Abstract
Introduction:
Primary urothelial carcinoma of the upper urinary tract accounts for ∼5% of all renal and urothelial malignancies. Although relatively uncommon, the incidence of upper tract transitional cell carcinoma (TCC) appears to be slowly increasing. Although alternative therapies, such as endoscopic ablation/resection and segmental ureteral resection, have been adopted, radical nephroureterectomy is considered the ideal treatment for upper tract TCC.1 Upper tract TCC is frequently multifocal, has a higher rate of ipsilateral ureteral recurrence, is often associated with higher grade disease, and, therefore, carries a poorer prognosis compared with bladder TCC. Thus, in the presence of a normal contralateral upper tract, complete removal of the ipsilateral kidney, ureter, and bladder cuff remains the gold standard treatment for large, high-grade, or invasive TCC.2 The procedure may be undertaken open or laparoscopically. The “standard” laparoscopic nephroureterectomy (LNU) technique has not been defined and continues to evolve. Variations include utilization of a pure laparoscopic technique vs a hand-assisted technique, transperitoneal vs retroperitoneal, and a myriad of approaches to deal with the lower ureter.3 Indeed, the issue of the most appropriate oncologic management of the lower ureter and bladder cuff has been the most debated and controversial aspect of this operation since McDonald et al. attempted to lessen surgical morbidity by advocating endoscopic resection of the distal ureter in 1952.4 Irrespective of the adopted technique, the challenge is to ensure adherence to principles of reproducibility of results, patient safety, and oncologic outcomes. We present a series of 12 patients with upper urinary tract urothelial carcinoma treated with a new technique of a purely laparoscopic approach for en-bloc dissection of the distal ureter and bladder cuff during nephroureterectomy that avoid the disadvantage of open “distal ureterectomy and bladder cuff excision” and patient repositioning.
Materials and Methods:
Since 2016, patients with upper urinary tract urothelial carcinoma have been managed at our institution by purely LNU with bladder cuff using three trocars, including the camera trocar and the same position. Chart review identified 12 cases, including 3 ureteral tumors and 9 renal pelvis tumors. Baseline demographics collected included age at presentation, gender, location of the tumor indication, and preoperative serum hemoglobin and creatinine level. Perioperative data included operative time, estimated blood loss, blood transfusion, length of hospital stay, and duration of catheterization.
Results:
Twelve patients (eight males, four females; age range: 42 to 70 years; median: 60) with upper urinary tract urothelial carcinoma underwent surgery using this technique. Overall, all the patients (100%) had localized upper urinary tract TCC without metastasis (eight in the right side and four in the left side). Median preoperative hemoglobin and serum creatinine were 13.4 g/dL and 1.09 mg/dL, respectively. The operative time ranged between 90 and 180 minutes (median: 130). Mean estimated blood loss was 100 mL (range: 20–300). The patients were discharged from the hospital on the second to fourth postoperative day. Complications were seen in three patients (25%). One patient developed clinical symptoms of urinary leakage after slippage of Foley catheter because of faulty balloon. The catheter was reinserted and removed later on after cystogram showed no leakage. The second patient developed urinary tract infection and he was treated with i.v. antibiotic. The third patient developed increase in serum creatinine level up to 3 ng/dL and he was treated conservatively with i.v. fluids. Overall, 33% of the patients harbored pathologic T3 disease. Lymph node invasion was present in no patients (0%) with a median number of 13 lymph nodes removed. All patients received intermediate unit care postoperative support and started regular diet on day 0. All patients were transferred to floor on day 1 postoperation. Median length of hospital stay was 2.9 day (2–4).
Conclusions:
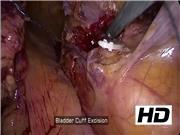
We describe an entirely laparoscopic removal of the kidney, ureter, and bladder cuff by a procedure that strictly adheres to oncologic principles (removal of the affected renal unit without opening the urinary tract), use only three ports (including the camera port) for accomplishing the whole procedure, and obviates the need for transurethral or open bladder cuff excision as well as intraoperative repositioning of the patient. This technique is efficient, technically feasible, and adheres to the oncologic principles of radical nephroureterectomy with bladder cuff.
These studies were done using only institutional resources and all authors affirm that they have no competing financial conflicts of interest.
The authors have received and archived patient consent for video recording/publication in advance of video recording of the procedure.
Runtime of video: 9 mins 43 secs
Get full access to this article
View all access options for this article.
