Abstract
Treatment of large symptomatic gastric lipomas often involves gastric resection. However, this operation is associated with a disturbance of normal physiology and postgastrectomy syndrome. Details of laparoscopic transerosal enucleation of a large symptomatic gastric lipoma are presented in a video. This minimally invasive technique allowed a fast postoperative recovery and maintenance of gastric anatomy and function.
Introduction:
Management of gastric lipomas is an issue of debate. For smaller lesions endoscopic resection is a safe and effective option. For larger and symptomatic lipomas the treatment commonly involves partial gastrectomy with open or laparoscopic approach. 1 –3 However, this operation may be associated with a disturbance of normal physiology and postgastrectomy syndrome. Pylorus preserving-gastrectomy has been suggested to minimize the postgastrectomy problems; nevertheless, delayed gastric emptying has been observed after this operation. 4 More recently, wedge resection using an endoscopic linear stapler has been proposed for gastric gastro intestinal stromal tumors (GIST); however for tumors located in the antrum, there is a high risk of narrowing the gastric lumen. Isolated cases of enucleation with open approach have been reported. 5
Case Report:
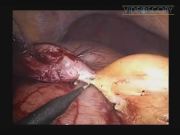
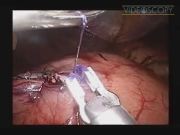
In the video, we report details of a laparoscopic transerosal enucleation of a large symptomatic gastric lipoma in a 75-year-old man. Preoperative endoscopy computed tomography scan and echoendoscopy revealed a submucosal lipoma of 6 cm in diameter, located on the gastric antrum. The patients underwent a laparoscopic enucleation of the lipoma. With the patient in a prone position, a 10-mm trocar was placed in the sovraumbelical region, and a 30° angled video scope was introduced; under direct visualization, two additional trocars were placed in the right (5 mm) and in the left pararectal spaces (10 mm). After exclusion of any other abdominal lesion, the greater omentum was partially dissected near the great curvature. A transverse, 4 cm long, incision was made through the serosa and muscularis layers of the anterior antral wall, just over the lesion. The lipoma was dissected and enucleated with the cautery hook and scissor without an incision of the mucosa. After the lesion was entirely freed, it was placed in a retrieval bag for extraction trough the sovraumbelical incision. Gastrotomy was closed with a running Vicryl suture. The postoperative course was uneventful and the patients are now asymptomatic at 12 months follow-up.
Conclusion:
This minimally invasive approach satisfied the growing demand for less invasive surgical procedures allowing a fast postoperative recovery, low level of postoperative pain with function-preserving surgery, and no postgastrectomy problems.
No competing financial interests exist.
Runtime of video: 3 mins 5 secs

Get full access to this article
View all access options for this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
