Abstract
Introduction:
Robot-assisted radical prostatectomy (RARP) is the reference surgical approach for treatment of localized prostate cancer. The main side effect may be a stress urinary incontinence. Different pelvic floor reconstruction's surgical techniques for continence improvement have been developed over the years. 1 The effectiveness of reconstruction of the posterior musculofascial plane is still controversial and several articles with various levels of evidence, including randomized control trials, challenge the efficacy of the different proposed techniques reporting controversial outcomes. However, to date posterior reconstruction of the rhabdosphincter as described, 2 or with a modified approach, is performed by >50% of all robotic surgeons. 3 As a matter of fact, different metanalysis reported significant functional advantages in the first 90 days after posterior reconstruction with low complications rates. 4 We present our initial robotic technique for musculofascial reconstruction of the posterolateral plane using the tendinous arch as support of the pelvic floor structures. This procedure was suggested by pelvic floor reconstruction in radical cystectomy in which peritoneal flap is anchored to endopelvic fascia. 5,6
Materials and Methods:
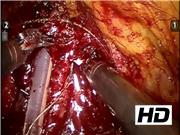
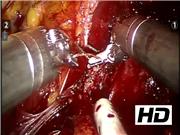
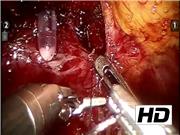
A total of 41 patients who underwent bilateral nerve sparing RARP from November 2017 to April 2018 were retrospectively evaluated. The surgical technique was developed and performed by a single surgeon (A.B.G.). In 20 patients was performed the lateral reconstruction of the musculofascial insertion of the Denonvilliers' attachment to the tendinous arch, whereas in the other 21 patients, no reconstruction was attempted. First step of the reconstruction begins with medial rectourethral muscle fixation to Denonvilliers' fascia; the second step is fixing the Denonvilliers' fascia laterally to endopelvic fascia through the support of the tendinous arch. The stitch is passed from the medial line to the lateral line, crossing superficially the tip of the neurovascular bundle (NVB), without clamping it. The NVB lies beneath the reconstructed plane that provides both a supplemental hemostatic action and is able to offer a support to the urethrovesical anastomosis providing a restoration of the fascial plane normally involved in urinary continence.
Results:
There was no statistically significant difference in age, body mass index, surgical pathology grade, and stage between the two groups. Our reconstruction technique requires a median surgical time of 8.2 ± 4 minutes, without any specific technique-related complications such as acute urinary retention, perineal pain, rectal perforation, bladder neck stricture, or perianastomotic urinary leakages. At 6 months follow–up, patients subjected to posterolateral reconstruction technique showed better rate and faster time to continence recovery.
Conclusions:
Our technique for reconstruction of the posterior musculofascial plane is feasible and reproducible. It, despite the small series of patients tested, could play a significant role working in synergy with the rhabdosphincter to ensure a better continence result. However, to date, it is not possible to assess whether continence advantage derives from the posterior reconstruction or to the lateral fixation; the superiority of this technique over the traditional posterior reconstruction is undefined yet. Longer follow-up and additional studies are warranted based on these encouraging results.
Contributorship Statement:
All authors equally contributed to the planning, conduction, and reporting of the work described in the video. Dr. Scarcella recorded and edited the video and prepared the article draft for the abstract with important intellectual input from Prof. Galosi, Dr. Dell'Atti, Dr. Maselli, and Dr. Leone. The surgical technique is Prof. Galosi's surgical innovation for musculofascial reconstruction of the posterolateral plane using the tendinous arch as support of the pelvic floor structures. All authors approved the final video and abstract article.
The authors have no direct or indirect commercial financial incentive associated with publishing the article and have no recognized financial or commercial interests.
Authors have received and archived patient consent for video recording/publication in advance of video recording of the procedure.
Runtime of video: 4 mins 48 secs
Get full access to this article
View all access options for this article.
