Abstract
Introduction and Objective:
To describe our technique and outcomes for the treatment of posterior urethral stenosis with the da Vinci Single Port (SP)® platform.
Methods:
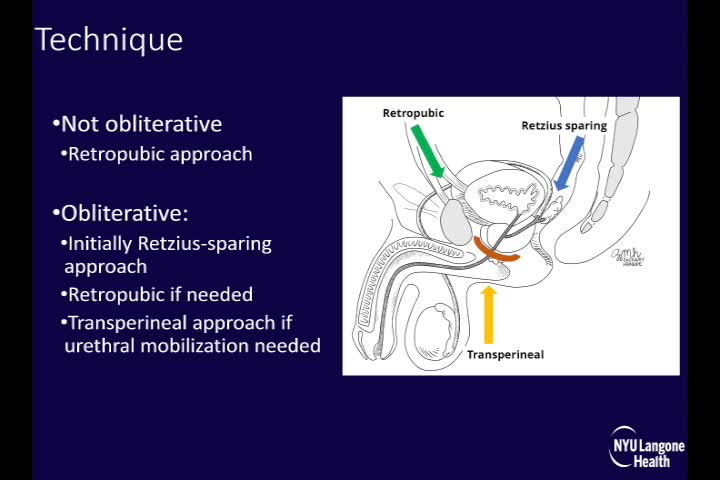
We retrospectively reviewed five patients who underwent SP robot-assisted laparoscopic posterior urethroplasty (SPRALPU) by a single surgeon from October 2018 to January 2019. Compared with multiport robotics, the SP robot allows for improved exposure and less instrument clashing in the deep pelvis. Variables included patient demographics, diagnosis and etiology, prior interventions, intraoperative variables, functional outcomes, and complications. Success was defined as passage of a 17F flexible cystoscope or absence of urinary symptoms. The operative technique involves SP port placement at a periumbilical location for transabdominal mobilization of the bladder neck and urethra. Cystoscopy is used to identify the level of the urethral stenosis. The stenotic segment is excised and the anastomosis completed using either excision and primary anastomosis or Y-V plasty. Combined abdominoperineal approach may be used for distal urethral mobilization to reduce tension.
Results:
The mean age was 64.8 years (range 51–77). Posterior urethroplasty was performed for vesicourethral anastomotic strictures (VUAS) (n = 1), VUAS with rectourethral fistula (n = 1), bladder neck contracture (BNC) (n = 1), BNC with bulbar urethral stricture (n = 1), which were caused by prostate cancer treatment (brachytherapy, radiation therapy, and prostatectomy), and prostatic urethra false passage (n = 1) because of traumatic intermittent catheterization in a patient with neurogenic bladder. Prior interventions included endoscopic balloon dilatation, urethral incision under direct vision, and Foley catheter placement. Four patients underwent SPRALPU without open conversion. Mean operative time was 417 minutes, estimated blood loss 220 mL, and length of stay 5.2 days. There were no intraoperative complications, although one case required open conversion because of SP robot failure; however, surgery was subsequently completed robotically using the Xi robot. Postoperative complications included ileus (n = 2), small bowel obstruction (n = 1), deep venous thrombosis (n = 1), urinary tract infection (n = 3), hematuria (n = 1), urethrocutaneous fistula (n = 1), abscess (n = 1), and osteomyelitis (n = 1). Catheters were removed at a median time of 32.5 days. All cases had patent urethral anastomoses with a median follow-up of 2.5 months. No patients experienced de novo urinary incontinence.
Conclusion:
SPRALPU is a feasible approach to an otherwise difficult reconstructive procedure because of challenges in exposure.
No competing financial interests exist.
Runtime of video: 5 mins 15 secs
A version of this video was presented at the World Congress of Endourology, October 29––November 2, 2019, in Abu Dhabi.
Keywords
Get full access to this article
View all access options for this article.
