Abstract
Introduction:
Pediatric surgery began with single-incision flank surgery and has evolved to standard multiport laparoscopic and robotic approaches. To decrease visibility of incisions, hidden incision endoscopic surgery was developed. Recent technological advances with the single-port (SP) robot have allowed for the transition back to single-incision surgery.
Materials and Methods:
A 10-year-old girl with a history of bilateral vesicoureteral reflux presented to clinic after an episode of right pyelonephritis. Renal ultrasonography showed right hydronephrosis and Mag 3 Lasix renogram showed concerns of obstruction of the right ureteropelvic junction with estimated 27% function on the left and 73% on the right. Because of symptomatic right ureteropelvic junction obstruction and worsening hydronephrosis, the decision was made to perform the first SP robotic pyeloplasty procedure in a pediatric patient. The SP platform has one 2.5 cm, 4-channel port, a 12 × 10 mm articulating camera, and 6 mm multiwristed instruments, including the Maryland dissecting forceps, Cadiere forceps, wristed needle driver, and curved scissors.
Results:
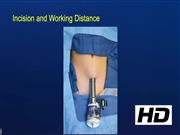
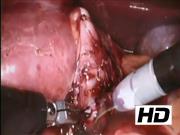
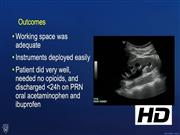
The port was placed in the Pfannenstiel line, and SP robotic pyeloplasty was completed without issues with space, triangulation, or articulation. There is loss of insufflation with use of laparoscopic instruments through an SP channel, as the seal on the port does not maintain a closed working system. The SP robot has since been utilized in seven patients with ages ranging from 23 months to 14 years. Six patients underwent robot-assisted dismembered pyeloplasty and one patient underwent robot-assisted Mitrofanoff using the da Vinci SP surgical system. Median operative time for all cases was 120 minutes, comparable with other robotic platforms. Estimated blood loss was <25 mL in all patients. All surgeries were completed through the SP without any intraoperative issues, need for extra ports, or conversion to alternate approaches. Minimal to no learning curve was present with the use of the SP system and observation from the approach did not differ from previous robotic systems. In older patients, no issues were present with instrument clashing, deploying the instruments, or achieving triangulation. Postoperatively, all patients were maintained on an alternating schedule of acetaminophen and ketorolac with no patients requiring opioid pain medications. All were discharged in <24 hours without complications. No postoperative adverse events were detected and all pyeloplasty patients had improvement with hydronephrosis. In addition, all parents were unanimously happy with the SP incision.
Conclusions:
SP robotic surgery is feasible in pediatric patients, but patient selection is fundamental to success. To optimize use, a 10-cm working distance must be maintained, limiting use to older children and teenagers. A shorter distance limits wristing of instruments as was experienced in the 23-month-old pyeloplasty. To help improve working space a Gel-Port can be utilized with the port retracted outside of the body to gain working space. In addition, needles can be placed into the abdomen after incision and before port placement to prevent loss of insufflation. Future development of the platform is needed to widen application to smaller patients.
Consent:
Consent was obtained from patient and parents to record this procedure.
Authors have received and archived patient consent for video recording/publication in advance of video recording of procedure.
Runtime of video: 4 mins 59 secs
No competing financial interests exist.
Get full access to this article
View all access options for this article.
