Abstract
Keywords
Introduction
Mental illnesses are prevalent in today’s society, with almost half of the Australian adult population experiencing one or more mental disorder(s) at some stage in their life (Slade et al., 2009). Deinstitutionalisation of the mentally ill aimed to improve integration with the rest of the community, but has resulted in many patients being admitted into correctional facilities instead (Baillargeon and Contreras, 2001; Buscema et al., 2000). Around the world, prisons may now be considered among the main centres for treatment of the mentally ill, despite the environment being the antithesis of everything required (Bressington et al., 2008; Buscema et al., 2000; Erickson et al., 2007; Gray et al., 2008; Lund et al., 2002). The correctional facility environment may also result in the development of disorders, especially insomnia and anxiety (Elger et al., 2002; Feron et al., 2005; Lekka et al., 2003).
Psychotropic drugs may be used to manage the symptoms of mental illnesses (Koda-Kimble et al., 2009; Psychotropic Expert Group, 2008; Rossi, 2009). Without such medications, the incidence of suicide, relapse and violent behaviour all markedly increase (Erickson et al., 2007; Herings and Erkens, 2003). A low rate of adherence to prescribing guidelines for psychotropes has consistently been identified in hospitals, community mental health centres and nursing homes (Byrne, 2008; Gisev et al., 2006; Goldney and Bain, 2006; Greve and O’Connor, 2005; Knott and Ibister, 2008; Magliano et al., 2004; Meagher and Moran, 2003). These studies found problems such as over- and under-dosing, multiple ‘when required’ (pro re nata, or PRN) orders, prescriptions for two drugs from the same therapeutic class (polypharmacy) and significant drug interactions. All of these issues stem from sub-optimal prescribing and poor patient outcomes may result.
To date, the research on medication use by prisoners has primarily focused on the use of antipsychotic medications, rather than the more encompassing category of psychotropes (Alia-Klein et al., 2007; Baillargeon and Contreras, 2001; Bains and Nielssen, 2003; Bressington et al., 2008; Lund et al., 2002; Martin et al., 2008; Veysey et al., 2007). However, there is a small body of literature on anxiolytics, hypnotics and antidepressants (Elger, 2004; Fos-Claver and Soler-Garcia, 2008; Lekka et al., 2003).
There are several reasons why it was important to determine how psychotropic medications are being prescribed for prisoners, and more specifically if any areas for improvement exist. Firstly, the internationally recognised human rights laws state that prisoners retain their right to be treated with respect and dignity, and therefore should not be subjected to cruel punishment (United Nations High Commissioner for Human Rights, 2007). The right to quality health services is also inherent in this concept (Bruce and Schleifer, 2008). Secondly, psychotropic medications may have severe adverse effects, including blood disorders, neuroleptic malignant syndrome, serotonin toxicity, and hypertensive crisis (Rossi, 2009). Optimal prescribing is required to minimise the risk of iatrogenic morbidity or mortality. Thirdly, time in a correctional facility may be an opportunity to improve the well-being of people who may not have regular contact with health professionals whilst in the community (Feron et al., 2005). Quality health care may improve their quality of life, as well as potentially reducing the risk of reoffending (Gray et al., 2008). For these reasons, it is important that a comprehensive understanding of prescribing practices is obtained. The aim of this review was to compile, evaluate and discuss the literature on the prescribing of psychotropic drugs for prisoners.
Methods
Search strategy and selection criteria
Qualitative and quantitative studies discussing the use of psychotropic medications for prisoners were reviewed using a protocol. The list of medications considered (Appendix 1) consisted of the drugs common to the psychotropic or psychiatric section of three nationally recognised references (Koda-Kimble et al., 2009; Psychotropic Expert Group, 2008; Rossi, 2009). Facilities where prisoners may be treated, such as prisons, jails, and forensic wards or hospitals, were included. A prescribing issue was defined as any practice by a doctor that was not in accordance with guidelines or accepted best practice, or any factor that potentially adversely affected the quality of prescribing. All levels of evidence were accepted, provided the study was methodologically sound.
In the first fortnight of October 2009, the following databases were searched: AMED, AMI, APAIS Health, CINAHL, CINCH-Health, Cochrane Library, DRUG, eMedicine Clinical Knowledge Base, Embase, International Pharmaceutical Abstracts, MEDLINE, Proquest 5000 International, PsycINFO, SCOPUS, and Web of Science. The search terms used were: (psychotrop* OR neurolept* OR psychoacti* OR antipsychot* OR antidepress* OR anxioly* OR hypnot* OR sedati* OR dependence OR mood stabilis*) AND (prison* OR correction* OR jail OR forensic OR gaol OR inmate OR felon OR incarcerate* OR offender* OR penitentiary OR remand OR convict*) AND (prescri*).
The inclusion criteria were: the study focused on adults’ time as prisoners and one or more drugs of interest, and discussed prescribing. The study could be set anywhere in the world, but the full text had to be available in English, as translation services were not available, and published between January 1999 and October 2009. The only immediate exclusion criterion was an inability to access the full text article.
Initial screening was based on title and abstract; full text documents were obtained for the articles appearing to meet the inclusion criteria. Where more than one article was written using the same raw data, both were included if at least one new prescribing issue was raised in the second article. The reference list of every relevant article was screened for potential additional useful articles, and the relevant articles were also searched in Google Scholar, SCOPUS and Web of Science for useful citations. Each of the eight Australian state and territory government correctional services websites and one specialised journal, the Journal of Correctional Health Care, were searched for related research. To minimise publication bias, 23 authors of included articles were emailed requesting further published or unpublished research articles and suggestions for other avenues for investigation.
During the full text assessment, the relevance of each study to the review was considered, as was the level of evidence, potential for bias, and methodological strengths and weaknesses. The latter were assessed using a checklist (Liberati et al., 2009) for qualitative or quantitative studies (CASP, 2006), and using a tool for assessing risk of bias (The Cochrane Collaboration, 2009). Reports were classified as higher or lower quality evidence, based on the methodology. The relatively small body of literature in existence on this topic discouraged exclusion of studies. Consequently, all relevant studies have been included, with notes on the lower-quality studies whose results must be interpreted cautiously.
Data extraction and study validity assessment
The data extraction was conducted on all retrieved articles by one author (EG), and then discussed with a second author for confirmation (JW). Differences in opinion were resolved by discussion. A spreadsheet was created for the collection and collation of the extracted data based on a template (Torgerson, 2003). This was completed twice: data was extracted, and then several days later each article was read again and the information on the spreadsheet was confirmed and augmented. Clarification was sought by email from the corresponding authors of several articles as to whether their study sample included prisoners. There were multiple categories in the data extraction spreadsheet, including referencing details, study setting and design, objective, participants, results, a quality appraisal for strengths and weaknesses, and prescribing issues.
Points arising from the data were coded, and codes were gradually refined and rechecked against original articles to ensure accurate representation of the identified prescribing issues. These were then grouped into themes, and have been reported in accordance with the tenets of the PRISMA Statement (Liberati et al., 2009).
Results
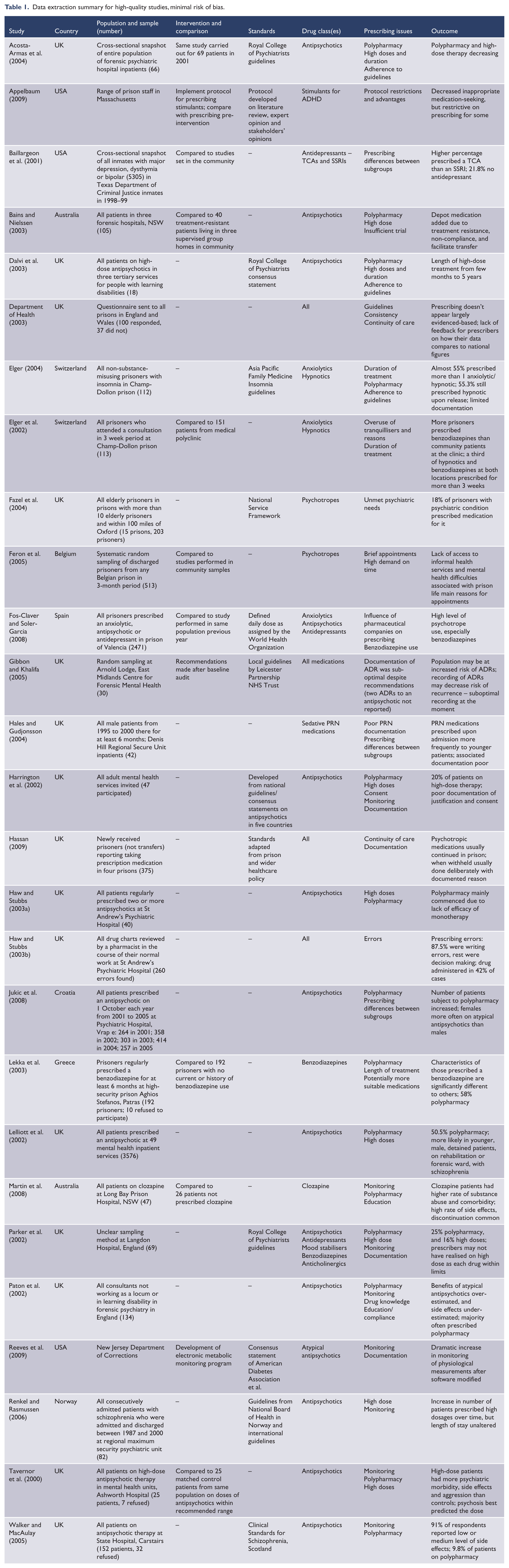
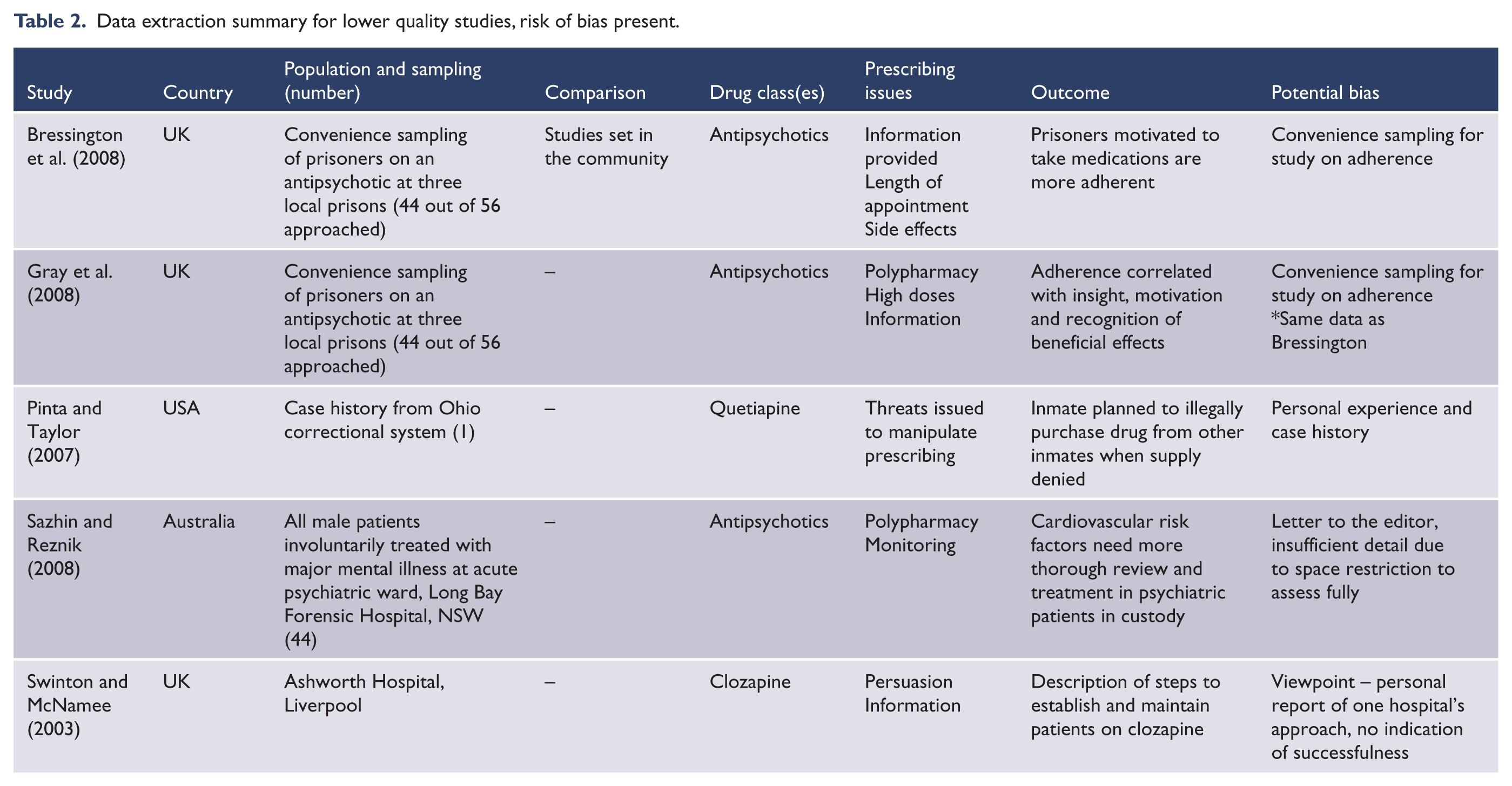
Database searching identified 595 reports (see Figure 1 for flow diagram). Of these, 226 were excluded through duplication, and 342 due to an irrelevant title or abstract. An additional six reports were found using other planned search methods. The full text version of one article was not obtainable. Data was extracted from the final sample of 32 articles (Tables 1 and 2).
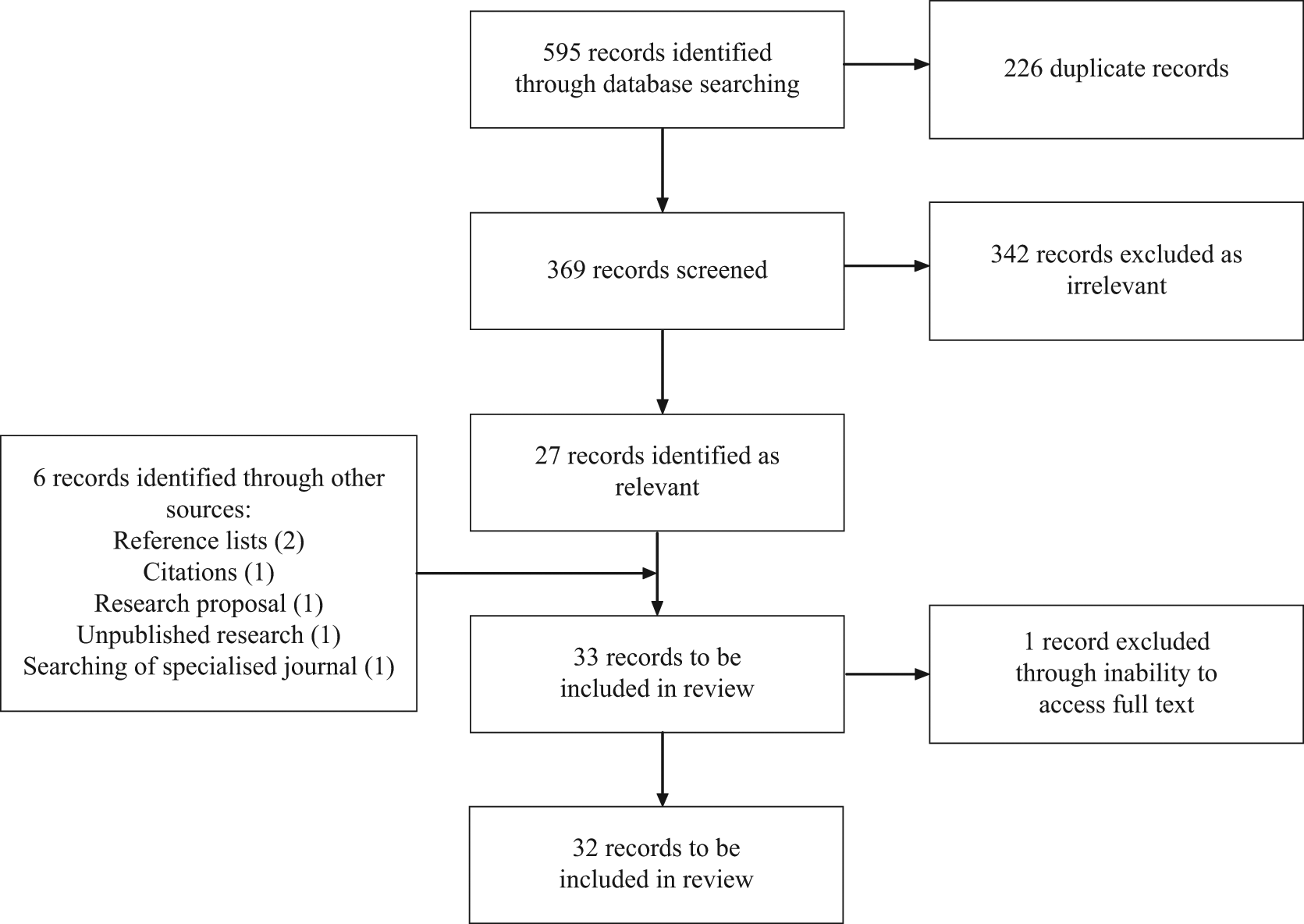
Data search flow diagram.
Data extraction summary for high-quality studies, minimal risk of bias.
Data extraction summary for lower quality studies, risk of bias present.
Identified themes
An extraordinarily high prevalence of mental illness amongst prisoners was noted, and the possible contribution of the setting to this finding, especially for insomnia and anxiety, was suggested in the literature. However, there was often a lack of comparisons in the prevalence of the issues identified between subgroups in the populations, such as between genders, age groups and ethnicities.
Theme one: polypharmacy
The most common theme identified was polypharmacy (Acosta-Armas et al., 2004; Bains and Nielssen, 2003; Bressington et al., 2008; Dalvi et al., 2003; Gray et al., 2008; Harrington et al., 2002; Haw and Stubbs, 2003a; Jukic et al., 2008; Lelliott et al., 2002; Martin et al., 2008; Parker et al., 2002; Paton et al., 2002; Renkel and Rasmussen, 2006; Sazhin and Reznik, 2008; Tavernor et al., 2000; Walker and MacAulay, 2005). Many national and international guidelines state that the use of more than one antipsychotic medication is strongly discouraged in almost all situations (Psychotropic Expert Group, 2008). The incidence and supposed advantages of combining different dosage forms, typically an oral atypical antipsychotic and a depot injection of a typical antipsychotic, were discussed (Bains and Nielssen, 2003; Haw and Stubbs, 2003a; Paton et al., 2002; Renkel and Rasmussen, 2006). Several studies sought practitioners’ justifications for these prescribing decisions; the most common rationalisations were an insufficient response to monotherapy (Bains and Nielssen, 2003; Harrington et al., 2002; Haw and Stubbs, 2003a), concerns about safety (Bains and Nielssen, 2003; Haw and Stubbs, 2003a) and adherence (Bains and Nielssen, 2003; Paton et al., 2002), a desire to leave medications unchanged if patients were reasonably well, and to not contribute to further deterioration if they were not well (Haw and Stubbs, 2003a). Linked to this theme were concerns about the influence of PRN medications, and the total dose of antipsychotic being received.
Polypharmacy of benzodiazepines and hypnotics was identified in two studies. One reported on the use of multiple benzodiazepines (Lekka et al., 2003), the other focused on the practice of combining a benzodiazepine and a hypnotic (Elger, 2004), as some benzodiazepines are indicated for insomnia (Rossi, 2009). This prescribing practice was most commonly found in patients with minimal improvement to their insomnia with one drug (Elger, 2004).
Theme two: high doses
The use of dosages above the maximum recommended daily dose is generally discouraged by guidelines, although some authors advocated their use in certain situations (Brotman and McCormick, 1990). One study found that polypharmacy was the greatest predictor of high-dose therapy, with patients prescribed more than one antipsychotic medication 41 times more likely to be on high doses than those on monotherapy (Lelliott et al., 2002). Although polypharmacy was not always considered, these problems were clearly linked (Acosta-Armas et al., 2004; Harrington et al., 2002; Haw and Stubbs, 2003a; Lelliott et al., 2002; Parker et al., 2002; Renkel and Rasmussen, 2006; Tavernor et al., 2000). PRN medications were also implicated in high dosages (Harrington et al., 2002; Lelliott et al., 2002). Several researchers wondered if prescribers were aware that the patients were on high-dose therapy and whether it was an intentional prescribing decision (Acosta-Armas et al., 2004; Harrington et al., 2002; Haw and Stubbs, 2003a; Parker et al., 2002). Concern was expressed about prescriber awareness of polypharmacy and PRN medications, and also for some patients on antipsychotic monotherapy (Acosta-Armas et al., 2004; Bains and Nielssen, 2003; Gray et al., 2008; Harrington et al., 2002; Haw and Stubbs, 2003a; Lelliott et al., 2002; Renkel and Rasmussen, 2006).
Theme three: duration of treatment
The duration of treatment was a third area of interest. Concern was expressed that there may have been an insufficient trial of monotherapy for patients on an antipsychotic before a second drug was prescribed to supplement the effect (Bains and Nielssen, 2003; Harrington et al., 2002). Patients had long periods of high-dose antipsychotic therapy without official review (Acosta-Armas et al., 2004; Dalvi et al., 2003; Parker et al., 2002).
Long duration of treatment with hypnotics (Elger, 2004; Elger et al., 2002) and benzodiazepines (Lekka et al., 2003) for insomnia was also an area of concern. Short-term therapy is desirable as benzodiazepines have been associated with an increase in hostility and aggression (Lekka et al., 2003).
Theme four: documentation and monitoring
Documentation and monitoring of patients was consistently raised as an area needing improvement (Acosta-Armas et al., 2004; Dalvi et al., 2003; Harrington et al., 2002; Martin et al., 2008; Parker et al., 2002; Reeves et al., 2009; Renkel and Rasmussen, 2006; Sazhin and Reznik, 2008; Swinton and McNamee, 2003; Tavernor et al., 2000). A lack of adherence to relevant guidelines recommending more specialised monitoring for antipsychotics was apparent, especially when high doses were employed (Acosta-Armas et al., 2004; Dalvi et al., 2003; Elger, 2004; Harrington et al., 2002; Parker et al., 2002; Renkel and Rasmussen, 2006). A need for more formalised monitoring of the efficacy of treatment for all psychotropes has been recommended (Elger, 2004; Fos-Claver and Soler-Garcia, 2008; Haw and Stubbs, 2003a; Martin et al., 2008; Swinton and McNamee, 2003). Documentation associated with PRN medications was found to be poor, an area of particular concern as prescribers and nurses may have different understandings of how and when PRN medication is to be used (Hales and Gudjonsson, 2004). Assessment of need for treatment was poorly documented (Elger, 2004; Fazel et al., 2004; Hales and Gudjonsson, 2004). Monitoring for side effects (Bressington et al., 2008; Martin et al., 2008; Tavernor et al., 2000; Walker and MacAulay, 2005) and the recording of adverse drug reactions (Gibbon and Khalifa, 2005) were both irregularly completed. A software program designed to improve the compliance of physicians with monitoring requirements recommended by guidelines was tested with promising results (Reeves et al., 2009). Documentation of consent to high-dose treatment was almost completely absent (Harrington et al., 2002; Parker et al., 2002), especially before an intervention (Acosta-Armas et al., 2004). However, one study set in the UK found that all 18 participants had given their consent, or appropriate forms had been completed where the patient was incapable of giving consent (Dalvi et al., 2003).
Theme five: environment
Prescribing issues associated with the environment in which the treatment occurred comprised the fifth theme. A lack of consistency was often noted between prescribers within a facility, and between different sites (Appelbaum, 2009; Department of Health, 2003; Lelliott et al., 2002; Parker et al., 2002; Walker and MacAulay, 2005). Prescribers working solely in correctional facilities may also suffer from a scarcity of unbiased information that community practitioners have in abundance, both on best practice (Department of Health, 2003; Fos-Claver and Soler-Garcia, 2008; Paton et al., 2002) and, in the UK, on their prescribing patterns compared with national data (Department of Health, 2003). Limited financial resources in these settings meant that other non-pharmacological treatment options may have been unavailable (Baillargeon et al., 2001; Bressington et al., 2008; Elger, 2004; Lekka et al., 2003), which can result in an increased workload for the general practitioner (Feron et al., 2005). The resulting high demand shortens appointment times (Bressington et al., 2008), which may be one of the explanations for prisoners feeling they did not receive sufficient information about their treatment (Bressington et al., 2008; Gray et al., 2008). The two studies revealing this possibility were classed as lower quality evidence in this review as they were both written using the same data from a study on satisfaction and adherence to therapy that employed convenience sampling.
The correctional facility environment and anxiety about legal proceedings and the future was frequently the cause of the insomnia, therefore patients may benefit from review before release to reduce the risk of withdrawal or unnecessary continued use of hypnotics and benzodiazepines in the community (Elger, 2004).
The continuity of care upon admission to, and on release from, these facilities has not been explored extensively, but current findings suggest significant room for improvement (Department of Health, 2003) (L. Hassan, 2009, personal communication). Physicians experienced difficulties in ascertaining what medications a patient was previously taking, and risked being pressured into prescribing against their better judgement through threats of legal action or suicide (Appelbaum, 2009; Pinta and Taylor, 2007). Drugs that were more likely to provoke this type of behaviour were the controlled drugs, and those that may be abused or were valuable for bartering; prescribers also need to consider the risk of intimidation of prisoners by others wishing to procure a supply of a certain drug (Appelbaum, 2009; Lekka et al., 2003; Pinta and Taylor, 2007). One of these reports was classed as lower quality evidence as it was a sole case study (Pinta and Taylor, 2007).
Conversely, the prescriber may need to use their powers of persuasion to convince a patient that the therapy would be beneficial (Swinton and McNamee, 2003). Although this issue was only directly raised by a lower quality report of methods employed by one facility (Swinton and McNamee, 2003), there were indirect mentions made several times of the need for prescribers to encourage compliance (Bains and Nielssen, 2003; Tavernor et al., 2000).
The independence of prescribers may be challenged by the desires and concerns of other staff about the potential for violent behaviour in certain prisoners. They may have been encouraged to prescribe more sedating drugs for those patients considered a risk (Acosta-Armas et al., 2004; Jukic et al., 2008; Parker et al., 2002). Differences in prescribing between subgroups based on gender, age and race have been reported, though the reasons behind this are not clear (Baillargeon et al., 2001; Fazel et al., 2004; Jukic et al., 2008; Lekka et al., 2003). It has been questioned whether the needs of prisoners are being met, as one study found that only 18% of older people with a psychiatric condition were prescribed medication (Fazel et al., 2004), and deficiencies were noted for those with depression (Baillargeon et al., 2001). Imposed protocols may also affect a physician’s prescribing autonomy. There were some complaints about the restrictiveness of an attention deficit hyperactivity disorder (ADHD) protocol, but there were also many positive remarks about the benefit of guidance and backing that it provided after implementation in an American state prison system (Appelbaum, 2009).
Prescribing errors have also been identified. Of the 311 prescribing errors found in one study, 87.5% were associated with prescription writing, and the remainder with decision making. The authors estimated that 85% of the errors would have been preventable had the electronic prescribing system available in community settings at the time been used (Haw and Stubbs, 2003b).
Discussion
Identified themes
Polypharmacy was widespread. Increased mortality rates, hospital admissions and severe adverse drug reactions have been associated with polypharmacy, so it should be avoided whenever possible (Baker et al., 2007; Bell et al., 2007). Use of more than one benzodiazepine and extended duration of treatment may increase the risk of side effects, dependence and tolerance (Rossi, 2009).
Very high doses of psychotropes, especially antipsychotics, were common. These high doses confer little or no increase in therapeutic effect, but significantly increase the risk of adverse effects including poor cognitive functioning and death (Gisev et al., 2006; Sim et al., 2008). Although there may be cases where regimens of polypharmacy or high doses are appropriate for an individual, the recommended associated documentation and monitoring were generally not being done. Antipsychotic medications can have a variety of undesirable effects on weight, blood glucose, blood pressure, and lipid levels (Rossi, 2009), so regular monitoring is required to enable early intervention if detrimental changes occur. Additionally, the recording of, and monitoring for, side effects and adverse drug reactions are important because of both the potential severity of adverse drug events and their potential impact on patient adherence and trust.
A wide variety of challenges faced when prescribing for prisoners were raised, but many of these were only found in one or two studies. An issue that was raised in several articles was poor continuity of care, both upon entering a correctional facility, and upon release. Continuity of care is also relevant when prisoners are transferred from one facility to another; consistency between prescribers and facilities has been noted as lacking by prisoners in this situation. A final issue was the use of persuasive or coercive techniques by some prisoners in an attempt to manipulate prescribing. Physicians need to be aware of this possibility.
Limitations of existing research
A number of limitations of the existing research became evident during the appraisal process. Several of the identified articles were written by the same authors. This may indicate that some facilities or regions are over-represented in the existing literature; almost all of the articles discussing polypharmacy were conducted in the UK. We do not know whether these issues are identifiable in other areas of the world. It was frequently challenging to determine whether studies included prisoners because of poor population and sample descriptions. Other common weaknesses included no justification of sample size or description of sampling method.
There was limited depth in the research. Many studies reported the incidence of polypharmacy, high-dose therapy, and the failure to adequately monitor physiological parameters; however, little research has been conducted to determine the reasons for, and possible solutions to, these issues. There was also limited replication of studies addressing issues more specific to prisoners.
Applications of this review
This review adds to current understanding of prisoner health, and may have several applications. Firstly, it provides an overview of previously identified areas for concern in prescribing for prisoners. This may be useful for physicians working in this area to review and improve their prescribing practices. Secondly, this review may prompt facilities to review their relationships and communication with other facilities and with practitioners in the community. This may help to standardise care and improve continuity of care upon admission or transfer. Thirdly, this review may prompt research into areas found to be minimally or poorly addressed in current literature. It may also provide some support for those aiming to improve health care in correctional facilities. Finally, policy makers may be able to more fully appreciate the possible avenues for resource allocation to provide the greatest improvement in prisoner health.
Limitations of this review
The risk of bias in the higher quality studies has been deemed to be low. As this review was based on qualitative rather than quantitative design, lower quality documents were included as they offered some new factors for consideration on potential prescribing concerns. There were only five studies that fell into this category, not significantly increasing the risk of bias of this review.
It was not possible to contact all of the authors of articles reviewed for information about other relevant research, published or otherwise. In addition, many authors failed to respond, presumably as they had no information to offer, but this cannot be confirmed.
Limitations were placed on the searches to improve manageability. The articles were restricted to those published from the beginning of 1999 onwards, although some of the studies included data from earlier than this, and those published in English. This could potentially bias the understanding of current standards for prisoners in countries where English is not the first language, as contradictory findings may have been published in another language. Forensic hospitals, high-security psychiatric wards, prisons and jails were all included in this review; issues identified in one setting may not necessarily apply to others.
Potential future research
Many of the included studies focused on assessing the prevalence of issues identified in other settings. To minimise the risk of the research becoming repetitive, it would be useful to focus attention of researchers on the influence of the prisoner’s environment on prescribing, as there has been comparatively little research conducted on this topic.
An approach or policy for continuity of care was not identified for prisoners. Research about the potential usefulness of effective community continuity of care models for prisoners would be beneficial.
If further studies are to be conducted on polypharmacy and high-dose therapy, more in-depth analysis would be required to fill gaps in the literature. Rather than merely reporting the prevalence of this issue, research should help to identify reasons for its occurrence, and ways to minimise this problem. Discovering the proportion of patients legitimately requiring high-dose therapy due to induction of metabolising enzymes or genetic differences would be useful. This has been briefly discussed as possible justification for the prescribing, but no studies investigating this potential explanation for prisoners were identified.
Descriptive studies are useful, especially initially to fully comprehend the nature and extent of a problem, but the time has come for something to be done with the knowledge that has been acquired.
Barriers to optimal psychotropic use
There are many barriers to optimal psychotropic use and care for mentally ill prisoners. The motivations and desires of prisoners, security staff, healthcare professionals, administrative staff and policy makers may be quite dissimilar, and any proposed change may be met with resistance (Appelbaum, 2009). There are also considerations of liability, as well as privacy of prisoners.
Identification of prisoners who may benefit from psychotropics is a significant hindrance to optimising treatment. Research has suggested the potential benefits of having standardised screening tools used in police holding cells to enable early identification and treatment of mentally ill detainees (Baksheev et al., 2010). Appropriate therapy may also reduce the risk of recidivism, as one study found that selective serotonin reuptake inhibitors decrease impulsivity; this is a contributing factor to violent crimes (Butler et al., 2010).
Conclusion
Very few examples of good practice were identified, together with many ways in which prescribing of psychotropic drugs to prisoners could have been improved. Prescribers may decide a patient warrants polypharmacy and/or high-dose therapy, and be able to justify their decision; however, this should be accompanied by the appropriate monitoring and documentation of decisions. The consequences for poor prescribing of psychotropic drugs could be iatrogenic morbidity or mortality. Prisoners are known to have elevated rates of mental illness, and prescribers are in a position to make a difference to their quality of life, be it positive or negative.
Footnotes
Appendix 1. Psychotropic drugs
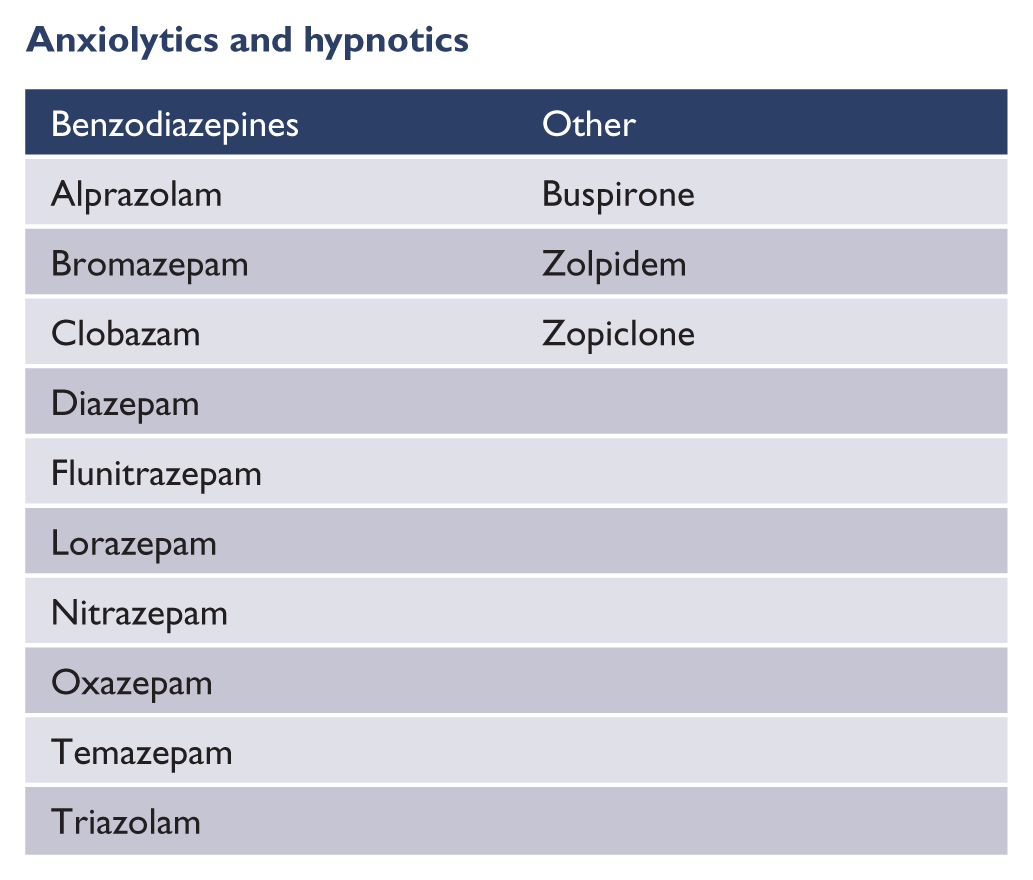
Anxiolytics and hypnotics
| Benzodiazepines | Other |
|---|---|
| Alprazolam | Buspirone |
| Bromazepam | Zolpidem |
| Clobazam | Zopiclone |
| Diazepam | |
| Flunitrazepam | |
| Lorazepam | |
| Nitrazepam | |
| Oxazepam | |
| Temazepam | |
| Triazolam |
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Declaration of interest
The authors report no conflicts of interest. The authors alone are responsible for the content and writing of the paper.
