Abstract
Objective:
There is growing evidence that anhedonia is a commonly experienced symptom among substance-using populations. This systematic review synthesises findings across a range of substances to address questions regarding the time course of anhedonia, how anhedonia relates to other symptoms of substance dependence and whether it is similarly prevalent across all addictive drugs.
Method:
A literature search was conducted on PubMed, PsycINFO and MEDLINE, yielding 32 studies that used self-report measures of anhedonia among participants with a history of a substance abuse, dependence or long-term daily use of addictive substances.
Results:
Findings from these studies indicate that anhedonia (1) is elevated in samples dependent on a range of substances; (2) typically appears as a consequence of substance abuse or dependence, and diminishes with abstinence; and (3) predicts increased drug cravings and the likelihood of relapse in those attempting abstinence.
Conclusions:
The common experience of anhedonia in substance-dependent populations, and its relationship to relapse, emphasises the importance of developing therapeutic interventions that specifically target anhedonia in the treatment of all substance use disorders.
Introduction
Anhedonia, defined as impaired capacity to experience pleasure (Snaith, 1993), is frequently reported in substance-dependent populations, particularly during and after withdrawal (Hatzigiakoumis et al., 2011). Anhedonia increases the likelihood of relapse in tobacco smokers attempting to quit (Cook et al., 2010; Leventhal et al., 2009), and positively correlates with drug cravings in detoxified alcohol- (Martinotti et al., 2008a, 2008b) and opioid-dependent (Janiri et al., 2005; Martinotti et al., 2008a) users, as well as recently abstinent tobacco smokers (Cook et al., 2004; Leventhal et al., 2009). This suggests that it may be a key obstacle to recovery from substance dependence. However, the mechanisms by which anhedonia influences craving and relapse remain largely unexamined. The nature of the causal and temporal relationships between anhedonia and substance use disorders remains an important, but largely unexamined question. The issue of whether anhedonia typically precedes the development of a substance use disorder, perhaps conferring vulnerability to addiction, or instead is a consequence of protracted substance use, perhaps abating with sufficient abstinence, has important clinical implications. While very few studies have directly addressed this question in humans, preclinical animal models suggest that reward responsiveness is chronically reduced following withdrawal from prolonged administration of alcohol (Schulteis et al., 1995), amphetamine (Cryan et al., 2003; Lin et al., 1999; Paterson et al., 2000; Wise and Munn, 1995), cocaine (Ahmed et al., 2002; Kenny et al., 2003; Markou and Koob, 1991), nicotine (Epping-Jordan et al., 1998; Skjei and Markou, 2003) and phencyclidine (Spielewoy and Markou, 2003).
While reward responsiveness typically recovered to baseline levels following extended abstinence, several of these studies found that increased dose or duration of drug administration resulted in larger (Ahmed et al., 2002; Lin et al., 1999; Markou and Koob, 1991; Schulteis et al., 1995) or longer-lasting (Ahmed et al., 2002; Lin et al., 1999; Markou and Koob, 1991; Skjei and Markou, 2003; Spielewoy and Markou, 2003) decline in reward responsiveness. Nevertheless, it is unclear how strongly these results can be generalised to human substance use disorders, and these studies do not shed light on the question of whether individual differences in anhedonia prior to drug administration influence drug use outcomes.
Although substance-dependent populations exhibit elevated rates of psychopathology (including mood disorders) associated with anhedonia (Grant et al., 2004), it is unlikely that psychiatric comorbidity alone can account for the elevated levels of anhedonia, and its associations with craving, relapse and other clinical characteristics, in these populations. A range of relevant studies have excluded participants with non-substance-related psychiatric diagnoses (see Table 1), but have nevertheless found elevated levels of anhedonia, correlational or predictive relationships between anhedonia and craving or changes in anhedonia levels over time, consistent with anhedonia having an important role in substance use disorders independent of its relationship with other psychiatric disorders. Therefore, research on the role of anhedonia in substance use disorders cannot be limited to examining comorbidity between substance use disorders and other general psychiatric categories (such as depression) where anhedonia is commonly experienced, but must instead seek to measure and analyse anhedonia as a specific construct. This review aims to examine the growing body of research that has taken this approach. There has been no systematic review of such findings to date, particularly in terms of synthesising results across substance classes.
Characteristics of the studies included in this review.
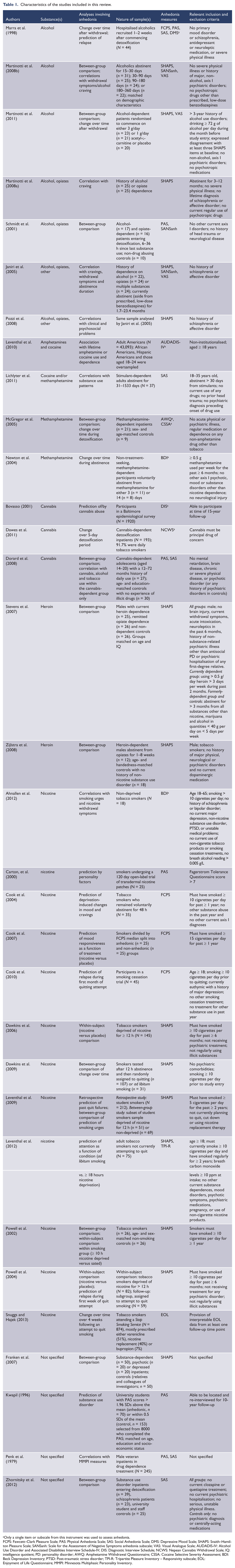
Only a single item or subscale from this instrument was used to assess anhedonia.
FCPS: Fawcett–Clark Pleasure Scale; PAS: Physical Anhedonia Scale; SAS: Social Anhedonia Scale; DMS: Depressive Mood Scale; SHAPS: Snaith–Hamilton Pleasure Scale; SANSanh: Scale for the Assessment of Negative Symptoms anhedonia subscale; VAS: Visual Analogue Scale; AUDADIS-IV: Alcohol Use Disorder and Associated Disabilities Interview Schedule-IV; DIS: Diagnostic Interview Schedule; NCWS: Nepean Cannabis Withdrawal Scale; IQ: intelligence quotient; PD: personality disorder; AWQ: Amphetamine Withdrawal Questionnaire; CSSA: Cocaine Selective Severity Assessment; BDI: Beck Depression Inventory; PTSD: Post-traumatic stress disorder; TPI-R: Tripartite Pleasure Inventory – Responsivity subscale; EOL: Enjoyment of Life Questionnaire; MMPI: Minnesota Multiphasic Personality Inventory.
The specific aim of this review was to examine the association between anhedonia and the maintenance of, and relapse to, substance use disorders, as well as other clinical correlates of anhedonia across different drug-using populations. A second aim was to examine the time course of anhedonia (i.e. whether it precedes or follows the development of substance dependence and if, and how rapidly, there is recovery of hedonic capacity with abstinence).
Methods
We conducted literature searches on PubMed, PsycINFO and MEDLINE. On each of these three databases, we conducted 12 literature searches on 23 May 2013. Each search incorporated three search terms from the following groups, combined with the Boolean operator AND: (1) anhedonia; (2) either drug, substance, alcohol or nicotine; (3) and either dependence, addiction or abuse. These searches yielded 245 unique, peer-reviewed, English-language reports. Reports were selected for inclusion in this review if they involved investigation of a human sample with a lifetime history of a defined substance use disorder (abuse or dependence) or long-term daily use of addictive substances, and used an instrument (self-report or structured interview) specifically designed to measure anhedonia (defined as reduced pleasure in pleasant activities) or hedonic capacity, or specifically reported analyses of a single-item measure of anhedonia from a larger instrument. Review articles and reports that only included samples composed entirely of participants with current, primary, non-substance-related psychiatric disorders were excluded. Application of these criteria allowed the inclusion of 27 articles. An additional five empirical studies meeting the inclusion criteria were identified from the reference list of these articles. Thus, we included a total of 32 articles in this review (see Table 1).
Results
Measures of anhedonia in the studies included in the review
The scales most commonly used to measure anhedonia in the identified studies were the Physical Anhedonia Scale (PAS) and Social Anhedonia Scale (SAS; Chapman et al., 1976), the Fawcett–Clark Pleasure Scale (FCPS; Fawcett et al., 1983) and the Snaith–Hamilton Pleasure Scale (SHAPS; Snaith et al., 1995). The PAS and SAS are intended to measure anhedonia experienced in physical pleasures and interpersonal activities, respectively, as a long-standing personality trait, and the validity of this has been supported in a substance-dependent population (Penk et al., 1979). While these scales are reported to have good indices of reliability and are moderately correlated with each other (Chapman et al., 1976; Penk et al., 1979), there are mixed views on their construct (convergent and discriminant) validity. The items of both scales have been criticised for their cultural and class bias, and the SAS appears to partly measure social adjustment, affiliativeness and anxiety, rather than anhedonia specifically (D’Haenen, 1996; Franken et al., 2007; Leventhal et al., 2006; Peterson and Knudson, 1983). As they are designed to measure trait anhedonia, they may be more valid for use in long-term longitudinal studies where anhedonia is assessed as a predictor of later substance dependence (e.g. Kwapil, 1996), rather than in studies assessing anhedonia, or its change over time, during specific states (e.g. substance dependence, withdrawal, abstinence).
The FCPS and SHAPS, unlike the PAS and SAS, are designed to measure state anhedonia, and may therefore be more suited to studies of change over time in anhedonia, and of the association of anhedonia with specific states (such as withdrawal). Both the FCPS (D’Haenen, 1996; Fawcett et al., 1983) and the SHAPS (Franken et al., 2007) have been shown to have excellent reliability, though this has only been assessed specifically in a substance-dependent population for the SHAPS. Both have been found to correlate moderately with the PAS in some samples (Fawcett et al., 1983; Franken et al., 2007), but not others (Leventhal et al., 2006). They both also show good indices of convergent and discriminant validity, and their items (particularly those of the SHAPS) show less cultural, class and age bias than the PAS and SAS (Leventhal et al., 2006). Some studies used single-item measures of anhedonia, such as visual analogue scales (VAS), to measure general hedonic capacity, or anhedonia items from larger symptom scales (e.g. the ‘loss of pleasure’ item from the Beck Depression Inventory (BDI; Beck et al., 1961), and the loss of interest/pleasure items from the major depression assessment modules included in various structured interview instruments based on the Diagnostic and Statistical Manual of Mental Disorders (DSM; American Psychiatric Association, 1980, 1994)). Some studies have used subscales of larger instruments, particularly the anhedonia/asociality subscale of the Scale for the Assessment of Negative Symptoms (SANSanh; Andreasen, 1982), though given that this subscale is intended to measure a mixture of constructs (anhedonia and asociality), it is not clear whether it is valid to present it as a measure of anhedonia specifically, as some included studies appear to do.
Alcohol
We identified six studies addressing anhedonia and alcohol dependence. Only one compared alcohol-dependent participants to non-substance-dependent controls. Alcohol-dependent patients showed significantly elevated anhedonia 6–36 h after their last drink, as indexed by the PAS and SANSanh, relative to controls (Schmidt et al., 2001).
Four studies addressed the question of change in anhedonia over time in recently detoxified, alcohol-dependent patients. Two of these studies, both of which used the SHAPS as their primary measure of anhedonia, found results consistent with a reduction in levels of anhedonia with increasing duration of abstinence (Martinotti et al., 2008b; Martinotti et al., 2011). Indeed, Martinotti et al. (2011) found that this reduction in anhedonia could be significantly accelerated by daily treatment with acetyl-
Three studies examined correlations between anhedonia, craving and withdrawal symptoms in abstinent, alcohol-dependent participants. Withdrawal symptoms were positively correlated with anhedonia as measured by the SANSanh (Janiri et al., 2005; Martinotti et al., 2008b), SHAPS (Martinotti et al., 2008b) and single-item VAS for hedonic capability (Janiri et al., 2005). Martinotti et al. (2008a, 2008b) also reported that anhedonia, as measured by both the SANSanh and SHAPS, was positively correlated with self-reported craving for alcohol, though Janiri et al. (2005) reported non-significant correlations between these measures. Martinotti et al. (2008a, 2008b) examined participants with a more restricted range of abstinence duration than the Janiri et al. (2005) sample. Marra et al. (1998) did not find any significant relationship between baseline anhedonia and a likelihood of relapse to alcohol abuse or dependence at the 2- or 6-month follow-up.
Amphetamines and cocaine
We identified four studies that examined anhedonia in participants dependent on amphetamines or cocaine. Two studies assessed anhedonia daily during periods of abstinence in methamphetamine-dependent samples and both found declines in anhedonia after several days of abstinence. McGregor et al. (2005) found that anhedonia, as assessed by single items from the Amphetamine Withdrawal Questionnaire and a modified version of the Cocaine Selective Severity Assessment, was elevated in methamphetamine-dependent inpatients relative to non-substance-dependent controls during the first 7–10 days of abstinence, but declined over this period, and then remained at similar levels to those reported by controls for the remainder of the 21-day observation period. Newton et al. (2004) found that methamphetamine-dependent participants who voluntarily abstained showed significantly elevated ratings on the anhedonia item of the BDI on the first and second day of abstinence. Anhedonia ratings normalised on the third day and remained low in those participants who were still abstinent when tested after 12–14 days of abstinence. Consistent with these reports, Lichlyter et al. (2011) reported that SAS scores in participants dependent on methamphetamine or cocaine who had been abstinent for at least 30 days were similar to normative scores reported for this instrument.
Lichlyter et al. (2011) also found no significant correlations between SAS scores and duration of abstinence (which ranged from 31 to 1533 days), latency from first use to first regular use or history of treatment-seeking. Thus, if such relationships exist, they may dissipate along with the anhedonia itself. Nevertheless, in a large population survey, Leventhal et al. (2010) found that lifetime prevalence of a period of at least 2 weeks of anhedonia (assessed with an item from the Alcohol Use Disorder and Associated Disabilities Interview Schedule) was associated with an approximately two- to threefold increase in the likelihood of lifetime cocaine or amphetamine use, after adjusting for lifetime experience of depressed mood and demographic, psychiatric and non-stimulant drug use measures. Among those who reported any lifetime amphetamine or cocaine use, anhedonia was associated with a two- to threefold increase in the likelihood of dependence on the drug. However, the cross-sectional nature of this study leaves unanswered questions regarding the temporal and causal nature of the relationship between anhedonia and stimulant dependence.
Cannabis
We identified three studies that examined the associations between anhedonia and cannabis use disorder. Two incorporated longitudinal designs and found results consistent with cannabis abuse playing a causal role in the emergence of anhedonia. Bovasso (2001) assessed anhedonia – using a single item from the National Institute of Mental Health Diagnostic Interview Schedule – and cannabis abuse in a Baltimore epidemiological survey conducted in 1980, and repeated these assessments in participants who were followed up during the period 1994–1996. Among participants who reported no lifetime depressive symptoms at baseline, those who were diagnosed with lifetime cannabis abuse at baseline were four times more likely than those with no baseline cannabis abuse to report having experienced at least one period of anhedonia lasting at least 2 weeks at any time during the 15-year follow-up period. On the other hand, in participants with no baseline cannabis abuse, baseline anhedonia did not significantly predict occurrence of cannabis abuse during the follow-up period.
Complementing the findings by Bovasso (2001), Dawes et al. (2011) found that abstinence from cannabis was associated with a decline in anhedonia. During their first day of inpatient withdrawal from cannabis, 62.9% of their cannabis-dependent participants reported experiencing at least some anhedonia (score > 1 on a VAS where scores ranged from 0 to 5 for an item worded ‘No matter how I try, I have not been able to find enjoyment in things’). By their fifth day, only 19.8% of inpatients reported anhedonia. Median VAS ratings dropped from 1.7 to 0 over this period.
Further supporting the presence of anhedonia in cannabis dependence, Dorard et al. (2008) found that cannabis-dependent adolescents and young adults recorded significantly higher PAS and SAS scores than controls with no experience of illicit drugs. PAS (but not SAS) scores discriminated significantly between cannabis-dependent and control participants after statistically controlling for depression, anxiety, alexithymia and sensation-seeking. Within the cannabis-dependent group, correlations between anhedonia measures and measures of cannabis, alcohol and tobacco use patterns did not reach significance.
Heroin and other opioids
We identified five studies meeting the inclusion criteria that examined anhedonia in opioid-dependent samples. Three compared opioid-dependent participants to non-substance-abusing controls. While Stevens et al. (2007) found that participants with either current or remitted heroin dependence reported significantly higher levels of anhedonia than controls, as measured by the SHAPS, Zijlstra et al. (2008) found no significant difference between the SHAPS scores of recently detoxified, heroin-dependent participants and controls. This may have been due to the smaller groups in the study by Zijlstra et al. (2008) compared to the groups in the study by Stevens et al. (2007), or the inclusion, by Zijlstra et al. (2008), of only tobacco smokers in both groups, which did not appear to be the case in the study by Stevens et al. (2007). Schmidt et al. (2001) found that opioid-dependent patients assessed 6–36 h after their last substance use showed significantly elevated SANSanh, but not PAS, scores relative to controls.
Two studies examined the correlations between anhedonia and cravings in abstinent, opiate-dependent participants. Both found that drug cravings were positively associated with anhedonia as measured by either the SHAPS or SANSanh (Janiri et al., 2005; Martinotti et al., 2008a). Janiri et al. (2005) also found that withdrawal symptoms were positively correlated with anhedonia. Duration of abstinence was negatively correlated with anhedonia, suggesting a decline in anhedonia over time with successful abstinence, although the use of a cross-sectional design in the study by Janiri et al. (2005) limits this interpretation.
Nicotine
We identified 12 articles that examined anhedonia in tobacco smokers. Five studies examined groups trying to quit smoking. An additional five studies examined the effects of short-term nicotine deprivation in smokers not attempting to quit. One studied the acute effect of nicotine on non-deprived smokers, while another examined the correlations between anhedonia and withdrawal symptoms and smoking urges in non-deprived smokers. The main findings that emerge from these studies are that anhedonia increases during short-term nicotine deprivation and then declines with increased duration of successful abstinence. Anhedonia predicts greater declines in positive affect and responsiveness to pleasant stimuli, and greater cravings, following nicotine deprivation, and increased likelihood of relapse in those attempting to quit.
As little as 10–12 h of nicotine deprivation increases anhedonia in tobacco smokers relative to their non-deprived state (Dawkins et al., 2006; Powell et al., 2002, 2004), though the SHAPS scores of smokers did not differ significantly from non-smoking controls, whether or not smokers were deprived of tobacco (Powell et al., 2002). Nicotine deprivation also caused reductions in colour-naming errors for pleasant versus neutral words on an emotional Stroop test, indicating reduced attention to the pleasant words (Dawkins et al., 2006; Powell et al., 2004), consistent with the decreased sensitivity to pleasant stimuli that defines anhedonia. In a study where smokers were randomly assigned to an attempt to quit or continue ad libitum smoking after 12 h of abstinence, Dawkins et al. (2009) found that, among the 30.8% of the group assigned to quitting who successfully abstained for the duration of the 3-month follow-up period, anhedonia declined significantly by the 1-week follow-up assessment and did not change significantly thereafter (at the 1- and 3-month follow-ups). At all follow-ups, their SHAPS scores did not differ significantly from the ad libitum smoking group.
Similarly, using the Enjoyment of Life Questionnaire, a three-item measure adapted from the SHAPS, Snuggs and Hajek (2013) found that the 66.9% of their participants who remained abstinent for 1 week reported significantly greater ability to experience pleasure than before quitting. This improvement was significantly larger than that reported by those who lapsed, who did not report a significant change in pleasure. The 22.4% of participants still abstinent after 4 weeks reported a further significant increase in pleasure experience.
While anhedonia increases after tobacco deprivation, the degree to which anhedonia is already present prior to deprivation also predicts other affective effects of tobacco deprivation. Higher anhedonia, as measured by the FCPS prior to tobacco deprivation, predicted greater reductions in positive affect, as measured by the Profile of Mood States, after 24 h of abstinence (Cook et al., 2004). Similarly, higher pre-deprivation anhedonia predicted reduced attention to pleasant stimuli after nicotine deprivation. Leventhal et al. (2012) used a modified Stroop test in which participants were presented with images of faces expressing either happiness, anger, fear, surprise or a neutral expression. Attention to happy faces – indexed by the speed, relative to the neutral faces, with which participants could identify a face’s gender – was not related to SHAPS scores in non-deprived smokers. However, after 18 h of tobacco deprivation, greater pre-deprivation anhedonia scores predicted reduced attention to happy (but not other emotional) faces, suggesting that a relationship between anhedonia and reduced attention to pleasant stimuli was ‘unmasked’ by tobacco deprivation.
Anhedonia also appears to interact with the impact of nicotine on affective processes even in non-deprived smokers. Cook et al. (2007) allowed smokers to smoke one of their own cigarettes, to ensure they were not in a nicotine-deprived state, 10 min prior to a positive mood induction during which participants smoked an additional experimental cigarette (either denicotinised or containing 1 mg nicotine). In participants with anhedonia below the median (as measured by the FCPS), this induction led to a sustained positive mood, as measured by the Positive and Negative Affect Schedule, regardless of whether or not the experimental cigarette contained nicotine. However, in participants with anhedonia scores above the median, only the nicotine-containing cigarette allowed a sustained positive mood response, suggesting that higher levels of anhedonia conferred a greater need to maintain high nicotine levels to allow the experience of pleasant affect.
These relationships between pre-deprivation anhedonia and affective changes during deprivation may help explain the predictive relationships between anhedonia and cravings and relapse found in several studies. Higher pre-deprivation anhedonia predicted an increased effect of 12-h tobacco deprivation on appetitive, but not aversive, smoking urges (Leventhal et al., 2009), and increased tobacco cravings after 24 h of abstinence (Cook et al., 2004). Cook et al. (2004) found that this increase in cravings was significantly mediated by a change in positive, but not negative, affect. Anhedonia predicted reduced positive affect between baseline and 24 h, and the reduced positive affect over this interval predicted increased cravings. Snuggs and Hajek (2013) found that increased pleasure experience was significantly associated with less urge to smoke and, more generally, with reduced withdrawal symptom severity, at both 1 and 4 weeks after quitting. However, scores on the BDI anhedonia item were not significantly correlated with urges to smoke or withdrawal symptoms in non-deprived smokers (Ahnallen et al., 2012). As with relationships between anhedonia and attention, this suggests that deprivation is required to ‘unmask’ associations between anhedonia and cravings.
Leventhal et al. (2009) also found that higher anhedonia, as measured by the SHAPS, predicted more self-reported, past failed quit attempts and a higher proportion of past quit attempts that ended with < 24 h of abstinence. One prospective study also supported this relationship between anhedonia and relapse. In currently euthymic tobacco smokers with a history of major depressive disorder, Cook et al. (2010) found that, after controlling for age, number of cigarettes smoked daily and pre-quit depressive symptom severity, higher anhedonia predicted earlier relapse (defined as 7 days consecutive smoking) during the first month of a quit attempt. When participants were divided according to FCPS score median split, less than 40% of the low-anhedonia group relapsed during the month, while over 80% of the high-anhedonia group relapsed.
While these studies suggest that higher pre-quit anhedonia levels increase the risk of relapse, there is no evidence that the acute post-quit increase, or subsequent decline, in anhedonia predicts relapse. Powell et al. (2004) found that the effect of 12-h nicotine deprivation on SHAPS scores did not significantly predict successful abstinence 1 week after being assigned to quit smoking. Snuggs and Hajek (2013) found that the degree of change in enjoyment of life after 1 week of abstinence did not significantly predict whether participants would still be abstinent 3 weeks later. It should be noted that the definition of relapse used by Powell et al. (2004) and Snuggs and Hajek (2013) – any smoking within the follow-up period – differed from that of Cook et al. (2010) – 7 days of consecutive smoking.
Multiple or unspecified substances
We identified six studies that either did not specify a particular substance under investigation (e.g. investigated ‘substance dependence’ in general), investigated samples described as poly-substance-dependent or reported data on samples composed of a mixture of participants dependent on different substances. Two compared substance use disorder patients in treatment to healthy controls. Franken et al. (2007) found significantly elevated anhedonia in inpatients being treated for substance dependence compared to general population controls. The SHAPS scores of substance-dependent participants were similar to those found in inpatients being treated for psychosis, but were significantly lower than in inpatients being treated for depression. Abnormally high anhedonia, as indicated by disagreement with three or more SHAPS items, was found in 2% of the general population sample, 32% of substance-dependent patients, 45% of psychotic patients and 75% of depressed patients. Zhornitsky et al. (2012) did not find a significant difference between the SAS scores of patients with substance use disorders entering detoxification treatment and controls.
Three reports examined correlates of anhedonia in abstinent, substance-dependent samples. In male military veteran inpatients of a drug dependence treatment programme – approximately 70% of whom were primarily heroin-dependent, with most of the rest primarily dependent on amphetamines and barbiturates – anhedonia, as measured by both the PAS and SAS, correlated positively with Minnesota Multiphasic Personality Inventory measures of social maladjustment, confused thinking, depression, poor morale and poor health (Penk et al., 1979). In participants with a history of poly-substance dependence, Janiri et al. (2005) found that drug cravings and duration of abstinence were not significantly correlated with scores on the SANSanh, SHAPS or VAS for hedonic capacity. However, in a separate analysis of 13 participants (including five with a history of opioid dependence, four with a history of alcohol dependence and four from the poly-substance-dependent group) identified as highly anhedonic due to their disagreement with three or more SHAPS items, all three anhedonia measures were positively correlated with craving and withdrawal symptom severity, and negatively correlated with abstinence duration, with the exception of correlations between SHAPS and withdrawal scales. In a sample of abstinent participants including 22 with a history of alcohol dependence, 24 with a history of opioid dependence and 24 with a history of poly-substance dependence, Pozzi et al. (2008) reported that associations between SHAPS scores and measures of medical, social, substance-related, legal and psychological problems in the past 30 days were either weak or absent.
One longitudinal study examined the relationship between anhedonia and later substance use disorder. Kwapil (1996) selected groups from a larger sample of 8000 university students who had been administered the PAS. One group included participants who scored at least 1.96 SDs above the mean PAS score (the physical anhedonia group) while another included participants whose scores were within 0.5 SDs of the mean (controls). Participants were followed up between 8.8 and 14.5 years later to assess whether they met the criteria for any substance use disorder at any time in the intervening period. Kwapil (1996) found that the anhedonic group had a slightly (but non-significantly) lower probability of developing a substance use disorder than controls.
Discussion
The studies included in this review highlight the prevalence and elevated levels of anhedonia in substance-dependent samples and indicate that frequent use of addictive substances contribute to the experience of anhedonia. While anhedonia is frequently associated with cravings and relapse, the studies reviewed here suggest that anhedonia does abate following sustained abstinence, and could therefore be considered as symptomatic of a current, or very recent, substance use disorder. The following sections discuss the findings from this systematic review in greater detail.
Presence of anhedonia in substance use disorders
Of the 32 publications reviewed, eight compared anhedonia in samples with current or past substance dependence to non-substance-dependent controls. Of these, five found evidence for elevated anhedonia in substance-dependent samples, including samples with current alcohol (Schmidt et al., 2001), cannabis (Dorard et al., 2008), methamphetamine (McGregor et al., 2005) and opioid (Stevens et al., 2007) and remitted opioid (Stevens et al., 2007) dependence. Measures used in these studies included the PAS, SHAPS and several single-item measures of anhedonia. Although Schmidt et al. (2001) and Zijlstra et al. (2008) did not find significant differences between their opioid-dependent participants and controls, both studies had smaller samples than the study by Stevens et al. (2007), and may have been underpowered.
Temporal relationship between anhedonia and substance use disorders
Longitudinal studies across a range of addictive substances indicate a decline in anhedonia following abstinence, though there may be differences between substances in the duration of the anhedonia experienced. For nicotine (Dawkins et al., 2009; Snuggs and Hajek, 2013), cannabis (Dawes et al., 2011) and methamphetamine (McGregor et al., 2005; Newton et al., 2004), anhedonia appears to decline substantially within the first week of abstinence, while in an alcohol-dependent sample, anhedonia continued to remain high after 10 days of abstinence and did not substantially reduce until after 30 days (Martinotti et al., 2011). This highlights the importance of conducting further longitudinal studies with samples dependent on other substances (e.g. opioids, cocaine, benzodiazepines), because time courses cannot be assumed to generalise across substances and the rate of recovery of hedonic responsiveness is likely to be a clinically relevant issue.
Reduction in anhedonia over time with abstinence is consistent with anhedonia being a reversible impairment induced by regular use of addictive substances, rather than a premorbid risk factor for the development of substance abuse. Indeed, only two longitudinal studies have examined whether anhedonia is a premorbid risk factor (Bovasso, 2001; Kwapil, 1996). Neither found support for anhedonia playing such a role, though Bovasso (2001) found that cannabis abuse did predict later anhedonia, adding further support to the conclusion that anhedonia can arise as a result of substance abuse.
Relationship between anhedonia and withdrawal, cravings and relapse
Fourteen of the papers reviewed reported data on the clinical correlates and consequences of anhedonia in substance-dependent samples. Anhedonia was found to correlate positively with withdrawal symptom severity in abstinent, alcohol- (Martinotti et al., 2008b) and opioid-dependent participants (Janiri et al., 2005). However, the validity of assessing ‘withdrawal’ symptoms several months after detoxification, as was the case for all of the participants in the Janiri et al. (2005) study and for the majority of participants in the Martinotti et al. (2008b) study, is questionable. Positive correlations between anhedonia and substance cravings have been reported in abstinent, alcohol- (Martinotti et al., 2008a, 2008b) and opioid-dependent (Janiri et al., 2005; Martinotti et al., 2008a) samples. Together with findings that anhedonia correlates with measures of social maladjustment, confused thinking, depression, poor morale and poor health in substance-dependent inpatients (Penk et al., 1979), these reports suggest that elevated levels of anhedonia are associated with numerous factors that could make recovery from substance dependence more difficult.
Anhedonia may be a prospective predictor of abstinence-related cravings as well as a correlate (Cook et al., 2004; Leventhal et al., 2009). This may reflect an increased desire among more highly anhedonic individuals to use substances specifically to facilitate experiences of positive affect. In tobacco smokers, higher levels of anhedonia predict greater loss of affective (Cook et al., 2007) and attentional (Leventhal et al., 2012) responses to pleasant stimuli, and greater declines in general positive affect (Cook et al., 2004) in the absence of nicotine. The prospective predictive relationship between anhedonia and cravings appears to be mediated by this loss of positive affect, but not by changes in negative affect (Cook et al., 2004). Moreover, anhedonia specifically predicts appetitive smoking urges (urges related to expectation of pleasure from tobacco use), but not aversive smoking urges (urges related to anticipated relief from negative affect), during nicotine deprivation (Leventhal et al., 2009). On the other hand, even smokers with high anhedonia scores may show normal responsiveness to pleasant stimuli when non-deprived (Cook et al., 2007; Leventhal et al., 2012). Thus, the reason some smokers report higher levels of anhedonia may not be due to a constantly present state of anhedonia, but instead a more rapid emergence of anhedonia when their nicotine levels decline, and therefore more frequent (if brief) periods of anhedonia when they are unable to maintain sufficiently high nicotine levels to allow normal hedonic responsiveness. It is important to replicate these findings in samples dependent on other substances.
The relationship between anhedonia and craving imply that higher levels of anhedonia may lead to a higher risk of relapse during attempted abstinence. However, empirical evidence for this is mixed. Leventhal et al. (2009) found that increased levels of anhedonia predicted more past failed quit attempts and a higher proportion of quit attempts that ended with relapse after less than 24 h. Cook et al. (2010) found a substantial effect of pre-quit anhedonia on the likelihood of relapse over a 1-month, post-quit follow-up period. However, the findings by Leventhal et al. (2009) are weakened by their reliance on retrospective recall of past quit attempts, and attempting to relate these to current state anhedonia. The inclusion, by Cook et al. (2010), of only smokers with a history of depression (although they were euthymic at the time of their participation in the study) may limit the generalisability of these findings.
Studies that measured baseline anhedonia after cessation of tobacco (Powell et al., 2004; Snuggs and Hajek, 2013) or alcohol (Marra et al., 1998) use found no predictive relationship between anhedonia and relapse. However, the very limited follow-up period (1 week) in the study by Powell et al. (2004) may not have been long enough to detect a relationship between anhedonia and relapse. By the time Snuggs and Hajek (2013) first measured anhedonia, 1 week after their participants quit smoking, 33.1% of their original sample had already lapsed, potentially biasing results. Further difficulties in interpretation relate to different criteria used to index relapse, including 7 days of consecutive use (Cook et al., 2010), any use at all (Powell et al., 2004; Snuggs and Hajek, 2013) or meeting DSM (third edition, revised) criteria for abuse or dependence (Marra et al., 1998). Different indices of relapse may be differentially sensitive to anhedonia; future studies could help clarify this question by analysing and presenting multiple indices of relapse over extended follow-up periods.
The most important difference between these studies, however, may be the time at which anhedonia was measured. The two studies that measured anhedonia while their participants were currently using their substance of dependence (nicotine in both cases) both reported a significant predictive relationship between anhedonia and relapse, while all three studies reporting negative findings measured anhedonia during abstinence. Thus, anhedonia while actively dependent may be more relevant to the risk of relapse than the degree of change in anhedonia following withdrawal.
Treatment of anhedonia in substance-dependent populations
Remarkably, only one study was found that investigated the treatment of anhedonia in substance dependence. Martinotti et al. (2011) found that daily intravenous treatment with acetyl-
There is a sizeable animal literature reviewed by Paterson and Markou (2007) suggesting that a range of chemicals, most of which are currently applied as antidepressants in humans, may attenuate anhedonia during substance withdrawal. Treadway and Zald (2011) suggest that behavioural activation may be a behavioural psychotherapeutic approach particularly suited to overcoming anhedonia, suggesting that studies using this approach among individuals with substance dependence should be pursued. Determining whether successful amelioration of anhedonia reduces cravings and relapse rates would also help to clarify whether anhedonia has a causal relationship with relapse or is simply a correlate of other factors that determine cravings and relapse.
Limitations of the current literature
Several limitations of the current literature were identified in this review. It is noteworthy how few studies examined the association between anhedonia and relapse in samples attempting to cease substance use. Only one of these four studies investigated a substance other than nicotine and only one analysed time to relapse. This represents a field with important clinical implications that deserves much more research attention. It is also remarkable how few studies examined the temporal and causal relationships between the development of substance dependence and anhedonia. Studies that examined the relationship between duration of abstinence and anhedonia using cross-sectional designs (Janiri et al., 2005; Martinotti et al., 2008b) or that used longitudinal designs but only examined successfully abstinent participants in samples with a high relapse rate (Dawkins et al., 2009; Snuggs and Hajek, 2013) are vulnerable to bias if those with higher levels of anhedonia are more likely to relapse earlier, and thus represent a lower proportion of those participating at later time points.
Lack of statistical control of potentially confounding variables, failure to report such variables in descriptions of sample characteristics or lack of matching groups on such variables, where relevant, limit the interpretation of many of these studies, including most of the reports of elevated anhedonia in substance-dependent samples (Dorard et al., 2008; Franken et al., 2007; Schmidt et al., 2001; Stevens et al., 2007). In addition, tobacco use is a key potential confounding variable in studies of samples dependent on substances other than nicotine. While several studies reported on samples described as abstinent from all addictive substances, they did not clarify whether this included nicotine; given the high rates of tobacco smoking in substance-dependent populations, it is unlikely that this is the case. However, as shown by this review, nicotine use is likely to impact on anhedonia and is therefore likely to be a hidden confounding variable in many of the studies reviewed.
The majority of the studies included in this review controlled for the potentially confounding effect of psychiatric comorbidity on anhedonia by excluding participants with current (and, in some cases, lifetime) mood and psychotic disorders (see Table 1). Two large population surveys (Bovasso, 2001; Leventhal et al., 2010) used the alternative approach of statistically controlling for the presence of such disorders in their analyses. However, a minority of reports either did not specify relevant psychiatric characteristics of their samples or whether they used psychiatric exclusion criteria (see Table 1). To aid the interpretation of the validity, meaning and generalisability of their findings, future studies should ensure that relevant psychiatric exclusion criteria are clearly reported. Where relevant, psychiatric characteristics, along with tobacco use and potentially confounding demographic factors such as age, sex, intelligence quotient and socio-economic characteristics, should be clearly reported and statistically controlled for if possible. In studies involving between-group comparisons, it would be ideal to match groups as closely as possible on such variables.
Conclusions
Overall, these findings suggest a number of commonalities across different addictive substances in the nature of the association between anhedonia and substance dependence. First, there is evidence for elevated levels of anhedonia among individuals dependent on alcohol, cannabis, methamphetamine and opioids. Second, studies of alcohol, cannabis, methamphetamine and nicotine-dependent samples highlight that anhedonia reduces over time with successful abstinence. Finally, anhedonia has been shown to correlate with other aspects of abstinence (such as duration of abstinence, craving and withdrawal symptoms) in studies of alcohol, nicotine and opioid-dependent populations. These findings emphasise the importance of addressing anhedonia in the treatment of substance dependence, and highlight the need for targeted interventions within clinical settings.
Footnotes
Funding
This research was supported by a grant from the National Health and Medical Research Council of Australia (1006749). Professor Yücel is supported by a National Health and Medical Research Council Fellowship Award (1021973).
Declaration of interest
The authors report no conflicts of interest. The authors alone are responsible for the content and writing of the paper.
