Abstract
Introduction:
Laparoscopic sleeve gastrectomy has gained increased acceptance for the treatment of obesity and its related metabolic complications. 1,2 Recently, single-incision laparoscopic surgery has evolved as one future trend of minimally invasive surgery providing the patient with almost invisible scars resulting in better cosmesis. 3 In this report, we describe how this minimally invasive single-incision laparoscopic surgical technique can be applied to sleeve gastrectomy without the use of any additional liver retraction device.
Materials and Methods:
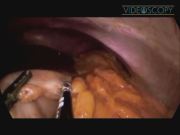
Our technique was exclusively performed on female patients, with a BMI of 35 kg/m2 to 45 kg/m2. Under general anesthesia, a 50-mm OCTO-Port® (AFS Medical) was inserted via a 4-cm vertical transumbilical incision, a pneumoperitoneum was established using continuous carbon dioxide insufflation. Using a 5-mm flexible grasper (Karl Storz) and a 5-mm Ligasure® (valleylab; Covidien), sleeve gastrectomy was started by dissection of the gastrocolic and gastrosplenic ligament, starting 6 cm proximal to the pylorus toward the angle of His. A 36F bougie was subsequently placed against the lesser curvature and used as a calibrating splint for the sleeve resection. The gastric sleeve was subsequently prepared using a Long Echelon Flex®, 60-mm, linear stapler (Ethicon Endo-Surgery; Johnson and Johnson). Reinforcement of the staple line and, in particular, of junctions of each staple firing was performed regularly by application of surgical clips (Ligamax; Ethicon). Finally, the transected stomach was removed directly through the port and the abdomen was closed using 0 Vicryl interrupted sutures. No intra-abdominal drains were used in our cohort.
Results and Conclusion:
A total of 50 patients underwent single-incision laparoscopic sleeve gastrectomy at our institution. No intraoperative or postoperative deaths occurred. The most significant complications were staple-line bleeding (n=2; 4%) and staple-line leakage (n=2; 4%), which were treated by relaparoscopy (n=3)/relaparotomy (n=1), abdominal lavage/drainage, clipping of the bleeding site, and oversewing of the stapleline. The physiological and anatomical reason in supporting the efficacy of sleeve gastrectomy is attributed to the reduction of total gastric capacity; subsequently, all patients in our cohort experienced a significant excess weight loss over time. Single-incision laparoscopic sleeve gastrectomy is a feasible and safe minimally invasive laparoscopic procedure for patients with morbid obesity.
None of the authors involved in the manuscript preparation have any conflicts of interest toward the manuscript itself, neither financial nor moral conflicts. In addition, none of the authors received support in the form of grants, equipment, and/or pharmaceutical items
.
Runtime of video: 6 mins 20 secs
The first two authors contributed equally to this work.


Keywords
Get full access to this article
View all access options for this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
