Abstract
Introduction:
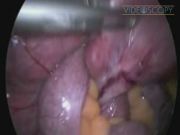
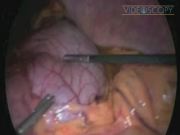
This video shows laparoscopic management of small bowel obstruction following Roux-en-Y gastric bypass for obesity. Gastric bypass mortality could reach 0.87%. 1 Fifteen to thirty percent of patients will visit the emergency room or require admission within 3 years of gastric bypass, and abdominal pain is the primary complaint in over half of these cases. 2 Internal herniation was reported at 4.7% when nonclosure of mesenteric defects was attempted. 3 Internal herniation was the cause of obstruction in this case. Late small bowel obstruction is either due to internal herniation, twist, stricturing, adhesions, or other causes unrelated to the gastric bypass such as tumors and foreign bodies.
Methods:
This was a 49-year-old female patient who underwent Roux-en-Y gastric bypass (it was a proximal type/the gastric bypass was performed using 70 cm of the biliopancreatic limb and 120 cm of the Roux limb and the mesenteric defects were closed using the Ethibond stitch) for obesity and type 2 diabetes, which have been cured, in 2009 and was presented on February 2013 with a 6-hour history of acute severe abdominal pain, nausea, and vomiting. The abdomen was distended and tender associated with tachycardia, hypotension, and tachypnoea. Initial blood tests showed increased inflammatory markers, high urea, compensated metabolic acidosis, and a high lactate level at 2.7 mM. Acute small bowel obstruction was confirmed by a CT scan. An urgent laparoscopic exploration was undertaken and an internal herniation of small bowel and twisting of jejunojejunostomy were diagnosed. The twisted bowel around the junction was blue, however, it regained normal color after reduction. It was a complete obstruction of the biliopancreatic limb, which was not draining through the efferent loop (alimentary loop) causing the obstructed loop syndrome; as a result, the stomach was hugely distended and impending to perforate and a reactionary turbid fluid was seen around it. The afferent Roux limb was also completely obstructed, but decompressed by vomiting. The viable alimentary bowel was reduced and the junction was untwisted. Closure of the hernia defect using Ethibond stitch was undertaken. The distended stomach was decompressed by aspirating 2 L of gastric fluids using the Veress needle, which was introduced through the left hypochondrium.
Results:
The patient developed postoperative atelectasis and was hospitalized for 7 days before being discharged in good health.
Conclusion:
Acute bariatric emergencies can be managed by the minimal access approach. Early diagnosis and involvement of bariatric team is crucial for the appropriate timing of the operation, avoiding major resection, and prevention of mortality and severe morbidity.
The authors have no conflicts of interest and no financial ties to disclose.
Runtime of video: 5 mins

Keywords
Get full access to this article
View all access options for this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
