Abstract
Approximately 57 patients with red ear syndrome have been reported in the literature since it was initially described in 1994. The clinical phenotype therefore continues to be defined and no consistent treatment response has been described. We report three new cases of red ear syndrome and suggest that the disorder may exist as a primary trigeminal or cervical autonomic cephalalgia, coexist with other rare trigeminal autonomic cephalalgias, or may be secondary. The pathogenesis in these different circumstances may be distinct, the triggers specific and, when secondary, the disorder may be more resistant to treatment.
Introduction
The red ear syndrome was first coined and described by Lance in 1994 (1, 2). He reported 12 patients with recurrent attacks of unilateral ear discomfort or burning associated with erythema of the ipsilateral ear. The disorder was idiopathic in two patients and associated with upper cervical disorders (arachnoiditis, cervical root traction, facet joint spondylosis), glossopharyngeal and trigeminal neuralgia, temporomandibular joint (TMJ) dysfunction and a thalamic syndrome in the remaining 10 patients
Since this initial description, approximately 45 patients have been described in the literature (3–13). Other secondary pathologies have been associated with the syndrome, including Chiari I malformation, herpes zoster virus infection of the C3–C6 dermatomes, and exercise-induced compression of the cerebellar tonsils (3). Various case reports have shown that the disorder need not necessarily result in significant ear pain, but rather only redness of the ear (4).
In addition, an association with primary headache disorders including migraine, chronic paroxysmal hemicrania (CPH), hemicrania continua (HC) and SUNCT syndrome has been reported (5, 6, 8, 9). Symptoms extending into the face and bilateral/alternating ear pain and erythema have also been seen, especially in those patients with migraine (5). The association with primary headache disorders that are all characterized by activation of cranial autonomic pathways suggests a similar underlying pathogenesis.
Perhaps because of the multiplicity of potential causes, there is no single treatment of choice and many patients have proven to be treatment resistant. We report three cases of red ear syndrome which were partially or completely responsive to indomethacin or ibuprofen.
Case 1
A 49-year-old female presented with a 2-year history of daily, paroxysmal, cold-induced attacks of left ear pain, accompanied by a bright red colour change of the ear. There were no other triggers reported. The erythema lasted 10–15 min and was followed by sharp lancinating pains over the V1 and V2 distributions of her left face, lasting up to 9 h. Partial relief of the pain was noted with manual compression of the left ear. Prior to neurological referral, she had been started on gabapentin 300 mg three times daily, which largely eliminated the facial pain. The patient's past medical history was remarkable for migraine, idiopathic congenital fusion of C1–C3 and enlargement of the cervical spinal canal, as well as bilateral TMJ dysfunction.
Physical examination revealed dysmorphic facial features with facial asymmetry, short neck and jaw prominence on the left. Clicking of the TMJ joint on the right was noted on palpation. Passive and active C-spine mobility was decreased in all axes. An attack was easily provoked in the office by cooling the left ear with a fan for a period of 5 min (Fig. 1). The same stimulus to the right ear did not elicit symptoms.
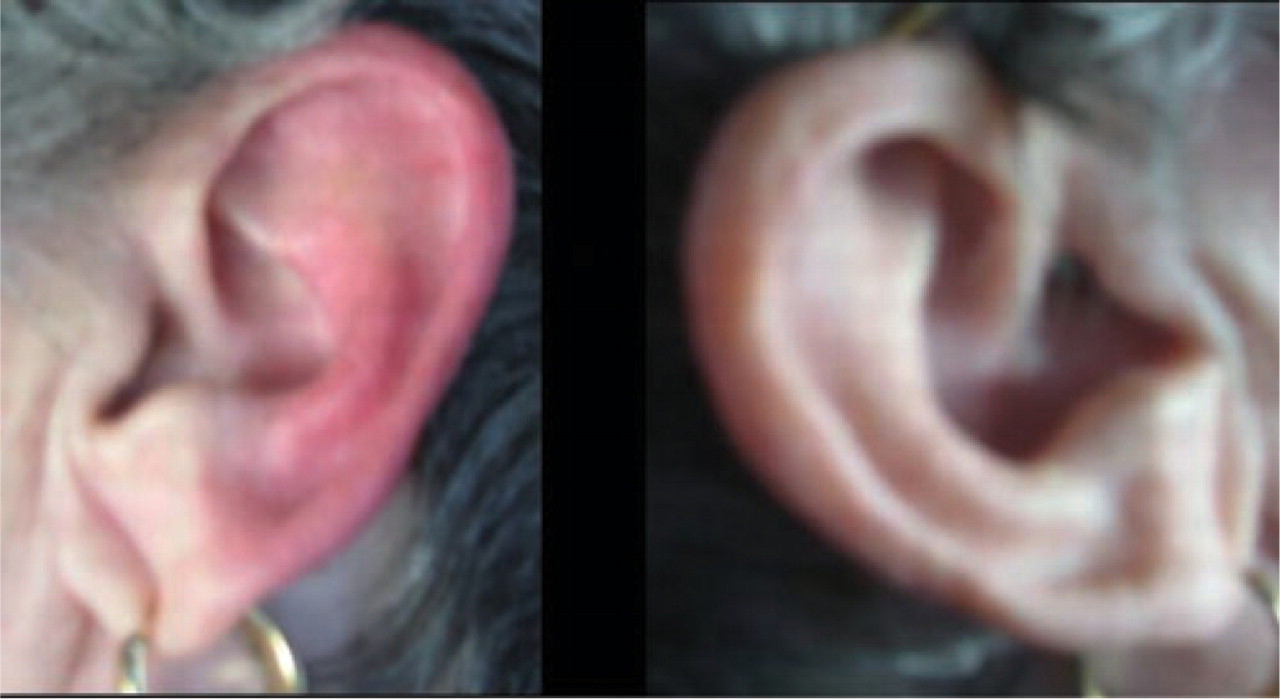
Erythema of left ear (patient 2) during episode.
Magnetic resonance imaging (MRI) of the brain and C-spine demonstrated a fusion of C1–C3 vertebrae with widening of the spinal canal at these levels. ENT and neurosurgical consultations found no additional pathology.
Based on her history and imaging findings, she was diagnosed with red ear syndrome. Consideration was given to treatment with anti-inflammatory medications. While on ibuprofen 400 mg/day the patient's attack frequency diminished dramatically from daily to bimonthly attacks. Given this significant improvement, she stopped taking gabapentin for facial pain. She has had no further recurrences of facial discomfort for 2 months after cessation of this therapy. The patient also stopped taking ibuprofen on a daily basis due to stomach upset and the treatment benefit has persisted.
Case 2
A 66-year-old female presented with a 5-year history of pain behind her left ear. The discomfort was initially episodic, occurring daily for 1–2 weeks, followed by periods of remission lasting months. Five years later, the pain had increased in severity with near daily symptoms in the late afternoon. About 50% of the time the pain was accompanied by a colour change in the left ear to a ‘bloody-red.’ No triggers for the onset of symptoms could be identified, but the discomfort was alleviated briefly by head movements. Prior to referral, the patient had started taking ibuprofen 400 mg in the evening which eliminated her attacks. Her past medical history was remarkable for progressive muscular atrophy of 13 years' duration, hypothyroidism and basal cell skin cancer.
Physical examination demonstrated a flaccid quadriparesis with profound wasting and weakness of upper and lower extremities, and tongue fasciculations. In addition, subjective impairment of pinprick and light touch sensation was noted behind the left ear as well as minimal left occipital nerve tenderness.
Multiple MRIs of the brain and upper cervical spinal cord were unremarkable, as was lumbar puncture done for investigation of motor neuron disease. Greater auricular nerve sensory conduction and trigeminal blink reflex studies were normal.
The patient was continued on ibuprofen and has had no relapses since starting the medication.
Case 3
A 58-year-old female presented with a 2-year history of recurrent daily attacks of red ear redness and discomfort. The symptoms began almost immediately after simultaneous root canals performed on two left mandibular teeth. During the procedure, the patient reported having her jaw opened uncomfortably wide for 4 h. Following the surgery, the patient developed TMJ pain as well as daily attacks of flushing, heat and redness of the left ear. In addition to the uncomfortable ear sensations, a third of the attacks were accompanied by erythema along the left maxillary region of the face. Each attack lasted from 30 min to 48 h and could be triggered by touching the ear, blow drying her hair and exposure to heat. The patient's past medical history was significant for episodic migraine without aura. At the time of presentation, she was on meloxicam, a non-steroidal anti-inflammatory drug, for osteoarthritis.
Physical examination demonstrated a left exotropia from childhood strabismus and a warm, red ear (Fig. 1).
Given the multiple triggers for red ear syndrome from the history, as well as a normal physical examination, neuroimaging was deferred. The patient was started on indomethacin 150 mg/day. Despite an initial reduction in frequency, the response was felt to be modest, waning over time, and the medication was discontinued. Botulinum toxin Type A injections subcutaneously along the pinna and a C2-facet injection of bupivicaine and corticosteroids were ineffective. The patient continues to experience symptoms.
Discussion
A variety of treatments have been employed for red ear syndrome. Propranolol, tricyclic antidepressants (amitriptyline and imipramine) and flunarizine have been reported to be partially effective. In a patient with TMJ dysfunction, a dental plate was reported to be curative (2, 4). In another case, surgical section of the C3 root resulted in disappearance of the ear pain without complete elimination of periodic erythema (2). In the cases associated with CPH, indomethacin was reported to be curative (9, 10). Local anaesthetic block of the second and third cervical roots abolished the sensation in one patient temporarily, but blockade of the auriculotemporal and posterior auricular nerves has been ineffective (2). Pizotifen, methysergide, facet joint denervation, occipital nerve and glossopharyngeal nerve sectioning have not been effective (2–12).
In two of the cases described above, ibuprofen led to resolution of the red ear syndrome. In neither case was a secondary cause of the red ear syndrome obvious. The third patient developed symptoms immediately after a traumatic dental procedure, after which she suffered from severe temporal mandibular joint pain for 3 weeks. Despite an initial and promising response to indomethacin, she ultimately failed to respond completely, the effect appeared to diminish and she discontinued the drug. She has subsequently failed treatment with botulinum toxin type-A injections into the left pinna and a left C-2 facet block.
These cases illustrate that, like most headache disorders, there are primary and secondary forms and while the pathogenesis of the red ear syndrome is not completely clear, its association with migraine and other trigeminal autonomic cephalgias has led to the suggestion that idiopathic cases might be due to an intrinsic dysregulation of the brainstem trigeminal-autonomic circuits rather than a local axon reflex (2). Support for this hypothesis comes not only from the co-occurrence of these disorders in the same patient, but also from the resolution of red ear syndrome when treatment is initiated for the coexisting headache disorder (e.g. indomethacin for CPH or β-blocker for migraine).
In the third patient, red ear syndrome appeared to be due to iatrogenic temporal mandibular dysfunction, and in such patients with secondary red ear syndrome the pathogenesis may indeed be different. The possibility that a local axon reflex might explain cases associated with TMJ dysfunction, especially when heat and touch provoke the symptom, has been raised before (2). Indeed, this patient's symptoms, unlike those of the two previous patients, were exquisitely sensitive to and provoked by heat and tactile stimulation. This of course was the rationale for trying botulinum toxin injections in this patient, since this neurotoxin has been shown to inhibit the release of vasoactive neuropeptides, including calcitonin gene-related peptide and substance P (14). Unfortunately, despite repeated injections on two separate occasions, the patient failed to respond.
These cases therefore illustrate and comfirm the following observations. First, red ear syndrome may exist as a primary trigeminal or cervical autonomic cephalalgia. Second, it may coexist with other rare trigeminal autonomic cephalalgias, indicating a similar underlying physiological substrate. Indeed, Lance and colleagues have proposed the term auriculo-autonomic cephalgia to illustrate the distribution of the pain and accompanying autonomic symptoms and signs (15). Finally, a secondary form may exist and, at least in the case of temporal mandibular dysfunction, the pathogenesis may be distinct, the triggers specific (heat/tactile stimulation) and the syndrome more resistant to treatment.
