Abstract
Background:
Arteriobiliary fistula is a rare pathology and is often attributable to iatrogenic causes. Acute presentation is common because of shunting of high-pressure blood from the hepatic artery into the bile duct. 1 Treatment options include percutaneous endovascular intervention 2 and rarely surgical intervention, often performed through laparotomy. Minimally invasive surgical intervention is rarely applicable. We report a case of robotic repair for a choledochoarterial fistula.
Patient and Method:
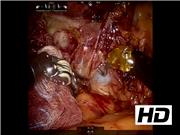
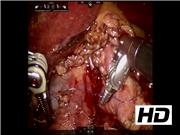
A 53-year old female was transferred because of gastrointestinal (GI) bleeding. Two weeks prior, the patient had undergone endoscopic retrograde cholangiography (ERC) for choledocholithiasis at an outside institution, but a large common bile duct (CBD) stone could not be removed. A plastic CBD stent was placed. The patient returned 10 days later with abdominal pain and recurrent GI bleeding. On abdominal CT angiogram, the proximal barb of the CBD stent was abutting, and possibly eroding into the right hepatic artery (RHA). A repeat ERC/endoscopy was performed and showed bright red blood and clot emanating from the ampulla, suggesting ongoing active arterial bleeding into the CBD. Based on the work-up, the indwelling CBD stent was in a false tract within the CBD wall and eroding or had penetrated the RHA. Endoscopic intervention was aborted. Owing to angulation of the RHA, percutaneous intervention with stenting was not feasible, and percutaneous intervention would have required coil embolization of the entire RHA. Surgical intervention was the next option. Since the patient was hemodynamically stable without hemodynamic support (blood pressure 140/85; pulse 85), a robotic approach to take down the fistula and repair of the arteriotomy was used. A robotic camera and three robotic instruments and one assistant port were used. The CBD was found to be markedly dilated because of intraductal blood and clot. The common hepatic artery was exposed for proximal control if needed. Distally, dissection of the retrocholedochal RHA revealed a choledochoarterial fistula between the anterior wall of the RHA and posterior wall of the CBD. During the dissection, a sudden gush of arterial blood was encountered with takedown of the fistula. Proximal control of the common hepatic artery led to hemostasis and the RHA puncture arteriotomy to be repaired with 4-0 Prolene. The arteriotomy was at the site of the fistula. Owing to friability of the bile duct tissue around the CBD, the opening in the CBD was not repaired. A fibrin glue was applied and a drain was placed. The CBD stone was removed by ERC postoperatively, and the CBD was re-stented through the true lumen. The patient recovered uneventfully and was discharged on postoperative day 6, with no further bleeding and a stable hemoglobin. On follow-up a few weeks later, the patient had no further bleeding. Endoscopic retrograde cholangiopancreatography was scheduled in 6 weeks to remove the stent.
Conclusion:
Iatrogenic extrahepatic arteriobiliary fistula is rare. With appropriate expertise and skills, robotic repair of choledochal RHA fistula is feasible and affords the patient the benefits of minimally invasive approach. This approach should only be performed in a hemodynamically stable patient. Based on our literature search, no previous reports document robotic repair of a choledochoarterial fistula.
No competing financial interests exist.
Runtime of video: 7 mins 48 secs

Get full access to this article
View all access options for this article.
