Abstract

Clinical History and Physical Examination:
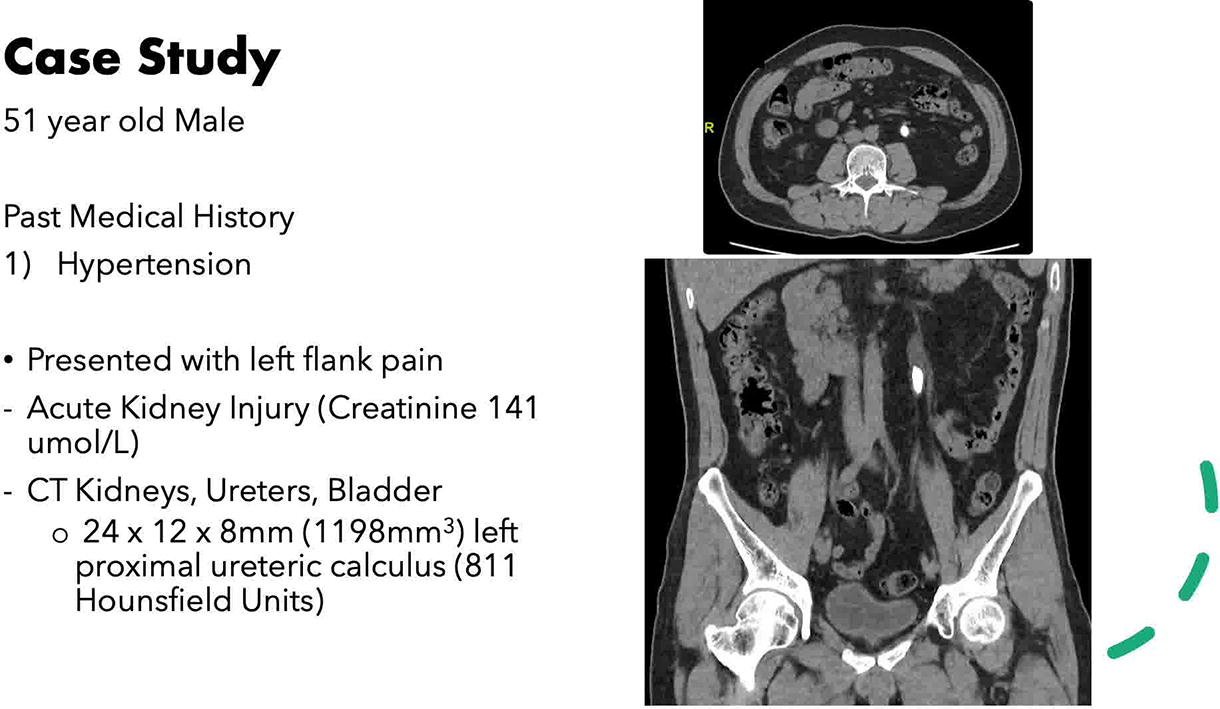
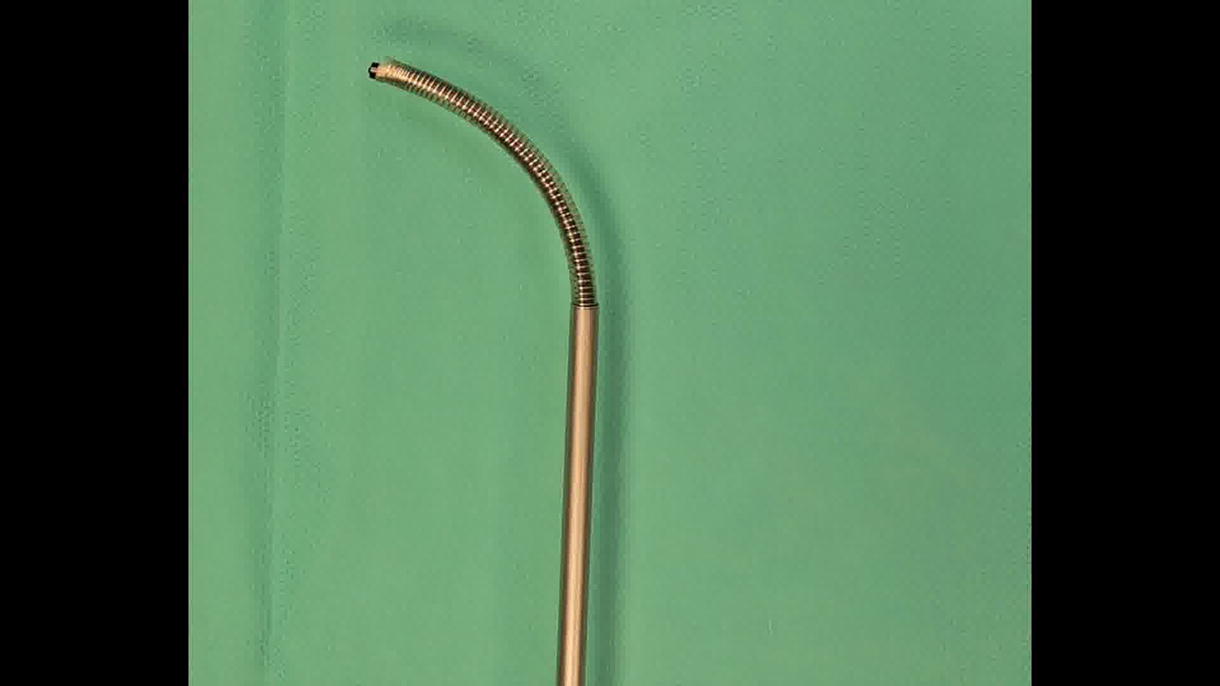
We demonstrate a novel technique utilizing a flexible and navigable suction ureteral access sheath (FANS) in an antegrade fashion for proximal ureteric stone lithotripsy. We present a 51-year-old gentleman who was admitted for left flank pain with renal angle tenderness on examination.
Diagnosis:
Computed tomography (CT) imaging revealed a 1198 mm3 L4 proximal ureteric stone.
Intervention:
As initial attempts at retrograde and percutaneous antegrade advancement of guidewires past the impacted proximal ureteric stone were unsuccessful, an 8 Fr percutaneous nephrostomy tube was inserted. In view of acute kidney injury, staged surgery was planned using an antegrade approach due to anticipated difficult retrograde access to the stone. A mini percutaneous nephrolithotomy (mPCNL) 15/16 Fr sheath, with antegrade use of a 12/14 Fr 40 cm FANS, and an 8.7 Fr flexible ureteroscope to steer the access sheath to the proximal edge of the stone. This was due to the rigid 12 Fr nephroscope not being able to visualize the calculus, despite maximal torque. Lithotripsy was then performed using a pulsed Thulium:YAG laser together with FANS suction.
Follow-Up/Outcomes:
At the end of surgery, there were no residual fragments radiologically or endoscopically. Laser ablation efficiency was 0.08 mm3/J. Visual inspection showed no ureteric injury. A 7 Fr 26 cm ureteric stent was placed, and a tubeless exit strategy was adopted. The patient was discharged within 24 hours with no complications. CT on postoperative day 18 demonstrated that the left ureter was stone-free. The outcomes of this technique should be further evaluated in future larger-scale studies.
Author Disclosure Statement:
Olivier Traxer is a consultant for Karl Storz, Coloplast, IPG Photonics, and Rocamed. Frédéric Panthier is a consultant for Dornier. Etienne Xavier Keller is a speaker and/or consultant for Coloplast, Olympus, Ambu and Boston Scientific. The remaining authors have nothing to disclose.
Patient Consent Statement:
Authors have received and archived patient consent for video recording/publication in advance of video recording of the procedure.
Runtime of video: 5 mins.
Get full access to this article
View all access options for this article.
