Abstract

Type 1 diabetes mellitus (T1DM) and latent autoimmune diabetes in adults (LADA) are organ-specific autoimmune diseases caused by an autoimmune response against pancreatic β cells, leading to loss of insulin secretion. LADA is characterized by onset of diabetes in adulthood, with slow progression to β cell failure. Patients may therefore present with clinical characteristics of both T1DM and type 2 diabetes mellitus (T2DM). 1 This makes LADA difficult to diagnose and treat appropriately. T1DM is routinely diagnosed based on clinical grounds, but the classification of T1DM or T2DM can be uncertain in some adult patients. Confirming T1DM in these patients may have important implications for availability of therapy. 2
Diagnosis of LADA and T1DM includes the detection of diabetes-specific autoantibodies and/or low concentrations of C-peptide. 2 NICE recommends measuring two different diabetes-specific autoantibodies with at least one being positive to diagnose LADA or T1DM, to reduce the false-negative diagnostic rate.2–4 NICE, however, makes no recommendation on which autoantibodies should be measured. Although several diabetes-specific autoantibodies assays are available, data from UK NEQAS indicate the most common antibodies measured are glutamic acid decarboxylase autoantibodies (GAD) and islet cell cytoplasmic autoantibodies (ICA). We offered analysis of ICA and GAD for the diagnosis of LADA, and if clinically indicated, to confirm T1DM in adults. We reviewed the clinical utility of measuring both ICA and GAD in these circumstances in patients aged ≥18 years.
Concordance between GAD and ICA results in 116 patients.
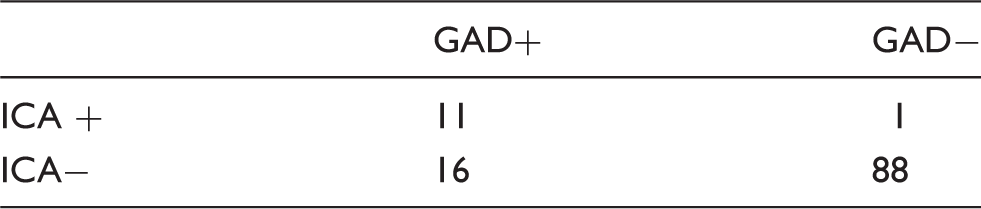
ICA: islet cell cytoplasmic autoantibodies; GAD: glutamic acid decarboxylase autoantibodies.
These results are consistent with reports that ICA titres decline more rapidly compared to GAD after onset of diabetes. 5 GAD antibodies, therefore, are more likely to remain positive when tested for the diagnosis of LADA or identification of T1DM in patients with long-standing diabetes. Assuming antibody negativity in both assays excluded autoimmune diabetes, both GAD and ICA had a diagnostic specificity of 100% but diagnostic sensitivities of 96% and 37.5% for GAD and ICA, respectively.
In conclusion, measuring ICA in addition to GAD in adults offers no added clinical value. ICA is also not cost-effective, particularly since ICA detection uses immunofluorescence analysis which is a manual, time consuming and therefore expensive method. We no longer offer ICA for detecting autoimmune diabetes in adults. Since C-peptide may better discriminate between T1DM and T2DM, the longer the test is done after diagnosis, 2 our current diagnostic strategy for identifying autoimmune diabetes in adults is measurement of serum C-peptide concentrations and GAD titres. The potential use of newer diabetes autoantibodies, including Zinc transporter 8 autoantibodies and Islet antigen 2 autoantibodies, 6 is being investigated in the diagnosis of LADA or reclassification to T1DM.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
Not applicable.
Guarantor
RG.
Contributorship
CF and AE conceived the study. CF collected the data. CF and LH performed data analysis. LH drafted the first manuscript and RG critically revised the manuscript. All authors approved the final version of the manuscript.
