Abstract
Introduction:
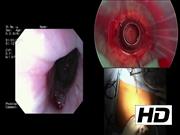
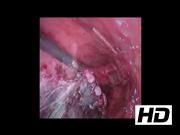
The endolaparoscopic transgastric approach allows minimally invasive access to luminally based benign or low malignant lesions. This is especially useful for lesions around the gastroesophageal junction (GEJ). 1 –3 This technique also allows minimally invasive access to the proximal stomach for reversal of vertical banded gastroplasty (VBG) also. 4 This video presents three separate applications of the endolaparoscopic transgastric platform, including a resection of juxta-cardiac gastrointestinal stromal tumor (GIST), proximal gastric endoscopic mucosal resection (EMR), and transgastric reversal of VBG.
Materials and Methods:
The patient is positioned in a modified Lloyd-Davies position with both arms out, under general anesthesia. The operation requires an endoscopist, a laparoscopist, and an assistant. The stomach is inflated using the gastroscope and transillumination of the anterior abdominal wall is used with needle localization to place the first port. An open cut down is used to find the anterior gastric wall and stay sutures are placed. A 12-mm balloon port is introduced under gastroscopic vision, into the inflated stomach. The gastroscope is then withdrawn into the esophagus and insufflation is maintained through the laparoscopic balloon port with high flow CO2 at 15 mm Hg. The procedure is completed depending on the specific application of the platform as detailed in the video. Transgastric ports are then converted to laparoscopic ports with closure using interrupted sutures or staples.
Results:
To date, 34 patients have undergone the described transgastric technique for resection of GIST. There were five complications (14.7%). Four had complications associated with postoperative bleeding, whereas one had a minor leak. The leak was caused by a technical problem and no air leak test was performed. Although reintervention was not required, it did prolong admission. Two out of the four bleeds required endoscopic intervention. There was no perioperative mortality. For GIST lesions, average tumor size was 42.0 mm and all resected margins were clear of tumor. Eighteen patients (75%) had adequate postoperative follow-up (average 88 months) with no evidence of recurrence or GEJ stenosis. Three EMR cases were completed and one case (33%) was complicated by bleeding that required endoscopic intervention. There were no leaks. Finally, nine cases of VBG reversal were performed with four cases of postoperative bleeding and two required endoscopic intervention. Again, there were no leaks and no perioperative mortality.
Conclusion:
The endolaparoscopic transgastric approach allows safe minimally invasive access to proximal luminally based lesions around the GEJ and VBG reversal. The procedure may be performed with standard laparoscopic and endoscopic setup.
No competing financial interests exist
.
Authors have received and archived patient consent for video recording/publication in advance of video recording of procedure
.
Runtime of video: 10 mins

Keywords
Get full access to this article
View all access options for this article.
