Abstract
Background
Diabetic nephropathy is one of the most common microvascular complications in patients with diabetes. MicroRNA (miRNA, miR) is closely related to the formation, development and pathophysiology of diabetic nephropathy. We aimed to investigate whether miR-193a-3p could be used as a potential biomarker for the diagnosis of diabetic nephropathy.
Methods
Plasma samples were collected from all the participants. TaqMan Low Density Array analysis was employed to obtain the miRNA profiles of plasma samples, and qRT-PCR was used to confirm the result. Receiver operating characteristic curves were employed to evaluate the specificity and sensitivity of miR-193a-3p for predicting diabetic nephropathy.
Results
The expression of miR-193a-3p and miR-320c was elevated and miR-27a-3p was decreased in diabetic nephropathy patients compared to patients with type 2 diabetes and healthy controls. We found that, in diabetic nephropathy patients, the elevated miR-193a-3p expression had a negative correlation with the level of evaluate glomerular filtration rate, while a positive correlation with the level of proteinuria. We further demonstrated that miR-193a-3p could be employed to distinguish patients with diabetic nephropathy. The Kaplan–Meier analysis showed that the high expression of miR-193a-3p significantly shortened the dialysis-free survival of diabetic nephropathy patients.
Conclusion
In conclusion, miR-193a-3p is involved in diabetic nephropathy pathogenesis and may serve as a potentially novel diagnostic biomarker for diabetic nephropathy.
Introduction
Diabetic nephropathy (DN) is one of the most common microvascular complications in patients with diabetes, and is the leading cause of the end-stage renal disease (ESRD) worldwide. 1 The latest epidemiological data show that from 2011 the percentage of diabetes-related chronic kidney disease in China exceeds chronic glomerulonephritis, and the gap between the two has increased year by year. 2 With the changes in China's dietary structure and the extension of human life expectancy, the incidence of diabetes and its complications have gradually increased. A domestic study shows that diabetes, especially diabetes-related complications, significantly increases the financial burden of diabetic patients. 3 The onset of DN is insidious, and patients often have no discomfort, so they usually enter the ESRD when they are diagnosed. The pathogenesis of DN is complicated. At present, there is no effective method to prevent the progress of DN. Therefore, early diagnosis of DN and corresponding interventions are of great significance to improve patient health and reduce social burden.
MicroRNA (miRNA, miR) is a non-coding single-stranded RNA consisting of 18–22 nucleotides, which regulates gene expression mainly after transcription. 4 MiRNAs play key roles in regulating cell cycle, apoptosis and differentiation by regulating mRNA degradation and translation. 5 Emerging studies have found that miRNAs are inextricably linked to various diseases such as tumour, kidney disease, cardiovascular disease and diabetes.6,7 Various studies have found that miRNAs are closely associated to the formation, development and pathophysiology of kidneys, DN, hypertensive nephropathy, glomerulonephritis, focal segmental glomerulosclerosis (FSGS), lupus nephritis and many other primary and secondary nephropathies.8–10
Recent studies have found that down-regulated miR-193a expression in human parietal epithelial cells could induce high expression of the podocyte marker Wilms' tumour protein 1 (WT 1), 11 and promote the cell to differentiate into podocytes. 12 In a mouse nephrotoxic nephritis model, inhibited miR-193a expression could reduce crescent formation and proteinuria production. 13 Christoph et al. demonstrated that doxycycline-induced miR-193a upregulation in FSGS mouse models reduced podocyte marker protein expression and promoted proteinuria formation. 14 The above studies indicate that miR-193a could affect kidney disease progression by regulating podocyte marker expression. However, the miR-193a expression pattern and function in DN are not clear.
In the present research, we explored miR-193a expression in the serum of DN patients and its correlation with clinical indicators, providing new ideas for delaying the progression of DN.
Methods
Patients and study design
All the participants were recruited at the Affiliated Wuxi No.2 People’s Hospital of Nanjing Medical University during December 2017 to May 2018. In this research, DN was defined based on several criteria: 1. The existence of previous type II diabetes (T2D) history; 2. The existence of persistent albuminuria or inhibited renal function; 3. Diabetes-caused kidney disease confirmed by biopsy. Patients with comorbidities of acute kidney injury or non-diabetic renal disease were excluded. Figure 1 shows the research approach of this work. In the discovery stage, plasma samples from six T2D patients, six DN patients and six healthy controls were collected. The levels of relative RNAs were analysed by microarray and qRT-PCR. In the validation stage, 30 T2D patients, 47 DN patients and 30 healthy controls were recruited. Then miR-193a-3p level was confirmed by qRT-PCR. Next, we investigated the correlations of evaluate glomerular filtration rate (eGFR) and proteinuria with miR-193a-3p overexpression in DN patients. An 18-month follow-up survey was performed to demonstrate the influence of miR-193a-3p on DN patients’ prognosis. This research was approved by the ethics commitment of the Affiliated Wuxi No.2 People’s Hospital of Nanjing Medical University. Corresponding informed consents were signed by all the participants.
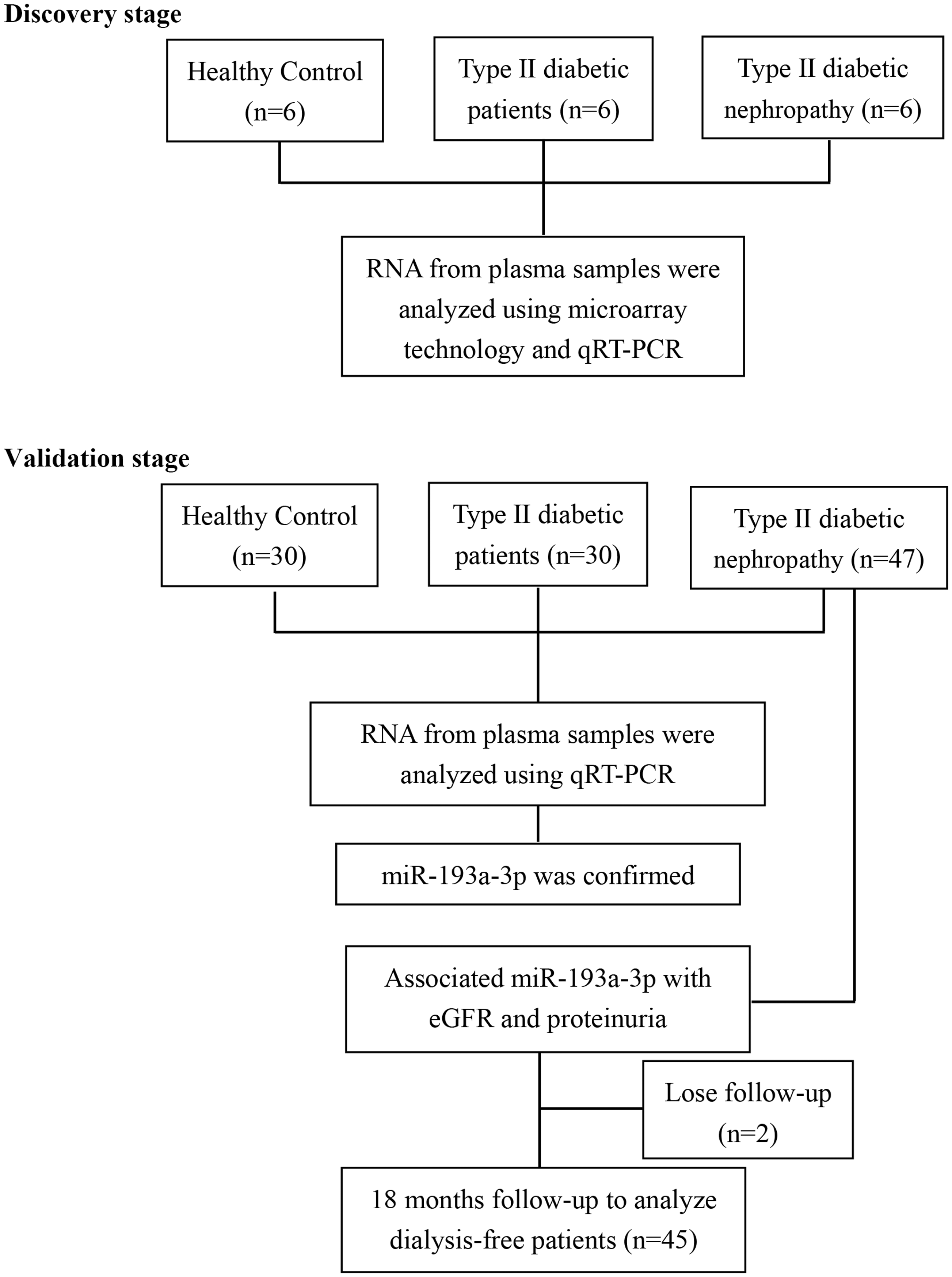
Schematic depiction of the research approach.
Sample preparation
EDTA tubes were used to collect peripheral blood samples from participants. After being centrifuged for 10 min at 3000
MiRNA microarray
TaqMan Low Density Array analysis was employed to obtain the miRNA profiles of plasma samples. TaqMan Array Human MicroRNA A1B Cards Set v3.0 was used. The internal control was U6 small nuclear RNA. Threshold cycle (CT) values were used to evaluate the relative abundances of the miRNAs. Fold change of miRNA was calculated by the comparative CT method.
qRT-PCR
The result of miRNA microarray was confirmed by qRT-PCR with TaqMan probes. The reverse-transcription was performed by One Step PrimeScript miRNA cDNA Synthesis kit (Takara, Shiga, Japan). PCR was performed by SYBR Green fluorescent quantitative PCR kit (Takara). The primer sequences used were as follows: miR-193a-3p, forward: 5′-TGGGTCTTTGCGGGCG-3′ and reverse: 5′-TGTGTTGTGCTGTGTCTGTG-3′; miR-320c, forward: 5′-AAAAGCTGGGTTGAGAGGGT-3′ and reverse: 5′-GCTGATCCACATCTGCTGGAA-3′; miR-27a-3p, forward: 5′-CTAATCGTGTT CACAGTGGCTAAG-3′ and reverse: 5′-TATGGTTTTGACGACTGTGTGAT-3′; U6, forward: 5′-CTCGCTTCGGCAGCACA-3′ and reverse: 5′-AACGCTTCACGAATTT GCGT-3′.
Statistical analysis
SPSS (version 18.0) and R version 3.0.1 were employed to perform statistical analysis. Normally distributed data were presented as mean ± SD and significance was analysed through two-tailed unpaired Student’s
Results
Baseline clinical characteristics of the participants
In the discovery stage, six T2D patients, six DN patients and six healthy controls were recruited. Characteristics of participants from the discovery stage are summarized in Table 1. In patients with DN, the level of serum creatinine was significantly higher than T2D patients and healthy controls. The pathogenesis of DN significantly decreased eGFR while enhancing the proteinuria.
Characteristics of participants from the discovery stage.
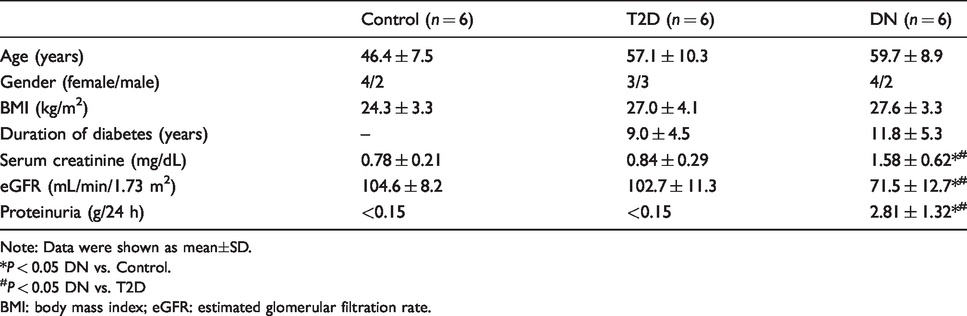
Note: Data were shown as mean±SD.
*
#
BMI: body mass index; eGFR: estimated glomerular filtration rate.
In the validation stage, 30 patients with T2D, 47 patients with DN and 30 healthy controls were recruited. Characteristics of participants from the validation stage are summarized in Table 2. In patients with DN, the duration of diabetes was longer than in patients with T2D. DN patients had higher systolic blood pressure than T2D patients and healthy controls. The tendencies of other characteristics in the validation stage were the same as those in the discovery stage.
Characteristics of participants from the validation stage.
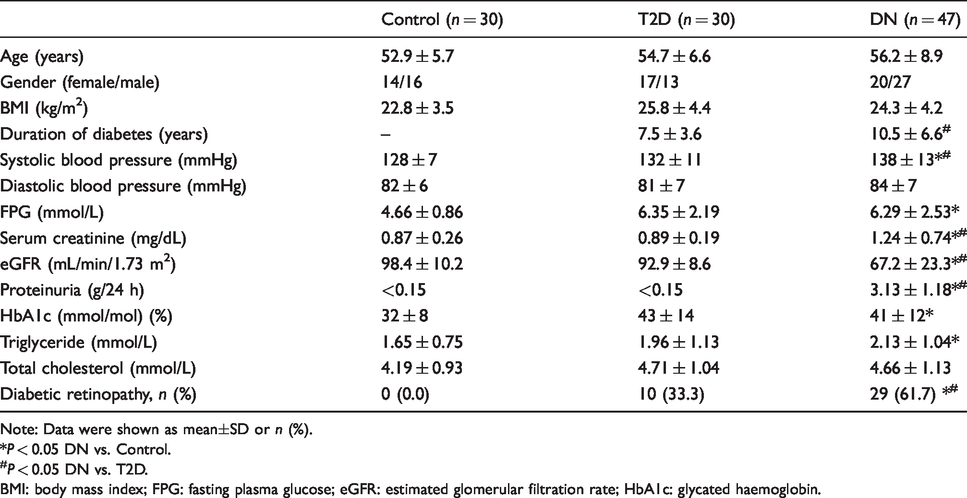
Note: Data were shown as mean±SD or
*
#
BMI: body mass index; FPG: fasting plasma glucose; eGFR: estimated glomerular filtration rate; HbA1c: glycated haemoglobin.
Identification of upregulated miRNAs in DN patients
We first analysed the differentially expressed miRNAs in plasma samples from DN patients through miRNA microarray. Figure 2(a) shows the miRNA expression heat map in healthy control, T2D patients and DN patients. Patients with DN had a significantly different plasma miRNA profile compared with that of healthy controls. The expression levels of miR-193a-3p and miR-320c were elevated, while miR-27a-3p was decreased in DN patients. Then we investigated miR-193a-3p, miR-320c and miR-27a-3p expression in healthy controls, T2D patients and DN patients through qRT-PCR (Figure 2(b)). Data from qRT-PCR indicated that both miR-193a-3p and miR-320c were highly expressed in DN patients. Furthermore, qRT-PCR results of plasma miR-193a-3p and miR-320c levels in individual participants with T2D, DN and healthy controls are shown in Figure 2(c). Patients with DN had significant higher miR-193a-3p and miR-320c levels in the plasma than patients with T2D and healthy controls.
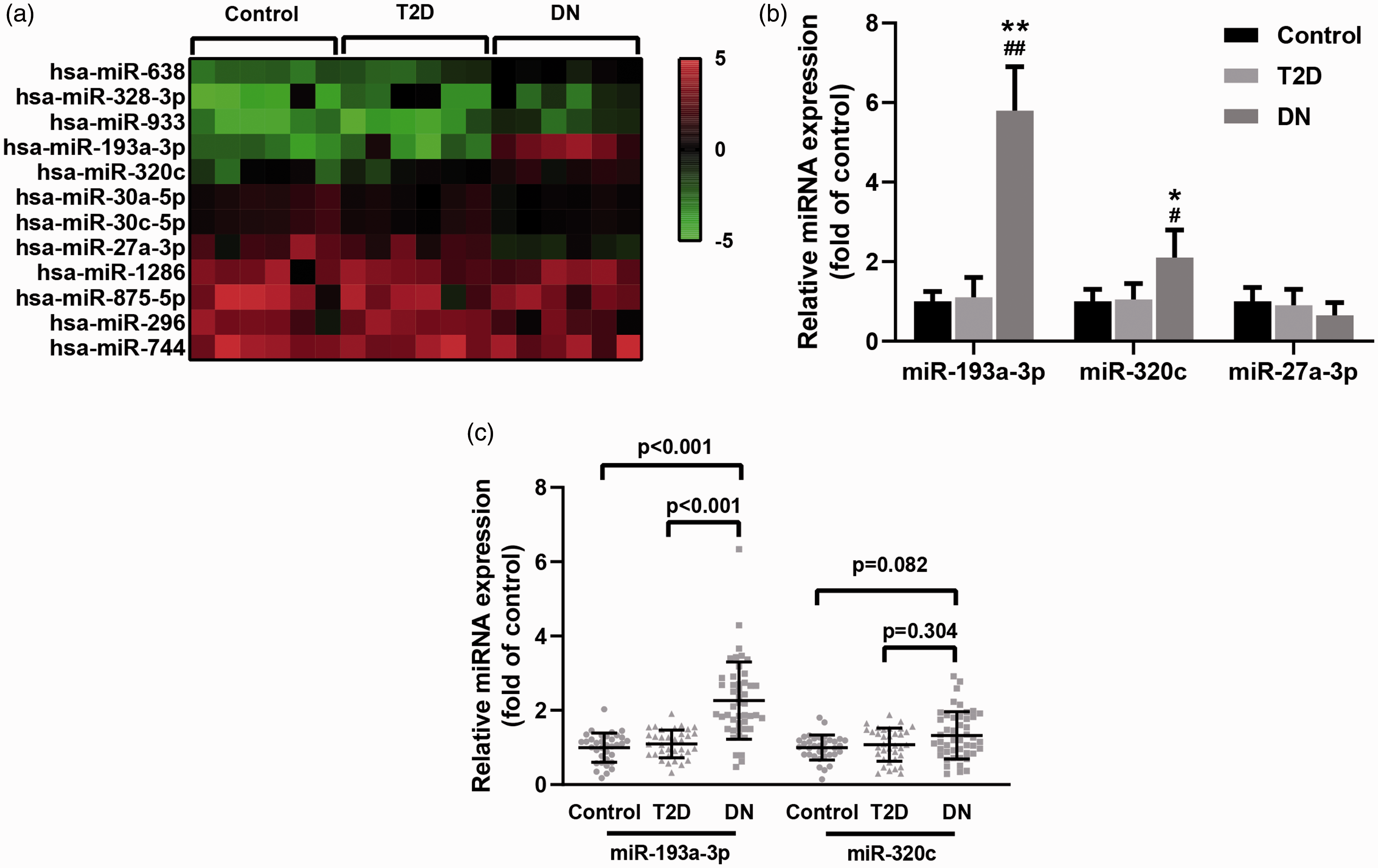
Analysis of miRNAs differentially expressed in plasma samples from patients with diabetic nephropathy (DN). (a) Heat map of expression levels of miRNAs in healthy control, T2D patients and DN patients. (b) Expression levels of miR-193a-3p, miR-320c and miR-27a-3p in healthy control (
Association of plasma miR-193a-3p and clinical outcomes of DN
It has been reported that the levels of proteinuria and eGFR were influenced by the pathogenesis of DN. Thus, the correlation between proteinuria/eGFR level and plasma miR-193a-3p level was investigated. We found that the enhanced miR-193a-3p expression had a negative correlation with the level of eGFR in DN patients (Figure 3(a)). However, the level of proteinuria had a positive correlation with miR-193a-3p (Figure 3(b)). So, the high expression of miR-193a-3 in DN patients enhanced the two clinical outcomes.
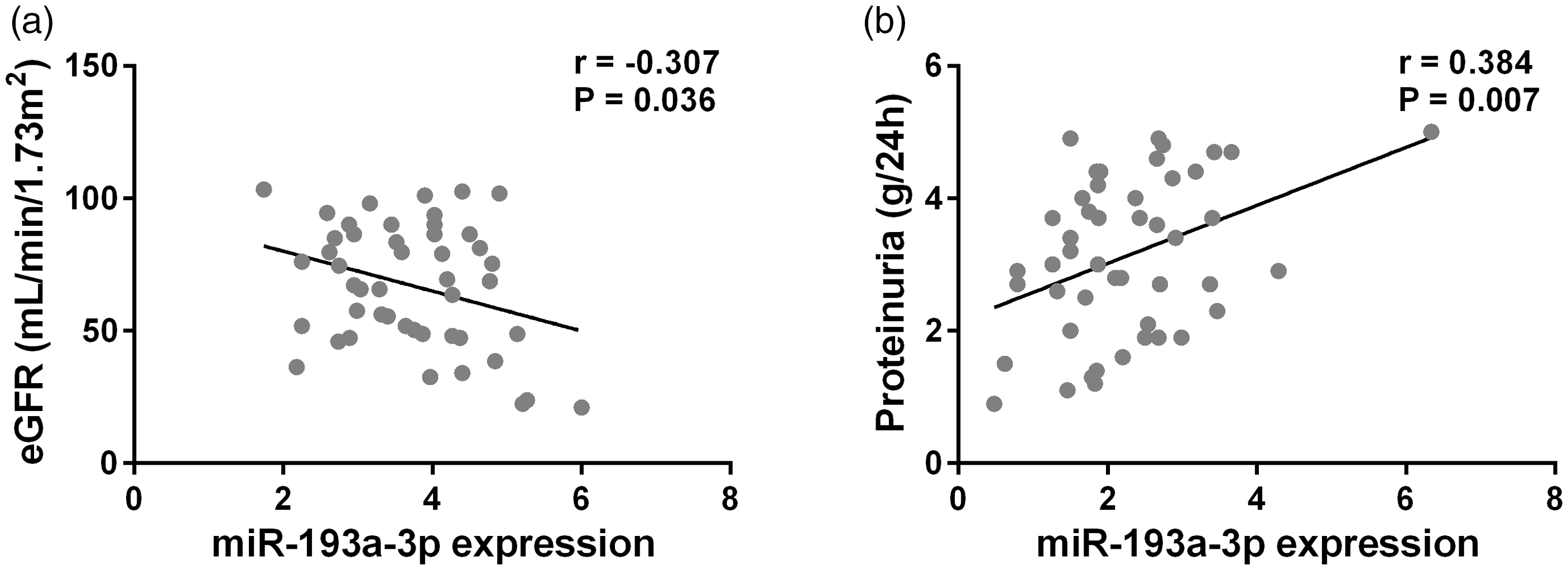
Pearson correlation of plasma miR-193a-3p with eGFR (a) and proteinuria (b) in DN patients (
Diagnostic value of plasma miR-193a-3p in DN
To evaluate whether plasma miR-193a-3p could act as a biomarker to diagnose DN, ROC curves were constructed (Figure 4(a)). Results showed that areas under the ROC curve (AUC) of miR-193a-3p was 0.876. Optical specificity and sensitivity of miR-193a-3p were 94.3% and 74.5%, respectively. These data indicated that miR-193a-3p could be used to distinguish patients with DN.
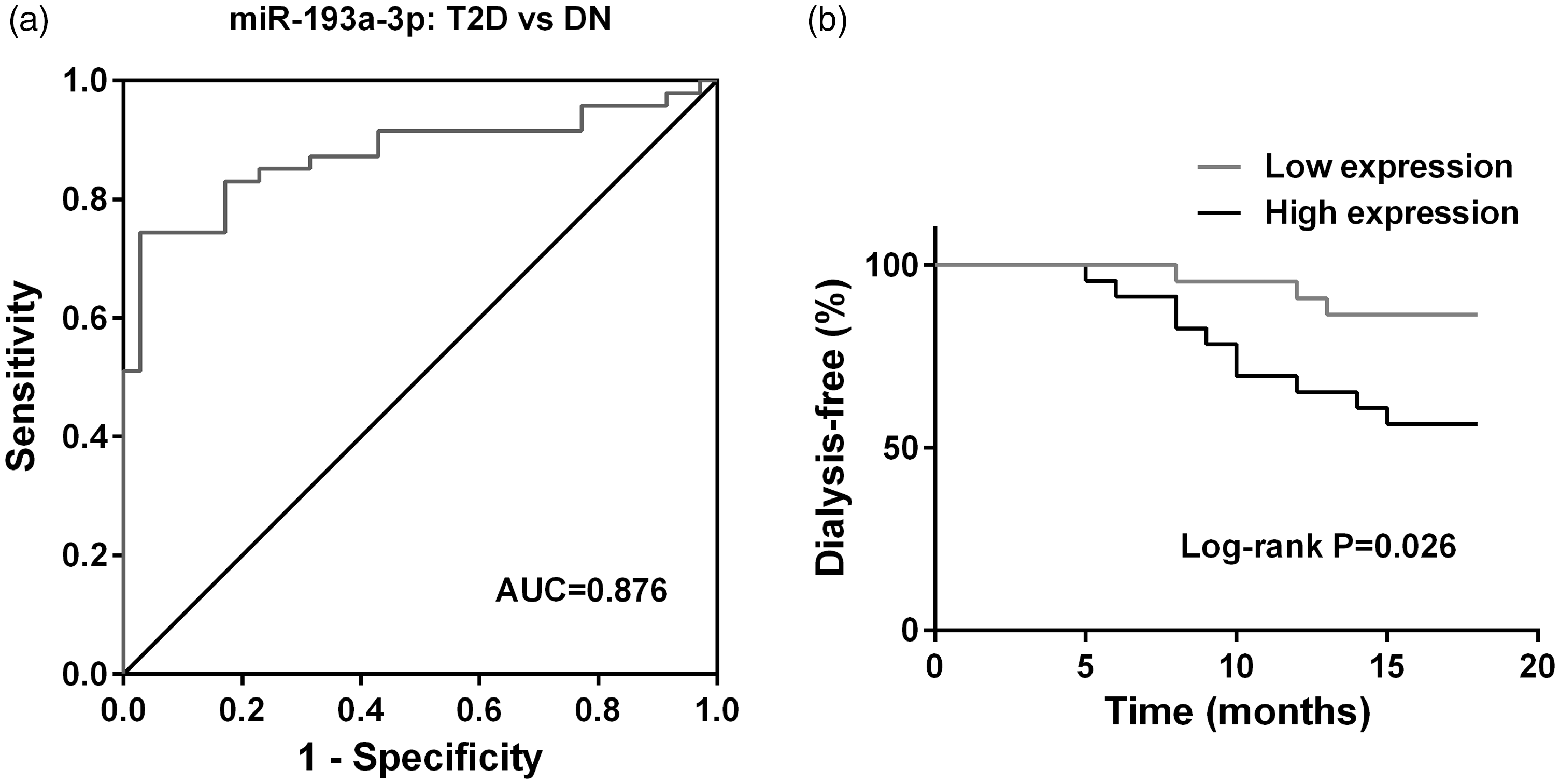
ROC curve analysis (a) was used to evaluate the diagnostic values of miR-193a-3p for discriminating T2D patients (
An 18-month follow-up survey was performed to demonstrate the relationship between miR-193a-3p expression level and the prognosis of DN patients. Kaplan–Meier analysis demonstrated that DN patients with high expression of miR-193a-3p showed worse dialysis-free survival than those with low expression (Figure 4(b)). Thus, the prognosis of DN patients was inhibited by the enhanced miR-193a-3p expression.
Discussion
As one of the serious complications of diabetes, renal damage caused by diabetes has become the main cause of end-stage renal failure in China. 15 DN has hidden changes and no obvious symptoms in the early stage of progression. 16 Patients often exhibit severe renal microvascular lesions at the time of consultation, and renal function damage is already in the irreversible stage, 16 which is one of the most important reasons for the high mortality rate of diabetes. Therefore, the selection of effective detection indicators for the early diagnosis is of great significance for the prevention, early treatment and improving the prognosis of DN. Traditional indicators for assessing renal impairment, such as serum creatinine and urea levels, have low specificity, accuracy and sensitivity, and the monitoring results are not satisfactory. 17
The current clinical diagnosis of DN mainly depends on the microalbuminuria and urine protein level of patients. 18 Early urine protein excretion in DN is slightly higher than that of normal people, which is called microproteinuria. 18 Once clinical proteinuria (urinary protein) appears, glomerular function declines irreversibly. In most patients, if they have entered the stage of clinical proteinuria, irreversible lesions have appeared in the kidneys. 18 Therefore, the emphasis on early detection and early treatment has shown great clinical value. 19 In this research, we also confirmed that the levels of serum creatinine and proteinuria were both significantly elevated in patients with DN. Meanwhile, DN patients had worse eGFR when compared with patients with T2D and healthy controls. At present, there is no mature diagnostic technology and effective early warning markers in this field, and further research is needed. Current treatment options only partially reduce the risk, and managing this complication is still an urgent need for people with diabetes.
MiRNAs belong to non-coding single-stranded small RNAs with a length of 21 to 23 nt. 20 They could target mRNAs, degrade target mRNAs or inhibit their translation, thereby blocking the production of target proteins. 21 MiRNAs play important regulatory roles in individual development, organ formation, cell proliferation, differentiation and apoptosis. 22 In addition to their intracellular biological regulatory functions, there is also more evidence that miRNAs could stably exist outside the cell, and the presence of miRNAs has been detected in the plasma, serum, urine and other fluids.23,24 Recently, emerging studies of circulating miRNA expression profiles in the blood have reported that some miRNAs with abnormal expression may be potential biomarkers in the occurrence and development of diseases, including diabetes.25,26 Although there have been no report on the use of circulating miRNAs to diagnose DN, it has recently been discovered that some miRNAs are involved in the regulation of DN disease-related genes. 27 It has been reported that overexpression of miR-377 could increase the production of fibronectin and vascular endothelial factors, and affect the changes in glomerular morphology. 28 MiR-192 is significantly down-regulated in chronic DN. By inhibiting the expression of zinc finger E-Box binding homeobox (Zeb)1/2, miR-192 promotes the accumulation of matrix collagen which eventually leads to the occurrence of DN. 29 Studies have found that transforming growth factor-β (TGF-β) could induce high expression of miR-216a and miR-217, both of which regulate the phosphatase and tensin homologue-protein kinase signalling pathway, leading to the proliferation and hypertrophy of glomerular mesangial cells. 30 MiR-29 promotes collagen expression under the inhibition of TGF-β, causing glomerular cell hypertrophy and renal fibrosis. 31 MiR-200 promotes the expression of TGF-β and causes renal tubular epithelial-mesenchymal transition and fibrosis, leading to the occurrence of DN. 32 Studies also have found that miR-21 and miR-451 are important down-regulated miRNAs in DN,33,34 suggesting that circulating miRNAs may become sensitive and novel biomarkers for the diagnosis of DN. In this paper, we analysed differentially expressed miRNAs in plasma samples from patients with DN through microarray technology. The expression of miR-193a-3p, miR-320c and miR-27a-3p was demonstrated to show a significantly different expression pattern between DN patients and T2D patients. It was shown that miR-193a-3p expression was dramatically elevated in patients with DN. Thus, miR-193a-3p was thought to be associated with the pathogenesis of DN.
MiR-193a is a member of the miR-193 family. It is located on the autosomal 17 and consists of 22 nucleotides in length. It mainly inhibits normal cell proliferation and cell cycle regulation. 35 Studies have shown that miR-193a acts as an important switch to regulate the differentiation of podocytes and parietal epithelial cells. 13 In a mouse model of focal segmental glomerulosclerosis, urinary protein increased in mice after induction with doxycycline, and miR-193a expression was increased in kidney tissues. 14 Therefore, we speculated that miR-193a could mediate kidney damage. To investigate the function of miR-193a-3p in the pathogenesis of DN, we detected the correlation between plasma miR-193a-3p level and two main clinical outcomes of DN, eGFR and proteinuria. As shown by Pearson correlation, eGFR had a negative correlation with plasma miR-193a-3p level. The enhanced miR-193a-3p expression in DN patients decreased glomerular function. Meanwhile, plasma miR-193a-3p level had a positive correlation with proteinuria. Thus, the clinical proteinuria of DN patients was also promoted by the enhanced miR-193a-3p expression. Since miR-193a-3p was found to be connected with the pathogenesis of DN, the diagnostic values of miR-193a-3p for distinguishing T2D patients were evaluated. ROC curve analysis showed that plasma miR-193a-3p could act as a biomarker to diagnose DN. Furthermore, the relationship between miR-193a-3p expression level and the prognosis of DN patients was investigated based on an 18-month follow-up survey. Kaplan–Meier analysis demonstrated that enhanced expression of miR-193a-3p decreased the dialysis-free survival in DN patients. The prognosis of DN patients was inhibited by the enhanced miR-193a-3p expression. However, the sample size in our study is small and it is a limitation of our study. The validation of miR-193a-3p as a biomarker candidate of diagnosis and prognosis needs to be further confirmed in a larger prospective study.
Conclusion
In conclusion, miR-193a-3p is involved in DN pathogenesis and may serve as a potentially novel diagnostic biomarker for DN.
Footnotes
Acknowledgement
None.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
This research was approved by the ethics commitment of the Affiliated Wuxi No.2 People’s Hospital of Nanjing Medical University.
Guarantor
KYZ will take full responsibility for the article.
Contributorship
Yan Hong, Jidong Wang, Lai Zhang, Wenjuan Sun, Xuefang Xu and Kaiyue Zhang performed the experiments, analysed and interpreted the data. Kaiyue Zhang was a major contributor in writing the manuscript. All authors read and approved the final manuscript.
