Abstract
There is little information about the perception of experimentally induced extracephalic pain in migraine. This study investigates the associations between mammography-related pain and migraine. A neurologist clinically assessed 630 women aged 40–74 years attending a population-based breast cancer screening programme. Headache criteria proposed by the International Headache Society were used. Mammography-related pain was measured on a 100-mm visual analogue scale. High levels of mammography-related pain were associated with migraine. This association was related to mammographic examination during the early follicular phase and menopausal status, but unrelated to differences in age, compression pressure, education, current use of hormonal replacement therapy, anxiety, and recent use of analgesics and antimigraine medication. The results of the present study indicate that migraine and compression-induced breast pain are related.
Introduction
Recent migraine research has focused on the existence (1) and high prevalence of cutaneous allodynia (2) and the comorbidity of migraine with other pain states such as spinal (3, 4) and musculoskeletal pain (5), abdominal pain (6) and endometriosis (7, 8). To our knowledge, the relation between breast pain and migraine has not previously been studied.
Mammography-related pain (MRP) is perceived by 1–85% in breast cancer screening programmes (9). Pain is induced by compressing the breasts between a plastic paddle and the film cassette. Mean pain intensity measured on a 100-mm visual analogue scale (VAS) is approximately 30 mm (10, 11).
Most information on comorbidity with other pain states comes from epidemiological studies based on questionnaires or interviews. Much less information has been collected on experimental pain in migraine in the general population (12, 13) or in population-based samples (14). Buchgreitz et al. (12) found higher cephalic tenderness scores in women with migraine than in women without headache, but no differences in men. No association between pressure pain thresholds (temporal muscle and index finger) and migraine were found.
It is interesting to know if migraine headache is associated with experimentally induced extracephalic pain. This study addresses the question: is migraine associated with differences in the perception of compression-induced breast pain?
Study population and methods
All women aged 40–74 years living in a small community in Östhammar, Sweden are invited every second year to a mammography screening programme (MSP). The women are identified in the official population registry of Statistics Sweden. The attendance rate is > 80% (15).
The source of the study population was women aged 40–74 years who lived in Östhammar during the study period from November 1997 to October 1998 and attended the local mammography unit (MUT), where they were asked to participate in our study. The names of women invited to attend the MSP on a particular working day are available at the local MUT. We invited 838 attending women to participate in our study. The study design has been described in greater detail previously (16). New knowledge on allodynia in migraine was the impetus to analyse data collected on MRP.
Interview, measures and definitions
Participants were interviewed at the MUT by a board-certified neurologist. Physical and neurological examinations were not performed.
The interview structure was based on the headache criteria proposed in 1988 by the International Headache Society (IHS) (17). This study focused on migraine headache. No information on tension-type headache was obtained. Migraine headache is referred to as migraine. Women had migraine if their headaches (i) fulfilled the criteria for migraine without aura or (ii) fulfilled the criteria for migraine with aura and the headaches in conjunction with the aura fulfilled the criteria for migraine without aura. Active migraine headache was defined as one or more migraine attacks in the previous year.
All women with migraine experienced inhibition (moderate disability) or prohibition (severe disability) of daily activities during migraine attacks. Frequency of migraine was measured in 10 predetermined categories as the number of days in the previous year during which the women had headache (1, 2–3, 4–6, 7–9, 10–12, 13–24, 25–48, 49–96, 97–180 and > 180 days). The use of predetermined categories speeded up the collection of continuous data.
The mammograms were obtained by a CGR mammograph (General Electric, Fairfield, CT, USA). The technician varied the compression pressure to achieve a balance between tolerable pain and high quality of the mammograms. The magnitude of the compression pressure was indicated by the mammograph (bar). The technician recorded the compression pressure of the left breast because the pressure indicator was easier to observe from the left than from the right side of the women. MRP was measured on a 100-mm VAS ranging from ‘no pain’ (= 0) to ‘pain as intense as you can imagine’ (= 100 mm).
Educational levels were combined into two classes (upper secondary school or university vs. any lower educational level) in all analyses.
We used the Somatic trait anxiety (STA) scale of the Swedish universities Scales of Personality (18) as a measure of anxiety. The STA scale comprises seven items. Each item is presented as a statement with a four-point response format, ranging from ‘Does not apply at all’ (= 1) to ‘Applies completely’ (= 4). The values were summarized. STA reflects tenseness, autonomic disturbances, and restlessness. The STA scale was chosen among other scales because it has been shown to be associated with active migraine (19).
Women were asked about the frequency of pain at four locations during the previous year: abdominal, thoracic, muscular and back pain. The questions were included in a questionnaire. To each question a four-point response format was given: ‘Never/seldom’, ‘Sometimes’, ‘Often’ and ‘Almost always/always’. Women almost always or always experiencing pain in one or more parts of the body were considered to have chronic non-cephalic pain.
Data on characteristics of menstrual cycles were obtained by means of the questionnaire. Data on the number of menstrual bleedings in the past year were collected using a six-point response format: none, 1–6, 7–9, 10–12, ≥ 13, or do not know. Women with at least six menstrual bleedings in the past year were asked how often their menstrual bleedings occurred within 2 days prior to or after the next expected menstrual bleeding. A four-point response format was given; never or seldom, sometimes, most times, almost all times or all times. Data on menopausal status, current use of hormone replacement therapy (HRT) (Anatomical Therapeutic Chemical classification codes G03C, G03D and G03F), prior hysterectomy and day of menstrual cycle were collected through direct interview. These data were used to identify women in natural (non-surgical) menopause, i.e. women who had had their last periods at least 1 year prior to the study. For the purpose of the study, women in the first 5 days of their menstrual cycle were considered to be in the early follicular phase. This definition is used in endocrinological research (20) and corresponds to the median length of menstrual flow in middle-aged Swedish women (21). No data on menstrual irregularities, ongoing menstrual flows or cycle length were collected.
Information was obtained about the intake of analgesics or antimigraine drugs during the 3 days prior to the study.
The neurologist was unaware of the participants' pain ratings, and the mammography technician was unaware of the participants' migraine status.
All women gave their informed consent to participation, and the Ethics Committee of the Medical Faculty, University of Uppsala approved the study (No. 97307).
Data analysis
Logistic regression analysis was used to analyse differences in characteristic between women with and without active migraine (Table 1).
Descriptive statistics of participants according to migraine status

∗ P-value from logistic regression analysis.
†High education was defined as upper secondary school or university.
‡Drug intake during 3 days prior to the study.
§Daily or near-daily muscular, abdominal, thoracic, or spinal pain in the previous year.
HRT, hormonal replacement therapy; STA, Somatic Trait Anxiety; MRP, mammography-related pain.
Initial analyses used logistic regression analysis to test if MRP treated as a continuous independent variable is associated with the dichotomous dependent variable migraine with and without controlling for differences in age (continuous), education (secondary school or university vs. any lower educational level), and compression pressure (continuous) (Reference Model of Table 2).
Association between migraine and mammography-related pain (MRP) in different models

AGE, age; EDU, educational level; CP, compression pressure at mammography; MRP, mammography-related pain; HTR, hormonal replacement therapy; MS, menopausal status; STA, Somatic Trait Anxiety; ANAL, intake of analgesics or anti-migraine drugs during 3 days prior to the study; CNCP, chronic non-cephalic pains; EFP, early follicular phase at mammography screening.
It was particularly interesting to analyse in more detail if the effect of MRP on migraine was confounded by STA (continuous), early follicular phase (yes vs. no), menopausal status (post menopause vs. pre-menopause or undetermined menopausal status), current use of HRT (yes vs. no), intake of analgesics or antimigraine drugs during 3 days prior to the study (yes vs. no), chronic non-cephalic pains (yes vs. no). Each of these six potential confounders and their interaction terms with MRP were added to the reference model in six separate models. Interaction terms were added in order to analyse if the effects of MRP on migraine differed across levels of the potential confounders (Table 2). Analyses of the effect of the early follicular phase included 628 women due to two missing values.
We explored the relationship between frequency of migraine and MRP in an ordinal logistic regression model. Due to sparse data, frequency was divided into three strata: 1–12, 13–48 and > 48 migraine days during the previous year. Frequency was the dependent variable. MRP (continuous) was the independent variable. The analyses were conducted with and without controlling for differences in age and education.
Correlations between MRP (continuous) on the one hand and compression pressure, age and STA were analysed by Kendall's non-parametric method.
The statistical program package JMP (version 5.11) was used. P-values < 0.05 were considered significant. All tests were two-sided.
Results
During the study period, 4398 women aged 40–74 years lived in Östhammar. We conducted the study on 32 working days. There were 996 women in the invitation lists on these days. Of the 996 invited women, 838 attended the MUT, where they were asked to participate in our study. Seven hundred and twenty-eight women agreed to participate.
Forty-two women felt that they were busy. They were later interviewed in their homes by telephone and did not receive the personality questionnaire. Thirty-one women did not return the questionnaire. Four women were excluded because their questionnaires contained too many missing values. Data on compression pressure and MRP were missing in another 21 women. This left 630 (75.2% of 838) women with a complete dataset.
The characteristics of women with and without migraine are given in Table 1. The prevalence of active migraine was 19.4% (95% confidence interval 16.3, 22.5). Women with migraine were statistically significantly younger and scored higher in STA than women without migraine, whereas the compression pressure did not differ between the groups. The proportion of women with migraine who were postmenopausal and of women who had recently taken analgesics or antimigraine drugs was statistically significantly higher than in women without migraine, whereas current use of HRT and examination during early follicular phase did not differ between the groups.
Mean VAS of MRP in women with migraine, women without migraine, and whole study population was VAS 18.9 mm (
Higher MRP ratings were associated with active migraine both in crude analysis and after controlling for differences in age, education and compression pressure (Table 2). The risk estimates for migraine in the reference model and in models 1a, 2a, 3a, 4a, 5a and 6a (Table 2) varied from 0.011 to 0.13, indicating that the risk for migraine increases by an increase in MRP and that there was no evidence of significant confounding. However, the interaction term between ‘menopausal status’ and MRP (P = 0.03) was statistically significant. This means that the effect of MRP on migraine differs according to menopausal status, which is illustrated in Table 3. In addition, the interaction term between ‘early follicular phase’ and MRP (P = 0.02) was statistically significant. The same analysis was also done after excluding postmenopausal women. The interaction term remained significant (P = 0.007). This means that the effect of MRP on migraine differs depending on whether women were in the first 5 days of their menstrual cycle on the day of the mammographic examination or not, which is illustrated in Table 4.
Mean mammography-related pain by migraine status and the presence of early follicular phase at mammography examination
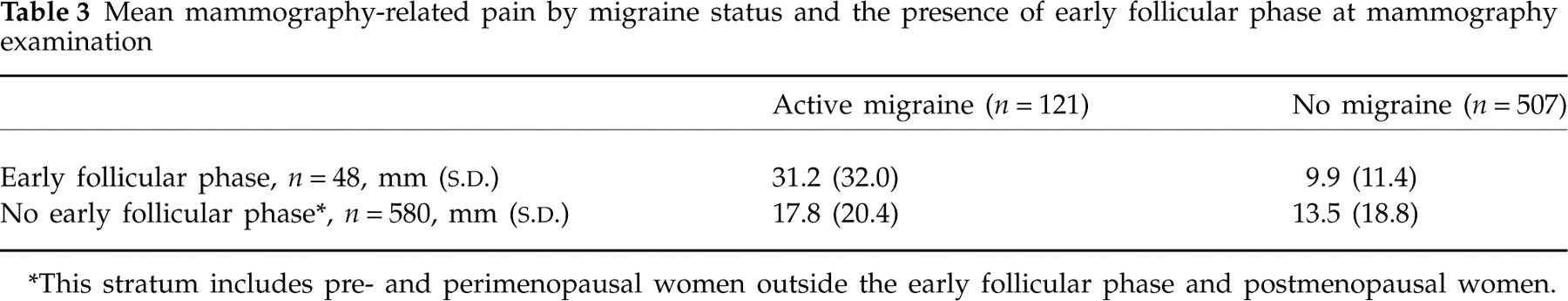
∗This stratum includes pre- and perimenopausal women outside the early follicular phase and postmenopausal women.
Mean mammography-related pain by migraine and menopausal status

Eighty of the 122 women (65.6%) with migraine experienced 1–12 migraine days during the previous year, 33 (27.0%) experienced 13–48 migraine days during the previous year, and nine (7.4%) experienced > 48 migraine days during the previous year. Only two women reported > 97 migraine days in the past year. This was the reason for not dividing frequent migraine any further. Frequency of migraine was not associated with MRP, controlling for age and education (ordinal logistic regression, 1 d.f., likelihood ratio χ2 = 0.001, P = 0.92).
High MRP was statistically significantly correlated with high compression pressure and high scores in STA (Kendall's τ= 0.08, P = 0.008 for both correlations). MRP decreased by advancing age, but this correlation was not statistically significant (Kendall's τ=−0.05, P = 0.07).
Discussion
We found that migraine was associated with high levels of breast pain induced by compression. Interestingly, menopause and mammographic examination during early follicular phase interacted with the migraine–MRP association, whereas adjustments for several variables changed the association only marginally.
The prevalence of migraine was 19%, which is similar to the findings in studies based on IHS criteria (22). The low frequency of women with chronic daily migraine attending the MUT may be due to previous painful experience of MRP. Women with ongoing migraines may also be less functional and less likely to go out and attend the MUT. The finding of a mean breast pain intensity of only 14 mm on a 100-mm VAS was somewhat lower in this study compared with previous findings of approximately 30 (10, 11). When the present study was conducted, women living in Östhammar had been invited up to seven times to attend the MSP. We suggest that the relatively low mean MRP was due partly to non-attendance of women with previous painful experiences (23) and gentle examinations by an experienced technician.
To our knowledge, this is the first report on migraine and breast pain induced by compression. The findings that women with migraine are more sensitive to compression of their breasts differ from what could have been expected from previous experimental research. Although new data collected by means of interviews support the idea that allodynia is present between migraine attacks (24), this is not supported by experimental research (1, 25–27).
Although there is a lot of knowledge about cutaneous pain perception and sensory innervation of the skin, much less is known about sensory nerves of the mammary gland responding to noxious stimuli (28). Increases in ductal pressure play a physiological role in milk ejection (29), which suggests that there are pressure-sensitive receptors within the breast. The highly sensitive nipple and areolas are usually not compressed during mammography examination. Compression force was positively related to MRP in this and in a previous study (30). Pain is usually experienced within the breasts (31). These observations are in line with the hypothesis that pressure changes within the mammary gland or its ducts are of greater importance in MRP than pressure applied to the skin. We speculate that the perception of cutaneous pain and MRP differs. If this is true, the results of the present study point to a pain mechanism hitherto not described in migraine—interictal hypersensitivity or allodynia of non-cutaneous tissue in migraine.
What is the cause of breast hypersensitivity in migraineurs? Sex hormones are thought to be of importance in migraine (32, 33), although some studies have questioned the existence of a large effect of menstruation (34, 35) and of menopause (36) on migraine. Breast tenderness and pains (37) are common in women and sometimes cyclic. We speculated that fluctuations in oestrogen levels may give rise to breast swelling and tenderness and migraine in the same women. Among women in their early follicular phase at the time of examination, mean MRP was substantially higher in migraineurs than in non-migraineurs (Table 3). The significant interaction between the occurrence of early follicular phase at the time of mammographic examination and migraine remained after exclusion of postmenopausal women. These findings are in line with the hypothesis that female hormones are a link between migraine and MRP. However, in postmenopausal women there was a similar large difference in mean MRP between those with and those without migraine, the highest mean being found in the former group (Table 4). Clearly, this finding was unexpected. We speculate that increased sensitivity is caused by interaction between involutional aberrations such as duct dilations, macrocysts and periductal fibrosis (38) and migraine. There were no large differences in MRP neither between migraineurs and controls not experiencing menstrual flow during examination nor in the group of pre- and per menopausal women as a whole (Tables 3 and 4). Thus, if oestrogens play a role in migraine and breast pains, as indicated by the data, there are probably different mechanisms according to hormonal status.
Some authors have proposed that HRT is an aetiological factor in migraine in women (36, 39), whereas others have not (40). HRT may cause mammographic increases in breast stroma density and breast pain in a significant percentage of postmenopausal women (41). In this study, HRT did not affect the association between migraine and MRP.
Did recent headaches facilitate or enhance breast pain perception as expected from central sensitization? First, the variable ‘recent intake of analgesics or antimigraine drugs’ was used as a surrogate variable for ‘the presence of migraine or any pain requiring medication in 3 days prior to the study’ and to account for the analgesic effect of such medications. Second, among women with migraine there was no association between number of days with migraine during the previous year and MRP. Third, a minority of women with migraine had frequent attacks. Fourth, daily or near-daily non-cephalic pains did not confound the association between migraine and MRP. Thus, it is felt that recent migraines, tension-type headaches or pains of other origin are unlikely to explain the increase in breast tenderness in migrainous women in this study.
The main strength of this study is that the same neurologist interviewed all participants using internationally accepted headache criteria. He was unaware of the MRP ratings. MRP was measured by a 100-mm VAS that has been used extensively in pain research. Furthermore, the study population was large and representative of the corresponding sex and age segment of the community with the exception of women aged 70–74 years, who were underrepresented (16, 42). Several potential confounders such as sociodemographics, hormonal factors, anxiety and chronic pain were taken into account in the analyses.
This study has some limitations. The compression pressure varied between participants. The reliability of the compression manoeuvre was not tested. There was a weak correlation between the recorded pressure and MRP. This may be explained by the multidimensional character of pain experience. Although the mean compression pressure was similar in migraineurs and non-migraineurs, and accounted for in the analyses, non-standardization of the compression pressure may introduce bias. Information was not collected on cycle length or ongoing menses, limiting the possibility to do additional analyses of the impact of hormonal factors on the relation between MRP and migraine. Further potential constraints are the uncertain validity of the measures of anxiety and ongoing headaches. STA measures the degree of a personality trait related to anxiety. No information was obtained specifically about tension-type headaches. The question about the presence of migraine or any pain requiring medication in 3 days prior to the study is probably sensitive but non-specific in relation to recent headaches. Only two women reported daily or nearly-daily migraines in this study, limiting the possibility to analyse the potential effect of frequent migraines on the association between MRP and migraine.
The results of this study should be confirmed in experimental studies of women in different hormonal status using methods to differentiate between cutaneous pain and pains of other origin. Standardization of pain stimuli as well as examinations both on headache-free days and during headaches would contribute considerably to the validity of future studies.
We believe that this study has yielded some important conclusions. Migraine and high intensity of compression-induced breast pains are associated. Menopause and mammographic examination during early follicular phase interacted with the migraine–MRP association. The results do not comply with recent hypotheses about cutaneous allodynia observed in experimental migraine research. It is suggested that the findings are explained by interictal breast hypersensitivity or allodynia.
Footnotes
Acknowledgements
The author thanks Lille-Mor Jansson, Yvonne Björn and Ingrid Lindquist for excellent research assistance, and Dr E Thurfjell (Department of Diagnostic Radiology) and Gunnar Berglund and Marita Berglind (Östhammar Mammographic Screening Unit) for their kind cooperation.
