Abstract
Objective:
To examine the incidence and risk factors of Clostridioides difficile infection (CDI) after otolaryngologic surgery.
Methods:
A retrospective cohort study of subjects undergoing otolaryngologic surgery was performed using the 2016 to 2021 American College of Surgeons National Surgical Quality Improvement Program (ACS-NSQIP). The incidence of CDI and potential risk factors were assessed.
Results:
One-hundred eighty-five surgical encounters experienced postoperative CDI out of 149 960, with a CDI incidence of 0.12% (8.8 cases per 10,000 patient-days). The greatest number of postoperative CDI was observed in head and neck reconstructive surgeries. On bivariate analysis, risk factors significantly and practically associated with the occurrence of CDI after otolaryngologic surgery were older age and longer operating times. Multiple logistic regression revealed that the CDI rate did not differ among otolaryngology subspecialties but was influenced by age, functional status, and operating times after controlling for relevant confounders.
Conclusions:
CDI after otolaryngologic surgery is a serious, costly complication with an incidence comparable to the national CDI rate. Knowledge of the preoperative risk factors associated with CDI may aid in the prevention of such infection after otolaryngologic procedures, thus decreasing patient morbidity and healthcare cost.
Introduction
As the most important cause of healthcare associated diarrhea and preventable nosocomial infection in the United States, Clostridioides difficile infections (CDI) are associated with significant patient morbidity and cost to the healthcare system.1-4 Thus, the United States Centers for Disease Control and Prevention and Centers for Medicare and Medicaid Services have implemented various initiatives to prevent CDI, with the latter agency even tying Medicare reimbursements to a hospital’s CDI rate.5,6 Known risk factors for CDI include recent antibiotic use (especially fluoroquinolones, third or fourth generation cephalosporins, clindamycin, carbapenems), older age, immunosuppression, gastrointestinal manipulation, and recent hospitalization.2,7 Additionally, frailty, a measure of increased vulnerability to poor health outcomes and disability,8,9 has been associated with a higher risk of postoperative complications and CDI.8-11 While the overall incidence of hospital-onset CDI in the United States has been reported to be about 8.3 cases per 10 000 patient days, 1 the incidence of postoperative CDI has been shown to vary by procedure and specialty.12,13 For example, Li et al 13 using the Veterans Affairs Surgical Quality Improvement Program, observed that the 30-day postoperative CDI rate ranged from 0.0% to 2.4% depending on specialty, with otolaryngology having a CDI rate of 0.17%. Postoperative consequences associated with CDI include longer length of hospital stay, greater readmissions, increased mortality, and unplanned re-operations.12-16 Although previous studies have investigated CDI in specific otolaryngologic procedures, these were limited to head and neck free flap and pedicled flap surgeries.17-19 Thus, the objectives of this study were to: (1) examine the incidence of CDI across all otolaryngologic procedures and investigate differences among subspecialties and (2) examine the risk factors associated with postoperative CDI occurrence, specifically frailty and operative times. We hypothesize that CDI will differ among otolaryngology subspecialties and that a higher risk of postoperative CDI will occur in patients that are frailer and have longer operative times.
Methods
Study Design
The American College of Surgeons National Surgical Quality Improvement Program (ACS-NSQIP) was utilized. The ACS-NSQIP is a nationally validated, risk-adjusted, 30-day postoperative outcomes based surgical data registry with over 600 participating hospitals across the United States. 20 The ACS-NSQIP data from 2016 to 2021 were used. All surgical cases whose specialty was labeled as otolaryngology (ENT) were included in the study. Cases that had preoperative sepsis were excluded from the study. This study was reviewed by the institutional review board at the University of Texas Health San Antonio and determined to be exempt (STUDY00000958).
Measures Evaluated
The main variable of interest was the occurrence of CDI. The principal operative procedure and associated principal current procedural terminology (CPT) code were used to categorize each subject into otolaryngology procedure type and subspecialty (see Table S1 in Supporting Information). Each surgical encounter had multiple CPT codes listed. However, the principal CPT code for each surgical encounter was labeled by NSQIP as the most complex procedure performed for that specific surgical case. Demographic variables, including age, gender, and race/ethnicity were included. Frailty and total operation time were also collected as potential risk factors. The variables that defined frailty were based on the 5-factor modified frailty index (mFI-5), which was created uniquely for the ACS-NSQIP and includes functional status, history of diabetes, history of chronic obstructive pulmonary disease, history of congestive heart failure, and history of hypertension. 21 The mFI-5 has been validated as a strong predictor of mortality and postoperative outcomes, thus being a credible measure of frailty. 21
Statistical Analysis
Univariate statistics (tabulations, frequencies, medians, and interquartile ranges) were used to describe demographic characteristics, comorbidities, and risk factors. Bivariate models, including t-test for continuous variables and chi-square or Fisher’s exact test for categorical variables, were used to compare characteristics between subjects who had CDI and those that did not. Cohen’s d for continuous variables and Cramer’s V for categorical variables were reported for effect size. Multivariable logistic regression models were used to evaluate the association between CDI and risk factors while controlling for potential confounders. Covariates included in the multivariable model were identified via the model building technique (forward selection, backward selection) that minimized the Akaike Information Criterion. Ultimately, the forward selection technique was chosen to build the final model with entry significance criteria set at .20. Odds ratios and 95% confidence intervals were reported for items in the final model. Alpha was set at .05 to determine statistical significance. Stata 18.0 (College Station, TX) was used to conduct all statistical analyses.
Results
A total of 149 960 surgical cases were included. Table 1 describes the sample population. The median age was 50 years old with majority of the subjects being female, identifying as White non-Hispanic, and undergoing a head and neck procedure. The postoperative CDI rate was 0.12% (8.8 CDI cases per 10 000 patient days) with a median of about 10 days between surgery and a diagnosis of CDI. Of the 185 CDI cases reported, free/regional flaps (23.8%), neck dissections (14.1%), laryngectomies (11.4%), glossectomies (partial/total; 10.3%), and thyroidectomies (8.7%), made up the majority of otolaryngologic procedures associated with postoperative CDI (Table 2).
Sample Characteristics of Study Participants.
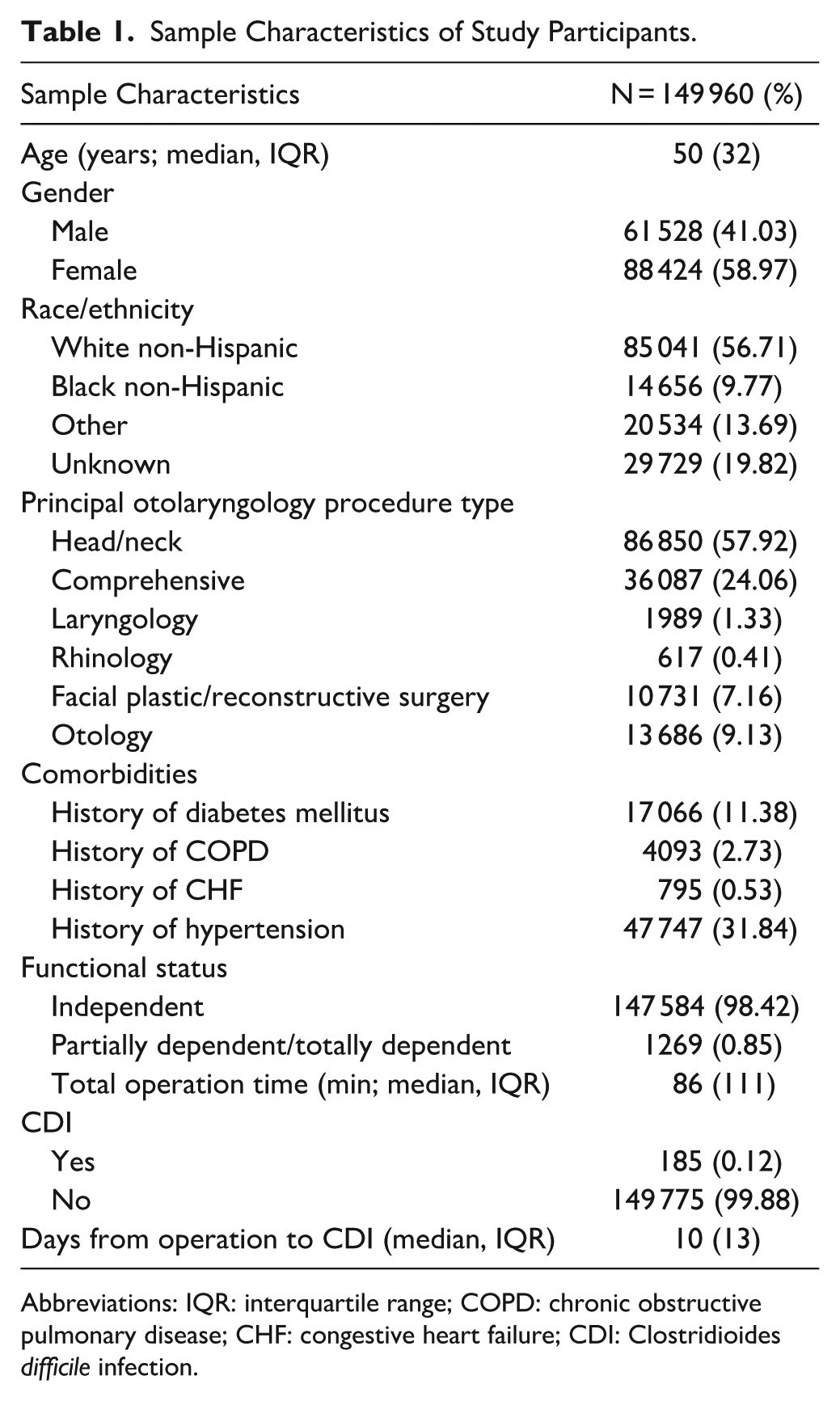
Abbreviations: IQR: interquartile range; COPD: chronic obstructive pulmonary disease; CHF: congestive heart failure; CDI: Clostridioides difficile infection.
Clostridioides difficile Infection by Surgery.
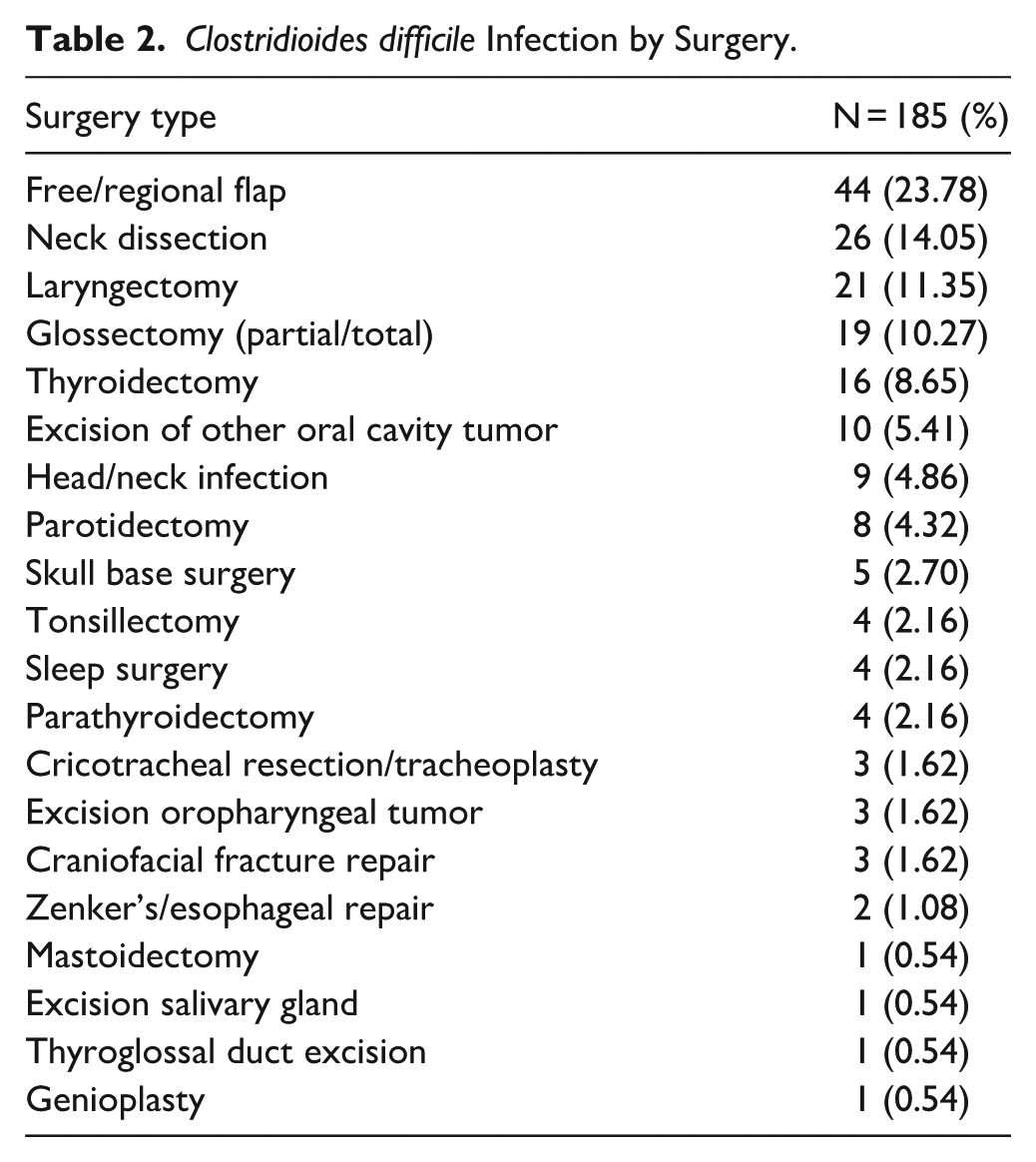
Table 3 displays the crude bivariate relationships between CDI occurrence and demographics, otolaryngology procedure type, frailty characteristics, and operative time. Characteristics statistically associated with CDI include age, gender, race/ethnicity, otolaryngology procedure type, history of chronic obstructive pulmonary disease, history of congestive heart failure, history of hypertension, functional status, and operative times. Effect sizes of the aforementioned variables revealed that older age (Cohen’s d = 0.774) and longer operative time (Cohen’s d = 1.847) had a strong strength of association with CDI while all other statistically significant variables had a weaker strength of association with CDI.
Bivariate Analysis of CDI by Demographics, Procedure Type, Frailty Characteristics, and Operative Time.
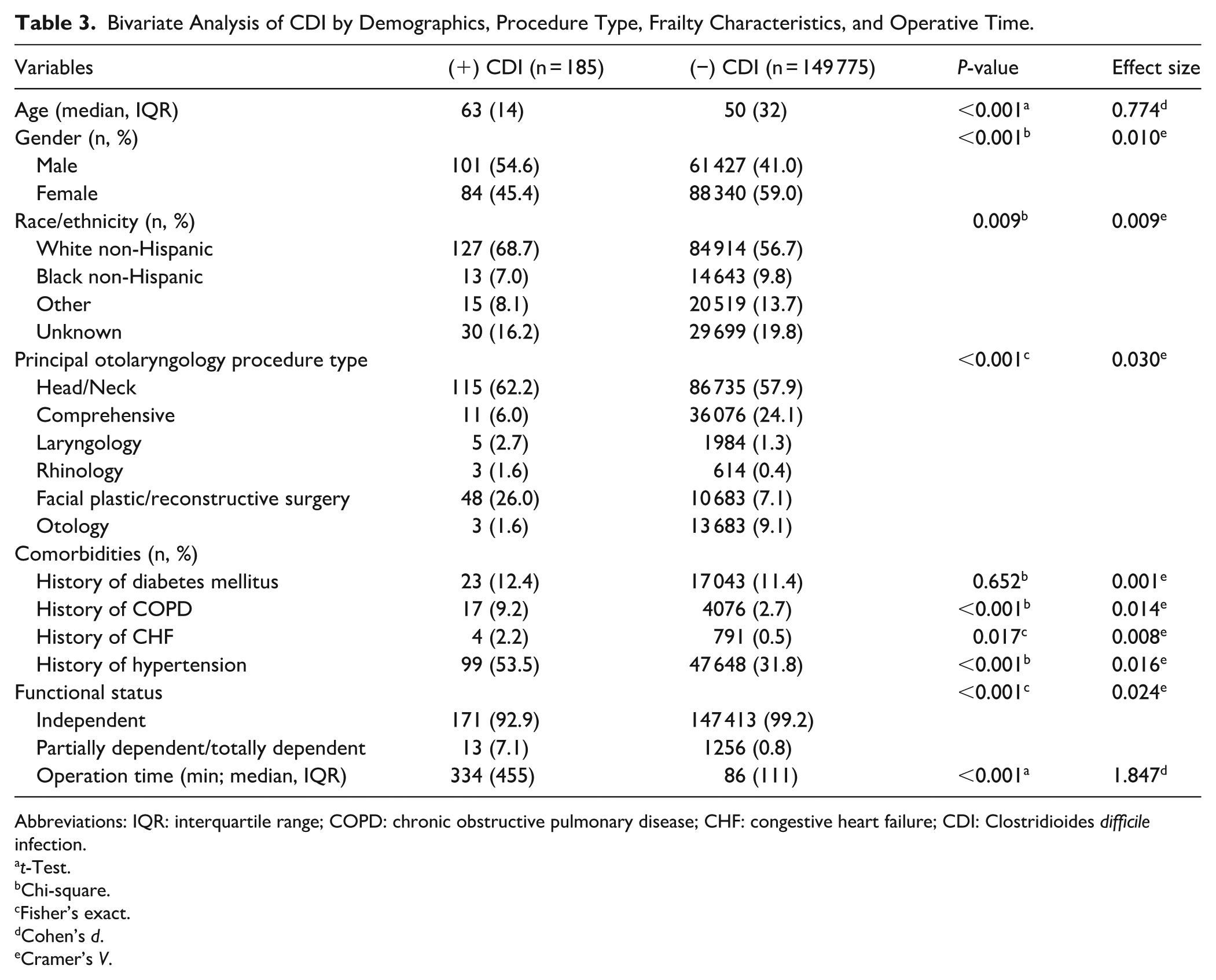
Abbreviations: IQR: interquartile range; COPD: chronic obstructive pulmonary disease; CHF: congestive heart failure; CDI: Clostridioides difficile infection.
t-Test.
Chi-square.
Fisher’s exact.
Cohen’s d.
Cramer’s V.
Figure 1 illustrates a forest plot displaying multivariable logistic regression evaluating the relationship among CDI and risk factors. After controlling for all other covariates in the model, the rate of CDI in various otolaryngologic subspecialties was not significantly different when compared to comprehensive otolaryngology. Additionally, older age, being partially dependent/totally dependent compared to independent, and longer operative times were significantly associated with postoperative CDI occurrence after controlling for all other covariates in the model. Functional status had a stronger association with CDI compared to all other variables in the multiple logistic regression model.
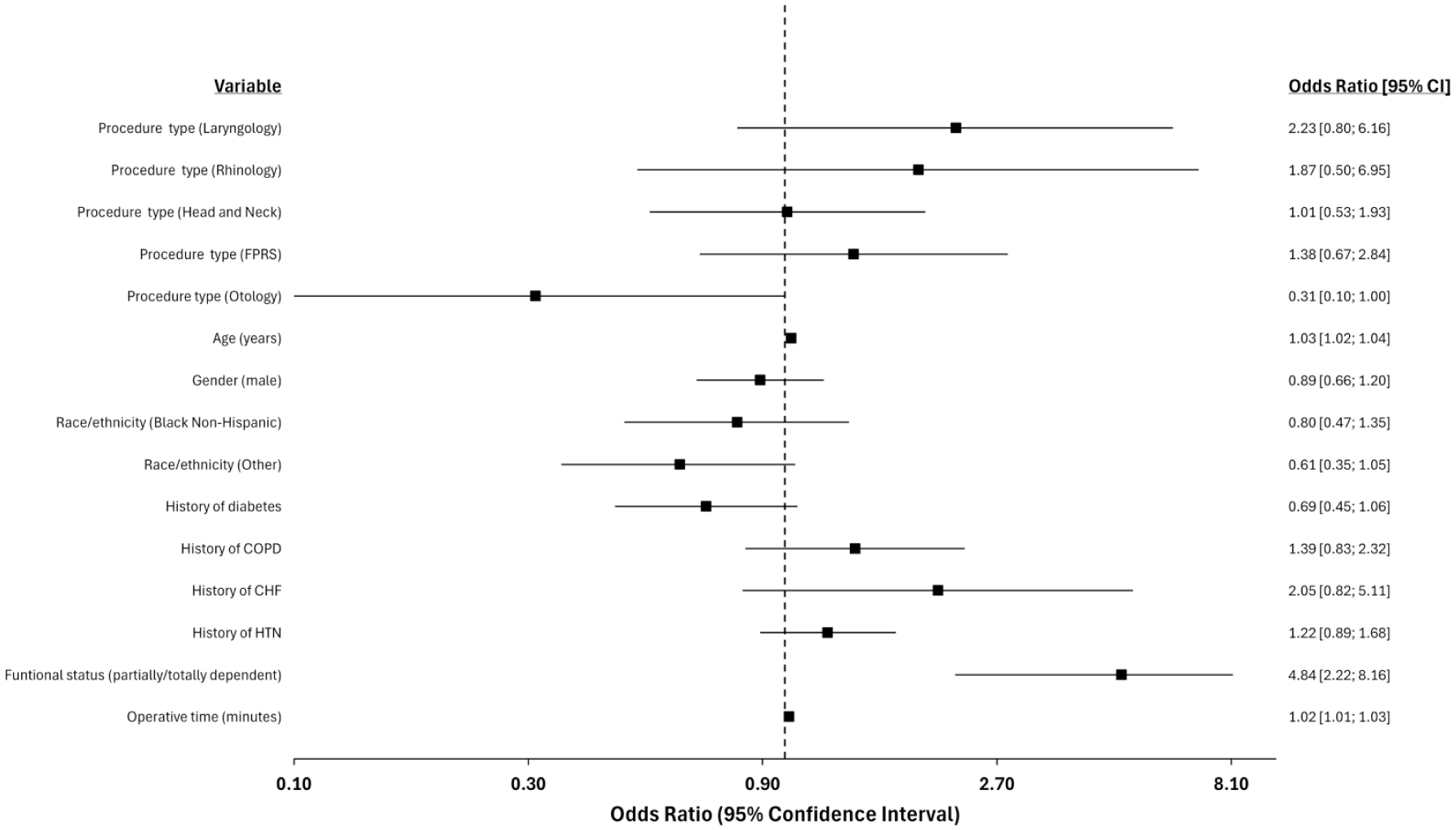
Forest plot displaying multivariable logistic regression evaluating the relationship among Clostridioides difficile infection, demographics, procedure type, frailty characteristics, and operative times. Reference values for various variables were as follows: procedure type = comprehensive, gender = female, race/ethnicity = White Non-Hispanic, functional status = independent. All odds ratios are adjusted for all other covariates in the model.
Discussion
CDI is a serious healthcare-associated complication with significant consequences for patient outcomes. In addition to the added morbidity and mortality associated with such infection, CDI comes with a substantial cost with reports estimating about $24 000 to treat a single case of primary CDI.3,22,23 This translates into a total annual CDI-attributable cost of about $1.9 to $7.0 billion.4,23 In the context of the postoperative period, where patients may be even more susceptible to this highly contagious infection, the cost is likely greater given the potential postoperative complications associated with CDI observed in this study. Thus, the need for CDI prevention after otolaryngologic surgery is substantial.
This study found that the CDI incidence after otolaryngologic procedures is about 0.12% or 8.8 CDI cases per 10 000 patient days, which is comparable to the national published CDI incidence rate and previously reported postoperative CDI rates.1,13 However, one must keep in mind that the ACS-NSQIP does not take into account postoperative outcomes in non-hospital settings, such as ambulatory surgical centers or private clinics, where majority of otolaryngologic procedures take place. 24 Thus, the true number of CDI cases after otolaryngologic procedures may differ than what this study suggests. While most of the procedures associated with CDI were those pertaining to head and neck and reconstructive surgery, no difference in CDI rate was observed between otolaryngology subspecialties after controlling for relevant confounders, such as demographic characteristics, operative times, and various comorbidities. Additionally, although crude bivariate analysis revealed a number of preoperative characteristics that was statistically associated with postoperative CDI, controlling for confounders revealed that age, functional status, and operative times were significantly associated with the occurrence of CDI, with functional status having a greater strength of association compared to age and operative times. Frailty, a measure of physiologic and biologic health resilience, encompasses functional status and has been shown to be a predictor of postoperative morbidity and mortality.8,9 As such, preoperative identification of frail patients with potential interventions, such as pre-habilitation, in addition to minimizing operative times, may decrease CDI occurrence.
While this is the first study to evaluate CDI after otolaryngologic surgery using a national surgical database, the primary limitation is the lack of data on perioperative antibiotic use, as this information is not reported by the ACS-NSQIP. This study limitation should not minimize the impact antibiotic prescribing patterns have on postoperative CDI as antibiotic use is likely an important confounder for certain results observed in this study. Previous studies have highlighted the inappropriate use of antibiotics in otolaryngologic surgery, especially in those with inaccurate penicillin allergy labels who are subsequently prescribed alternative antibiotics that harbor a higher risk of CDI.25-27 Despite this primary limitation, this is the first study to give insights into the incidence and potential risk factors of CDI over a broad range of otolaryngologic procedures.
Since the postoperative CDI rate in otolaryngologic surgery was observed to be comparable to the overall national CDI rate (both operative and nonoperative), one can infer that otolaryngologists have room to improve on CDI prevention. With further strides in antibiotic stewardship along with a better understanding of the preoperative risk factors that put patients at risk for CDI, otolaryngologists can effectively make the postoperative period safer and decrease healthcare expenditures. Additional limitations due to the design of the ACS-NSQIP database include the potential for coding error, the retrospective nature of data collection, and outcomes being limited to only 30 days postoperatively.
Conclusion
CDI is a serious complication after otolaryngologic surgery. Understanding of the types of procedures and potential risk factors associated with postoperative CDI after otolaryngologic surgery may aid in the prevention of such infection, leading to improved postoperative patient outcomes and decreased healthcare costs.
Supplemental Material
sj-docx-1-aor-10.1177_00034894251396752 – Supplemental material for Risk Factors for Clostridioides difficile Infection After Otolaryngologic Surgery: An ACS-NSQIP Analysis
Supplemental material, sj-docx-1-aor-10.1177_00034894251396752 for Risk Factors for Clostridioides difficile Infection After Otolaryngologic Surgery: An ACS-NSQIP Analysis by Matthew Y. Liu, Dylan Z. Erwin, Melis N. Bayrak, David W. Jang and Philip G. Chen in Annals of Otology, Rhinology & Laryngology
Footnotes
Acknowledgements
None.
Ethical considerations
This study received ethical approval from the University of Texas Health San Antonio IRB (STUDY00000958) on September 18, 2025. This is an IRB-approved retrospective exempt study.
Consent to participate
The Institutional Review Board of the University of Texas Health San Antonio waived the need for patient consent for the collection, analysis and publication of the retrospectively obtained and anonymized data for this non-interventional study.
Consent for publication
Not applicable.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Philip Chen is a consultant for Medtronic, advisory board for Sanofi, Amgen, and GlaxoSmithKline, speaker’s bureau for GlaxoSmithKline and Optinose, and has research funding from Aerin Medical. None affect this research. David Jang is a consultant for Medtronic and a speaker for Sanofi and Regeneron. None affect this research.
Data availability statement
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
