Abstract
It is a general belief that migraine attacks are prone to occur on days off. Only a few studies, however, have addressed this issue. The objective of this study was to investigate the periodicity of migraine with respect to weekly (circaseptan) variations. Eighty-nine females of fertile age who had participated in a previous questionnaire-based study volunteered to record in detail every migraine attack for 12 consecutive months. Eighty-four patients completed recordings for a mean of 311 days (S.D. = 95.9, range 30-365). A total of 2314 attacks were recorded. Migraine occurrence was almost equally distributed during the week, except on Sundays, when there were significantly fewer attacks (
Wolff's Headaches and other head pains, 4th edn (1).
Introduction
Leisure sickness is considered relatively common, especially in migraine (2). According to some questionnaire-based and retrospective studies the frequency of migraine attacks may exhibit a weekly pattern with increased susceptibility to attacks at weekends (3–8). These findings were not supported in a small prospective study (9). Cull reported the highest number of attacks on Fridays and Saturdays based on a review of 960 attacks (10). No statistical analysis was done and there is actually a uniform distribution in this material. Torelli et al. found increased numbers of migraine attacks at weekends for men but not for women in a small diary study (11). A circaseptan (weekly) recurrence of migraine was also found in a prospective diary study from Italy (12). The authors of this study found a peak incidence on Sundays and lowest frequencies on Wednesdays. Osterman et al. found weekly periodicity for both patients with tension headache and those with migraine (13). However, they found a peak on Thursdays and Saturdays and lowest frequencies on Sundays and Mondays. We set out to investigate the weekly distribution of migraine attacks.
Methods
One hundred and sixty-nine female migraineurs who had participated in a previous questionnaire-based study were invited to keep diary cards where dates and characteristics of all their migraine attacks over 52 consecutive weeks were annotated (14). Eighty-nine patients responded. All were of fertile age and had no concomitant serious disorder. They were diagnosed according to the criteria set by the International Headache Society (15). Patients with missing data (attacks not consecutively recorded) and patients with more than 14 days per month with headache were excluded. We reviewed all diary entries covering the period between March 2004 and April 2005. Besides Sundays, this period also included 11 public holidays when public offices, shops, enterprises, banks and schools were closed. According to IHS
Statistics
Data were analysed with SPSS software (version 12.0 for Windows; SPSS Inc., Chicago, IL, USA) and Excel spreadsheet (Excel 2002, Microsoft Inc., Seattle, WA, USA). The data consisted of a number of individual time series, with a wide range of frequencies. A box-and-whisker plot was given to visualize the sample variation. Given that Si denotes every Sunday with an attack for person
Results
Three patients were excluded due to missing data and two patients were excluded due to chronic migraine or medication-overuse headache. Only 58 had complete recordings over the 52 weeks. Twenty-six patients completed records for 4–48 weeks. The mean ±
Demographics and headache characteristics of all patients invited to record their migraine attacks

MA = migraine with aura, MoA = migraine without aura.
Nine patients were shift-workers, eight were students, one was unemployed and one was incapable of paid employment. Patients completed recordings for a mean of 311 days (

Boxplot showing individual data.
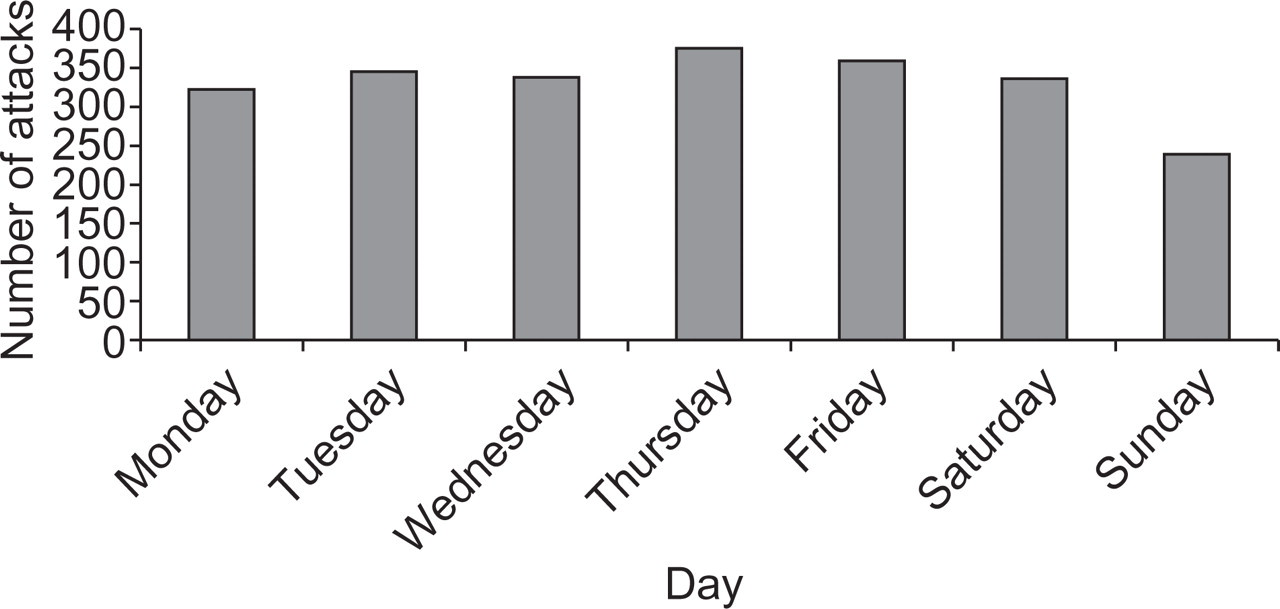
Histogram of the weekly variation in migraine onset.
Migraine occurrence was almost equally distributed during the week, except on Sundays, when there were significantly fewer attacks (

Distribution of onset of migraine attacks by day of the week vs. type of migraine and work.
Distribution of onset of migraine attacks by day of week vs. type of migraine and work
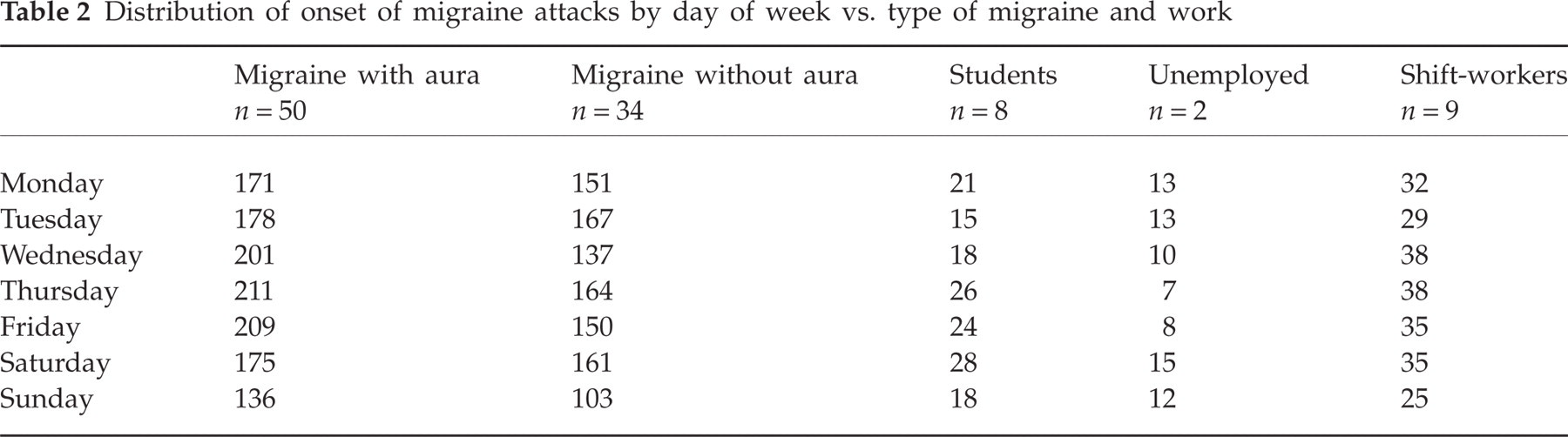
The temporal distribution with fewer attacks on Sundays was not found in the aggregated subgroup of students, unemployed and shift-workers (
Discussion
The presence of biological circaseptan rhythms (7-day cycles) is highly controversial, and the most obvious reasons for weekly phenomena seem to be attributed to the societal 7-day week (17). We have shown that migraine attacks less frequently occur on Sundays and holidays. A major strength of this study is the prospective approach and the restricted study population, which made it possible to reduce confounding before data were collected. Based on the selection of patients in the previous study (14), the population studied constituted a very homogenous group. By inspection, individual groups, as listed in Table 1, did not differ much from the entire group. Diary cards with missing values were excluded, and hidden frequencies should not be a major concern. Not every person under observation experienced the same number of holidays, and an estimate based on the total observation time had to be made for the persons who did not complete their recordings for 52 weeks. Due to this and the fact that the holidays were not equally distributed throughout the year, the estimated RRMH may be slightly biased. The box-and-whisker plot (Figure 1) shows that variation in individual data can not explain the low frequency of attacks on Sundays compared with the other days of the week.
Torelli et al. concluded in their first study of weekend migraine that the weekend is merely a trigger factor in migraine without aura (5), and in the second study that weekend headache is a disorder typically affecting men (11). Our study does not add information regarding migraine in males, nor does it throw light on the role of caffeine as discussed by Coutourier et al. (7). However, release from stress and the inability to adapt to the non-working situation has been a way of explaining weekend migraine (2, 8, 11, 18, 19). Our study indicates the opposite; rest on days off protects against migraine. In Norway, Sundays and public holidays are statutory holidays. Most people do not work on Saturdays either, but traditionally Saturdays are much busier than Sundays when no shops, banks, etc., are open. Unfortunately, no information about which patients actually worked at weekends and when patients had their annual holiday was available. However, patients not in jobs did not experience fewer attacks on Sundays, indicating that work and probably work-related stress influence the weekly pattern of migraine. In a registration of short-time sickness-related absenteeism in Norwegian industry, 6.2% was due to headache, mostly migraine (20). In a French cohort-study approximately 0.7% of the annual numbers of working days were lost on average per individual with migraine (21). Increasing social demands can result in both increased health problems and a substantial cost for society (22). Migraine alone has been estimated to cost the European society a total of €27 billion (23).
Overall, we found fewer attacks at weekends and on days off, suggesting that the opinion of Wolff is wrong (1). Our study contradicts the finding of peak incidences on Sundays in patients with migraine without aura, and does not support that patients without aura as compared with patients with aura are more likely to have attacks at weekends (3, 12). The term
In summary, our study suggests that days off protect against migraine.
