Abstract
Purpose. Extracellular acidity is a marker of highly aggressive
breast cancer (BC). pH-low insertion peptides (pHLIPs) target the acidic tumor
microenvironment. This study evaluates the distribution and therapeutic efficacy of
radioiodine-labeled pHLIP variant 3 (Var3) in a mouse model of BC.
Methods. The binding of fluorescein isothiocyanate (FITC)- or
radioiodine-125 (125I) labeled Var3-pHLIP to MDA-MB-231, 4T1, and SK-BR-3
BC cell lines under different pH values was evaluated in vitro. The distribution of
125I-labeled Var3-pHLIP and wild-type- (WT-) pHLIP in tumor-bearing
mice was analyzed in vivo using micro-SPECT/CT imaging. The therapeutic efficacy of
radioiodine-131 (131I)-labeled Var3-pHLIP in MDA-MB-231 xenografts was
evaluated by relative tumor volume measurement and immunohistochemical analysis.
Results. The binding ability of FITC- or 125I-labeled
Var3-pHLIP to tumor cells increased with the decrease in pH. The tumor-to-background
ratio of 125I-Var3-pHLIP in BC xenografts showed the best imaging contrast
at 24 h or 48 h postinjection. The uptake of 125I-Var3-pHLIP in MDA-MB-231
xenografts at 2 h postinjection was significantly higher than that of
125I-WT-pHLIP (
1. Introduction
Breast cancer (BC) is the leading cause of cancer death among women [1]. Triple-negative BC (TNBC) is a highly aggressive BC subtype with a high rate of relapse and metastasis and a low survival rate [2]. Chemotherapy resistance is common in TNBC, and the efficacy of endocrine and antihuman epidermal growth factor receptor-2 (HER2) therapies is limited [3]. Therefore, new effective targeted therapies are needed.
Acidosis in the tumor microenvironment promoted by the Warburg effect is a hallmark of cancer. The extracellular pH in this environment is below 6.5 because of H+ production and excretion, whereas extracellular pH in healthy tissue under physiologic conditions is 7.2–7.4. In addition, the acidic microenvironment is not affected by clonal selection and thus is promising for diagnostic imaging and targeted therapy [4].
The 37-amino-acid pH-low insertion peptide (pHLIP) is water-soluble at
This study compared the in vivo distribution of 125I-WT-pHLIP and 125I-Var3-pHLIP in mice-bearing human BC xenografts and investigated the therapeutic efficacy of 131I-Var3-pHLIP in MDA-MB-231 xenografts.
2. Materials and Methods
2.1. Cell Culture
The human BC cell lines MDA-MB-231 (triple-negative BC), 4T1 (stage IV BC), and SK-BR-3 (HER2-positive BC) were purchased from The Cell Bank of the Chinese Academy of Sciences (Shanghai, China) and were cultured in DMEM (Gibco, NYC, USA) containing 4.5 g/L glucose, 10% fetal bovine serum (Gibco, NY, USA), and 1% penicillin-streptomycin (Sigma, St Louis, MO, USA). Cells were incubated at 37°C in a humidified incubator with 5% CO2.
2.2. Peptide Synthesis and Fluorescent Labeling
pHLIP was synthesized by GL Biochem Ltd. (Shanghai, China) through solid-phase chemical synthesis. The amino acid sequences of WT- and Var3-pHLIP are ACEQNPIYWARYADWLFTTPLLLLDLALLVDADEGTK and ACDDQNPWRAYLDLLFPTDTLLLDLLWK. The N-terminal of pHLIP was conjugated with fluorescein isothiocyanate (FITC), and fluorescence in vitro was measured at 495 nm excitation and 519 nm emission.
2.3. Peptide Labeling with 125I or 131I and In Vitro Stability
WT-pHLIP and Var3-pHLIP were labeled with 125I for in vivo imaging experiments, and Var3-pHLIP was labeled with 131I for therapeutic efficacy experiments. Radioactive iodine binds to tyrosine residues in pHLIPs. Peptides were dissolved in 200 μL of 0.02 M PBS (pH 7.4) to reach a concentration of 1 mg/mL and mixed with 10 μL of Na125I (74 MBq) or 20 μL of Na131I (925 MBq). Chloramine-T (20 μL, 5 mg/mL) was added to the test tubes and mixed for 70 s at room temperature. The reaction was stopped by adding 200 μL of sodium metabisulfite (5 mg/mL). The peptides were eluted in ethanol through a C18 column equilibrated with 20 mL of 100% ethanol and 20 mL of distilled water. The radioactive purity of 125I-WT-pHLIP, 125I-Var3-pHLIP, and 131I-Var3-pHLIP was determined using thin-layer chromatography. Furthermore, the radiochemical purity of 125I-WT-pHLIP, 125I-Var3-pHLIP, and 131I-Var3-pHLIP was measured, and chemical stability was determined at 24 and 48 h at room temperature (25°C) in PBS and at 37°C in serum.
2.4. Fluorescence Imaging of FITC-Labeled Peptides In Vitro
DMEM medium and MES buffer were mixed at different volume ratios (100 : 0, 50 : 1,
25 : 2, 25 : 6, and 5 : 2) to simulate extracellular environments with a pH of 7.8,
7.4, 7.0, 6.6, and 6.2, respectively. MDA-MB-231, 4T1, and SK-BR-3 cells were seeded
in 24-well plates at a density of
2.5. In Vitro Cell Binding Assay
Cells were incubated with 125I-WT-pHLIP or 125I-Var3-pHLIP for
1 h at 37°C in the medium at different pH values ranging from 6.2 to 7.8 (6.2, 6.6,
7.0, 7.4, 7.8). At the same time, cells in the medium at pH 6.2 were further
incubated with 125I-labeled peptide with an excess of unlabeled peptide
(25 μg/well). The supernatant was aspirated into a tube. The
cells were then washed twice with PBS of the corresponding pH to remove unbound
radioactivity. The wash solution was also added to the supernatant tube containing
free radioactivity (
2.6. Measurement of Cell Viability Using the Cell Counting Kit-8 (CCK-8) Assay
MDA-MB-231, 4T1, and SK-BR-3 cells were seeded in 96-well plates (
2.7. Animal Models
Five-week-old female athymic BALB/c nude mice (Shanghai Slaccas Experiment Animal
Corp., Shanghai, China) were used in our study. Mouse xenograft models of MDA-MB-231,
4T1, and SK-BR-3 cells were produced by the subcutaneous injection of
2.8. Micro-SPECT/CT Imaging of 125I-Labeled Peptides
Three days before micro-SPECT/CT imaging, 300 μL of 1% Kl solution was administered to mice by oral gavage once a day, and 0.1% Kl was added into the drinking water to block thyroid gland activity. Mice-bearing MDA-MB-231, 4T1, or SK-BR-3 tumors were intravenously injected with 3.7 MBq of 125I-WT-pHLIP or 125I-Var3-pHLIP. Each group contained four mice. The mice were anesthetized by isoflurane inhalation, placed in the prone position, and scanned using a four-head SPECT/CT system (U-SPECT/CT, MI-Lab, Netherlands) and dedicated multipinhole apertures with a diameter of 1.5 mm at 1, 2, 4, 24, and 48 h after injection of 125I-labeled peptides. CT images were acquired after static SPECT imaging (10 min/frame). The images were reconstructed using U-SPECT REC software and analyzed using PMOD software version 3.9 (Switzerland). Regions of interest (ROIs) were drawn in the tumors and organs, including the brain, heart, liver, lungs, kidneys, intestine, and bladder, at various time points. The radioactivity per gram (ID%/g) in the ROIs was measured to obtain the dynamic tumor-to-background ratio (TBR, muscle tissue was used as the background) and the in vivo distribution and kinetics of 125I-WT-pHLIP and 125I-Var3-pHLIP in the xenograft models of BC.
2.9. Therapeutic Efficacy of 131I-Var3-pHLIP in MDA-MB-231 Xenografts
Twenty mice-bearing MDA-MB-231 human BC xenografts were divided into four groups of
five animals. Group 1 was injected with 131I-Var3-pHLIP in the tail vein
on days 0 and 3 (29.6 MBq each day). Groups 2, 3, and 4 were injected with the same
volume of Var3-pHLIP, 131I (29.6 MBq), and saline solution, respectively.
Tumor size was measured every 2 to 4 days postinjection (pi) for 26 days using a
caliper. Tumor volumes (
2.10. Immunohistochemical Analysis
The animals were sacrificed by cervical dislocation. The tumors were excised, fixed in paraformaldehyde, embedded in paraffin, and sectioned. The sections were mounted on glass slides, dewaxed in xylene, dehydrated through a graded ethanol series, and incubated in 3% hydrogen peroxide for 25 min. The samples were incubated with rabbit anti-human caspase 3 (1 : 100, Servicebio, Wuhan, China) and rabbit anti-human Ki67 (1 : 500, Servicebio, Wuhan, China) antibodies for 1 h at room temperature. Slices were washed with PBS thoroughly and incubated with HRP-labeled secondary antibody for 1 h at room temperature. Then, DAB kit was used for visualization and examined by light microscopy, and cells containing brown pigment were considered positively stained.
2.11. Statistical Analysis
Data were analyzed using the SPSS version 20.0 (SPSS Inc., Chicago, IL, USA) and
GraphPad PRISM version 7.0 (GraphPad Software, La Jolla, CA, USA) and represented as
3. Results
3.1. Synthesis and Purification of Peptides
High-performance liquid chromatography analysis showed that the concentration of the main constituent of WT-pHLIP was 91.4% with a retention time of 14.9 min, whereas the concentration of the main component of Var 3-pHLIP was 95.7% with a retention time of 9.5 min. Mass spectrometry analysis showed that WT-pHLIP had a peak at m/z 1135.4 and a molecular weight of 4536.1 Da, and Var3-pHLIP had a peak at m/z 1240.3 and a molecular weight of 3724.2 Da.
3.2. Radiochemical Purity and In Vitro Stability
The radioactive purity of 125I-WT-pHLIP, 125I-Var3-pHLIP, and 131I-Var3-pHLIP was 99.6%, 98.9%, and 99.5%, respectively. At room temperature in PBS buffer, 125I-WT-pHLIP, 125I-Var3-pHLIP, and 131I-Var3-pHLIP had a stability of >95% at 24 h and >90% at 48 h. After 24 and 48 h at 37°C in serum, the stabilities were 86.8% and 86.6% for 125I-WT-pHLIP and 83.2% and 82.6% for 125I-Var3-pHLIP, respectively.
3.3. Fluorescence Imaging and Cell Viability at Different pH Values
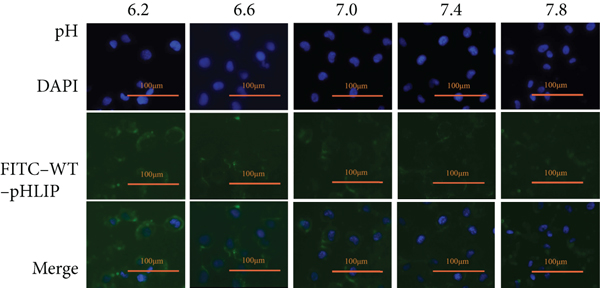
Fluorescence imaging showed that the in vitro distribution of FITC-Var3-pHLIP and FITC-WT-pHLIP in the cell membrane decreased from pH 6.2 to pH 7.8 in the cell lines MDA-MB-231 (Figures 1(a) and 1(b)), 4T1, and SK-BR-3 (Supplemental Figures 1(a)-1(b)). The CCK8 results showed no significant difference in cell viability between MDA-MB-231 (Figures 2(a) and 2(b)), 4T1, and SK-BR-3 (Supplemental Figure 2) treated with or without these two types of pHLIP at the same pH value. Furthermore, there was no significant difference in cell viability between pH treatments.

Fluorescence imaging and cell viability at different pH values. Fluorescence imaging (×100) demonstrated that the ability of (a) FITC-labeled variant 3 pH-low insertion peptide (var3-pHLIP) and (b) FITC-labeled wild-type (WT)-pHLIP to bind to MDA-MB-231 cell line increased with the decrease in pH (7.8, 7.4, 7.0, 6.6, and 6.2).
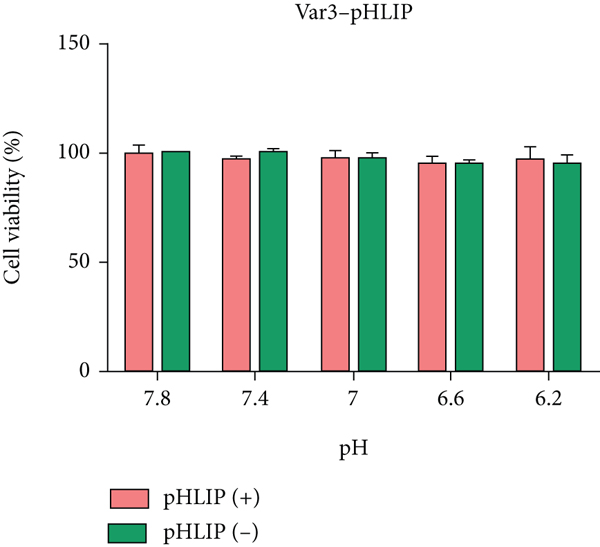
Cell Counting Kit-8 (CCK-8) assay showing cell viability. CCK8 assay showed no significant difference in cell viability in MDA-MB-231 cell line after treatment with (a) FITC-Var3-pHLIP and (b) FITC-WT-pHLIP under different pH conditions.

3.4. Binding Fractions of 125I-Labeled pHLIPs to Cells at Different pH Values
The binding fractions to MDA-MB-231 cells from pH 7.8 to 6.2 were

Binding fractions of 125I-labeled pHLIPs to MDA-MB-231 cells at
different pH values. The binding fractions to MDA-MB-231 cells from pH 7.8 to
6.2 were
3.5. In Vivo Imaging and Distribution of 125I-Labeled pHLIPs in Mice
In vivo micro-SPECT/CT imaging at 1, 2, 4, 24, and 48 h after injection of
125I-pHLIP demonstrated that the TBR of 125I-Var3-pHLIP and
125I-WT-pHLIP was the highest at 24 or 48 h in the three types of
xenografts, and imaging contrast was the highest at these two time points (Figures
4(a) and 4(b)). The TBR of 125I-Var3-pHLIP was
significantly higher than that of 125I-WT-pHLIP at 48 h in MDA-MB-231
xenografts (

In vivo micro-SPECT/CT imaging and distribution of 125I-labeled
pHLIPs in MDA-MB-231, SK-BR-3, and 4T1 breast cancer xenografts. (a)
Tumor-to-background ratio (TBR) of 125I-labeled variant 3
(Var3)-pHLIP and 125I-labeled wild-type (WT)-pHLIP in xenografts
peaked at 24-48 h after injection. The TBR of 125I-Var3-pHLIP was
significantly higher than that of 125I-WT-pHLIP at 48 h in
MDA-MB-231 xenografts (
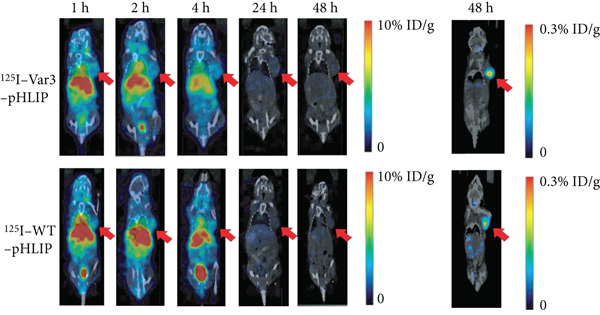

The distribution of 125I-Var3-pHLIP in tumors was the highest at 2 h pi (
The radioactive count in major organs or tissues of MDA-MB-231 tumor-bearing nude mice (Tables 1 and 2) and other two BC mice models (Supplemental Table 1-4) decreased over time. The uptake of 125I-Var3-pHLIP and 125I-WT-pHLIP was high in the heart, liver, lungs, bladder, and kidneys.
Distribution of 125I-Var3-pHLIP in MDA-MB-231 tumor-bearing nude
mice (%ID/g,
Distribution of 125I-WT-pHLIP in MDA-MB-231 tumor-bearing nude mice
(%ID/g,
3.6. Therapeutic Efficacy of 131I-pHLIP (Var3) In Vivo
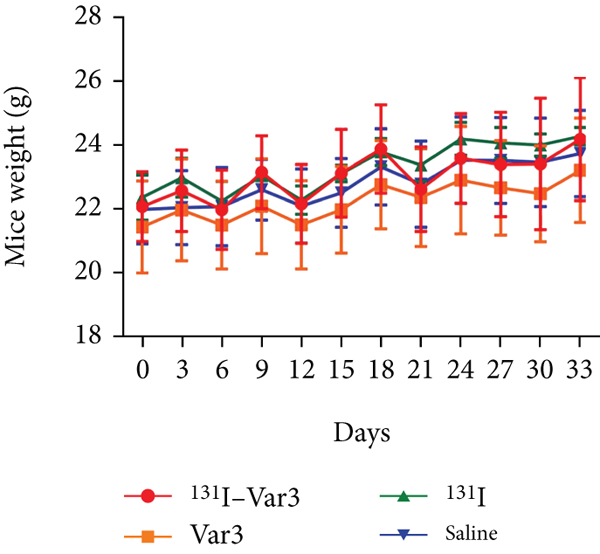
The relative tumor volume in MDA-MB-231 xenografts was significantly lower in the
131I-Var3-pHLIP-treated group (

Therapeutic efficacy of 131I-labeled variant 3 pH-low insertion
peptide (Var3-pHLIP) in mice-bearing MDA-MB-231 xenografts. (a) Images of
MDA-MB-231 xenografts in the four study groups (


The immunohistochemical expression of Ki67 and caspase 3. The Ki67 expression was lower, and the caspase 3 expression was higher in the 131I-Var3-pHLIP-treated group than in the other three groups (magnification, ×365).
4. Discussion
The increased acidity in the extracellular environment due to the Warburg effect in highly aggressive cancers, including TNBC, where endocrine and molecular therapies are ineffective, is a new therapeutic target. pHLIPs sense the pH in the vicinity of the plasma membrane. The protonation of two aspartate residues in the spanning domain of pHLIP in an acidic environment allows the insertion of this peptide across the plasma membrane [12].
WT-pHLIP, Var3-pHLIP, and Var7-pHLIP are currently the most promising peptides of the
pHLIP family. Positron emission tomography and fluorescence studies showed that,
compared with WT-pHLIP, the distribution of Var3-pHLIP and Var7-pHLIP in the liver was
lower probably because of their lower hydrophobicity at physiological pH. Var7-pHLIP is
shorter and less hydrophobic than Var3-pHLIP, increasing clearance from the blood and
liver but potentially decreasing its uptake by tumors [9, 14]. Therefore, Var3-pHLIP was selected for this study. A previous study
showed that the uptake of [17]F
and 64Cu-labeled Var3-pHLIP in 4 T1 xenografts was
The ability of pHLIP to target the acidic microenvironment of tumors allows its use as drug carriers. Studies have covalently bound therapeutic drugs that cannot cross the plasma membrane (phallacidin [18], amanitin [17], protease-activated receptor 1-activating peptide [19], antimiR-155 [11]) to the hydroxyl terminus of pHLIP, allowing drug release to tumors. 131I labeling is simpler than conjugating the above drugs to pHLIP. The present study showed that 131I-Var3-pHLIP inhibited tumor growth in MDA-MB-231 xenografts through ionizing radiation damage. However, treatment had some limitations. First, 131I-Var3-pHLIP was widely distributed in blood-rich organs such as the liver, heart, and lungs, increasing radiation damage to these normal organs. Second, 131I-Var3-pHLIP was cleared quickly from tumors, and its distribution in tumor tissue at 24 h pi was 12.5% of that at 2 h pi; thus, repeated injections are necessary to achieve the radiation dose required for effective treatment. Therefore, developing pHLIP variants with higher retention in tumor and faster blood clearance is necessary to improve the therapeutic efficacy and safety of 131I-labeled pHLIPs. Third, previous studies have shown that local inflammation was closely associated with increased acidity of extracellular microenvironment in the involved organs and tissues, which makes pHLIPs accumulate in the inflammatory diseases such as arthritis [7], pneumonia [20], and active vulnerable plaques [21]. Thus, inflammatory disease may increase the interpretation complexity of pHLIP for cancer imaging and tumor selectivity of pHLIP as a therapeutic vehicle.
5. Conclusions
Radioiodine-labeled Var3-pHLIP effectively targeted breast cancer cells in an acidic environment and inhibited the growth of MDA-MB-231 xenografts by ionizing radiation.
Footnotes
Data Availability
The datasets generated and analyzed during the current study are available from the corresponding author on reasonable request.
Ethical Approval
All animal experiments conformed to the guidelines of the Animal Care and Use Committee of Ruijin Hospital, School of Medicine of Shanghai Jiao Tong University and to the National Institutes of Health Guide for the Care and Use of Laboratory Animals (Publication No. 8023, revised in 1978). Tumor samples were immediately snap-frozen and stored at -80°C, and the specimen collection was approved by the Medical Ethical Committee of the hospital.
Conflicts of Interest
The authors have declared that no competing interest exists.
Authors’ Contributions
Biao Li contributed to the study conception and design. Material preparation, data collection, and analysis were performed by Min Zhang and Yue Xi. Hong Chen and Wangxi Hai carried out the experiments. The first draft of the manuscript was written by Min Zhang and Yue Xi, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript. Min Zhang and Yue Xi contributed equally to this work.
Acknowledgments
This research was supported by the National Natural Science Foundation of China (No. 81501499) and Shanghai Municipal Key Clinical Specialty (shslczdzk03403). We thank the staff, Xiabin chen, from Jiangsu Huajing Molecular Imaging & Drug Research Institutes Co., Ltd., China for the technology support of radioiodine labeling of peptide.
