Abstract
Background
Pancreaticoduodenectomy (PD) is a complex surgery that often has the best outcomes at high-volume centers. The influence of neighborhood socioeconomic status and location of care is poorly studied. This study aims to evaluate the relationship between hospital volume, patient outcomes, and socioeconomic disparities.
Methods
We utilized a statewide hospital discharge database from Pennsylvania (2017-2021) to analyze 1316 PD cases. Hospitals were categorized by volume based on the total number of cases performed in the 5-year study period. Multivariable logistic regression was employed to assess mortality, 30-day readmission, and non-routine discharge, adjusting for patient demographics, hospital characteristics, and Distressed Communities Index (DCI) scores.
Results
Patients in lowest-volume hospitals are more likely to live in distressed communities compared to those in medium- and higher-volume hospitals. Outcomes were similar between medium- and higher-volume hospitals for mortality (AOR = 0.578, P = 0.472), readmission (AOR = 1.118, P = 0.666), and non-routine discharge (AOR = 1.249, P = 0.289). Among patients from distressed communities, there were no significant differences in mortality, readmission, or non-routine discharge between medium- and higher-volume hospitals (all P > 0.4). The travel distance between a lowest- vs medium-volume hospital is not substantially different.
Conclusions
Urban distressed patients are close to medium-volume centers but disproportionately go to lowest-volume centers with worse outcomes. Medium-volume hospitals provide clinical outcomes for PD surgery that are comparable to those of higher-volume hospitals and should serve as a viable alternative for patients from distressed communities who face access barriers to high-volume centers.
Introduction
Pancreaticoduodenectomy (PD), commonly referred to as the Whipple procedure, is a complex surgical intervention predominantly indicated for malignant tumors of the pancreas, periampullary carcinomas, and cholangiocarcinoma. It is widely recommended that PD be performed in high-volume hospitals, 1 as these institutions demonstrate superior clinical outcomes. Numerous studies have consistently shown that high-volume hospitals are associated with lower mortality rates, reduced readmission rates, shorter hospital stays, and fewer postoperative complications compared to low-volume hospitals.2-5 Importantly, several studies also demonstrate equivalent outcomes at medium- compared to high-volume centers.6,7 With an increasingly educated and mobile patient population, high- and medium-volume centers have increased their volume while many low-volume centers have stopped performing complex surgical procedures altogether. It is acknowledged that as this landscape is evolving, certain patient groups are at risk of losing access to complex surgical care. The volume/outcome relationship has been well studied, but the identification of those patients who continue to go to low-volume centers and the reasons for their lack of access to higher-volume centers is poorly studied.
Our previous systematic review highlighted that studies rarely incorporate race and ethnicity when comparing high-, medium-, and low-volume hospitals. 8 Further, the few studies that have considered these factors suggest that PD outcomes may vary significantly based on race and ethnicity. A key factor often omitted from these studies is the neighborhood socioeconomic status, which is even less reported in PD outcomes studies. With the growing recognition of the importance of social determinants of health, the Distressed Communities Index (DCI) has been increasingly incorporated into outcomes research as a metric for socioeconomic well-being. The DCI highlights economic disparities across U.S. communities by categorizing areas into 5 tiers of well-being: prosperous, comfortable, mid-tier, at risk, and distressed. 9 It utilizes 7 key indicators—education level, employment, poverty rate, housing vacancy, income ratio, and changes in jobs and businesses—to provide insights into economic conditions and disparities within and between regions. Hunter et al reported that severely distressed communities exhibited higher rates of comorbidities, resource utilization, postoperative complications, and mortality. 10 In a study involving cardiac patients, those in the highest DCI quartile had 1.6 times higher odds of mortality compared to those in the lowest quartile. 11 Other studies across various surgical fields have similarly found that the DCI significantly impacts surgical outcomes.10,12
No study to date has specifically examined the impact of the Distressed Communities Index (DCI) on PD surgical outcomes, and the interaction between DCI, hospital volume, and outcomes remains unknown. It is plausible that the distribution of distressed communities varies across hospitals and may influence PD outcomes. For instance, Sutton et al reported disparities in the referral and treatment of pancreatic cancer patients based on socioeconomic, demographic, and geographic differences. 13 Additionally, 1 component of the DCI, estimated income, was found to be associated with higher odds of receiving treatment at high-volume hospitals. 13 Given the critical role hospital volume plays in PD-related outcomes, it is essential to investigate how distressed communities are demographically distributed across hospital volumes and how their surgical outcomes differ from those of the general population. In this study, we utilized a statewide hospital discharge database to examine the relationship between PD surgery volume, community socioeconomic conditions, and outcomes.
Methods
Data Source
We utilized the hospital discharge data spanning from 2017 to 2021, provided by the Pennsylvania Health Care Cost Containment Council (PHC4). This comprehensive database includes information on surgical procedures performed in Pennsylvania hospitals, encompassing patient demographics, locations, diagnostic details, types of admission, discharge statuses, lengths of hospital stays, and characteristics of the hospitals. Our study was granted exemption status from Institutional Review Board approval as it is based on de-identified, publicly accessible data.
Study Cohort
We extracted all pancreaticoduodenectomy cases based on the International Classification of Diseases, 10th Revision (ICD10) procedure codes (0FBG0ZZ and 0DB90ZZ) within PHC4’s hospital discharge database from 2017 to 2021.
Variables of Interest
The primary outcomes of interest include in-hospital mortality rate, 30-day readmission, and non-routine discharge following a pancreaticoduodenectomy procedure.
We included the following patient demographic and socioeconomic characteristics, clinical characteristics, and hospital characteristics: age groups (<45 years, 45-64 years, 65-74 years, and 75 years or older), race (White, Black, and Other), payers’ categories (commercial, Medicare, and others), hospital locality (rural, small town, and urban/suburban), year of diagnosis, distance (calculated as distance between patients’ residential address from hospitals using zip code), and patient neighborhood Distressed Communities Index (DCI) score 9 as covariates.
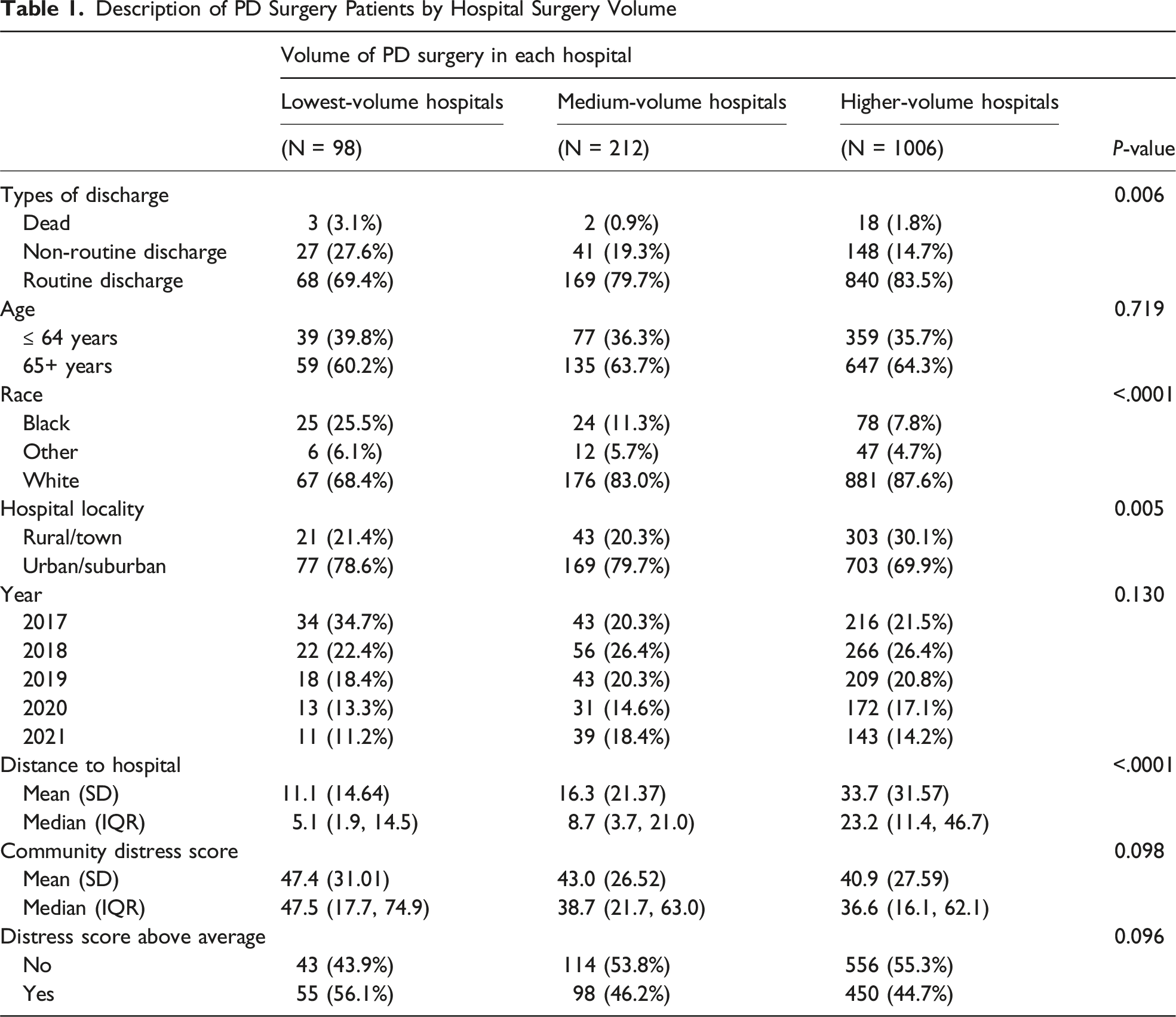
We categorized hospitals into 3 groups: lowest- (≤25 cases), medium- (26-50 cases), and higher-volume hospitals (>50 cases) according to the number of cases performed over the 5 years of the study period. A variety of volume ranges are described in the literature. There was no standardized threshold to distinguish high- and low-volume hospitals, as various studies employed different criteria. These thresholds were often categorized into levels such as very low, low, medium, medium-high, high, and very high. For instance, Birkmayer et al and Kasumova et al defined very low-volume hospitals as those performed fewer than 1 pancreaticoduodenectomy (PD) case and 7 cases per year, respectively.14-16 Similarly, definitions for low-volume hospitals varied: Conroy et al used 2-4.99 cases and Geus et al used 11 cases.17,18 Definitions for medium-, high-, and very high-volume hospitals also differed across studies. For example, Conroy et al classified high-volume hospitals as those performing more than 5 PD cases annually, while Kasumova et al set the threshold at 80 or more PD cases per year.16,17 The higher-volume hospitals in PA might be considered only medium volume in other locations; however, they represent the highest volume centers in the state. We therefore selected the categories of “lowest, medium, and higher” to label the hospital groups. Most patients (over 60%) were aged 65 years and older. Black patients represented a smaller proportion at higher-volume hospitals (7.8%) compared to medium-volume (11.3%) and lowest-volume hospitals (25.5%). The mean Distressed Communities Index score was higher in lowest-volume hospitals (47.4) compared to medium-volume (43.0) and higher-volume hospitals (40.9). Notably, 56.1% of patients treated at lowest-volume hospitals resided in communities with an above-average distress score, compared to 46.2% in medium-volume hospitals and 44.7% in high-volume hospitals.
Statistical Analysis
We provided descriptive statistics including frequency, mean, standard deviation, median, and interquartile range for the study cohort. We stratified the sample based on the hospital volume where the procedures were performed, categorized as lowest, medium, or higher. To compare demographic, socioeconomic, clinical, and hospital characteristics across these groups, chi-squared tests were used for categorical variables and Kruskal-Wallis tests were used for continuous variables.
Multivariable logistic regression analyses were employed to examine the association between hospital volume and surgical outcomes, considering patient demographics, Distressed Communities Index score, clinical factors, and other hospital characteristics. For clarity and brevity, we define distressed patients as those residing in communities with higher distress scores (ie, DCI above average). We assessed outcomes including in-hospital mortality, readmission, and non-routine discharge in the whole sample and in a subgroup of distressed patients, reporting adjusted odds ratios (AORs), 95% confidence intervals (CIs), and P-values. Statistical significance was set at a two-sided P-value of less than 0.05. All statistical analyses were conducted using SAS version 9.4 (SAS Institute Inc, Cary, NC, USA).
Results
Description of PD Surgery Patients by Hospital Surgery Volume
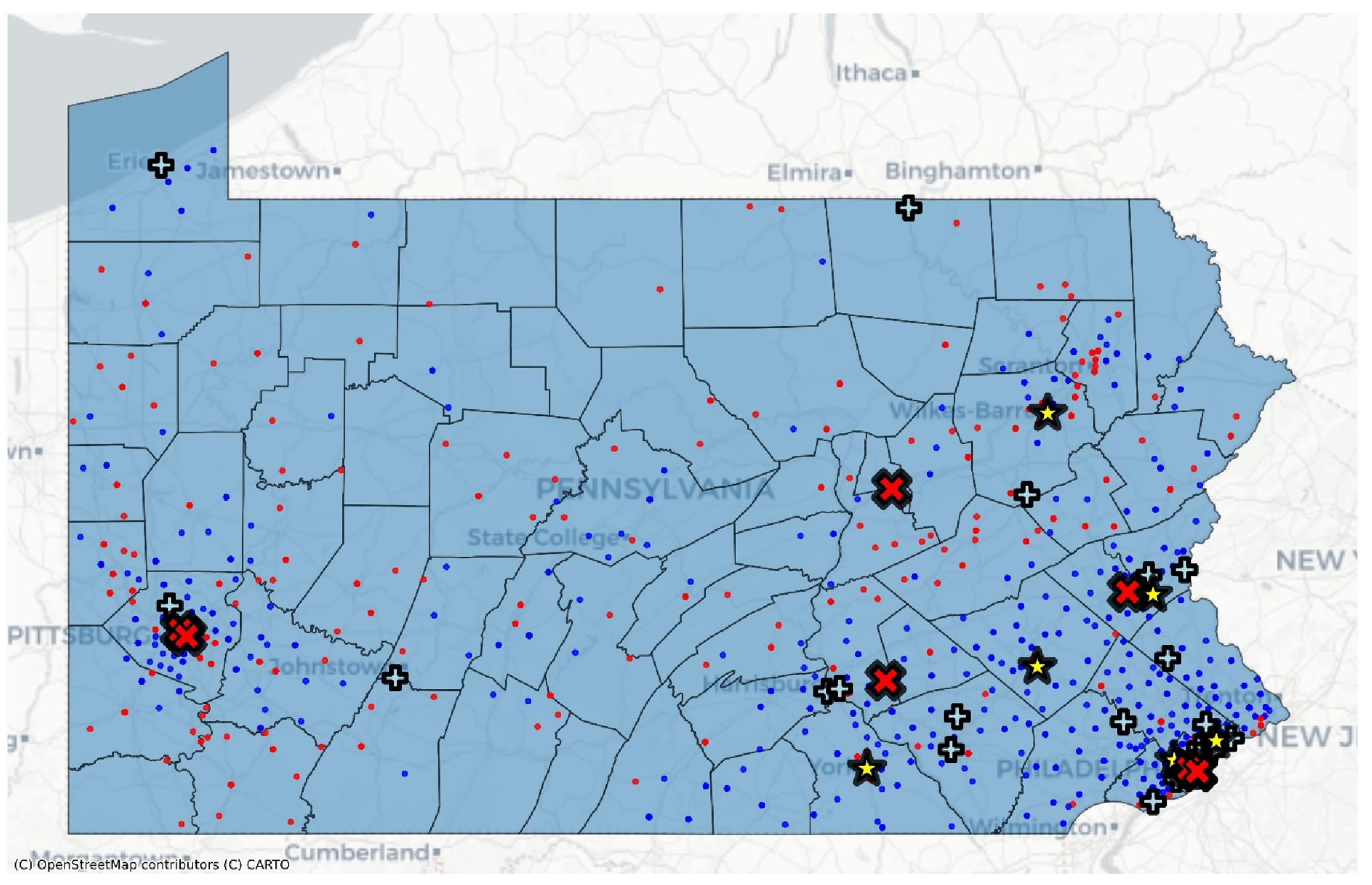
Geographic Distribution of Hospital Volume Categories and Distressed Zip Codes Across Pennsylvania for Pancreaticoduodenectomy. Blue Dots Represent Not-distressed Zip Codes; Red Dots Represent Distressed Zip Codes. Light Blue “+” Symbols Represent Lowest-Volume Hospitals; Yellow Star Symbols Represent Medium-Volume Hospitals; Red “×” Symbols Represent Higher-Volume Hospitals. County Polygons Are Shaded Light Blue
Results of Multivariate Logistic Regression for Mortality, Readmission, and Non-routine Discharge in the Whole Sample
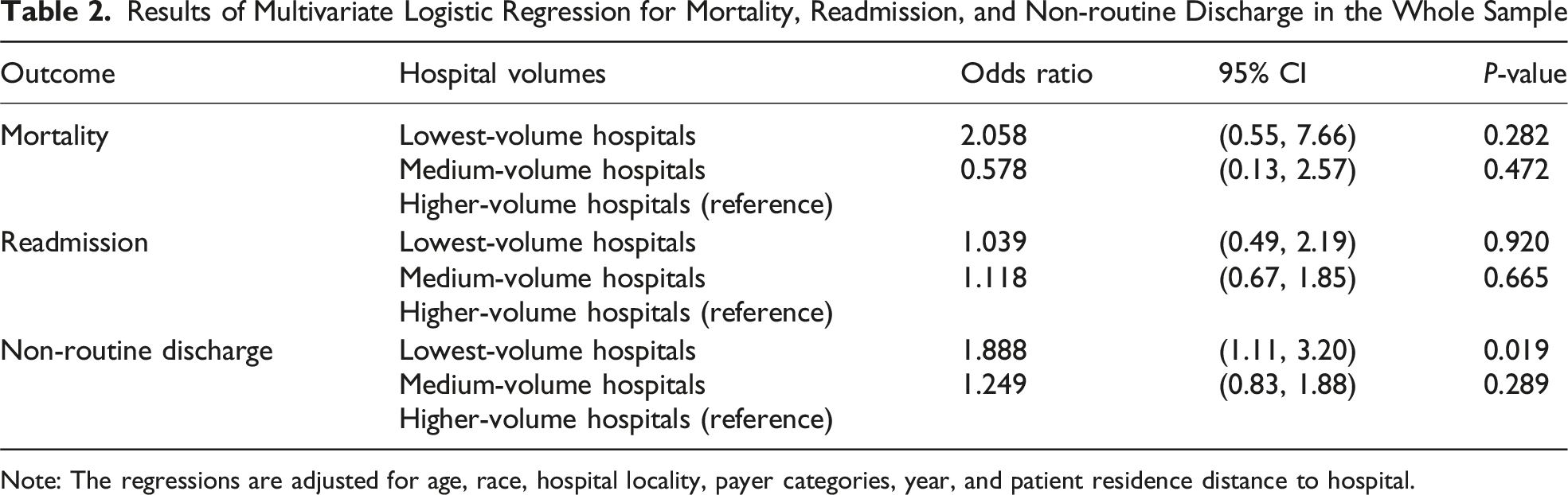
Note: The regressions are adjusted for age, race, hospital locality, payer categories, year, and patient residence distance to hospital.
Results of Multivariable Logistic Regression for Mortality, Readmission, Non-routine Discharge in Patients Living in Communities With Above Average Distress Scores
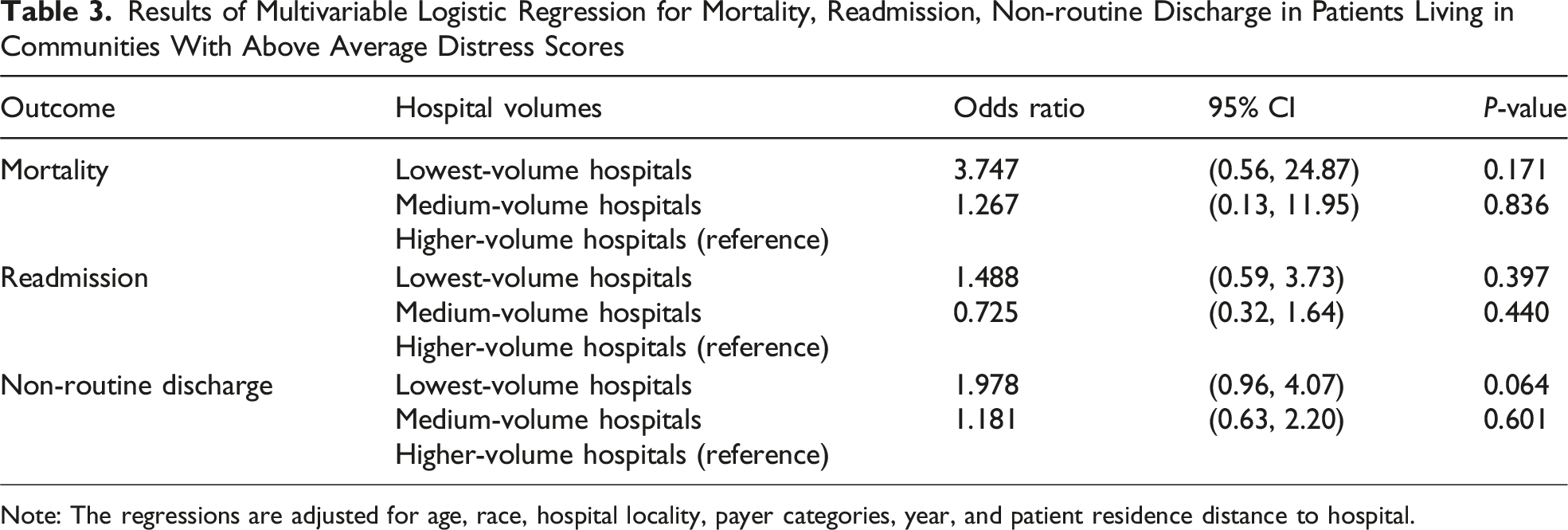
Note: The regressions are adjusted for age, race, hospital locality, payer categories, year, and patient residence distance to hospital.
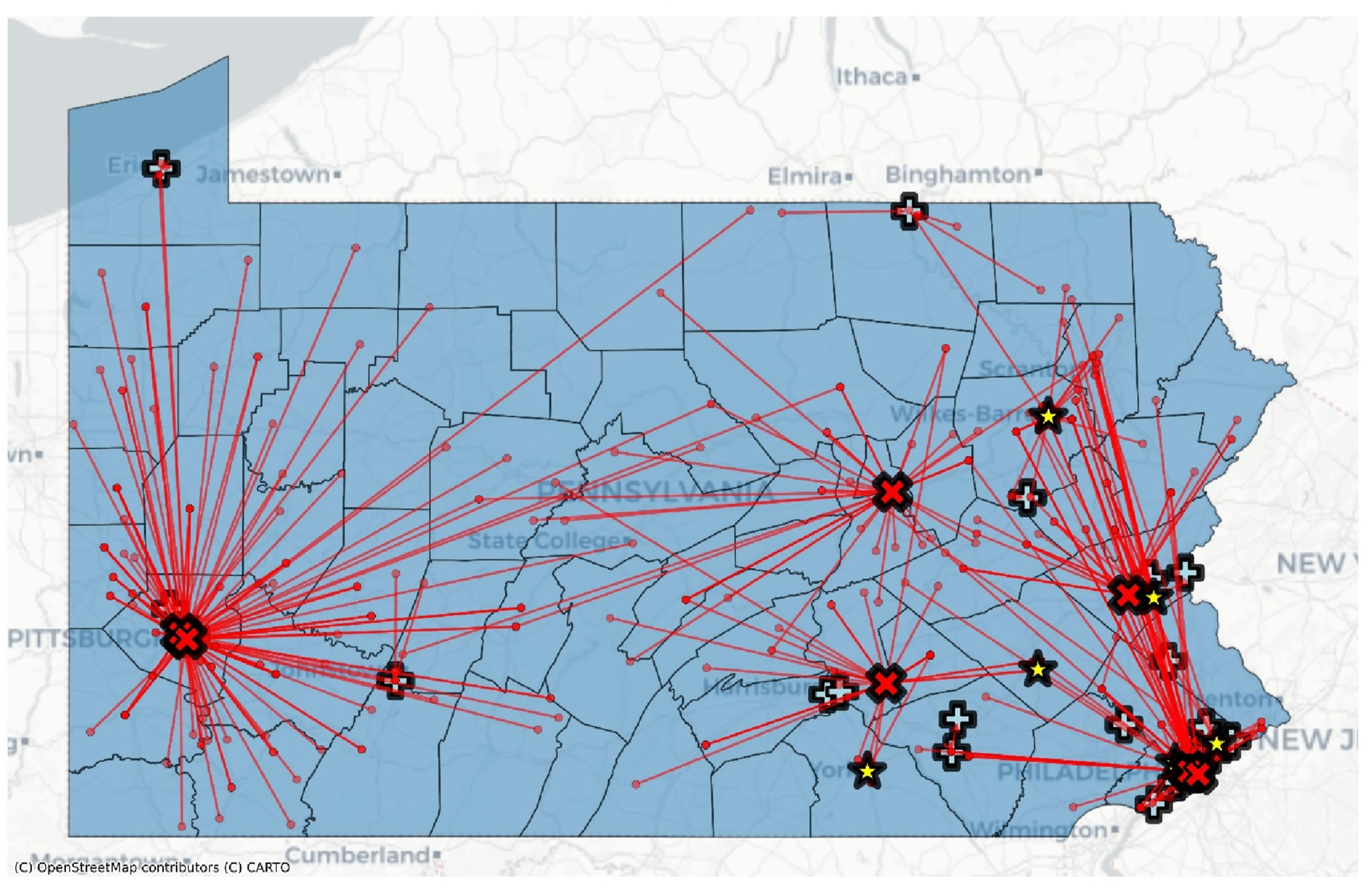
Distressed Residential Zip Codes and the Hospitals That Performed Pancreaticoduodenectomy Across Pennsylvania. Red Dots Mark Distressed ZIP Codes; Solid Red Arrows Illustrate Travel Patterns From Distressed ZIP Code to the Hospital Where Surgery Was Performed. Light-Blue “+” Symbols Represent Lowest-Volume Hospitals, Yellow Star Symbols Represent Medium-Volume Hospitals, and Red “×” Symbols Represent Higher-Volume Hospitals. County Polygons Are Shaded Light Blue
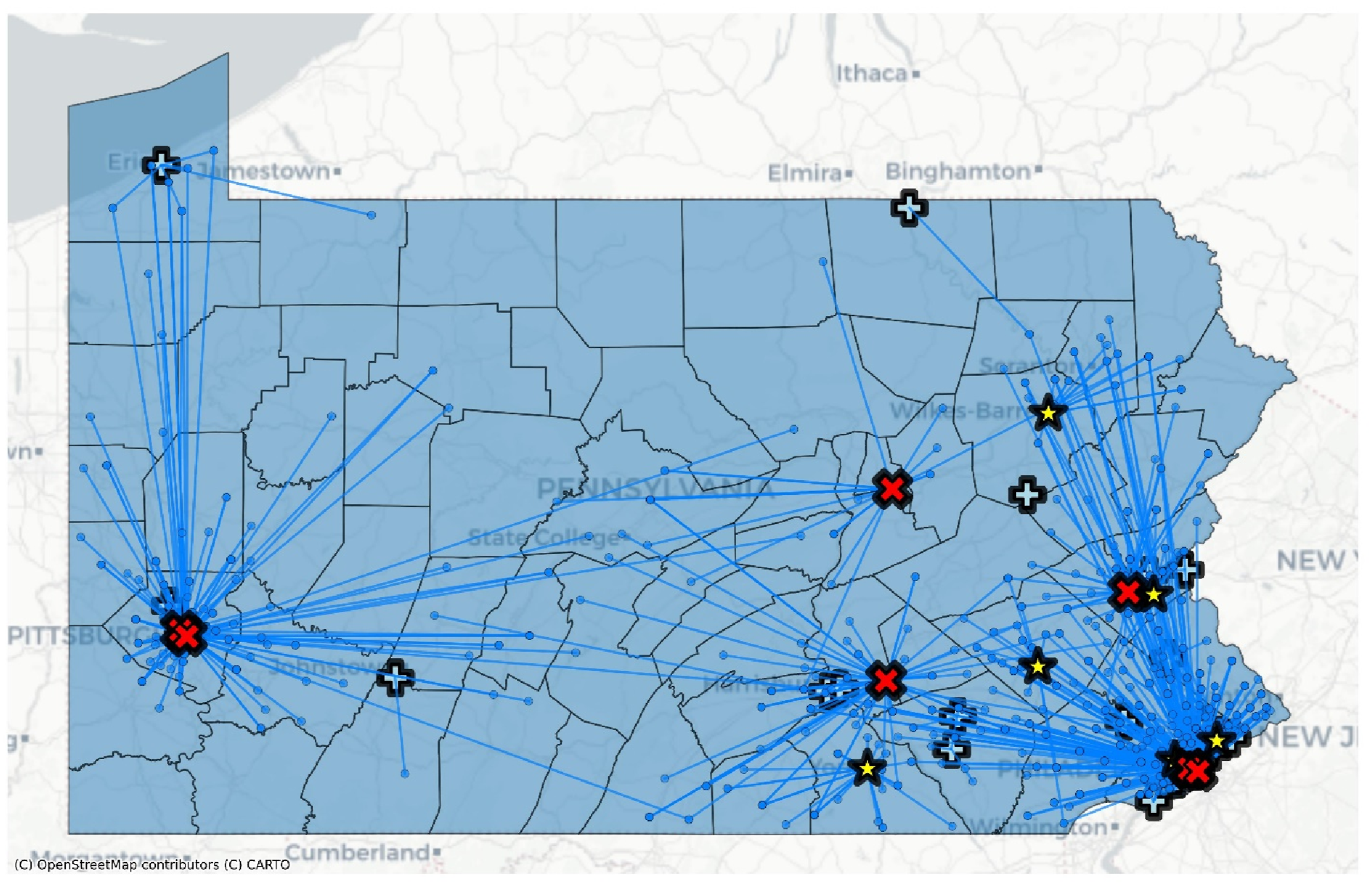
Not-Distressed Residential Zip Codes and the Hospitals That Performed Pancreaticoduodenectomy Across Pennsylvania. Blue Dots Mark Not-Distressed ZIP Codes; Solid Blue Arrows Illustrate Travel Patterns From Not-distressed ZIP Code to the Hospital Where Surgery Was Performed. Light-Blue “+” Symbols Represent Lowest-Volume Hospitals, Yellow Star Symbols Represent Medium-Volume Hospitals, and Red “ × ” Symbols Represent Higher-Volume Hospitals. County Polygons Are Shaded Light Blue
Discussion
In this study, we evaluated the relationship between hospital volume and clinical outcomes, including in-hospital mortality, readmission, and non-routine discharge, with a particular focus on the influence of patients’ neighborhood socioeconomic status. Our findings revealed a significant association between lowest-hospital volume and higher rates of non-routine discharge, aligning with existing literature that suggests worse patient outcomes in lowest-volume hospitals17,19,20 and attributing the higher success rates in higher-volume hospitals to greater hospital experience and surgeon expertise.3,6,21,22 Although lowest-volume hospitals in our study exhibited higher mortality rates, the regression results were not statistically significant, potentially due to the low incidence of mortality. Of the 1316 surgeries analyzed, only 23 deaths were recorded. When comparing medium- and higher-volume hospitals, we observed no statistically significant differences in any of the surgical outcomes examined, including mortality, readmission, and non-routine discharge. These findings reinforce that the difference in surgical outcomes between medium- and higher-volume hospitals is substantially smaller than that between lowest- and higher-volume hospitals.
Patients in lowest-volume hospitals had higher mean community distress scores, and a greater percentage of distressed patients go to lowest-volume hospitals, compared to those living in less distressed communities. Among the subgroup of patients living in communities with higher distress scores, the odds of mortality, readmission, and non-routine discharge were higher for lowest-volume hospitals compared to higher-volume hospitals although not statistically significant. The higher concentration of distressed patients in lowest-volume hospitals may reflect broader systemic issues within the health care system, such as disparities in socioeconomic factors, health care accessibility, and referral patterns. Distress scores are derived from socioeconomic indicators, including education, employment, poverty rate, housing, income, and changes in jobs and businesses. Systematic differences in these factors across hospital volumes may contribute to the observed disparities in clinical outcomes. For example, Sutton et al (2022) found that higher income was associated with increased odds of receiving treatment at high-volume hospitals.
A higher percentage of Black patients underwent PD surgery in lowest-volume hospitals (Table 1), while a greater proportion of White patients underwent PD surgery in higher-volume hospitals. These findings are consistent with prior literature on racial disparities in PD surgery17,23-25 and suggest that minority patients from distressed communities are more likely to receive PD surgery at lowest-volume hospitals, potentially leading to poorer surgical outcomes. Ironically, many of these patients are geographically close to medium- and higher-volume centers, as seen in Figure 4. This geographic variation suggests the presence of 2 distinct subpopulations within distressed patient groups. Rural White patients in central Pennsylvania often reside far from hospitals and tend to travel to medium- or high-volume centers, whereas urban Black patients frequently utilize the lowest-volume centers despite living in close proximity to medium- and high-volume facilities. These findings are consistent with prior research indicating that although Black patients often reside nearer to higher-quality hospitals than White patients, they remain 25%-58% more likely to undergo surgery at lower-quality facilities.26-29 This paradox deserves further exploration as travel distance may not be the actual barrier to accessing a higher-volume center. Health insurance, referral patterns, specialty resources, health literacy, or other factors may be responsible for the hospital chosen.28,30-32 Geographic Distribution of Hospital Volume Categories and Residential Zip Codes for Whites and African Americans. White Dots Represent Whites Residential Zip Codes; Yellow Dots Represent African Americans Residential Zip Codes. Light-Blue “+” Symbols Represent Lowest-Volume Hospitals, Yellow Star Symbols Represent Medium-Volume Hospitals, and Red “ × ” Symbols Represent Higher-Volume Hospitals. County Polygons Are Shaded Light Blue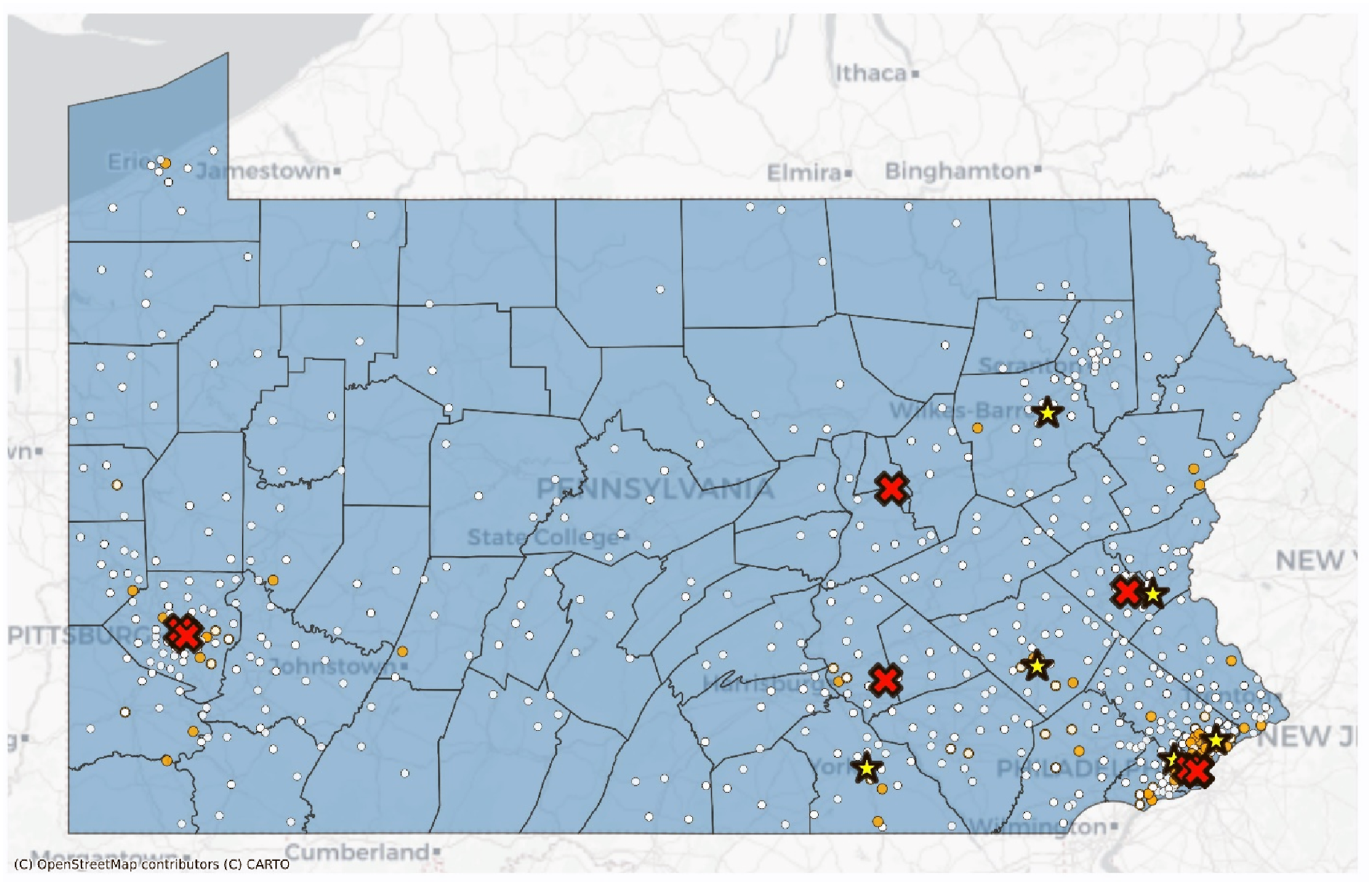
This finding may have important implications for improving patient outcomes. Given that the median distances to lowest-, medium-, and higher-volume hospitals are 5.1, 8.7, and 23.2 miles, respectively, referrals to medium-volume hospitals might be a reasonable option, particularly for distressed patients. Although higher-volume hospitals generally have the highest success rates, the significant distance (23.2 miles, with an interquartile range of 11.4 to 46.7 miles) may pose an access barrier, especially for patients in distressed communities in Pennsylvania. Medium-volume hospitals could serve as a practical compromise, offering closer proximity while achieving outcomes comparable to those of higher-volume hospitals. As described above, further exploration of factors involved in hospital selection should be undertaken. Although the median travel distance between the lowest- and medium-volume hospitals was modest (5.1 vs 8.7 miles), patients treated at high-volume centers traveled substantially farther (median 23.2 miles). This overall pattern was statistically significant (P < .0001), underscoring the potential geographic access barriers associated with receiving care at high-volume hospitals, though travel distance may also serve as a surrogate for broader social and economic challenges that merit further exploration.
This study has several limitations. The data set represents only hospitals in Pennsylvania, so the results may not be generalizable to other regions in the United States. Although we controlled for various patient demographics, insurance status, socioeconomic factors, and hospital characteristics, there may still be other unmeasured variables, such as detailed clinical factors, surgeon characteristics, or health plan referral requirements that could influence hospital choice and surgical outcomes. Future studies should further explore the complex relationship between hospital volume, surgical outcomes, and socioeconomic factors, incorporating a broader range of patient and physician characteristics in nationally representative data sets. Some patients are not near any health center at all and must travel a significant distance no matter where they choose to go. Another limitation of our analysis is the use of the DCI, a neighborhood-level metric derived from zip code-level data. While DCI captures important area-level socioeconomic indicators, it does not directly measure individual patients’ income, wealth, or financial well-being. As such, patients living in the same zip code may experience markedly different socioeconomic circumstances, and the DCI may obscure within-area heterogeneity. This ecological limitation is important to consider when interpreting associations between community distress and surgical outcomes. The absence of surgeon-level procedure data precludes us from analyzing the influence of individual provider volume. Prior research has shown that surgeon experience is a strong determinant of outcomes for high-risk procedures such as the Whipple.33-35 At the same time, hospital volume may capture other critical elements of care, such as nursing expertise, intensivist support, and perioperative infrastructure, which also contribute meaningfully to patient outcomes.36-39 Future studies incorporating both surgeon and hospital volume metrics would provide a more comprehensive understanding of the factors driving surgical quality. Additionally, the rarity of mortality events in our sample made it difficult to detect statistically significant differences. Our findings reflect observed treatment patterns rather than causal determinants of access. Future studies incorporating patient or provider surveys, qualitative interviews, or linked data sets could help elucidate the multilevel factors, such as insurance constraints, referral practices, health literacy, and local availability of specialty care that influence where patients undergo complex surgery. Such studies will be critical if we are to address disparities in health care and surgical outcomes.
Conclusion
Our study highlights the racial and socioeconomic differences among patients having PD at lowest-, medium-, and higher-volume centers in Pennsylvania. It is well established that higher-volume centers have better outcomes, but as complex surgical care becomes regionalized it is important to understand who loses access to care and what the barriers are for patients. Our study should be a starting point for further work to address these disparities.
Footnotes
Acknowledgment
The Pennsylvania Health Care Cost Containment Council (PHC4) is an independent state agency responsible for addressing the problem of escalating health costs, ensuring the quality of health care, and increasing access to health care for all citizens regardless of ability to pay. PHC4 has provided data to this entity in an effort to further PHC4’s mission of educating the public and containing health care costs in Pennsylvania. PHC4, its agents, and staff have made no representation, guarantee, or warranty, express or implied, that the data—financial, patient, payor, and physician specific information—provided to this entity are error-free or that the use of the data will avoid differences of opinion or interpretation. This analysis was not prepared by PHC4. This analysis was done by the authors. PHC4, its agents, and staff bear no responsibility or liability for the results of the analysis, which are solely the opinion of this entity.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Author Disclosures
The authors have no relevant financial support, conflicts of interest, or commercial interest to disclose.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
