Abstract
Clinical History:
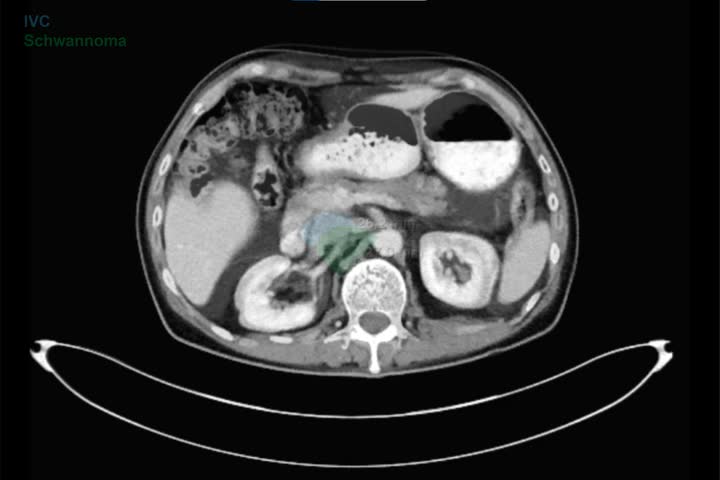
The patient is a 53-year-old man who presented to gastroenterology with complaints of abdominal pain. Endoscopy returned negative; however, CT of the abdomen demonstrated a right-sided heterogenous hypodense 2.6 × 2.7 cm retroperitoneal mass posterior to the inferior vena cava at the level of the renal hilum. PET CT demonstrated increased fluorodeoxyglucose avidity in the right retrocaval area with no evidence for metastasis. The case was then reviewed by surgical oncology and surgical excision was determined to be the best approach. Urology was ultimately consulted given the mass's retroperitoneal location.
Physical Examination:
Vitals were within normal limits and the physical examination was benign, including abdominal examination (soft, nontender, no palpable masses, no evidence of distention, rebound tenderness, or guarding).
Diagnosis:
Interventional radiology performed ultrasound-guided percutaneous biopsy, which stained positive for S100 and Sox 10, consistent with schwannoma.
Intervention:
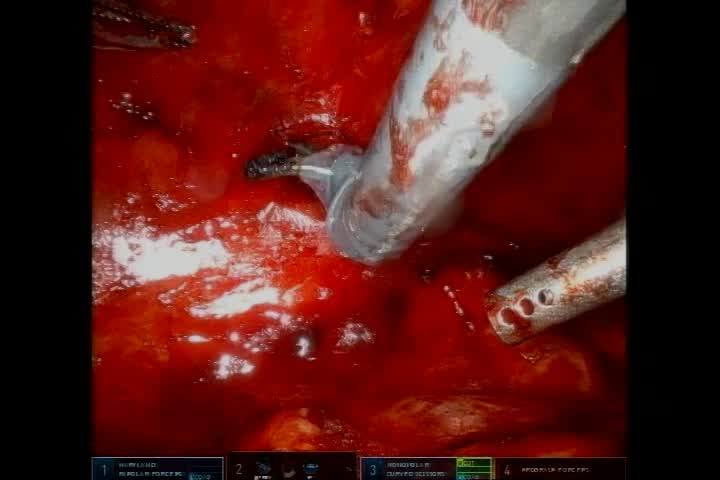
Robotic retroperitoneoscopic resection was determined to be the best approach given the mass's location. Urology was consulted given familiarity with the mass's location and the robotic retroperitoneoscopic approach. Upon entry into the retroperitoneum, a vertebral body osteophyte was encountered; however, careful attention to preoperative imaging and retroperitoneal landmarks enabled proper orientation and excision of the schwannoma with grossly negative margins.
Follow-Up/Outcomes:
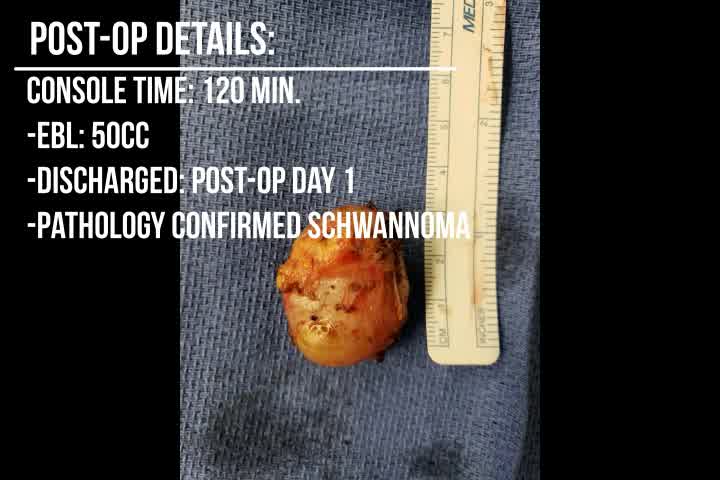
The console time was 120 minutes and estimated blood loss was 50 mL. The patient's postoperative course was uneventful, and he was discharged the next day. The patient was seen 6 months postoperative with no evidence of recurrence and has made a complete recovery.
No competing financial interests exist.
Patient Consent Statement:
Authors have received and archived patient consent for video recording/publication in advance of video recording of procedure.
Runtime of video: 5:00 mins
Get full access to this article
View all access options for this article.
