Abstract
Introduction and Objectives:
Ultrasound (US)-guided percutaneous nephrolithotomy (PCNL) and its advantages have been described extensively for the past few years, 1,2 but it has yet to achieve widespread acceptance. This resistance is attributed to inadequate training of urologists in the use of US, even though studies have shown the learning curve to be shorter with US-guided puncture as compared with fluoroscopy-guided puncture, 3 with comparable outcomes in both. 4 We intend to demonstrate certain risk reduction strategies to safely perform total US-guided PCNL.
Materials and Methods:
We performed this procedure in two patients. We then reviewed the steps of the procedure one by one to identify and demonstrate strategies to safely perform this procedure and overcome the challenges posed.
Results:
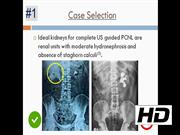
Both patients had single obstructing renal pelvic calculi <2 cm in maximum size, with moderate hydronephrosis. Procedure was completed in both patients in <60 minutes, with no complications. Postoperatively, both patients were discharged in 2 days. They had no residual fragments at follow-up. The risk reduction strategies proposed include selection of the correct case (ideal kidneys for this procedure are renal units with moderate hydronephrosis and absence of staghorn calculi) 5 ; placing a ureteral catheter with retrograde instillation of saline; correctly attaching the puncture attachment to US probe and using the needle guide on the monitor for puncture; confirming puncture by observing the needle tip on monitor, getting better orientation by moving the US probe and observing clear urine egress on withdrawing the stylet; confirming position of glidewire by observing it on monitor; and confirming effective dilatation by observing the tip of dilator and glidewire on US, following the direction of glidewire, tactile feedback provided on entering the pelvicaliceal system and observing urine egress from end of dilator.
Conclusion:
Total US guidance for puncture and dilatation in PCNL is safe and effective, with the advantage of eliminating the radiation exposure to the surgeon, patient, and health care personnel. However, careful patient selection is key, and keeping these risk reduction strategies in mind can lead to better outcomes.
We have received and archived patient consent for video recording/publication in advance of video recording of procedure.
No competing financial interests exist.
Runtime of video: 5 mins 58 secs
This abstract was presented at the 40th Congress of the Société Internationale d'Urologie (Virtual, 2020). All rights reserved. Reused with permission.
Music link:

Keywords
Get full access to this article
View all access options for this article.
