Abstract
Background
Pancreaticoduodenectomy (PD) is associated with better outcomes in high-volume hospitals. However, it is unknown whether and to what extent the improved performance of high-volume hospitals may be associated with racial and socioeconomic factors, which have been shown to impact operative and postoperative outcomes in major surgeries. This review aims to identify the differences in racial and socioeconomic characteristics of patients who underwent PD surgery in high- and low-volume hospitals.
Methods
PubMed, Cochrane, and Web of Science were systematically searched between May 1, 2023 and May 7, 2023 without any time restriction on publication date. Studies that were conducted in the United States and had a direct comparison between high- and low-volume hospitals were included.
Results
A total of 30 observational studies were included. When racial proportions were compared by hospital volume, thirteen studies reported that compared to high-volume hospitals, a higher percentage of racial minorities underwent PD in low-volume hospitals. Disparities in traveling distance, education levels, and median income at baseline between high- and low-volume hospitals were reported by four, three, and two studies, respectively.
Conclusion
A racial difference at baseline between high- and low-volume hospitals was observed. Socioeconomic factors were less frequently included in existing literature. Future studies are needed to understand the socioeconomic differences between patients receiving PD surgery in high- and low-volume hospitals.
Introduction
The Whipple procedure, or pancreaticoduodenectomy (PD), is a major surgical operation to treat benign and malignant neoplasms originating from the pancreas, peri-ampullary carcinomas, and cholangiocarcinoma. Because of the complexity of the procedure and associated potential complications, PD is often recommended to be performed in high-volume hospitals. 1 Research has found that high-volume hospitals have shorter average hospital stays, lower readmission rates, and reduced mortality rates.2–5 Factors contributing to this higher success rate may include hospital experience and surgeon expertise. 6 However, it is not fully understood how much of the better performance can be attributed to patient characteristics or if there are fundamental differences between patients treated at high-volume and low-volume hospitals.
The results of major surgical outcomes can be heavily influenced by patients’ socioeconomic characteristics. 7 Studies that investigated hospital volume-based disparities in various types of surgeries indicated that racial and socioeconomic characteristics are significant factors in such disparities.8,9 For instance, in a study with more than 1 million inpatient sample, 10 Bennett et al (2010) reported that operative mortality is strongly associated with patients' socioeconomic status. The study also reported a higher mortality rate among patients with the lowest socio-economic status. Another study by Liu et al 8 (2006) on multiple surgical operations including pancreatic cancer resections suggested that Blacks, Hispanics, and Asians are less likely to be treated at high-volume hospitals.
Socioeconomic factors such as income can have substantial influence on postoperative PD outcomes.7,11 A study by Jerath et al (2020) reported that among 13 types of major surgery patients including PD, the risk of postoperative complications and 30-day mortality was significantly higher among patients in the lowest income quartile. 11 Education is another major socioeconomic factor that can significantly affect outcomes in pancreatic surgery. 12 In a study that included pancreatic resection patients, the length of hospital stay was greater among patients with lower health literacy level. 12 Similarly, current research suggests the existence of a geographical disparity in the form of distance or rurality which may affect surgical outcomes. 13
Racial disparity is another key factor that can affect surgical access and outcomes. Khubchandani et al 14 (2018) reported a lack of emergency general surgery hospitals in counties with a larger proportion of African Americans. Whites also have been shown to have higher rates of surgery per 100,000 people compared to Black or Hispanic population suggesting disparity in access. 15
As discussed above, existing evidence suggests that there is a substantive impact of racial and socioeconomic factors on operative and postoperative surgical outcomes. Therefore, it is plausible that better surgical outcomes in high-volume hospitals for PD are also potentially driven by patients’ characteristics such as race and socioeconomic profile. To date, many studies have compared operative and postoperative PD-related outcomes in high- and low-volume hospitals; however, few have explored the extent to which the disparities in surgical outcomes between high- and low-volume hospitals can be attributed to differences in patient populations in terms of race and socioeconomic status. Therefore, by using the existing evidence, this study aims to systematically review racial and socioeconomic characteristics among patients who underwent PD in high- and low-volume patients to ascertain any differences.
Methods
We followed the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines for the systematic search. 16 Using the PRISMA guideline, we searched three electronic databases: PubMed, Cochrane, and Web of Science. We used various combinations of the three basic search terms (pancreaticoduodenectomy, high-volume hospitals, and low-volume hospitals), details of which are provided in the supplementary file. The systematic search was conducted between May 1, 2023 and May 7, 2023, and no time restriction was place on publication date of the articles.
Study eligibility
We included studies that examined patient outcomes from PD. Studies that included both high- and low-volume hospitals were included. We excluded studies that were not conducted in English, and only studies that were conducted in the United States were included. We also excluded studies that included other surgical procedures such as distal pancreatectomy and total pancreatectomy, etc. along with PD. The exclusion criteria also extended to the studies that did not have a direct comparison between high- and low-volume hospitals. Further, studies that mainly examined the impact of surgeon volume were excluded. The inclusion criteria were not limited to the type of studies (observational or randomized control trials).
Study selection
Two authors independently screened the titles and abstracts to match the eligibility criteria. Full text of the studies that matched eligibility criteria was then evaluated. The detailed study selection process is provided in the flow chart (Figure 1). Overall, the search in three databases produced 1301 studies. After applying the inclusion and exclusion criteria, we finally included 30 studies. Study selection flow chart.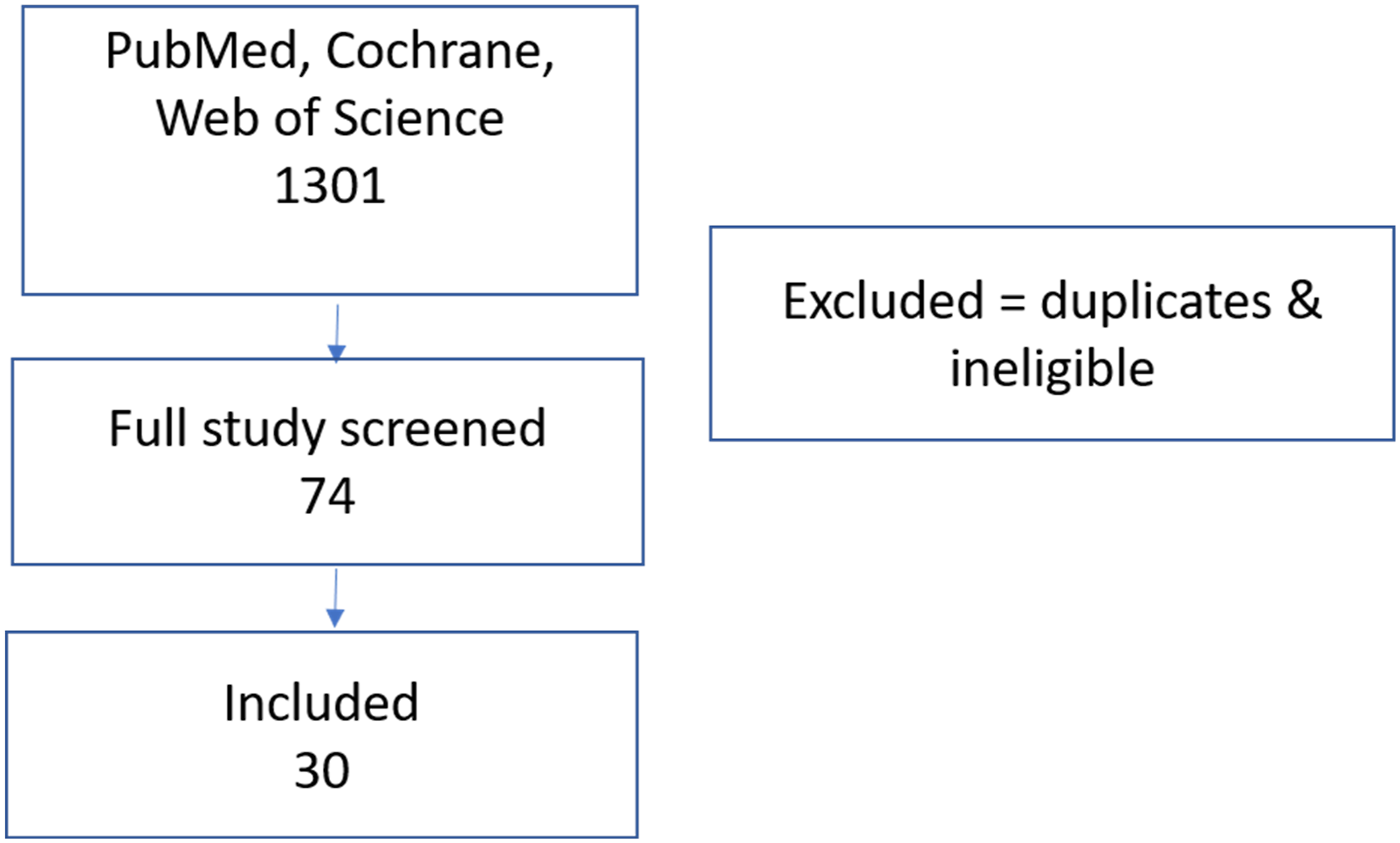
Results
A Comparison Between High- and Low-Volume Hospitals.
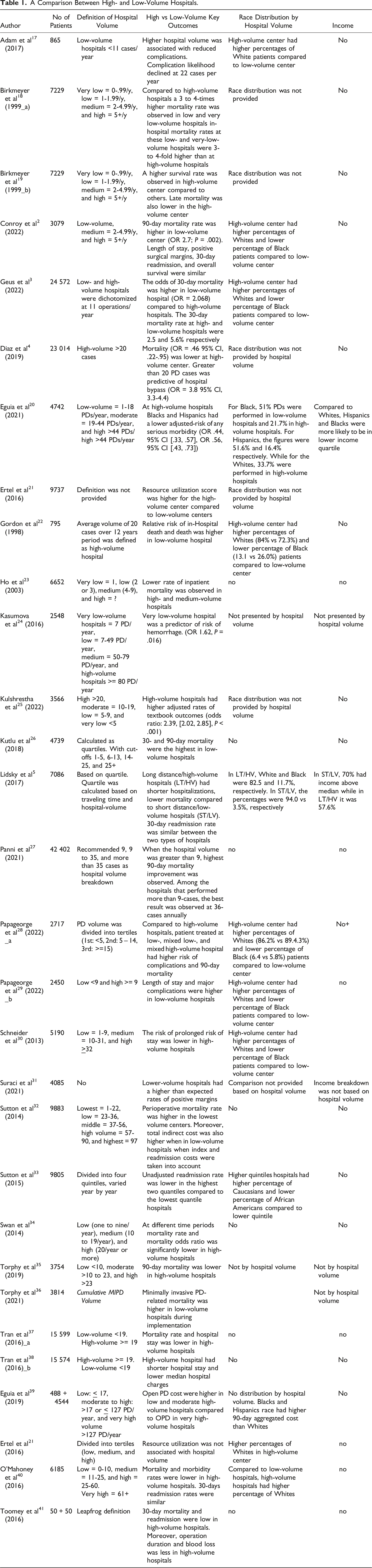
Definition of hospital volume
There was no universal cut-off used to define high- and low-volume hospitals. The thresholds were defined using various cut-offs, including categories such as very low, low, medium, medium-high, high, and very high. For example, Birkmeyer et al (1999 a,b) and Kasumova et al (2016) defined very low-volume as less than 1 PD case and 7 cases/year, respectively.18,19,24 Similarly, the definition of low-volume varied. Birkmeyer et al (1999_a) used 1-1.99 cases, Conroy et al (2022) used 2-4.99 cases, Geus et al (2022) used 11 cases, and so on.2,3,18 Similarly, various cut-off values were used to define medium, high, and very high volume. Conroy et al defined high-volume hospitals as those with greater than 5 PD cases per year while Kasumova et al (2016) defined high-volume hospitals as those with 80 or more PD cases per year.2,24 Some studies used quantiles and tertiles for defining high- and low-volume hospitals.21,28,33 One study used cumulative volume over the years for defining hospital volume, 36 while another study combined traveling distance along with hospital volume for the definition. 5
Race and ethnicity
Only one study was found that primarily focused on race as the key variable. 20 Eguia et al (2021) reported that at high-volume hospitals, Blacks and Hispanics had a lower adjusted risk of any serious morbidity (OR .44, 95% CI [.33, .57], OR .56, 95% CI [.43, .73]) 20 than non-Hispanic Whites at high-volume hospitals. Thirteen studies reported that a higher percentage of Whites underwent PD surgery in high-volume hospitals while a lower percentage of Blacks and Hispanics had their PD performed in high-volume hospitals.2,3,5,17,20–22,28,29,33,39,40 Other studies did not include race in the analysis.
Socioeconomic characteristics
Income
Baseline differences in income level of patients at high- vs low-volume hospitals were only provided in two studies.5,20 The findings on baseline income levels diverged in those two studies. Eguia et al (2021) reported that Hispanics and Blacks were more likely to be in the lower income quartile compared to Whites. 20 In contrast, Lidsky et al (2017) reported that patients in long travel/high-volume hospitals had a lower median income compared to the patients in short travel/low-volume hospitals. 5
Education
Education level was rarely included as one of the key characteristics in the studies. Only three studies reported education levels.5,25,35 Kulshrestha et al (2022) reported that lower educational attainment was associated with worse standard surgical outcomes such as 30-day readmission, 90-day mortality, prolonged hospitalizations, etc. However, they did not provide a breakdown of educational levels between high- and low-volume hospitals. Lidsky et al (2017) reported that the proportion of patients with education above median was similar between short travel/low-volume (58.8%) hospitals and long-distance/high-volume hospitals (58.0%). 5 Torphy et al 35 (2019) adjusted for education in the propensity scoring but did not provide a breakdown by hospital volume.
Transportation
Birkmeyer et al 19 (1999_b) reported that low-volume hospitals had substantially lower percentages of patients from their hospital referral regions compared to high-volume hospitals (11% vs 60%). The authors also reported that the in-hospital mortality rate of local patients in low-volume hospitals was higher compared to those from a distant location, whereas in the high-volume hospitals, the mortality rate of local patients was slightly better. Geus et al 3 (2022) reported that the median travel distance of the patients in high-volume hospitals was much higher (27.9% vs 9.8%) compared to low-volume hospitals. Diaz et al (2019) reported that patients are more likely to bypass the nearest hospital (68.8%) and travel to a high-volume hospital. 4 The authors also reported that PDs at high-volume centers were associated with lower mortality. Lidsky et al (2017) incorporated traveling distance in their categorization of high- and low-volume hospitals. 5 The median distance for short travel/low-volume was 3.2 miles while for long travel/high-volume hospitals the average distance was 97.3 miles. The authors reported that traveling to a high-volume hospital was associated with better 30-day and 90-day mortality.
Two additional studies included travel distance in their analysis. Torphy et al 35 (2019) adjusted the propensity score for distance from the hospitals but did not provide the distribution by hospital volume. The distance was also considered as one of the confounders by Kutlu et al 26 (2018), but how the distance was distributed between high- and low-volume hospitals was unavailable.
None of the 30 included studies examined other socioeconomic characteristics such as marital status, neighborhood quality, and food security.
Key outcome
Classification of Studies Based on Key Outcomes.

Discussion
In this study, we systematically reviewed the existing literature on PDs performed in high- and low-volume hospitals. We particularly focused on disparities in patient characteristics in these two types of hospitals.
In this review, we found 13 studies that reported a racial difference at baseline between high-volume and low-volume hospitals.2,3,5,17,20–22,28,29,33,39,40 It was observed that most high-volume centers had higher percentages of non-Hispanic White PD patients than low-volume centers. The high-volume hospitals had lower percentages of African American and Hispanic PD patients compared to low-volume hospitals. For example, Eguia et al (2021) reported that Black and Hispanics were less likely than Whites to undergo PD in high-volume centers. 20 The hospital volume-related racial disparity in PD is consistent with prior literature on surgical procedures in general.14,15 Previous studies indicated that Hispanics and non-Hispanic Blacks are less likely to be treated at high-volume centers.8,42 Dimick et al (2013) reported that despite a comparatively higher percentage of Black patients living near high-quality hospitals (determined by composite measures that include hospital volume along with other measures), they are more likely than White patients to undergo surgery in low-quality hospitals. 42 In a systematic review, Haider et al 43 (2013) suggested that hospital volume may play a role in minority-based outcome disparity. A potential solution to such disparity could be changes in policy which would increase the access of ethnic minorities to high-volume hospitals. Eguia et al reported that minorities treated in high-volume hospitals had better outcomes than minorities treated in low-volume hospitals, 20 suggesting that such policies would improve outcomes for minorities. However, none of the studies examined how racial differences in high- and low-volume hospitals affect operative and postoperative outcomes in high- and low-volume hospitals.
We observed that social determinants of health such as income and education were less frequently incorporated in PD research. In this review, we did not find any study that evaluated the impact of income levels on hospital volume-based outcomes. We found only two studies that reported income in the baseline characteristics.5,20 Income levels can have a substantial impact on PD outcomes as income can affect access to health care, cancer screening, and overall health status.44,45 Lower income is often associated with delayed diagnosis and treatment. 46 Although not specific to PD, previous studies have reported that lower income levels are associated with higher length of stay and higher mortality rates. 11 Therefore, it would be interesting to see how income levels impact access to PD surgery in high- and low-volume hospitals as well as how it impacts postoperative complications. The only study reporting income and hospital volume found that short travel/lower-volume hospitals had a higher percentage of PD patients with income levels above the median. 5 The reason for higher percentages of above median income patients in low-volume hospitals could be due to the fact that cost of pancreatic surgery in low-volume hospitals is generally higher than the high-volume hospitals.47,48
Education level is another key social determinant that was very rarely included in PD research. Education level can significantly impact health literacy and understanding, medical information processing, and informed decision-making.49,50 A study by Kugelman et al 51 (2017) reported that patients with lower educational attainments are more likely to experience postoperative complications following a surgical procedure. We did not find any study that evaluated the impact of education level and hospital volume-based outcomes among PD patients. Examining the impact of education on mortality rate, readmission, and postoperative complications among PD patients in high- and low-volume hospitals is an important future research direction.
Traveling distance from the hospital is another factor that impacts patients’ decisions. Onega et al (2008) reported that certain population groups have difficulty accessing specialized cancer care, and travel time was higher for specialized cancer treatment facilities. 52 Although there were only two studies in this area, both indicated that high-volume hospitals had more patients from outside of the residential area while low-volume hospitals have more patients from the local area.4,19 Many patients may bypass low-volume hospitals for PDs in high-volume hospitals. 4 However, other than distance we did not find any studies that evaluated transportation barriers (eg reliable transportation) in PD surgery. It would be interesting to investigate whether and how the transportation barrier plays a role in patients' preference in choosing high- vs low-volume hospitals.
We also found that the impact of other social determinants such as marital status, neighborhood and built environment, and social and community context were vastly understudied when examining the impact of hospital volume on PD patient outcomes.
Most studies included in this review reported better clinical outcomes for PD patients operated in high-volume hospitals. In general, better outcomes in high-volume hospitals are attributed to several factors such as the experience and expertise of the surgical team, availability of multidisciplinary teams, necessary infrastructure and resources, comprehensive and specialized postoperative care, and development of standardized protocols for patient care. However, biological and social differences in patient characteristics can significantly influence PD-related outcomes in high- and low-volume hospitals. This review showed that some patient characteristics such as race and distance from the referral hospital are unequal in these two types of hospitals. It is plausible that other important social determinants such as income, educational level, food security, transportation barrier, and access to care could also be different between high- and low-volume hospitals. It was also observed that most of these parameters were largely absent in PD research in the United States. Therefore, future studies should emphasize including these parameters in the analysis.
This systematic review has some limitations. We did not review studies that included other surgical procedures along with PD. As the primary aim of this review was to evaluate racial and socioeconomic factors and there is a lack of quantifiable data in these categories, we did not perform a meta-analysis.
Nevertheless, this review provides comprehensive details of patient characteristic differences between high- and low-volume hospitals based on existing literature. This review highlights that racial distribution, income levels, and distance from referral hospitals are different at baseline between high- and low-volume hospitals. Moreover, in this review, we found that many socioeconomic factors are understudied and their role in the outcomes related to high- and low-volume hospitals is unknown. Future studies should focus more on the role of socioeconomic factors in PD-related operative and postoperative outcomes at high- and low-volume hospitals.
Supplemental Material
Supplemental Material - Racial and Socioeconomic Differences and Surgical Outcomes in Pancreaticoduodenectomy Patients: A Systematic Review of High- Versus Low-Volume Hospitals in the United States
Supplemental Material for Racial and Socioeconomic Differences and Surgical Outcomes in Pancreaticoduodenectomy Patients: A Systematic Review of High- Versus Low-Volume Hospitals in the United States by Mohammad Ikram, Chan Shen, and Colette R. Pameijer in The American Surgeon™.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
