Abstract
Introduction:
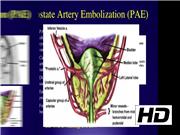
Prostate artery embolization (PAE) has gained popularity as an alternative minimally invasive technique for the treatment of benign prostatic hyperplasia (BPH). 1,2 However, there is limited data on the efficacy of PAE compared with standard treatments for BPH such as transurethral resection of the prostate or prostatectomy. A recent meta-analysis reported that PAE demonstrates efficacy, but slightly less than standard treatments. 3 We propose that PAE may be used in conjunction with surgery for BPH as a risk reduction strategy to minimize adverse perioperative events in high-risk patients. This video shows the PAE procedure with subsequent robotic simple prostatectomy (RSP) in a chronically anticoagulated Jehovah's Witness for bladder outlet obstruction secondary to BPH. We also report our institutes' initial experience of using PAE as an alternative to surgery for the treatment of BPH in high-risk patients. To our knowledge, we report the first multidisciplinary use of PAE before RSP to reduce perioperative bleeding risk in a high-risk surgical patient.
Materials and Methods:
PAE was performed on 11 patients (mean age 72.2 years) at a single academic institution. One of the patients was elected for RSP as definitive surgery to achieve immediate effect and PAE was used before surgery. Indications included refractory lower urinary tract symptoms (LUTSs), urinary retention, and gross hematuria. Urology evaluation included cystoscopy, preoperative and postoperative international prostate symptom score (IPSS), and postvoid residual (PVR) measurements during visits wherein no acute intervention was required. Patients felt to be unacceptable surgical candidates were referred to interventional radiology (IR) for PAE, which was performed under conscious sedation using femoral or radial artery access to embolize prostate arteries with gelatin microspheres to occlusion. Intraprocedural cone beam CT provided detailed vascular anatomy and confirmed embolization. Patients were discharged home the same or following day and were followed by both urology and IR. The patient who received RSP underwent surgery 1 day after PAE was performed and was subsequently followed after discharge.
Results:
Mean prostate size was 160.3 cc. Before PAE, mean IPSS was 24.5 with a quality of life (QoL) measurement of 4.7, and mean PVR was 456.4 cc. After PAE, mean IPSS was 8.1 with QoL of 2 and PVR was 143.2 cc. In the patient with PAE and surgery, preoperative and postoperative IPSSs with QoL were 21/6 and 3/0, respectively. His PVR also improved postoperatively from 350 to 124 cc. He underwent an uneventful RSP with console time of 189 minutes and estimated blood loss of <100 mL. All patients reported resolution of hematuria and improvement in LUTS in follow-up (mean 4 months). There were no major (Clavien >2) complications.
Conclusions:
Use of PAE before RSP is a feasible risk reduction strategy in high-risk patients to mitigate blood loss. PAE can also be used in patients who cannot undergo definitive surgery for BPH for resolution of LUTSs. Preoperative PAE could potentially be offered to other high-risk patients requiring complex surgery for BPH, regardless of preferred surgical approach. Long-term follow-up of PAE with and without subsequent surgery is required.
Author(s) have received and archived patient consent for video recording/publication in advance of video recording of procedure.
No competing financial interests exist.
Runtime of video: 9 mins 50 secs

Keywords
Get full access to this article
View all access options for this article.
