Abstract
This study aimed to identify patient characteristics linked to mistaken treatments and major adverse cardiovascular events (MACE) in percutaneous coronary intervention (PCI) for coronary artery disease (CAD) using deep learning-based fractional flow reserve (DEEPVESSEL-FFR, DVFFR). A retrospective cohort of 3,840 PCI patients was analyzed using latent class analysis (LCA) based on eight factors. Mistaken treatment was defined as negative DVFFR patients undergoing revascularization or positive DVFFR patients not receiving it. MACE included all-cause mortality, rehospitalization for unstable angina, and non-fatal myocardial infarction. Patients were classified into comorbidities (Class 1), smoking-drinking (Class 2), and relatively healthy (Class 3) groups. Mistaken treatment was highest in Class 2 (15.4% vs. 6.7%, P < .001), while MACE was highest in Class 1 (7.0% vs. 4.8%, P < .001). Adjusted analyses showed increased mistaken treatment risk in Class 1 (OR 1.96; 95% CI 1.49–2.57) and Class 2 (OR 1.69; 95% CI 1.28–2.25) compared with Class 3. Class 1 also had higher MACE risk (HR 1.53; 95% CI 1.10–2.12). In conclusion, comorbidities and smoking-drinking classes had higher mistaken treatment and MACE risks compared with the relatively healthy class.
Keywords
Introduction
Coronary Artery Disease (CAD) refers to ischemic cardiac conditions resulting from inadequate blood supply in the coronary arteries. The presence of coronary artery stenosis (CAS) represents one of the most prevalent pathological foundations underlying CAD. This condition restricts the coronary arteries’ blood flow to the myocardium, resulting in inadequate myocardial blood supply and subsequently causing symptoms associated with CAD such as angina and myocardial infarction. 1 CAD is a significant health concern globally, affecting both developed and developing countries, leading to high mortality and imposing substantial economic burdens on patients.2-4 Percutaneous coronary intervention (PCI) serves as a crucial therapeutic approach for CAD and has been scientifically proven to enhance the prognosis of patients with notable CAD. 5
In clinical practice, physicians frequently employ coronary computed tomography angiography (CCTA) technology in conjunction with multi-position coronary angiography (CAG) findings to visually evaluate the necessity of stent implantation in diseased vessels. 6 When vascular stenosis exceeding 20% is identified, a validated quantitative coronary angiography (QCA) algorithm is utilized for precise quantitative assessment. 7 However, this method has inherent limitations. The accuracy of visual assessment is heavily reliant on the expertise of the physician due to its subjective nature. 8 Furthermore, existing QCA algorithms may exhibit an inclination towards overestimating the degree of coronary stenosis, consequently leading to a notable false-positive rate. 9 Misinterpretation of disease severity by physicians can result in misguided treatment measures and subsequently elevate the risk of major adverse cardiac events such as all-cause mortality, non-fatal myocardial infarction, or emergency revascularization, ultimately contributing to an unfavorable prognosis.10–12
With the popularization of the concept of precision medicine, fractional flow reserve (FFR), which accurately assesses the impact of coronary stenosis on myocardial blood flow, is currently considered the gold standard for diagnosing CAD and has been incorporated into related guidelines in many countries. 13 However, as an invasive procedure, FFR inherently carries the potential risks of vascular injury, hemorrhage, and infection. 14 In recent years, there has been a gradual implementation of an enhanced approach for calculating DEEPVESSEL-FFR (DVFFR) using deep learning technology. 15 This advancement further integrates computational fluid dynamics (CFD) with traditional CCTA to assess cardiovascular diseases accurately and intelligently. It combines the non-invasiveness of CCTA with the accuracy of FFR diagnostics, representing a novel non-invasive method for assessing hemodynamic abnormalities in stenosed coronary arteries. 16 In a previous prospective study conducted on 63 patients undergoing DVFFR examination, the diagnostic performance of DVFFR was compared against wire-based FFR as the reference standard using indicators such as area under the curve (AUC), sensitivity, specificity, positive predictive value, and negative predictive value. The results demonstrated a high level of concordance between DVFFR and FFR, with comparable precision in identifying functional myocardial ischemia to that of the gold standard FFR, thus highlighting the exceptional accuracy of DVFFR. 17
Despite its significant advantages, DVFFR’s prevalence in medical practice remains insufficient. In clinical practice, physicians often rely on visual assessments and QCA algorithms to determine the degree of stenosis in coronary arteries and make decisions regarding revascularization treatment. However, this decision-making process may lead to overestimation or underestimation of lesions, resulting in erroneous treatment decisions. Such occurrences are prevalent in medical practice and can significantly increase the risk of adverse patient outcomes. The objective of this study was to identify distinct classes of CAD patients undergoing PCI using latent class analysis (LCA). Additionally, we aimed to investigate the association between these classes and both mistaken treatment decisions and major adverse cardiac events (MACE), with the goal of analyzing patient characteristics that necessitate a fractional flow reserve-guided stenting strategy for improved patient prognoses.
Methods
Study Population
This single-center cohort investigation was conducted at Beijing Anzhen Hospital, focusing on patients with coronary artery stenosis ranging from 30% to 90% in arteries exceeding a diameter of 1.5 mm, as confirmed by CCTA, who subsequently underwent PCI. The inclusion criteria were: (1) age range between 18 and 75 years, (2) a maximum interval of 3 months between CCTA and the initial CAG examination, without PCI performed during this period, and, (3) the provision of informed consent. A total of 6,900 individuals met these criteria. Exclusion criteria included: (1) a history of PCI or coronary artery bypass grafting (CABG), (2) poor CCTA image quality precluding DVFFR calculation, (3) presence of cardiogenic shock or cardiac arrest before PCI, (4) procedural failure of PCI, (5) malignant tumors impacting survival, and, (6) loss of follow-up. Ultimately, 3,840 patients were deemed eligible for analysis. Informed consent was duly obtained from each participant involved in the study.
Data Extraction
In our study, a comprehensive dataset was meticulously compiled, encompassing demographic information such as age and sex, along with a detailed record of comorbidities and medical history, including hypertension, hyperlipidemia, diabetes, acute myocardial infarction (AMI), stroke, peripheral arterial disease (PAD), smoking status, and alcohol consumption. Additionally, the study precisely measured and documented the values of DVFFR for the left anterior descending (LAD), left circumflex (LCX), and right coronary artery (RCA).
Procedures
CCTA imaging was conducted using a 256-row Revolution CT scanner (GE Healthcare, Waukesha, WI, USA). In preparation for the procedure, patients were administered sublingual nitroglycerine. The imaging protocol began with standard calcium scoring, followed by enhanced scanning using a bolus-tracking method. This scanning range extended from 1 cm below the tracheal bifurcation to the heart’s apex. For enhanced image clarity, an iodine-based contrast agent, Iopromide (Ultravist, Bayer AG, Germany, 370 mg iodine/ml), was injected at a rate of 4–6 ml/s, with the total administered volume ranging from 50 to 80 ml. 18
DVFFR employs an advanced, internally developed deep learning model known as a tree-structured recursive neural network to seamlessly integrate imaging, structural, and functional features along the vascular path for a comprehensive vessel assessment. This innovative approach enables accurate and rapid prediction of FFR values at each vascular point. Under the guidance of an experienced radiologist, DVFFR assessments utilize this model to intricately correlate anatomical and hemodynamic patterns within the coronary artery tree, as acknowledged by the Chinese National Medical Products Administration (NMPA). 19 By utilizing CCTA images, the software constructs a detailed three-dimensional arterial network model that facilitates nuanced DVFFR calculations. The algorithm considers arterial complexities, lesion specifics, and blood flow dynamics in a comprehensive manner to ensure thorough analysis. Assessment times range from 5 to 30 min/patient, depending on the quality of imaging data, as supported by various studies. 20
Coronary angiography was conducted by at least two experienced cardiologists during hospitalization. Prior to angiography, patients uniformly underwent antiplatelet therapy, receiving an initial dose of 300 mg of aspirin, followed by a maintenance dose of 100 mg, in addition to either clopidogrel (with an initial dose of 300 mg and a maintenance dose of 75 mg) or ticagrelor (initially 180 mg, followed by 90 mg). Furthermore, all patients were subjected to lipid-lowering therapy using statins, barring instances of statin intolerance caused by drug allergies, definitive statin-induced liver injury, myopathy, etc. A subset of patients was also treated with ezetimibe in combination with statins. In accordance with their clinical necessities, patients also received other essential medications. Throughout the surgical interventions, standard doses of unfractionated heparin (70 to 100 IU/kg) or bivalirudin were administered for anticoagulation purposes. The application of glycoprotein IIb/IIIa receptor antagonists was left to the discretion of the operating surgeon. To ensure a comprehensive evaluation of each coronary artery, imaging was carried out from at least two distinct angles for every artery. When necessary, additional specialized angles were employed, tailored to the patient’s specific coronary anatomy, to afford a complete and clear depiction of the coronary lesion areas. Upon the conclusion of the angiography, the decision to proceed with PCI was determined by the operating surgeon based on lesion characteristics. PCI involved balloon pre-dilation, utilization of specialized balloons, implantation of second-generation drug-eluting stents, and balloon post-dilation. All administered medications and PCI procedures conformed to the current clinical guidelines. 21
Outcomes
The primary outcome of this study was defined as mistaken treatment. This term specifically refers to cases where patients with a negative DVFFR (DVFFR > 0.80) underwent revascularization or those with a positive DVFFR (DVFFR ≤ 0.80) did not undergo revascularization. 17
The secondary outcome was a composite measure comprising MACE, which encompassed all-cause mortality, rehospitalization due to unstable angina (UA), and non-fatal myocardial infarction (MI). Patients underwent systematic follow-up assessments, which were conducted at 3, 6, 9, and 12 months initially, followed by evaluations at 24 and 36 months thereafter, performed by trained healthcare professionals. Data collection on MACE and medication usage was facilitated through direct patient or family visits to the outpatient office or via telephonic surveys. In cases where a singular adverse event occurred multiple times during the follow-up period, only the initial occurrence was considered for inclusion in this study.
Statistical Analysis
Latent class analysis was executed utilizing the poLCA package in R Statistical Software (R-project; R Foundation for Statistical Computing, Vienna, Austria, version 4.2.1), aiming to categorize beneficiaries based on eight distinct comorbidities and elements of medical history, namely hypertension, hyperlipidemia, diabetes, AMI, stroke, PAD, smoking status, and alcohol consumption. The derivation of latent class definitions was achieved through maximum-likelihood estimation. This approach was employed to ascertain the most prevalent patterns across the eight variables, considering a class range of 2 to 7. The determination of the optimal number of classes was guided by the analysis of the first minimum of the Akaike Information Criterion (AIC), Bayesian Information Criterion (BIC), and the Chi-square (χ2) statistic. An additional criterion for optimal class selection was the prevalence of the smallest class, which was required to constitute at least 10% of the cohort sample. Then the demographic and clinical characteristics of the study cohort were categorized based on the optimal LCA classes identified. To further validate the accuracy of the LCA stratification method, a random forest classification was employed to statistically demonstrate the significance of each variable in relation to the primary outcome.
For variables following a normal distribution, we presented them as mean ± standard deviation (SD), and their inter-group comparisons were conducted using analysis of variance (ANOVA). Categorical variables were reported as frequencies (percentages), with their comparative analysis between groups executed using the Chi-square test.
To investigate the association between LCA class and mistaken treatment, both univariate and multivariate logistic regression analyses were conducted, with results presented as odds ratios (ORs) and 95% confidence intervals (CIs). In a parallel approach, the association between LCA class and both MACE and its individual components was analyzed using univariate and multivariate Cox regression analyses, the results of which were expressed in terms of hazard ratios (HRs) and 95% CIs. The multivariate models incorporated confounding variables, such as sex, age, and the DVFFR values of LAD, LCX, and RCA.
Subgroup analyses were conducted to discern the relationship between LCA class and mistaken treatment across different age and sex subgroups, with the calculation of p for interaction. To circumvent the issue of having too few participants in certain age subgroups, the median age was used as the cutoff value. Multivariate logistic analysis within these subgroups was applied to compute OR values, using Class 3 as the reference group.
All tests conducted were two-sided, and a p<0.05 was deemed to indicate statistical significance. All methods were in strict adherence to relevant guidelines and regulations. Data analysis was performed using Stata V.15.1 software and R software (R-project; R Foundation for Statistical Computing, Vienna, Austria, version 4.2.1).
Results
Clinical Characteristics of Participants
A total of 3840 patients were included (Figure 1), with an average age of 55.81 ± 10.17 years. Among them, there were 1930 males (50.3%) and 1910 females (49.7%). The optimal number of classes was determined to be three. Significant differences were observed among the three classes of patients in terms of age, sex ratio, hypertension, hyperlipidemia, diabetes, AMI, stroke, PAD, smoking status, alcohol consumption, and the values of the LAD, LCX, and RCA measured by DVFFR (Table 1). Patients were divided into three different classes based on 8 types of comorbidities and medical history (Figure 2). In Class 1, the prevalence rates of hypertension, hyperlipidemia, diabetes, stroke, and PAD were 82.9%, 79.6%, 29.9%, 19.3%, and 34.6%, respectively. This class, having numerous comorbidities, was termed the comorbidities class. Class 2 had a 100% occurrence rate of drinking and smoking, with an AMI occurrence rate of 2.2%. All patients in this class engaged in risky behaviors of drinking and smoking; hence, it was named the smoking-drinking class. Class 3 patients had the fewest comorbidities and risky behaviors and were thus called the relatively healthy class.
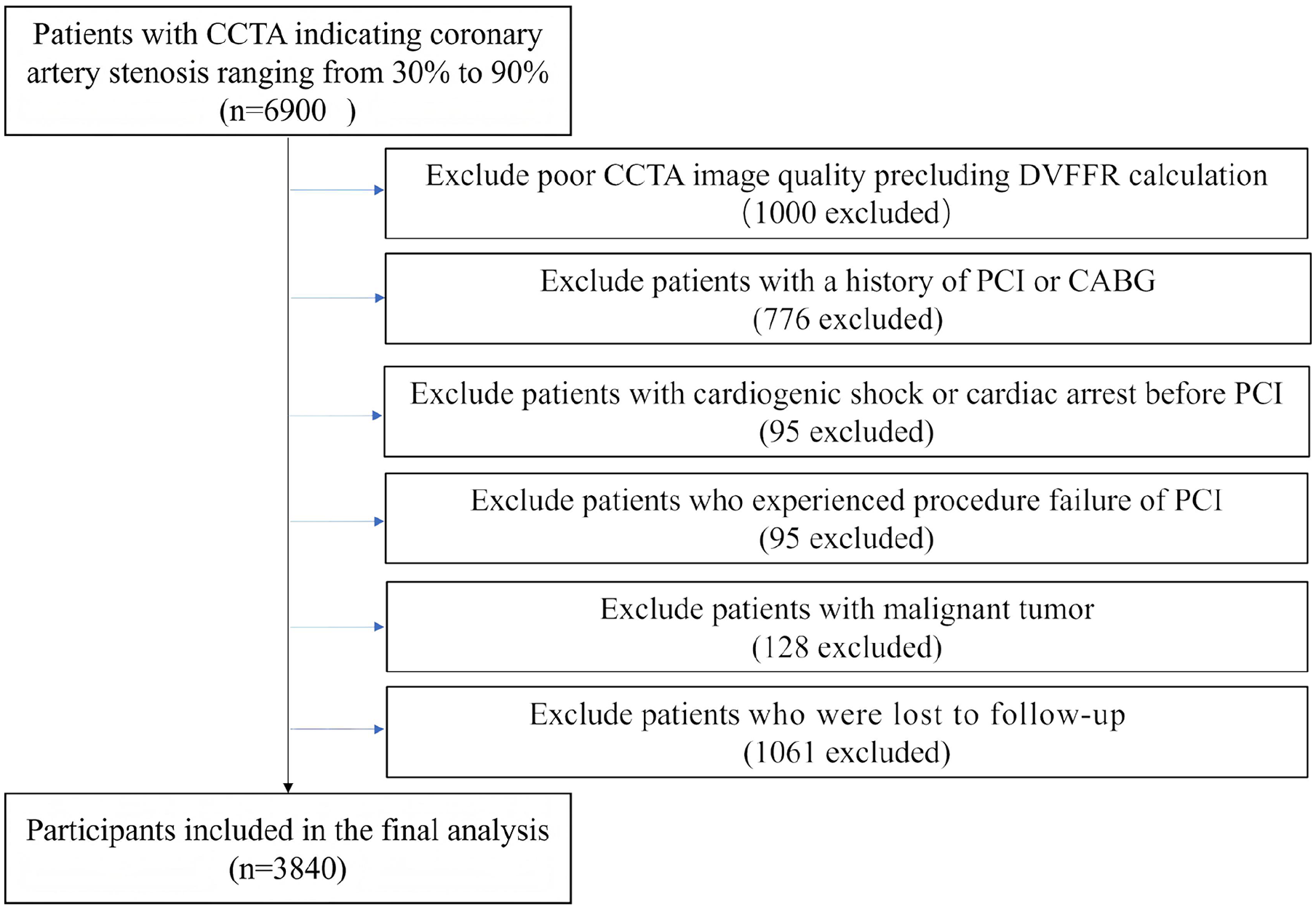
Flow chart of study population.
Characteristics of Patients Stratified by LCA Class.
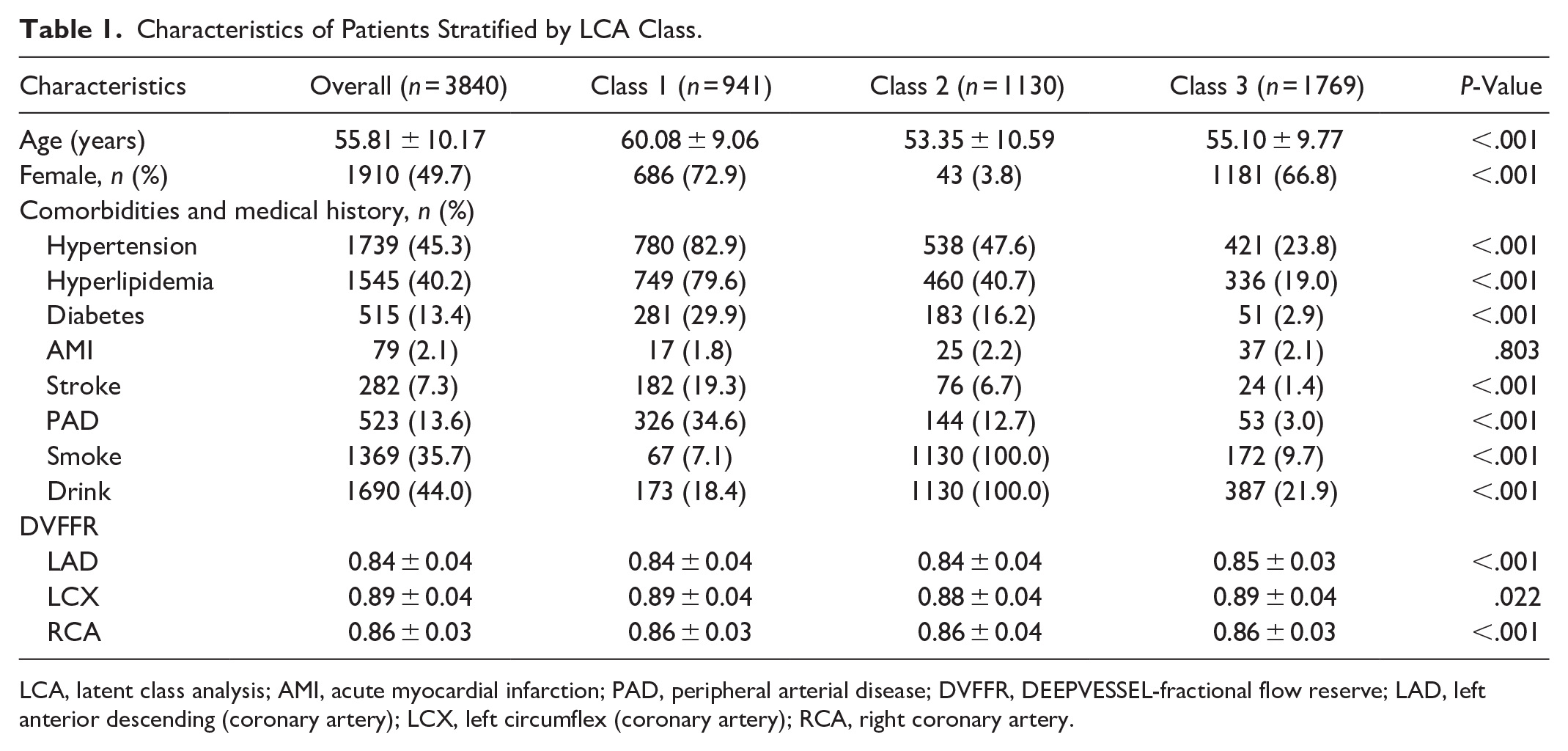
LCA, latent class analysis; AMI, acute myocardial infarction; PAD, peripheral arterial disease; DVFFR, DEEPVESSEL-fractional flow reserve; LAD, left anterior descending (coronary artery); LCX, left circumflex (coronary artery); RCA, right coronary artery.
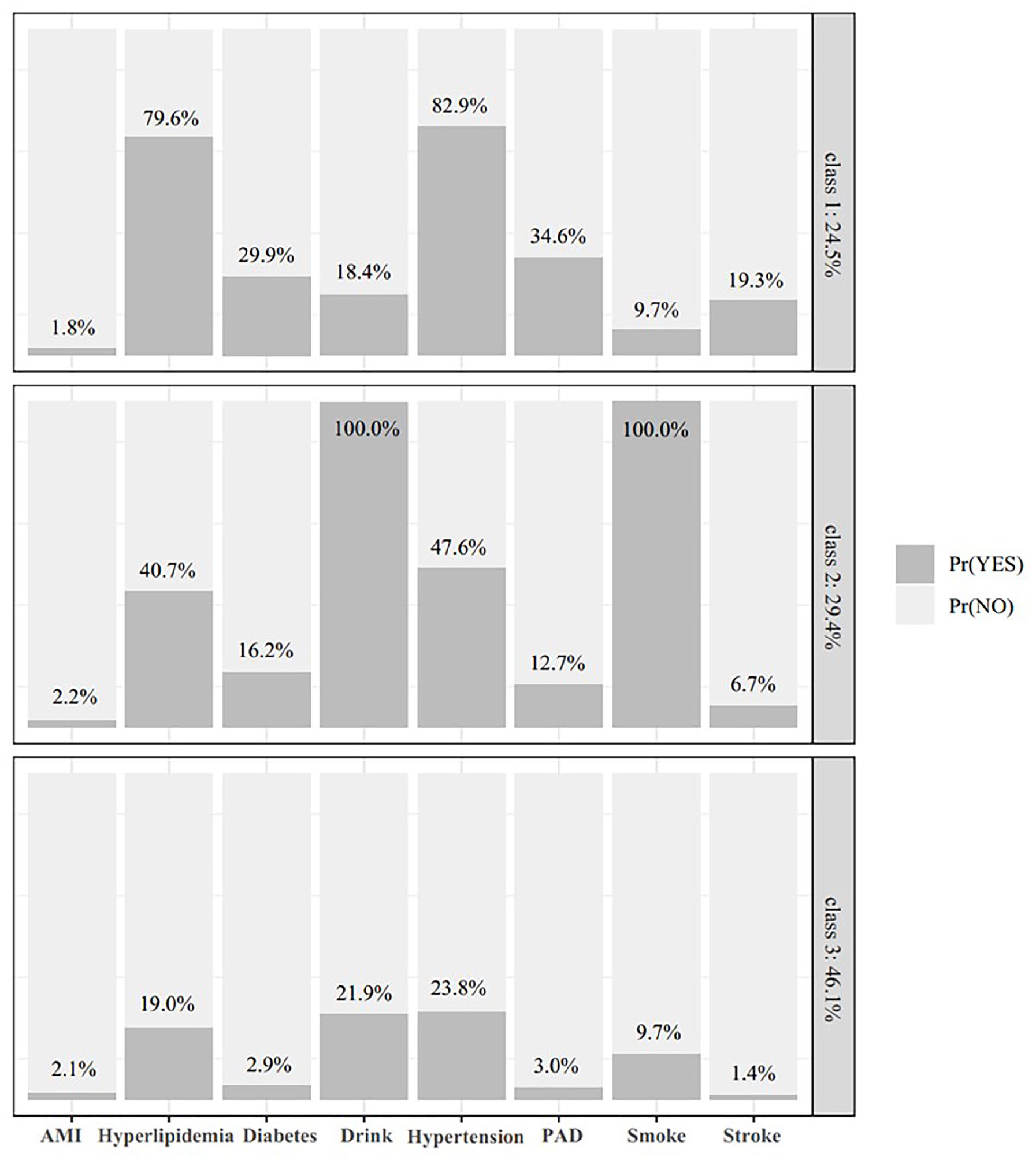
Characteristics of the optimal LCA class.
Outcomes
Among all patients receiving treatment, 11.1% experienced mistaken treatment, while 5.9% of patients encountered MACE. The incidence of mistaken treatment was highest among patients in Class 2, and this difference was statistically significant (Class 1 vs. Class 2 vs. Class 3: 14.2% vs. 15.4% vs. 6.7%, P < .001). Patients in Class 1 had the highest rates of MACE (Class 1 vs. Class 2 vs. Class 3: 7.0% vs. 6.6% vs. 4.8%, P < .001) and rehospitalization due to UA (Class 1 vs. Class 2 vs. Class 3: 6.1% vs. 6.1% vs. 4.1%, P < .001), with significant differences between classes. As for all-cause mortality (Class 1 vs Class 2 vs Class 3: 14.2% vs 15.4% vs 6.7%, P > .005) and non-fatal MI (Class 1 vs Class 2 vs Class 3: 0.4% vs 0.6% vs 0.7%, P > .005), the differences among the three classes did not achieve statistical significance (Table 2).
Outcomes of Patients Stratified by LCA Class.
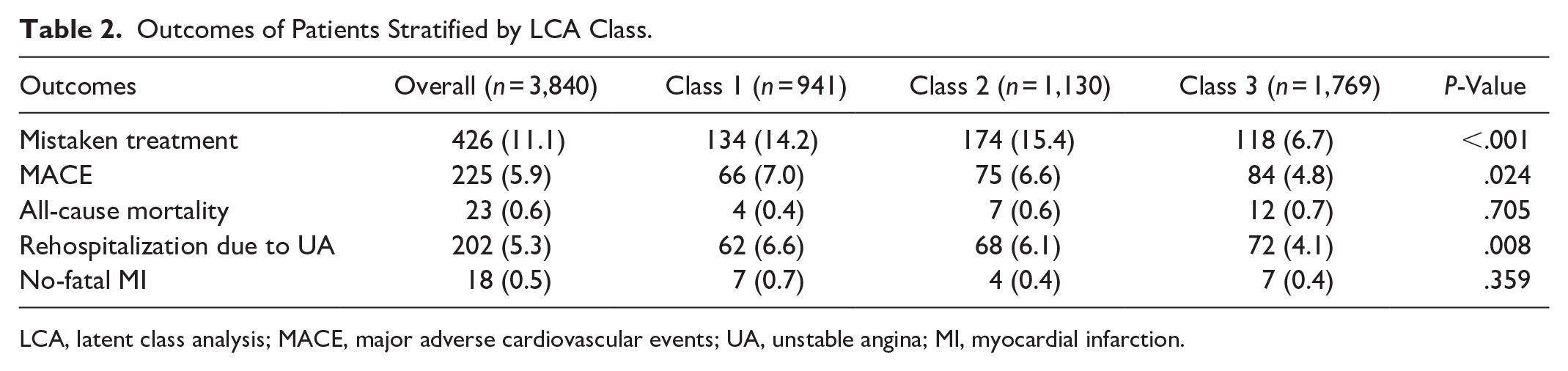
LCA, latent class analysis; MACE, major adverse cardiovascular events; UA, unstable angina; MI, myocardial infarction.
Association Between LCA Class and Outcomes
Logistic regression analysis was conducted to explore the correlation between clinical phenotypes and mistaken treatment. The results are shown in Table 3. Compared with the relatively healthy class (Class 3), patients in the comorbidities class (Class 1) (OR, 2.32; 95% CI, 1.79–3.02; P < .001) and the smoking-drinking class (Class 2) (OR, 2.55; 95% CI, 1.99-–3.26; P < .001) exhibited a significantly increased risk of mistaken treatment. However, there was no significant difference in the risk of mistaken treatment between the comorbidities class and the smoking-drinking class (OR, 0.91; 95% CI, 0.71–1.16; P = .461). After adjusting for age and sex, compared with the relatively healthy class (Class 3), patients in the comorbidities class (OR, 1.96; 95% CI, 1.49–2.57; P < .001) and the smoking-drinking class (Class 2) (OR, 1.69; 95% CI, 1.28–2.25; P < .001) still exhibited a significantly increased risk of mistaken treatment, although the risk was reduced. There was no significant difference between these two classes (OR, 1.07; 95% CI, 0.76–1.50; P = .707).
Association Between LCA Class and Mistaken Treatment Outcome.
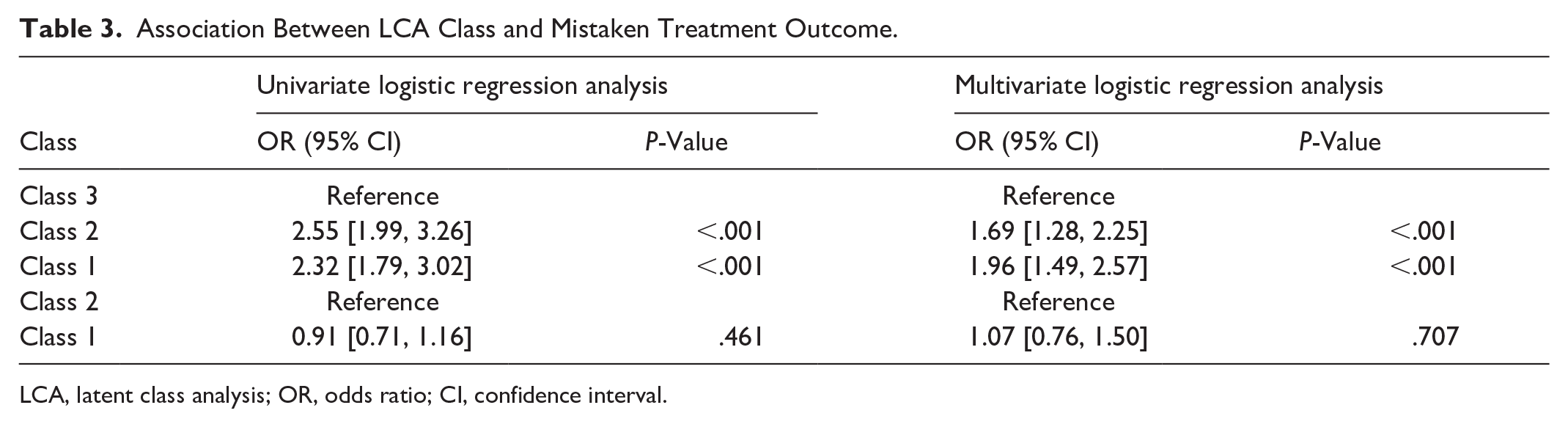
LCA, latent class analysis; OR, odds ratio; CI, confidence interval.
A Cox regression analysis was performed to examine the association between clinical phenotypes and MACE, with the findings detailed in Table 4. Relative to the relatively healthy class, both the comorbidities class and the smoking-drinking class exhibited a significantly elevated risk of MACE (Class 1 vs Class 3: HR, 95% CI: 1.73, 1.25–2.39, P < .001; Class 2 vs Class 3: HR, 95% CI: 1.41, 1.03–1.92, P < .001) as well as rehospitalization due to UA (Class 1 vs Class 3: HR, 95% CI: 1.91, 1.36–2.68, P < .001; Class 2 vs. Class 3: HR, 95% CI: 1.49, 1.07-2.08, P < .001). However, after adjusting for age and sex, the risk of MACE (Class 1 vs Class 3: HR, 95% CI: 1.53, 1.10–2.12, P = .012) and rehospitalization due to UA (Class 1 vs Class 3: HR, 95% CI: 1.71, 1.21–2.41, P = .003) remained significantly higher in the comorbidities class compared with the relatively healthy class. Conversely, no significant difference was found in the risk of MACE (Class 2 vs Class 3: HR, 95% CI: 1.09, 0.76–1.55, P = .645) and rehospitalization due to UA (Class 2 vs Class 3: HR, 95% CI: 1.13, 0.77–1.64, P = 0.538) between the smoking-drinking class and the relatively healthy class. While, in the analysis of all-cause mortality and non-fatal MI, no statistically significant differences were observed when comparing the comorbidities class and the smoking-drinking class to the relatively healthy class.
Association Between LCA Class and MACE, Including Individual MACE Components.
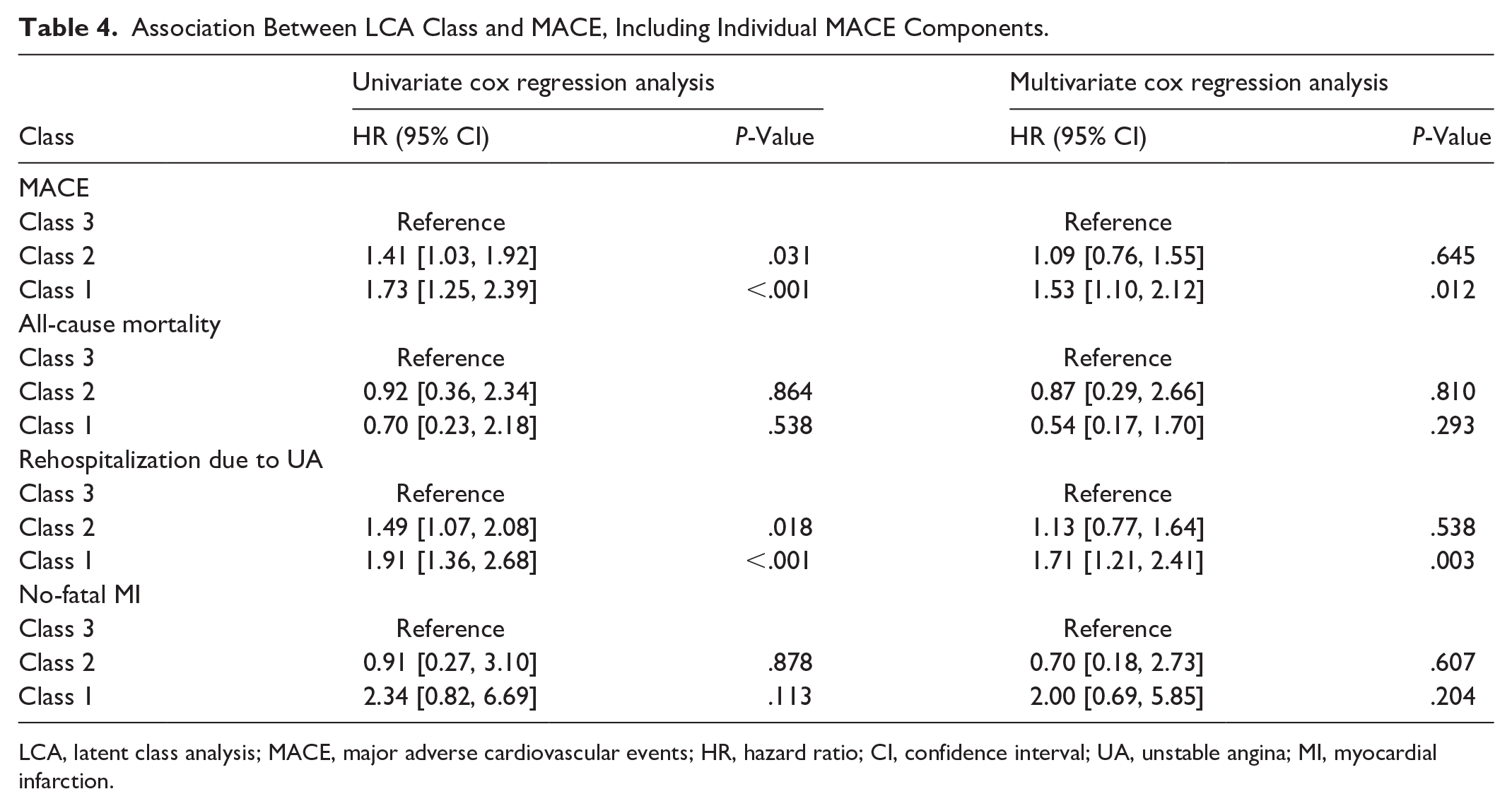
LCA, latent class analysis; MACE, major adverse cardiovascular events; HR, hazard ratio; CI, confidence interval; UA, unstable angina; MI, myocardial infarction.
Validation
The random forest classification demonstrated that hypertension and diabetes were the most influential predictors of mistaken treatment decisions, followed by smoking, stroke, and drinking behaviors, while acute myocardial infarction exhibited minimal predictive significance (Supplemental Figure S1). In this analysis, variable importance was quantified using the Mean Decrease Gini index, 22 with higher values indicating superior discriminative capacity within the classification model. These computational findings strongly corroborated our LCA stratification: Class 1 patients, defined by multiple comorbidities, showed hypertension and diabetes with the highest Gini importance metrics; Class 2 patients, characterized by smoking and drinking behaviors, similarly displayed substantial predictive influence in the model. This statistical validation confirmed the clinical relevance of our identified patient phenotypes in relation to treatment decision errors.
Subgroup Analysis
Subgroup analysis results (Figure 3) indicated that, within age subgroups and the male sex subgroup, compared with Class 3, both Class 1 and Class 2 significantly increased the risk of mistaken treatment. In contrast, within the female subgroup, only Class 1 showed a significant elevation in the risk of mistaken treatment compared with Class 3. Importantly, no significant interactions were observed within the subgroups of age and sex (P > .05).
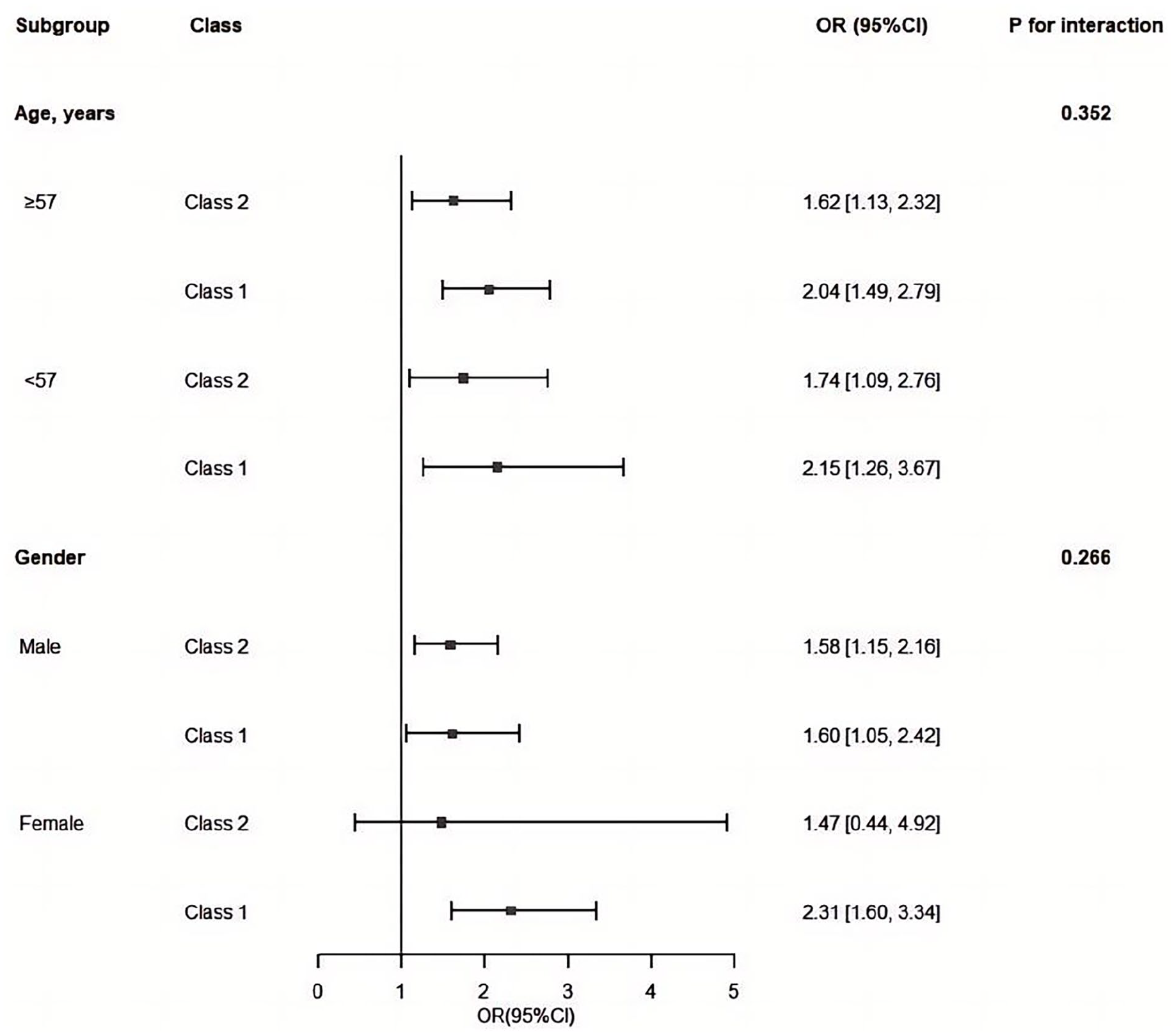
Subgroup analysis of associations between LCA class and mistaken treatment outcome.
Discussion
In the population with CAD undergoing PCI, we employed the LCA model to identify three classes. This study explored the correlation between different classes, the likelihood of patients receiving mistaken treatment, and their prognoses. The results indicated that patients in the comorbidities class and the smoking-drinking class were at an increased risk of receiving mistaken treatment compared with the relatively healthy class, with concurrently worse prognoses. However, no significant difference was observed in the risks and prognoses between the comorbidities class and the smoking-drinking class. Furthermore, this study did not find any significant interaction within the subgroups of age and sex. Using CCTA results to calculate DVFFR and guide clinical decisions may help advance the goal of precision treatment, offering patients more accurate and effective medical services.
Traditional risk factors contribute to the onset and progression of CAD, leading to poor patient prognoses. Previous studies demonstrated a significant correlation between CAD severity and long-term MACE risk. Of particular concern were CAD patients with a history of AMI, as their AMI history significantly worsened their prognoses. 23 Additionally, unhealthy lifestyle habits such as smoking and drinking also increased MACE risk in CAD patients.24,25 From a treatment perspective, co-existing stroke increased the risk of poor recovery outcomes in CAD patients; concomitant PAD significantly increased the risk of decreased CABG surgery efficacy.26,27 Pathologically, diabetes promoted an increase in coronary artery plaque volume in CAD patients, thereby increasing mortality risk. 28 Hypertension and hyperlipidemia were also widely recognized as independent risk factors for mortality in patients with CAD.29,30 Previous studies have classified patients with those risk factors using the LCA model. Jahangiry et al. 31 classified patients undergoing CABG into two groups based on 11 potential risk factors. One group was primarily characterized by obesity, diabetes, and hypertension. The other group was defined by smoking, drinking, opiate addiction, and a history of MI. This finding highlighted that individuals with these particular risk behaviors and history were vulnerable to developing severe CAD requiring surgical intervention at an earlier age than those whose risk profile was dominated by metabolic conditions. These group characteristics identified through LCA in this previous study exhibited similarities to our research, simultaneously providing potential evidence supporting the LCA classification scheme employed in our study. 31
Our study divided the population into three classes using the LCA model to explore which patient characteristics benefited most from preoperative DVFFR assessment and decision-making based on DVFFR results. DVFFR, known for its excellent safety and convenience, has shown significant value in clinical applications. Its advantage lies in not requiring specialized coronary guidewires, microcatheters, or the vasodilatory drugs needed for traditional FFR measurements. 32 Additionally, previous research indicated that DVFFR was non-inferior to traditional FFR, providing evidence-based medicine support for clinical decision-making guided by DVFFR. 17
Given the large base of CAD patients, physicians inevitably make errors in clinical judgment, often based solely on the visual assessment of coronary angiography narrowing. This may lead to delayed treatment for patients who truly need it or overtreatment for those who do not. Our study was the first to compare the evaluation efficacy of DVFFR with the traditional visual assessment of coronary angiography combined with the QCA algorithm, delving into the characteristics of patients prone to receiving mistaken treatment, thereby providing a more accurate basis for clinical decision-making. The findings suggested that for CAD patients with multiple comorbidities and smoking or drinking habits, relying solely on visual assessments of coronary angiography to evaluate lesion severity is insufficient. Further DVFFR examinations were necessary to ensure diagnostic accuracy. For patients with fewer comorbidities and risky behaviors, visual assessment of coronary angiography results already had high reliability, negating the need for additional tests, thus reducing the economic burden on patients and saving medical resources.
Another noteworthy aspect of the study is that there were no significant differences observed between the comorbidities class and the smoking-drinking class in terms of the risk of receiving mistaken treatment or the risk of major adverse cardiac events MACE. This observation further underscored the critical need for attention and intervention targeting patients’ unhealthy lifestyles, such as smoking and drinking. Despite the absence of significant differences in the risk of mistaken treatment, or MACE, between the comorbidities and smoking-drinking classes, both groups exhibited a trend toward an increased risk of MACE. This trend served as a reminder of the importance of closely monitoring the prognoses of individuals exhibiting these characteristics while maintaining a focus on diagnostic accuracy. Additionally, no significant interactions were found in the subgroup analysis, indicating that the impact of age and sex on the risk of mistaken treatment was consistent across different subgroups. This finding validated the general applicability of our conclusions across different age and sex groups, thus emphasizing the importance of preventing the risk of mistaken treatment in the entire population. Considering not all medical facilities have the capability to perform FFR assessments, CCTA, with its more relaxed implementation conditions, provides an innovative and reliable solution for areas with limited medical resources.
The study utilized a non-invasive assessment method, DVFFR, which relies on CCTA imaging that requires both contrast agent and radiation exposure, but avoids the invasive catheterization needed for traditional FFR. This approach emphasizes the importance of integrating CCTA with DVFFR in evaluating coronary artery stenosis and its impact on myocardial blood flow. This approach proposed an innovative strategy to reduce erroneous treatment decisions and optimize patient management in PCI. By combining advanced imaging techniques with deep learning algorithms, DVFFR enabled a more accurate and personalized assessment of CAD, potentially improving diagnostic accuracy and guiding treatment decisions. This research highlighted the application of precision medicine in contemporary cardiovascular disease management and showcased the potential of leveraging deep learning technology to enhance disease diagnosis and inform treatment strategies. The integration of CCTA and DVFFR represented a promising step towards a more targeted and effective approach to managing patients with CAD undergoing PCI.
Our findings offer a novel perspective for optimizing personalized CAD management. Previous research by Yang proposed a model for predicting CAD prognosis, and our LCA-identified subgroups, such as the smoking-drinking group and the complication group, align with their classification to some extent, validating our study’s reliability. 33 However, our results regarding mistaken treatment decisions are unprecedented, providing new insights into CAD management. Future research could integrate these findings into existing risk prediction models or develop new decision-support tools. For example, a comprehensive model incorporating patient phenotypes and risks of mistaken treatment decisions could be constructed. Such a model would not only assess prognostic risk but also predict potential treatment decision errors, aiding clinicians in formulating more precise, individualized treatment plans. Nonetheless, realizing this goal necessitates further prospective studies, incorporating additional potential factors and validation in larger populations. This approach would contribute to the development of more reliable and practical clinical decision-support tools, ultimately enhancing the personalization of CAD management and improving patient outcomes.
Limitations
This study had several limitations. Since the DVFFR was calculated based on previous CCTA results, its accuracy might have been influenced by the quality of the CCTA images. While previous studies have shown DVFFR to be non-inferior to invasive FFR, it’s important to acknowledge that DVFFR may have limitations compared with invasive or other non-invasive methods for assessing functional coronary artery stenosis. Additionally, as a single-center retrospective study, there may have been selection bias, and we were unable to perform external validation. Despite efforts to adjust for confounders, there may be other unmeasured or unknown factors that could influence the observed associations. Future large-scale, multi-center prospective studies are needed to validate the conclusions of this study.
Conclusion
The present study used the LCA model to categorize CAD patients undergoing PCI into three groups based on eight risk factors. Compared with patients in the relatively healthy class, those in the comorbidities class and the smoking-drinking class were more likely to receive mistaken treatment, which was further associated with poorer prognoses and manifested as a higher risk of MACE. However, it is noteworthy that no significant differences were observed in the risk of mistaken treatment decisions or MACE risk between the comorbidities class and the smoking-drinking class. This conclusion remained consistent across different age and sex subgroups.
Supplemental Material
sj-docx-1-ang-10.1177_00033197251350182 – Supplemental material for Latent Class Analysis Identifies Distinct Patient Phenotypes Associated With Mistaken Treatment Decisions and Adverse Outcomes in Coronary Artery Disease
Supplemental material, sj-docx-1-ang-10.1177_00033197251350182 for Latent Class Analysis Identifies Distinct Patient Phenotypes Associated With Mistaken Treatment Decisions and Adverse Outcomes in Coronary Artery Disease by Jing Qi, Zhiqiang Wang, Xiaoteng Ma, Zhijian Wang, Yueping Li, Lixia Yang, Dongmei Shi and Yujie Zhou in Angiology
Footnotes
Acknowledgements
None.
Ethical considerations
The study was conducted in accordance with the Declaration of Helsinki and was approved by the Ethics Committee of Beijing Anzhen Hospital (Ethics approval number: 2020-024I), with the need for written informed consent waived.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Author Contribution
All authors contributed to: (1) substantial contributions to conception and design, or acquisition of data, or analysis and interpretation of data, (2) drafting the article or revising it critically for important intellectual content, and, (3) final approval of the version to be published.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the grant from National Key Research and Development Program of China (2022YFC3602500).
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The raw data analyzed in this article can be available upon request from the authors.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
