictive strength of the findings (e.g. Dawson, 1997). Furthermore, many studies failed to statistically control for concurrent substance use (e.g. Dåderman and Lidberg, 1999; Dåderman et al., 2002; Hammersley and Pearl, 1997). Similarly, although some studies clearly defined aggression (i.e. violent crime including manslaughter and assault; Dåderman and Edman, 2001; Dåderman and Lidberg, 1999; Dåderman et al., 2002, 2012; Haggård-Grann et al., 2006; Lundholm et al., 2013; Moore et al., 2010), only two studies utilised the same questionnaire (Conflict Tactics Scale-Revised; Afifi et al., 2012; Mattson et al., 2012), and five studies inferred aggression from endorsement of one (Hakansson et al., 2011; Hammersley and Pearl, 1997; Nabors, 2010; Stalans and Ritchie, 2008) or two (Dawson, 1997) items, reducing the interpretability of findings. Such variable operationalisation limits the ability to compare findings and form accurate conclusions about the benzodiazepine–aggression association.
Nonetheless, a tentative conclusion may be drawn regarding the role of dose with reference to the findings of two similar forensic studies. Both case-crossover designs, the studies operationalised violence as violent interpersonal crime (i.e. manslaughter, assault, murder), and employed structured interviews with convicted male violent offenders undergoing forensic psychiatric evaluation (n=133; Haggård-Grann et al., 2006), and remand prisoners suspected of violent crime (n=194; Lundholm et al., 2013). The studies demonstrated that benzodiazepines consumed alone (i.e. without alcohol) and in regular doses were associated with a reduced risk of violence (Håggard-Grann et al., 2006; Lundholm et al., 2013), but an increased risk of violence was associated with an unusually high intake of benzodiazepines (Lundholm et al., 2013). However, these findings must be considered in light of the following limitations. That is, they rely on ambiguous definitions of ‘regular’ or ‘unusually high’ doses, and on uncorroborated retrospective self-report from forensic samples.
Discussion
The literature review demonstrated a relative paucity of published papers explicitly examining the benzodiazepine–aggression relationship given its clinical importance. Of those papers which met the inclusion criteria, the majority of findings pertain to experimental studies of acute low doses of benzodiazepines, or cross-sectional examination of self-report data. Although it was not feasible to conduct a meta-analysis, according to our review of these studies it appears that benzodiazepine use is moderately associated with subsequent aggressive behaviour. Nine (69.2%) of the experimental studies reported a significant increase in behaviour indicative of aggression. However, study methodology may have impacted the observed outcomes, and there are clear limitations in generalising from simulated responses in contrived experimental settings to interpersonal aggression. Indeed, the clinical studies reported aggressive responding in less than 1% of participants (0.6%) during benzodiazepine treatment. However, as aggressive responding was not a focus of these studies, many lacked detail which limited the ability to draw conclusions to inform clinical prescribing practices. Although an association between benzodiazepine use and aggressive behaviour was indicated in the majority of the cross-sectional studies (n=17) and both prospective studies, the varied operationalisation of aggression and benzodiazepines impedes analysis of the proportion of individuals reporting benzodiazepine-related aggression. Moreover, as the correlational nature of these studies precludes analysis of temporal causality, their findings may reflect increased benzodiazepine use in order to manage aggressive tendencies. The discrepancies within the literature regarding the benzodiazepine–aggression relationship likely relate to differing methodologies, samples, and benzodiazepines tested.
Sample
The most methodologically rigorous studies (Levels 4 and 5) were conducted primarily on non-clinical samples (71%) such as undergraduates or social drinkers, with only two high-level studies exploring a clinical or forensic sample. The lack of high-quality evidence pertaining to these latter populations greatly hinders our ability to understand the clinical and legal implications arising from the benzodiazepine–aggression relationship.
Drug type
Diazepam was the most commonly examined benzodiazepine, and was associated with increased responding indicative of behavioural aggression in five out of six methodologically strong experimental studies. The second most commonly investigated benzodiazepine, alprazolam, was only investigated in two methodologically strong experimental studies, but both demonstrated enhanced aggressive responding post-consumption. Unfortunately, some benzodiazepines were examined in fewer than two studies, limiting our understanding of whether all benzodiazepines are at risk of aggressive responding. Consideration of the impact of short-acting versus long-acting benzodiazepines was based on the stringently controlled laboratory experiments. Enhanced responding indicative of aggressive behaviour was found in 62.5% of the studies exploring a short-acting benzodiazepine (i.e. alprazolam, oxazepam, triazolam, lorazepam), compared to 83.3% of the studies exploring diazepam (a long-acting benzodiazepine). Whilst this suggests a greater risk for long-acting benzodiazepines, this interpretation is given cautiously, as the findings per specific type of benzodiazepine varied, and enhanced behaviour indicative of aggression was not demonstrated following consumption of an intermediary benzodiazepine, clorazepate.
Dose
The inconsistent nature of the clinical and experimental dose-related findings suggests that a dose effect does not adequately explain benzodiazepine-related aggression. Aggression, or behavioural responses indicative of aggression, can result after both acute (single dose) and chronic (continuous treatment) administration of benzodiazepines. Examination of approximate DZM equivalent doses suggested that therapeutic doses (i.e. 5–10 mg) may be more likely to be associated with aggressive responding when administered acutely, whereas higher doses (i.e. 40 mg, 80 mg) may be more risky following chronic administration. However, this interpretation is made cautiously, due to the potential confound of study sample (i.e. healthy versus clinical, respectively).
Personality
Four cross-sectional studies explicitly examined personality; however, the use of targeted sampling (i.e. flunitrazepam using violent offenders; Dåderman and Lidberg, 1999; Dåderman et al., 2002) and the lack of non-violent control groups (Dåderman and Edman, 2001; Dåderman et al., 2012) precludes definitive conclusions that personality influences flunitrazepam-related violence. Controlled laboratory testing also demonstrated that diazepam-enhanced aggressive responding was associated with low levels of trait anxiety (Wilkinson, 1985) and high levels of hostility (Cherek et al., 1990). These findings suggest that trait levels of anxiety and hostility may indicate a vulnerability to the experience of benzodiazepine-related aggression; however, further research is needed to corroborate and clarify the role of interpersonal vulnerabilities in this response.
Limitations
Owing to the inclusion criteria, only the studies which explicitly examined the relationship between benzodiazepine consumption and subsequent aggressive behaviour were reviewed, and therefore clinical drug trials where aggressive behaviour was observed, but not explicitly measured or discussed in the design, were not identified. Furthermore, the review was limited to English studies and published data, which can limit the generalisability of the data (Cole and Kando, 1993). Operationalisation of aggression in the cross-sectional studies was considerably inconsistent, and studies often failed to control for concurrent substance use, use control or comparison groups, or clearly report methodological or statistical techniques. In addition, use of urinalysis or blood samples to corroborate reports of benzodiazepine use was extremely rare. Overall, the quality of the included studies was poor, indicating a need for higher quality studies exploring the benzodiazepine-aggression relationship. Of concern, none of the clinical studies considered benzodiazepine-related aggression a primary focus. Furthermore, investigation of forensic participants and individual differences was rare, reducing our ability to draw conclusions regarding the forensic implications of this review. Moreover, the majority of the experimental studies examined male-only samples (Ben-Porath and Taylor, 2002; Berman and Taylor, 1995; Cherek et al., 1990, 1991; Pietras et al., 2005; Wallace and Taylor, 2009; Weisman et al., 1998; Wilkinson, 1985), limiting generalisability to females, who have been demonstrated to use benzodiazepines for non-medical reasons more than males (Drugs and Crime Prevention Committee, 2007; Loxley, 2007; McGregor et al., 2011).
Conclusions
Anecdotal evidence indicates that the benzodiazepine–aggression response is an urgent clinical issue with serious clinical and forensic implications. The reviewed literature suggests that although there appears to be a moderate association between some benzodiazepines and subsequent aggressive behaviour in humans, the circumstances under which aggressive behaviour is likely to follow benzodiazepine consumption remain poorly understood. The evidence base requires high-quality and systematic investigation of the various benzodiazepines and doses. Jones and colleagues (2011) outline recommendations to reduce benzodiazepine-related harms when prescribing; however, there is limited evidence to further inform practice policy or legal defences. Such examination is especially pertinent, with increasing evidence that amnesia is a common consequence of benzodiazepine use (e.g. Chavant et al., 2011; Dåderman et al., 2003; Tannenbaum et al., 2012), which, when coupled with their afore-mentioned disinhibitory properties, may lead to unprecedented use of benzodiazepine-related legal defences (i.e. impaired responsibility, consideration of mitigating circumstances) in cases involving interpersonal violence. Advances in the literature are pertinent at a time when Australia has recently re-scheduled alprazolam to a controlled drug and considers similarly up-scheduling other benzodiazepines to Schedule 8.
Footnotes
Author contributions
The research question was posed by BA and PS. Database searches were conducted by BA, and BA and PS independently screened articles for inclusion in the review. Qualitative synthesis and initial draft manuscript was composed by BA, and all authors were involved in the writing and editing process.
Funding
No funding was sought for this systematic review.
Declarations of interest
We declare that none of the authors are in receipt of financial support, or have any relationship that may pose a conflict of interest in relation to the content presented in the submitted manuscript. Dan Lubman has received speaking honorarium from AstraZeneca and Janssen, as well as provided consultancy advice to Lundbeck.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
