Abstract
Aims
To synthesize evidence on outcomes of treatment strategies for management of primary hepatic artery aneurysms (HAAs).
Methods
A PRISMA-compliant systematic review was conducted. Due to rarity of the disease, all reported cases which underwent operative or endovascular intervention for true HAA were pooled from case reports and case series to create a single cohort of patients. Descriptive statistics, logistic regression models, and Kaplan-Meier statistics were used for analyses.
Results
62 patients from 41 case reports and one case series were included. The mean age was 60.9 and 77% were male; 66% were symptomatic with pain as the most common symptom (76%). The mean diameter and length of aneurysms were 47.4 mm and 55.8 mm, respectively. The anatomy of aneurysm was hostile in 39% and 11% were ruptured at presentation. In terms of treatment, 74% were treated via operative approach and 26% via endovascular approach. Hostile anatomy was the only predictor for selecting operative approach (OR: 8.72, P = .031). Technical success was achieved in 98%; postoperative mortality and morbidity occurred in 5% and 16%, respectively. The probabilities of graft patency at 60 months were not different between the operative and endovascular approaches (86% vs 90%, P = .961); however, the probability of recurrence-free survival was higher after operative approach (100% vs 85%, P = .046).
Conclusions
Accepting type 2 error and confounding by indication as the limitations, both operative and endovascular techniques seem to be safe and feasible in management of true HAA. Hostile anatomy may be the main determinant of selecting operative approach over the endovascular approach.
Introduction
True hepatic artery aneurysms (HAAs) are rare with incidence of less than 0.2% representing up to 20% of visceral artery aneurysms. 1 Although most HAAs are asymptomatic, they may cause abdominal pain, jaundice, or gastrointestinal bleeding; moreover, they can rupture in approximately 40% of cases resulting in hypovolemic shock with a high risk of mortality if not recognized and managed early. 2 The risk of rupture of HAA increases when the diameter is more than 2 cm; consequently, based on the recommendations from the current guidelines, HAA with a diameter greater than 2-2.5 cm should be treated.3,4
Hepatic artery aneurysm can be managed via endovascular approach or operative approach. Endovascular treatment options include coil embolization or placement of covered stent graft.3,4 Operative treatment options include liver resection, interposition bypass using vein or prosthetic grafts, arterial transposition using splenic or gastroepiploic arteries, exclusion aortohepatic bypass using vein or prosthetic grafts, aneurysmectomy without reconstruction when adequate collateral supply is present, patch angioplasty, or primary anastomosis when possible.3,4 Nevertheless, due to rarity of the disease, the available evidence on treatment strategies for management of true HAA in terms of indications, success rate, and outcomes is indeed limited. Consequently, we aimed to conduct a comprehensive meta-analysis to synthesize the best available evidence on treatment strategies for management of true HAA.
Adopted Evidence Synthesis Strategy due to Rarity of HAA
Hepatic artery aneurysm is a rare condition; therefore, it was expected that the best available evidence consists mainly of case reports and a limited number of case series. We implemented the following strategies in order to use the best available evidence efficiently: (1) We created a separate cohort of patients from the individual case reports where the required data at patient level was available. (2) We pooled the results of the above cohort with results of the available case series.
Accepting that case-based evidence may be vulnerable to publication bias, confounding by indication, and the reported outcomes may not reflect the real-world practice, the above strategy would allow evidence synthesis using data from case reports and case series which is currently considered as the best available evidence.
Methods
Methodological and Reporting Compliance
The methodology of the study followed the Cochrane Handbook for Systematic Reviews (version 6.4), 5 and the reporting of the study followed the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) 2020 statement standards. 6
Eligibility Criteria
Study Design
Due to rarity of true HAA, it was expected that the best available evidence to be developed mainly from case reports and a very limited number of case series; consequently, all case reports, case series, case-control studies, cohort studies, and randomized controlled trials were considered eligible for inclusion in this study. Meta-analyses, systematic reviews, review articles, and scoping reviews were excluded. Moreover, the articles with no available full text and without adequately detailed abstracts were excluded.
Population
All patients aged 18 or over who underwent intervention for true HAAs were eligible for inclusion. Both symptomatic and asymptomatic cases were included. Patients with pseudoaneurysms (false aneurysms) related to underlying abdominal pathology, abdominal trauma, previous abdominal procedures, or liver transplant were excluded.
Intervention
Both endovascular and operative approaches were considered as interventions of interest. Endovascular treatment options of interest included coil embolization or placement of covered stent graft. The operative treatment options of interest included liver resection, interposition bypass using vein or prosthetic grafts, arterial transposition using splenic or gastroepiploic arteries, exclusion aortohepatic bypass using vein or prosthetic grafts, aneurysmectomy without reconstruction when adequate collateral supply was present, patch angioplasty, or primary anastomosis when possible.
Outcomes
The outcomes included technical success (defined as successful completion of the procedure or operation regardless of the outcomes), 30-day mortality (defined as death due to any cause within 30 days of the procedure or operation), 30-day complications (defined as any complications within 30 days of the procedure or operation), length of hospital stay, graft occlusion, need for reintervention, long-term complications (defined as complications occur or persist after 30 days of the procedure or operation), primary graft patency (defined as the time from placement of graft until it becomes blocked or non-functional or it requires intervention to maintain its patency), and aneurysm recurrence-free survival.
Information Sources and Search Strategy
Two independent authors used search keywords, limits, thesaurus headings, and operators to develop a search strategy which was used in the following electronic sources: MEDLINE, Scopus, CENTRAL, the ISRCTN registry, the ICTRP registry, and ClinicalTrials.gov. The following combination of keywords was used: (hepatic artery [MeSH Terms] OR hepatic artery) AND (aneurysms [MeSH Terms] OR aneurysm). The search had no language restrictions, and the last date for the search was 20 June 2025. The reference lists of the included studies were also searched for more eligible studies.
Study Selection, Data Collection, and Data Items
The titles and abstracts of the identified articles were reviewed by two separate authors, and the full text of potentially eligible articles was retrieved to select the eligible articles. A third author was consulted if there was disagreement in study selection between the first two authors. The data items (bibliometric parameters, study design, age, sex, symptoms, site of aneurysms, diameter and length of aneurysms, hostile anatomy of aneurysms (defined as no proximal neck at the celiac trunk, involvement of proper hepatic artery bifurcation, or involvement of bifurcation of left and right hepatic arteries), emergency presentation (acutely unwell with jaundice due to external compression by HAA, gastrointestinal bleeding, or hypovolemic shock due to HAA rupture), elective presentation (asymptomatic, abdominal pain, or clinically stable jaundice), treatment received, type of graft or repair, and the outcome measures) were determined by the authors at the protocol development stage followed by a pilot-testing technique of randomly selected studies. Data collection was done by two independent authors.
Study Risk of Bias Assessment
The Joanna Briggs Institute critical appraisal tools were used by two independent authors to evaluate the risk of bias in the included case reports and case series. A third author was consulted if there was any disagreement.
Effect Measures and Synthesis Methods
The MedCalc software (version 22.009) was used for analyses. The baseline characteristics in the cohort of case reports were summarized using descriptive statistics; mean for continuous variables and percentages for dichotomous variables. Because individual-level data related to baseline characteristics and outcomes were available from the case reports, a cohort of patient was created which allowed primary statistical analyses such as Kaplan-Meier survival analysis and logistic regression analyses. Kaplan-Meier survival analysis was performed to determine probability of primary graft patency and aneurysm recurrence-free survival. Moreover, logistic regression analyses were modeled to identify predictors of selecting operative approach instead of endovascular approach. Age, symptomatic status, aneurysm diameter, emergency presentation, hostile anatomy, and ruptured aneurysm were considered as independent variables, and the treatment approach was considered as the dependent variable. The analyses were exploratory, unit of analysis was individual patient, and in case of missing data, the protocol planned to contact the corresponding author of the article for information. All statistical tests were two-tailed, and statistical significance was assumed at P < .05.
Results
Study Selection and Study Characteristics
The search yielded 2543 articles. Screening the titles and abstracts directly excluded 2500 articles because they did not meet principal eligibility criteria. The full-text review of the remaining 43 articles also excluded 7 articles (5 articles had no full-text, one did not have stratified data for HAA, and one article had overlapping data with another eligible article). Consequently, 36 articles, 41 case reports,7-40 and one case series, 41 comprising 62 patients, were included. The study PRISMA flow diagram is shown in Supplemental Figure 1. The details of included articles are provided in Supplemental Table 1.
Risk of Bias in Studies
The results of risk of bias assessment for case reports based on Joanna Briggs Institute critical appraisal tools are shown in Supplemental Table 2.
Baseline Characteristics of Included Population
Baseline Characteristics of the Included Patients
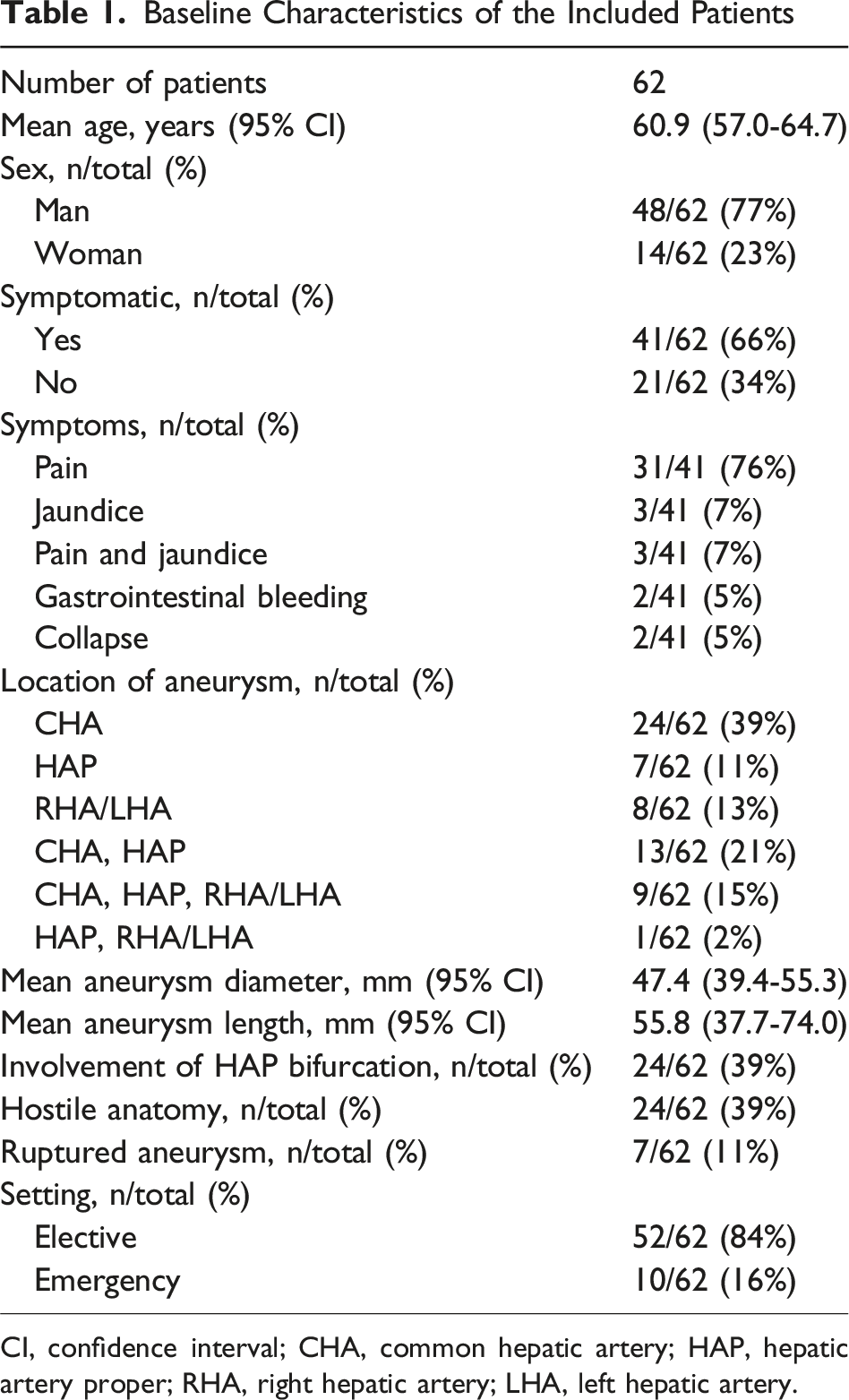
CI, confidence interval; CHA, common hepatic artery; HAP, hepatic artery proper; RHA, right hepatic artery; LHA, left hepatic artery.
Treatment Strategies
Detail of the Therapeutic Procedures Performed
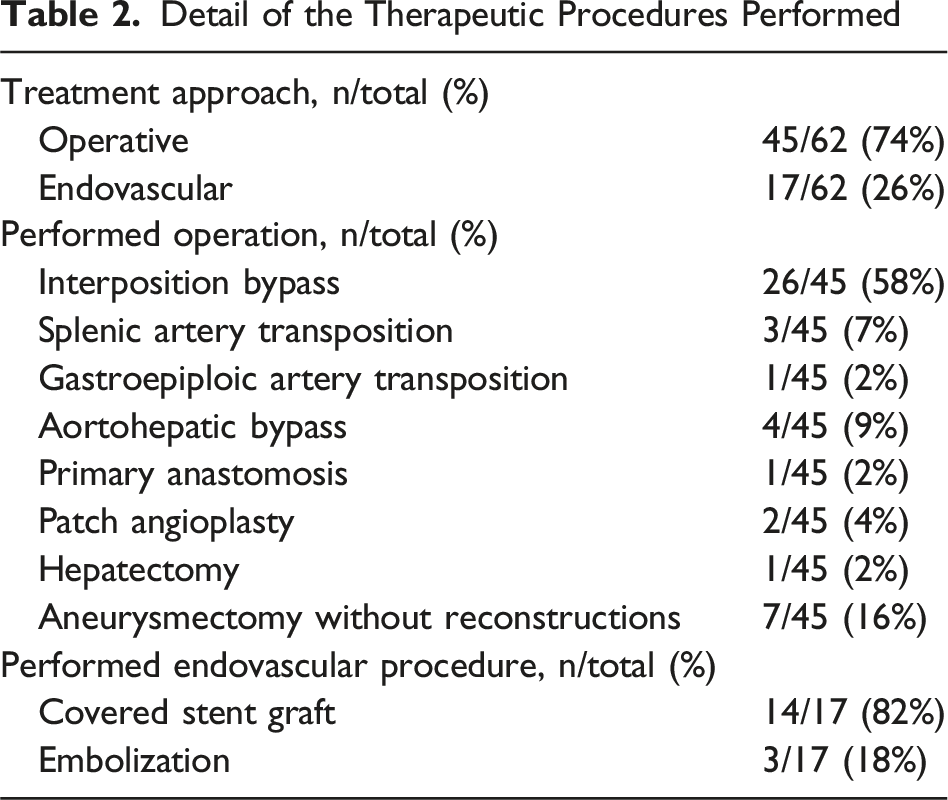
Outcomes
Summary of Outcomes
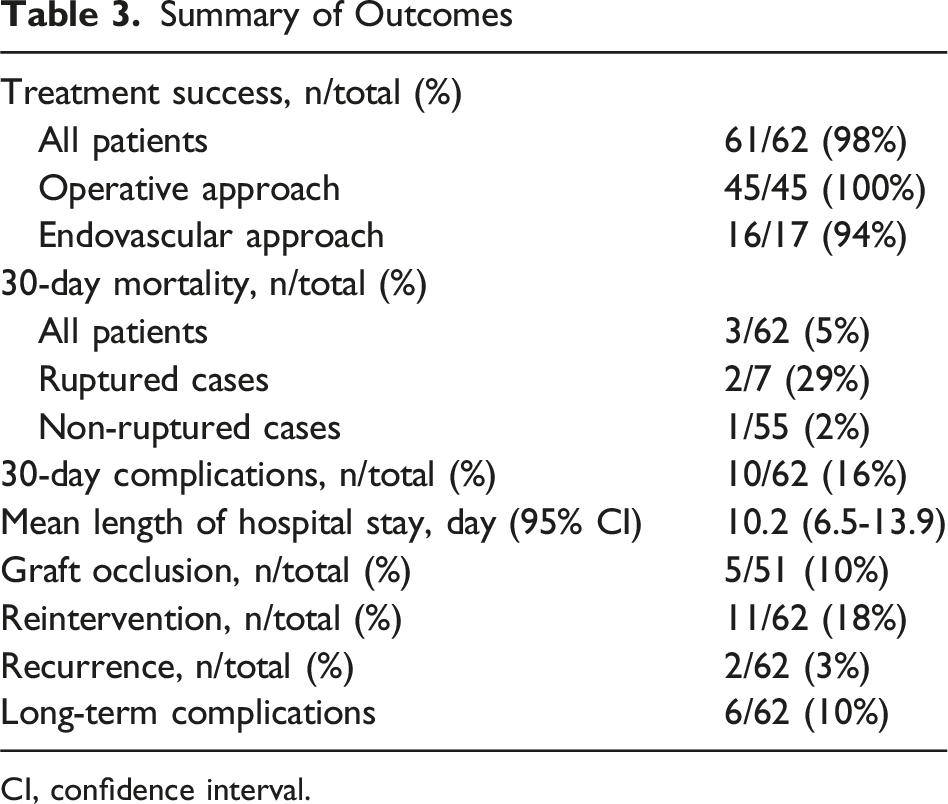
CI, confidence interval.
Primary Patency
Kaplan-Meier survival analysis showed that probability of primary patency at 60 months was 87% in all cases, 90% after endovascular approach, and 86% after operative approach. There was no difference in primary patency between endovascular and operative approaches (P = .961) (Supplemental Figure 2). Subgroup analysis based on reconstruction methods used during operative approach showed that the probability of primary patency at 24 months was 100% after arterial transposition, 80% after interposition bypass, and 67% after aortohepatic bypass. Subject to type 2 error, there was no statistical difference between the methods used (P = .529) (Supplemental Figure 3).
Recurrence-free Survival
Kaplan-Meier survival analysis showed that the probability of recurrence-free survival at 60 months was 95% in all cases, 85% after endovascular approach, and 100% after operative approach (Supplemental Figure 4). The probability of recurrence-free survival at 60 months was higher after operative approach (P = .046). Subgroup analysis based on endovascular techniques used showed that the probability of recurrence-free survival at 24 months was 90% after covered stent graft and 67% after embolization. Subject to type 2 error, there was no statistical difference between the technique used (P = .284) (Supplemental Figure 5).
Predictors for Selecting Operative Approach
Results of Logistic Regression Analysis for Predictors of Selecting Operative Approach Instead of Endovascular Approach
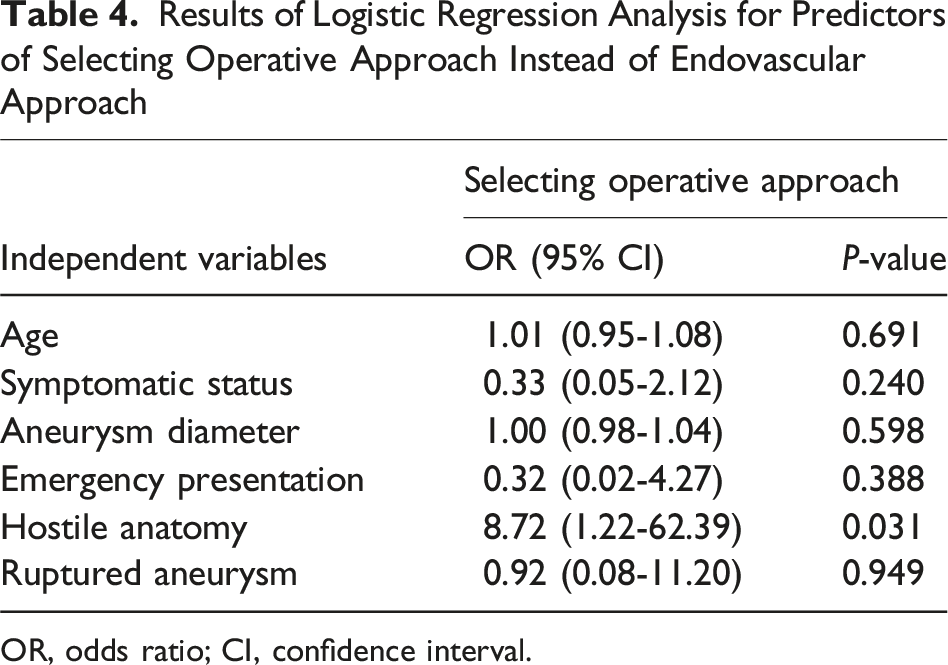
OR, odds ratio; CI, confidence interval.
Discussion
We conducted a comprehensive meta-analysis to synthesize the best available evidence on treatment strategies for management of true HAA. Analysis of 62 patients from 41 case reports and one case series showed that both operative and endovascular techniques were feasible and safe in management of true HAA. Hostile anatomy was the main determinant of selecting operative approach over the endovascular approach. While there was no difference in primary patency between the operative and endovascular techniques, the operative techniques were associated with better recurrence-free survival.
This study is the first meta-analysis which evaluates treatment strategies for management of true HAA; therefore, the results cannot be directly compared with other studies. However, Barrionuevo et al 1 conducted a systematic review to investigate management of all visceral artery aneurysms and pseudoaneurysms including renal artery, splenic artery, hepatic artery, pancreaticoduodenal and gastroduodenal arteries, superior mesenteric artery, celiac artery, jejunal, ileal, and colic arteries, and gastric and gastroepiploic arteries. 1 Barrionuevo et al 1 showed that although there was no difference in mortality between open and endovascular approaches, the endovascular approach resulted in shorter length of hospital stay, lower rates of cardiovascular complications, and higher rates of reintervention. 1 However, due to combining true aneurysms with pseudoaneurysms, including different types of visceral aneurysms, and different analytical strategies to the current study, the results from the study by Barrionuevo et al 1 cannot be directly compared with the results of the current study.
Both operative and endovascular techniques were associated with high technical success rate. However, most cases with hostile anatomy were treated operatively. This suggests that the high technical success rates were likely to be due to confounding by indications, hence high success rate. This may suggest that if cases with hostile anatomy had undergone endovascular treatment, the risk of technical success or outcomes might have been different. For example, only 2 patients with hostile anatomy underwent endovascular treatment and one of them required reintervention due to endoleak 2 months after the procedure. Consistent with the above, hostile anatomy (no proximal neck at the celiac trunk, involvement of proper hepatic artery bifurcation, or involvement of bifurcation of left and right hepatic arteries) was the only predictor for selecting operative approach instead of endovascular approach based on logistic regression analysis.
Among the patients who underwent operative management, 16% had aneurysmectomy without reconstructions with good short-term and long-term outcomes. These patients either had replaced left or right hepatic arteries, or had very good collateral vessels; hence, the lack of arterial reconstruction did not compromise the blood supply to the liver. This is a very important finding and highlights that aneurysmectomy on its own may be sufficient and appropriate in cases with good collateral arterial supply.
Subgroup analyses did not show statistically significant differences in primary patency between different operative treatment strategies. Similarly, there was no statistically significant difference in recurrence-free survival between different endovascular treatment options. We believe that this could be due to type 2 error associated with small sample size of current study. Visual assessment of Kaplan-Meier curves suggests that use of interposition bypass or arterial transposition may be preferred techniques to aortohepatic bypass unless there is no proximal neck at the celiac trunk. Moreover, use of covered stent graft may be the preferred technique to coil embolization. Nevertheless, larger sample size is required for definite conclusions.
The European Society for Vascular Surgery (ESVS) published clinical practice guidelines on the management of diseases of the mesenteric and renal arteries and veins which recommended endovascular or open surgical treatment of asymptomatic HAA with a diameter ≥30 mm. 42 While the ESVS evidence synthesis team recognized the trend towards endovascular repair of HAA, they did not find adequate evidence to provide indications regarding either the type of treatment or thresholds for repair of HAAs; consequently, their recommendations were based on the evidence from studies conducted on other visceral artery aneurysms. 42 Moreover, the Society for Vascular Surgery clinical practice guidelines on the management of visceral aneurysms (not updated since 2020) recommended an endovascular-first approach to all HAAs when anatomically feasible but also supported open technique. 3
The current study has the following limitations. The sample size was small which would subject the results to type 2 error. Moreover, the included cases in this study underwent operative or endovascular procedure based on the anatomy of the aneurysm, expertise available, and patient’s clinical circumstances; therefore, the results of current study are subject to confounding by indication. We demonstrated the confounding by indication using logistic regression analysis and interpreted the results taking the above points into accounts. The available evidence is derived mainly from case reports which inevitably subject the results to selection bias. We applied Kaplan-Meier survival statistics on aggregated case report data. While this is a recognized evidence synthesis strategy when available evidence is limited to case reports,43,44 Kaplan-Meier analysis assumes non-informative censoring which may induce bias when used for selectively published cases. On the other hand, the small sample size might have affected the results of logistic regression analyses as reflected by the wide confidence interval for hostile anatomy and ruptured aneurysm.
While the results of current study support safety and feasibility of both operative and endovascular management of true HAAs, the findings should be interpreted cautiously given anatomy-based selection of treatment modality, substantial heterogeneity in reconstruction techniques, and the rarity of complications and reinterventions. Consequently, the results of current study are mainly descriptive and should be used mainly for hypothesis synthesis in future studies rather than for establishing comparative effectiveness. Nevertheless, the current study provides the best available evidence on treatment strategies for true HAA and it used objective and robust methods in evidence synthesis. Therefore, in absence of higher level of evidence, the results of current study may also help decision-making in clinical practice in management of such a rare condition.
Based on the results of the current study, the following statements may be reasonable as implications for real practice: • True HAA with hostile anatomy (no proximal neck at the celiac trunk, involvement of proper hepatic artery bifurcation, or involvement of bifurcation of left and right hepatic arteries) may not be suitable for endovascular treatment and should be treated using operative approach. • Both endovascular and operative techniques are feasible and safe in management of true HAA with favorable anatomy; however, operative approach may result in better recurrence-free survival. • In presence of adequate collateral arterial supply to the liver, aneurysmectomy without reconstructions may be safe with satisfactory outcomes. • The risk of mortality in cases with ruptured true HAA is high, and the operative approach may be preferred in cases with extrahepatic rupture.
Conclusions
Accepting type 2 error and confounding by indication as the limitations, both operative and endovascular techniques seem to be safe and feasible in management of true HAA. Hostile anatomy may be the main determinant of selecting operative approach over the endovascular approach.
Supplemental Material
Supplemental Material - Treatment Strategies for Management of True Hepatic Artery Aneurysms: A Systematic Review and Meta-Analysis
Supplemental Material for Treatment Strategies for Management of True Hepatic Artery Aneurysms: A Systematic Review and Meta-Analysis by Shahab Hajibandeh, Shahin Hajibandeh, Giorgio Alessandri, and Nicola de Liguori-Carino in The American Surgeon™
Footnotes
Ethical Considerations
Patient consent and approval from Research Ethics Committees were not required in this study because the study design was a meta-analysis which did not have direct involvement of patients and used non-identifiable data.
Author Contributions
Conception and design: NDL and GA.
Data collection and data analysis: Shahab H and Shahin H.
Analysis and interpretation: Shahab H and Shahin H.
Writing the article: Shahab H and Shahin H.
Critical revision of the article: Shahab H, Shahin H, GA, and NDL.
Final approval of the article: Shahab H, Shahin H, GA, and NDL.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The corresponding author (Shahab H) will provide any additional data related to this study on reasonable request.
Supplemental Material
Supplemental material for this article is available online.
