Abstract
Giant condyloma acuminata (GCA), or Buschke-Löwenstein tumor, is a rare exophytic cauliflower-like growth in the anogenital region. The spectrum of treatment options is wide, ranging from the application of topical ointments to the performance of an abdominoperineal resection. Currently, wide local excision is the most common approach and may entail the creation of a protective loop ileostomy or implementation of flaps or grafts that facilitate closure. We describe a unique surgical approach for the management of circumferential GCA void of the use a protective loop ileostomy, flaps, or grafts. Our report highlights that the implementation of a radical, circumferential, wide excision resulting in “free-floating anus” and healing via secondary intention can ultimately lead to excellent functional and cosmetic results and therefore may be considered a minimally invasive surgical option for patients afflicted with a large, circumferential GCA.
Case Presentation
The patient was an otherwise healthy 30-year-old male with a history of tobacco and alcohol-use disorder who presented with a 7-month history of what he described as anal warts that caused daily bleeding and constant pain exacerbated by bowel movements or straining. He denied a history of same-sex intercourse or sexually transmitted diseases. His physical exam was remarkable for a circumferential fleshy anal condyloma with internal components spanning just distal to the dentate line and extending radially 5 centimeters (cm) beyond the anal verge with the anterior perineal portion of the lesion extending 2 cm into the scrotal base. The remainder of his exam was within normal limits. Following an informed discussion, the patient consented for a wide local excision of the mass with plans for closure via secondary intention.
Operative Technique
Following induction with general anesthesia, the patient was placed in the lithotomy position and an examination revealed stable findings from his initial clinic visit (Figure 1A). The procedure began by using a number 15 blade to excise a representative sample which on frozen section confirmed the presence of condyloma acuminata without evidence of carcinoma. Electrocautery was then used to demarcate a 1 cm circumferential excision border around the lesion. This incision was extended into the subcutaneous fatty plane and continued in a circumferential fashion, while taking great care to avoid violating the perianal musculature. The peripheral en bloc circumferential excision included a 4 × 2 cm portion of the posterior scrotal skin while the internal circumferential excision margin in the anal canal was proximal to all visible disease. The remaining “free-floating” anal mucosa within the anal canal was secured to the surrounding subcutaneous tissue and internal sphincter using interrupted 2-0 chromic sutures (Figure 1B). To facilitate drainage, a .5-inch Penrose drain was placed in the anal opening and secured to the skin with 2-0 silk sutures (Figure 1C). Figure 1D shows the excised specimen with the anal mucosa at its center. Notably, the perineal defect included a scrotal component with exposed dartos fascia just anterior to the perineal body. The scrotal skin was advanced over the exposed dartos fascia and secured to the perineal body using 3-0 braided absorbable and chromic sutures. The remainder of the wound was irrigated and after hemostasis was achieved, it was left open to close via secondary intention and wet-to-dry dressings. The patient was extubated in the operation room (OR) and transferred to the post-anesthesia care unit without incident and subsequently admitted for observation. Following evaluation by occupational and physical therapy and wound care teaching, the patient was discharged on postoperative day 2. Final pathology of the specimen revealed a condyloma acuminatum of the anus measuring 7.5 cm in its greatest dimension, without the evidence of high-grade dysplasia or carcinoma. All margins, including circumferential, internal, and peripheral external, were grossly and histologically free of dysplasia. (A) Image of preoperative perianal region; (B) perianal region following the excision of lesion with “free-floating” anal mucosa secured to internal anal sphincter; (C) placement of Penrose drain within anal canal; (D) excised specimen demonstrating circumferential GCA and gross negative margins.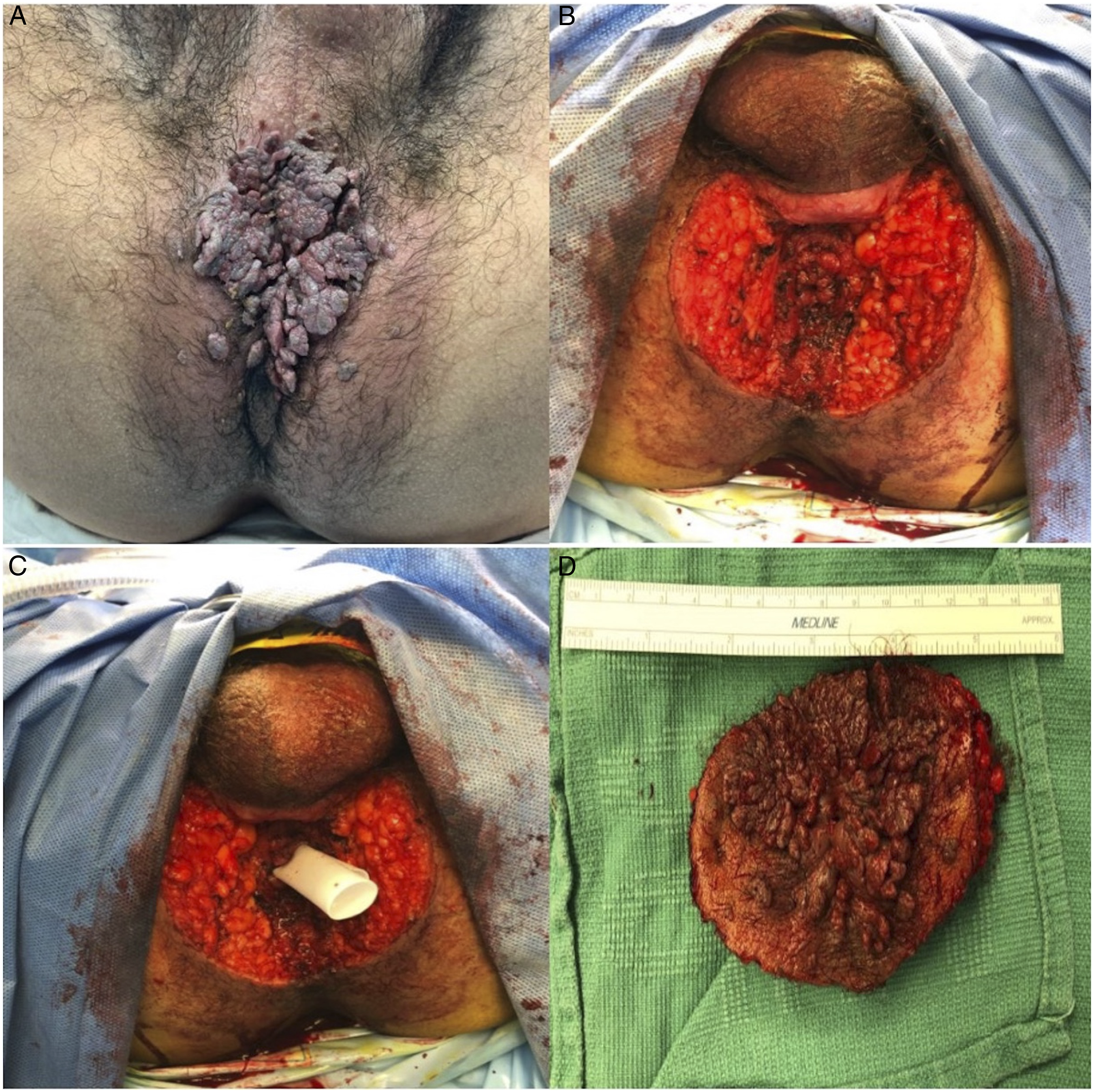
Subsequent Follow-Up
At the patient’s first postoperative visit (day 31), he was doing well overall but experiencing some anal discomfort with fecal evacuation. Examination revealed a well-healing perineal wound with mild stenosis of the neoanus (Figure 2A and B). He was discharged from clinic and recommended to begin daily dilations with a commercially available anal dilator and a bowel regimen of daily docusate and mineral oil to minimize discomfort. He returned to clinic for routine follow-up on postoperative day 57 with difficulty evacuating and examination revealed worsened neoanal stenosis. The wound was otherwise healing well. Because of impressive neo-anal stenosis and worsening symptoms, the patient underwent an anorectal examination under anesthesia (EUA) on postoperative day 59. His anal canal was found to be severely strictured, prohibiting full passage of the surgeon’s fifth digit beyond the neoanus. A 1 cm thick circumferential band of granulation tissue at the level of the neoanus was released with cautery. Gentle dilation of the neoanus was performed first digitally and then followed with Hegar dilators. At the conclusion of the case, the surgeon’s full index finger was able to traverse the neoanus with ease. He was discharged home with plans to continue home digital anal dilations. He continued to do well and had regular bowel movements ranging from one to two per day. A representative image from postoperative day 81 (from index procedure) is shown in Figure 2C. (A) Perianal region on postoperative day 31 demonstrating a healthy, granulating wound and closure via secondary intention; (B) digital rectal examination on postoperative day 31 demonstrating mild stenosis; (C) perianal region on postoperative day 81 demonstrating further closure via secondary intention; (D) perianal region on postoperative day 329 demonstrating a well-healed neo-anus without signs of stricturing.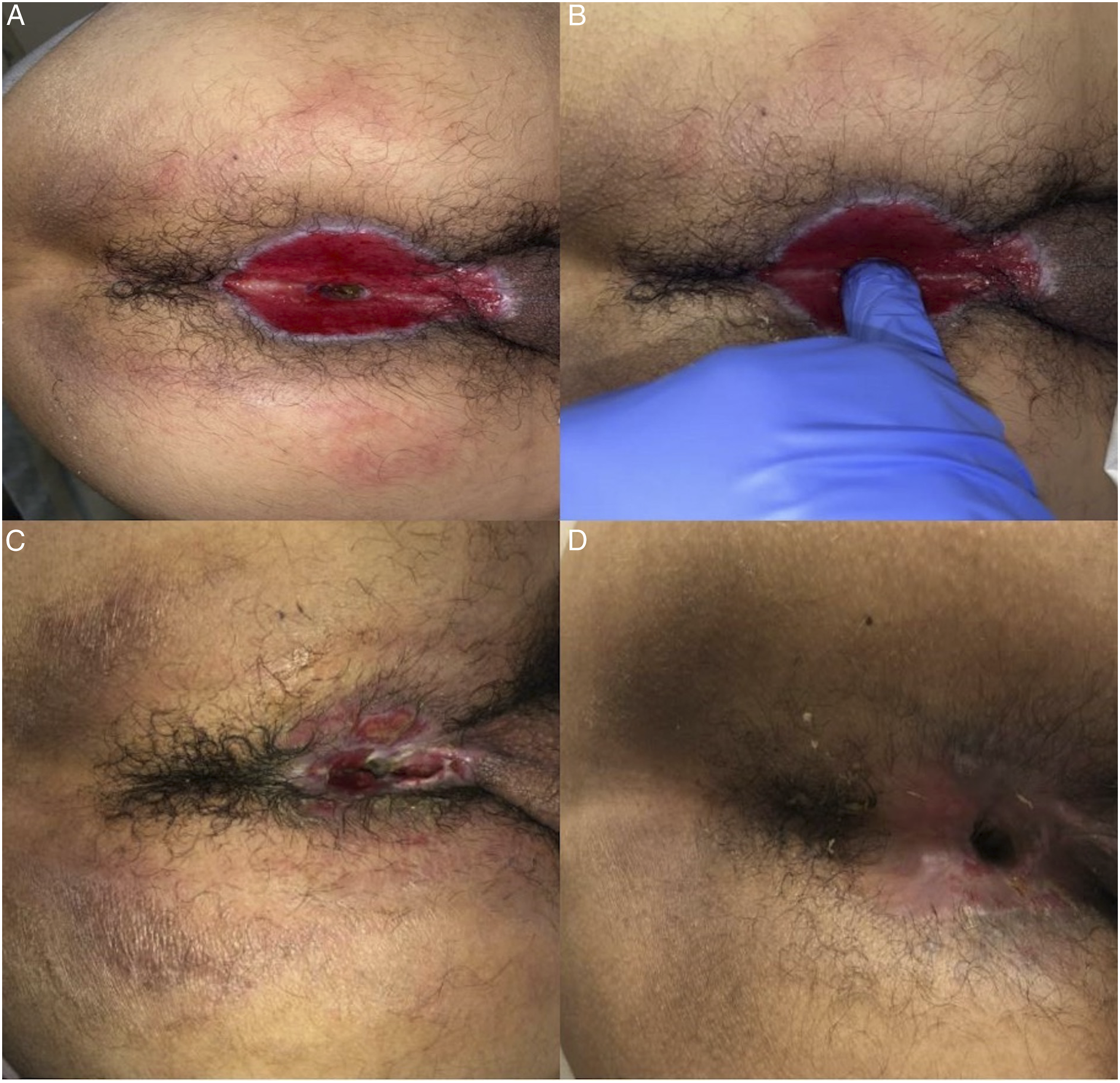
On postoperative day 92 (from index procedure), he underwent a repeat EUA and digital dilation and the scar tissue encountered within the neoanus was gently released. No masses or lesions were found on examination. The patient was discharged with instructions to continue home dilations with a Hegar dilator kit.
At his most recent clinic visit on postoperative day 329 (from the index procedure), he reported regular bowel movements without constipation or incontinence, with only minor bleeding from the operative site associated with wiping. Examination revealed that the site was healing well, with no signs of stricturing (Figure 2D).
Conclusion
En bloc resection of a large GCA with healing by secondary intention has not been widely adopted, as reflected in the paucity in publications including isolated case reports1,2 and a case series published in 2015. 3 We performed a radical resection that left an area of anal mucosa without its normal anatomic circumferential attachments, thereby creating a “free-floating anus.” Compared to prior published techniques that involved extensive flap coverage and multiple serial procedures, at times including fecal diversion, our approach relied on healing by secondary intention and resulted in minimal scarring, optimal cosmesis, with minimal to no impact on the patient’s sphincter function at 1 year follow-up. Furthermore, we were able to avoid many of the feared complications associated with graft or flap failure, such as ischemia, necrosis, or infection. Although our patient did experience minor stenosis of the neoanus, after serial dilations he was noted at last clinic visit to have well-formed bowel movements without fecal incontinence and apparent good quality of life. Because of fears of long-term anal stenosis and incontinence, neither of which occurred in our patient, this technique has not been widely adopted. We believe that the “free-floating anus” approach void of flap coverage and/or proximal ileostomy is an effective and desirable surgical alternative for carefully selected patients presenting with large, circumferential GCA.
Footnotes
Author Contributions
W.Y.L., V.H., D.N.V., and L.H.C.: Writing-Original Draft; Writing-Review and Editing. J.G.G.: Writing-Original Draft; Writing-Review and Editing; Supervision; Conceptualization.
Declaration of Conflicting Interests
The author declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Dr. Guillem had a role as a Consultant for Intuitive Surgical, Inc.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
This study (Ref ID: 392321) was examined by the UNC Office of Human Ethics (Study #: 23-0762) and was determined that this case report does not constitute human subjects research as defined by federal regulations and therefore does not require IRB approval.
Informed Consent
The patient has consented to the submission of the case report for publication, and the authors affirm that the patient provided informed consent for publication of the de-identified images in Figures.
