Abstract
Introduction
Short Synacthen Test (SST), a standard diagnostic test to confirm Adrenal insufficiency (AI), involves substantial expenses.
Objectives
This study aimed to assess the predictive value of baseline Cortisol levels for SST outcomes and establish baseline cut-off levels for confirming AI to minimize the necessity of SST.
Methods
All SST data from 2019 to 2024 at National Hospital Kandy, Sri Lanka, were obtained retrospectively. A peak Cortisol ≥500 nmol/L at 30 or 60-min post-SST was considered as a normal adrenal reserve, whereas failure indicated AI. Pearson’s correlation and Logistic Regression analysis assessed baseline and post-SST Cortisol at 30 and 60-min. A 2 × 2 table assesses test agreement. Receiver operating characteristic (ROC) curve analysis evaluated the SST outcomes at 30 and 60-min separately assessing sensitivity, specificity, and area under the curve (AUC).
Results
A total of 307 patients were enrolled, and 63.19% exhibited a failed SST response. Baseline Cortisol positively correlated with post-SST Cortisol at 30-min (r = 0.74, P < .05) and 60-min (r = 0.68, P < .05) with a good AUC for both 30 min (AUC = 0.855) and 60 min (AUC = 0.829). Baseline Cortisol demonstrated the higher odds ratio per unit (OR = 1.015 per nmol/L), indicating greater sensitivity to small changes. ROC curves were utilized to derive cut-offs for baseline Cortisol levels predicting SST outcomes. At 30-min, baseline Cortisol <135 nmol/L suggests AI (100% sensitivity, 44% specificity), and >381.5 nmol/L indicates normal adrenal reserve (100% specificity, 21.8% sensitivity). Similarly at 60-min, baseline Cortisol <75.3 nmol/L suggests AI (100% sensitivity, 19.7% specificity), and >357 nmol/L indicates normal adrenal reserve (100% specificity, 16.8% sensitivity).
Conclusions
Applying these cut-offs could avoid 41.69% (30 min) or 19% (60 min) of total SSTs, excluding AI and normal adrenal reserve. 30-min SST Cortisol correlates more strongly with baseline Cortisol, showing a higher r-value, higher OR and AUC. Hence, 30-min provides better cut-offs with higher sensitivity and specificity minimizing need for SST. Patients with baseline Cortisol between 135 and 381 nmol/L can undergo SST with only a 30-min Cortisol measurement.
Introduction
Adrenal insufficiency (AI) is a potentially life-threatening condition that occurs when the adrenal glands fail to produce sufficient amounts of Cortisol. 1 The Short Synacthen Test (SST) is widely regarded as the most frequently utilized diagnostic test for assessing adrenal reserve. 2 It involves measuring Cortisol levels at baseline, and again at 30 and/or 60 min after the administration of synthetic ACTH (Synacthen).
The Insulin Tolerance Test (ITT) is considered the “gold standard” for diagnosing adrenal insufficiency.2–4 However, ITT carries significant risks, including potential life-threatening events, making it less frequently utilized in clinical practice. Cortisol levels taken 30 or 60 min after the ITT show a strong correlation with those from the SST, which makes the SST a safer alternative.2,5
Despite its widespread use, the SST remains an expensive and resource-intensive test, requiring specialized facilities and significant time from both patients and staff. Furthermore, during the recent economic crisis in Sri Lanka, there has been a shortage of Synacthen, further complicating its routine application.
Emerging evidence suggests that baseline Cortisol levels may predict SST outcomes, potentially reducing extra cost for additional tests, need for Synacthen, and lowering overall healthcare costs. This approach could streamline the diagnostic process with a single 9 am Cortisol as an outpatient test, improving patient-clinician satisfaction by making the process more efficient and less invasive.
The objectives of this research are as follows: 1. To determine the predictive value of baseline Cortisol levels in evaluating SST outcomes. 2. To assess the association between baseline Cortisol and the 30 and 60-min post-SST Cortisol measurements. 3. To compare the effectiveness of SST at 30 min versus 60-min in diagnosing adrenal insufficiency. 4. To establish a regional baseline Cortisol level for diagnosing adrenal insufficiency.
Methods
Study design and setting
This retrospective study was conducted at the Department of Chemical Pathology in collaboration with the Department of Endocrinology at the National Hospital Kandy, Sri Lanka, from January 2019 to December 2024. Data were obtained from the Laboratory database, with all information anonymized to ensure patient confidentiality. Ethical approval was granted by the Ethical Review Committee of the National Hospital Kandy (Reference Number: NHK/ERC/137/2024).
Inclusion and exclusion criteria
Inclusion criteria
Adult patients (≥18 years of age) who underwent SSTs at the Endocrinology Unit, National Hospital Kandy, during the study period.
All patients completed the SST following the standard protocol as per hospital guidelines.
All cortisol samples analyzed using the same immunoassay analyzer (VITROS 3600).
Exclusion criteria
Pediatric patients (under 18 years of age).
Pregnant women and women using hormonal contraception.
Patients with pre-existing endocrine disorders.
Assay for cortisol measurement
Serum Cortisol was measured using a competitive immunoassay performed on the VITROS 3600 immunoassay analyzer. Antigen–antibody complexes were captured via the biotin–streptavidin interaction and detected through a chemiluminescent reaction.
Short Synacthen test (SST) protocol
The SST was performed following the standard protocol of the Endocrinology Unit. If the patient was on steroids, discontinue hydrocortisone or prednisolone 24 h prior, and dexamethasone 48 h prior, in accordance with the endocrinology protocol and under appropriate monitoring. Baseline Cortisol levels were measured before administering 250 µg of Synacthen at 9–9.30 am, with subsequent levels taken at 30- and 60-min post-administration. According to the standard protocol of the Endocrinology Unit in Sri Lanka, and based on the immunoassay technique used, a post-SST Cortisol level of ≥ 500 nmol/L at either the 30- or 60-min time point indicates a normal adrenal reserve, while levels below this threshold suggest adrenal insufficiency.
Statistical analysis
The statistical analysis was performed using SPSS version 22. Descriptive statistics, including means, medians, and standard deviations, were calculated for relevant variables. The Pearson correlation coefficient was used to assess the relationship between baseline Cortisol levels and post-SST Cortisol levels at 30 and 60-min P < .05 was considered indicative of a statistically significant difference.
Receiver Operating Characteristic (ROC) curve analysis and Logistic Regression analysis was performed to determine the predictive value of Cortisol levels in diagnosing adrenal insufficiency. Sensitivity, specificity, and the area under the curve (AUC) were calculated to assess the diagnostic performance of the SST at the 30 and 60-min marks.
Results
A total of 306 patients were enrolled in the study, including 145 males (47.2%) and 161 females (52.8%). Of these, 63.19% (n = 194) exhibited a failed SST response, indicating adrenal insufficiency (AI), while the remaining 36.81% (n = 112) had normal adrenal reserve.
SST response by sex
Out of 145 male patients, 90 (62%) showed a failed response to the SST, while 104 (64%) out of 161 female patients had a failed response. The difference in SST response between males and females was not statistically significant (P > .05).
Correlation between baseline cortisol and Post-SST cortisol levels
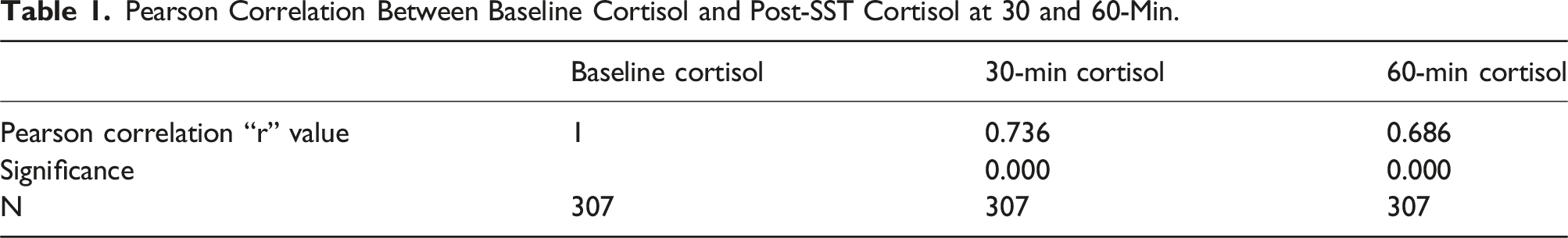
The results of Pearson correlation analysis revealed a strong and statistically significant positive correlation between baseline Cortisol and post-SST Cortisol at 30-min (r = 0.736, P < .05).
Pearson Correlation Between Baseline Cortisol and Post-SST Cortisol at 30 and 60-Min.

Logistic regression and predictive value
The logistic regression analysis demonstrated that baseline Cortisol levels were a statistically significant for AI, as determined by the SST. For every 1 nmol/L increase in baseline Cortisol, the odds of a positive SST result increased by 1.5% (odds ratio = 1.015, 95% confidence interval: 1.012–1.019, P < .001). This indicates a clear positive association between higher baseline Cortisol levels and the likelihood of an adequate adrenal response. The model showed moderate explanatory power, with a Nagelkerke R2 of 0.392, indicating that baseline Cortisol accounted for approximately 39.2% of the variance in SST outcomes.
ROC curve analysis and predictive value
Receiver Operating Characteristic (ROC) curve analysis was conducted to evaluate the predictive value of baseline Cortisol levels for predicting the outcome of the SST at both 30 and 60-min. The Area Under the Curve (AUC) for baseline Cortisol at 30-min was 0.855 (Figure 1(a)), and at 60-min was 0.829 (Figure 1(b)) which indicates strong predictive ability. ROC curve analysis for Baseline Cortisol in the SST response at 30-min (a) and at 60-min (b). Baseline Cortisol has strong predictive ability at both levels as evident by AUC greater than 0.8.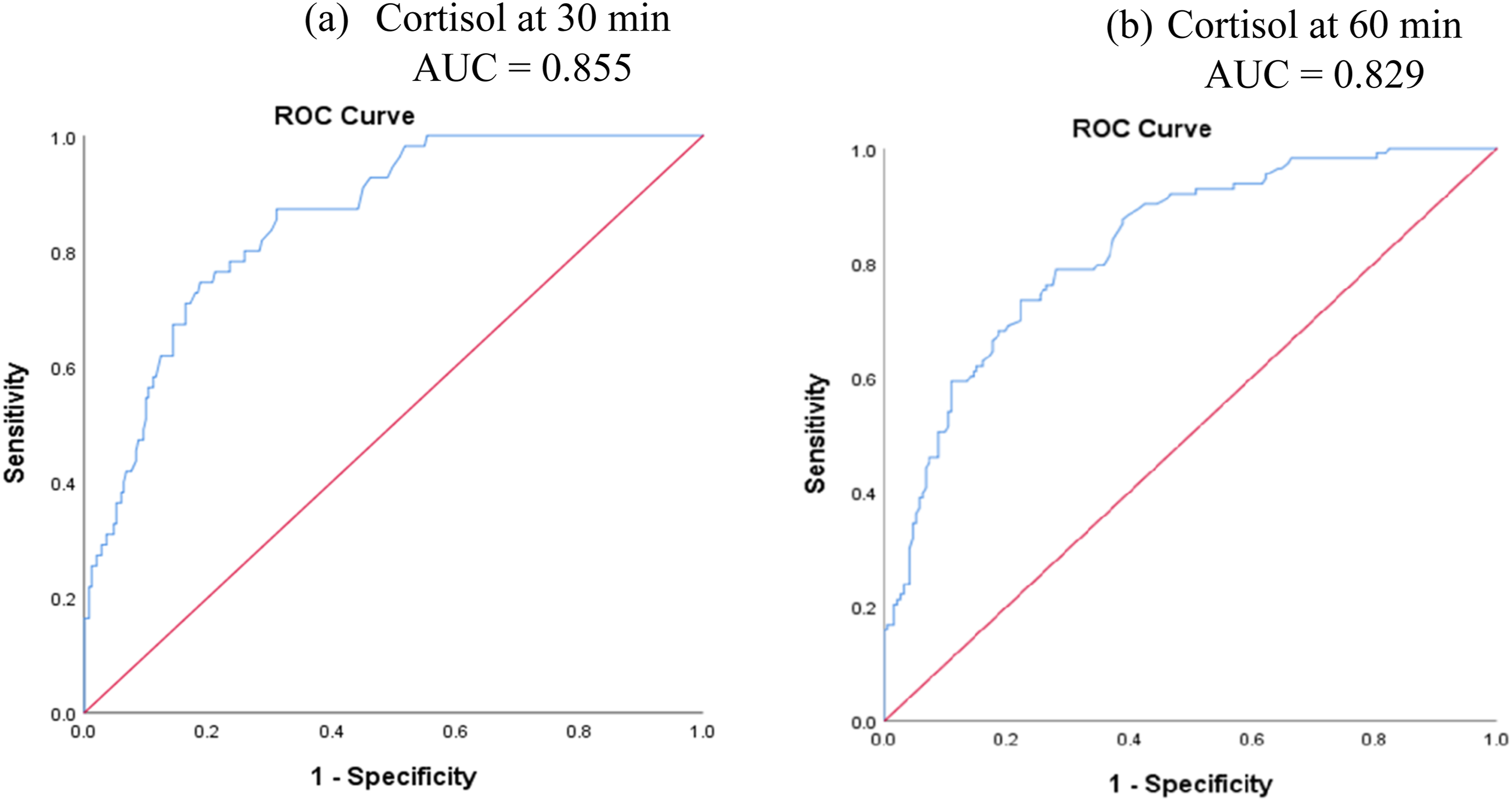
2 × 2 contingency analysis and diagnostic concordance between 30- and 60-min post-SST cortisol
Among patients who were positive at 30 min (n = 55), all remained positive at 60 min, demonstrating 100% concordance. Notably, 57 patients (22.7% of those initially negative) converted from negative at 30 min to positive at 60 min, and no cases were observed in which patients were positive at 30 min but negative at 60 min. Overall, 194 patients (63.4%) were negative at both time points, and 55 patients (18.0%) were positive at both. The association between the two time points was statistically significant (Cohen’s κ = 0.550, P < .001), indicating moderate agreement. The 30-min Cortisol measurement is superior for ruling in SST positivity, whereas the 60-min measurement is more effective at minimizing false negatives (Table 2).
Cut-off values for baseline cortisol levels
ROC curves were utilized to derive cut-offs for baseline Cortisol levels predicting SST outcomes. If the SST is positive (test positivity), it indicates that AI is excluded.
2 × 2 Contingency Analysis.

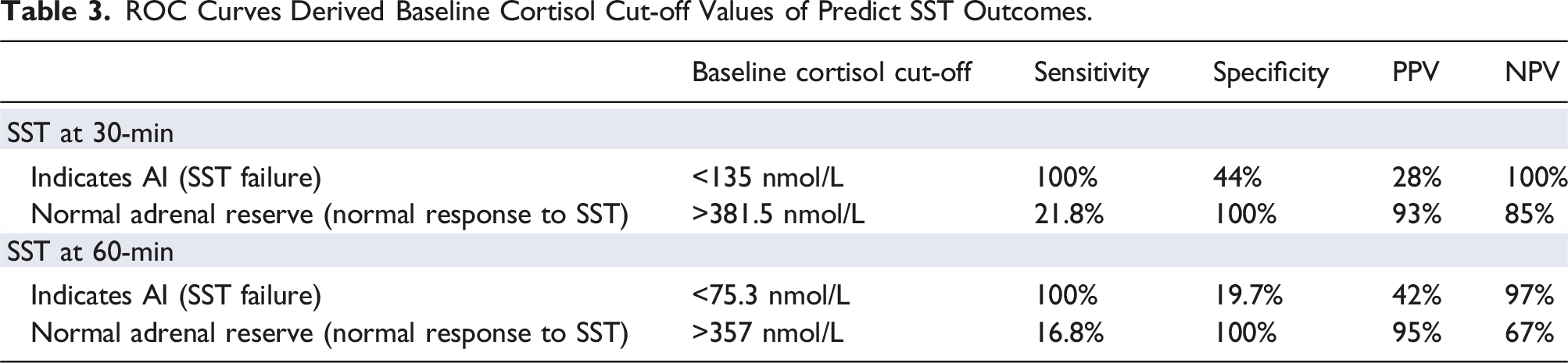
ROC Curves Derived Baseline Cortisol Cut-off Values of Predict SST Outcomes.
Discussion
This study involved 306 patients, with 63.19% exhibiting a failed SST response, indicating AI. The difference in SST response between males and females was not statistically significant, indicating that sex does not have a significant impact on SST outcomes in adrenal insufficiency. 6
A strong positive correlation between baseline Cortisol and post-SST Cortisol at 30-min (r = 0.736) and a moderate correlation at 60-min (r = 0.686) were observed. The correlation was stronger at 30-min, reinforcing the utility of baseline cortisol in predicting adrenal function at an earlier time point.
Logistic regression analysis demonstrated that baseline cortisol was a significant predictor of SST outcome.
Both time points demonstrated strong predictive ability with AUC values above 0.8, indicating high accuracy. Discriminative performance, assessed by AUC analysis, showed that 30-min Cortisol had the highest AUC (0.855), while 60-min Cortisol demonstrated a slightly lower AUC (0.829).
These results support the use of baseline Cortisol as a useful screening tool, as it significantly predicts SST outcomes. The 30-min Cortisol shows strong diagnostic performance and perfect concordance with 60-min positivity, making it a reliable confirmatory marker. Although the 60-min Cortisol has slightly lower overall discriminative value, it helps identify additional patients with normal adrenal function. Relying solely on the 30-min measurement risks underdiagnosing normal adrenal function and consequently over-diagnosing AI in nearly 20% of patients.
Cut-off values for baseline Cortisol were established to aid in diagnosing AI. As a screening test, SST’s primary role is to identify all potential cases of AI, which requires a cut-off with higher sensitivity and NPV. At 30-min, Cortisol levels <135 nmol/L indicated AI (100% sensitivity and NPV), while levels >381.5 nmol/L confirmed normal adrenal reserve (100% specificity and 93% PPV). At 60-min, Cortisol levels <75.3 nmol/L indicated AI (100% sensitivity, 97% NPV), and levels >357 nmol/L confirmed normal adrenal reserve (100% specificity, 95% PPV).
Many studies have investigated the use of a single serum Cortisol measurement to predict SST failure in various populations, each deriving different cut-off values based on their specific cohorts.2,4,6–13 The appropriate cut-offs can vary depending on factors such as the studied population, the Cortisol assay used, the SST protocol, and the criteria for diagnosing AI.
A study in Caerphilly, UK, involving 506 SSTs, found that a baseline Cortisol <124 nmol/L indicated SST failure with 100% specificity, while a Cortisol >314 nmol/L predicted normal SST with 100% sensitivity. 2 In Switzerland, a study of 804 subjects showed that a baseline Cortisol ≤100 nmol/L had a PPV of 93.2% for diagnosing AI, and a baseline Cortisol ≥450 nmol/L had a NPV of 98.7% for ruling out AI(11). A Tunisian study with 153 patients revealed that a baseline Cortisol <110 nmol/L had 100% sensitivity for SST failure, while >406 nmol/L showed 100% specificity for an adequate response to SST(4). In Sheffield, UK, a study of 393 SSTs found that baseline Cortisol <160 nmol/L had a high PPV (58%) for predicting SST failure, and >339 nmol/L had a high NPV (100%). 6 A study from Cambridge, UK, involving 450 patients, showed that baseline Cortisol <56 nmol/L predicted SST failure with 100% specificity, while >374 nmol/L predicted normal SST with 100% sensitivity. 7 A Sri Lankan study involving 217 patients found that baseline Cortisol levels less than 89.1 nmol/L are likely to indicate adrenal insufficiency (AI), while levels above 478 nmol/L suggest normal adrenal reserve. 13 Additionally, some studies have focused on identifying baseline Cortisol cut-offs for normal adrenal reserve, but they have not specifically addressed the cut-offs required for diagnosing AI. 8–10,12 Recent research aimed at evaluating hypothalamo-pituitary-adrenal (HPA) axis recovery has yielded important findings.14,15 One study showed that a 30-min Cortisol level during the SST, using a threshold of 350 nmol/L, can be a reliable marker of AI recovery. 14 Another study proposed a predictive model that combines previous SST outcomes with current baseline Cortisol levels to predict the results of subsequent SSTs. 15
In contrast to other studies, we compared the 30-min and 60-min values of the SST to evaluate the most appropriate time point for assessing the SST response. The baseline Cortisol cut-offs for SST were established to streamline testing. For the 30-min SST, a baseline Cortisol below 135 nmol/L suggests adrenal insufficiency, and above 381 nmol/L indicates normal reserve. Only patients with Cortisol levels between 135 and 381 nmol/L should proceed with 30-min SST. Applying this, 42% of total SSTs could be avoided, with 58% requiring the test. For the 60-min SST, a baseline Cortisol below 75.3 nmol/L suggests AI, and above 357 nmol/L indicates normal reserve. Only patients with Cortisol levels between 75.3 and 357 nmol/L should proceed with 60-min SST. In this case, only 19% of SSTs could be avoided, and 81% would still require 60-min SST. The cut-offs developed in our study differ from those of a previous Sri Lankan study. 13 However, our study included a larger population, which provides more reliable findings. A limitation of our study is that we did not account for the influence of patient demographics or clinical factors such as comorbidities, medication use, or the underlying etiology which may have significantly impacted cortisol responses.
We found more favorable findings associated with the 30-min SST Cortisol compared to the 60-min SST. The 30-min SST showed a stronger positive correlation with baseline cortisol, with a higher r-value and AUC. It also provided better cut-off values for baseline Cortisol, minimizing the need for SST and offering higher sensitivity, specificity, and both negative and positive predictive values. Though less discriminative, 60-min Cortisol identifies more with normal adrenal function but requires more SSTs.
Conclusions
In conclusion, our study suggests that baseline Cortisol measurement, ideally taken at 9 am, should be the first step in the evaluation of patients with suspected adrenal insufficiency. This simple, cost-effective approach can help triage patients efficiently and reduce unnecessary testing. We found that SST with 30-min Cortisol measurement is the most effective test for confirming adrenal insufficiency, offering a reliable diagnostic tool while minimizing resource use compared to the full 60-min protocol.
Based on our findings, we recommend the following clinical approach:
Baseline Cortisol < 135 nmol/L: suggest to be treated as AI.
Baseline Cortisol > 381 nmol/L: suggest to be managed as having normal adrenal reserve.
Baseline Cortisol between 135 and 381 nmol/L: should undergo the SST with only a 30-min Cortisol measurement to confirm the diagnosis.
Further validation of these thresholds in larger, multi-center studies will be important for confirming the robustness of our recommendations.
Footnotes
Acknowledgements
Department of Chemical Pathology, National Hospital Kandy, Sri Lanka.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for this article’s research, authorship, and/or publication.
Ethical approval
Obtained by Ethical Review Committee, National Hospital Kandy, Sri Lanka. Reference Number: NHK/ERC/137/2024.
Guarantor
Jayawardana RDP, Consultant Chemical Pathologist, National Hospital Kandy, Sri Lanka.
Contributorship
Premadasa T: Designed the study, Collected the data, interpreted the data, and drafted the manuscript.
Sujith EM: Statistical analysis of data.
Samarathunga EPA: Collected the data and Critical revision of the manuscript.
Shameela NMF: Collected the data.
Basnayaka BMKS: Collected the data.
Antonypillai CN: Designed the study and critical revision of the manuscript.
Jayawardana RDP: Designed the study and critical revision of the manuscript.
