Abstract
Introduction:
Many different endoscopic techniques for ureterocele puncture have been described, including use of laser or Bugbee electrode with one large incision or many small holes. Puncture risks potential perforation through the bladder and intraperitoneal complications. Here we describe the novel Scissor Ureterocele unRoofing Endoscopic (SUuRE) technique and present our experience.
Materials and Methods:
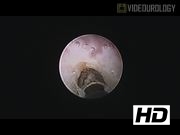
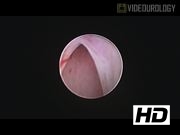
We performed a retrospective review of eight patients, seven females and one male, treated with the SUuRE technique from June 2014 to August 2016. Data collected included gender, patient's age at time of surgery, manner of presentation to urology, birth history, antibiotic use, perioperative urinary tract infections (UTIs), findings from postnatal and postoperative ultrasonographs, findings from the initial and postoperative voiding cystourethrogram (VCUG), additional urologic imaging, operative technique, and additional urologic surgeries. Under general anesthesia, the patients were placed in lithotomy position. The 9.5F Wolfe offset cystoscope (Catalog No. 8626.431) or the 11F Stortz offset cystoscope (No. 27031F) is inserted into the bladder. The ureterocele is identified, followed by the uninvolved ipsilateral and contralateral ureteral orifices. If the opening to the ureterocele is readily identified, one blade of the 3F endoscopic scissors or the KARL STORTZ 5F endoscopic scissors (No. 27034S) is inserted and the scissors are used to splay the ventral wall of the ureterocele open. If the opening to the ureterocele is not readily identified, a 3F Bugbee electrode (No. 27770AA) is used to puncture the ventral wall along the inferior aspect. The Bugbee electrode is then exchanged for the scissors that are used to open the ventral wall of the ureterocele. The cystoscope is then advanced into the ureterocele to identify the ureteral orifice that subtends it. Blood loss is minimal, no further electrocautery is needed.
Results:
The SUuRE technique was performed at a mean age of 6 months (range 1–11 months). Seven (87.5%) patients presented with prenatal detection of hydronephrosis and ureterocele, one (12.5%) patient presented with a febrile UTI. All patients were on antibiotic prophylaxis throughout the surgery. Seven of the eight patients had duplex systems and ectopic ureteroceles. Seven of eight patients (87.5%) had ipsilateral upper pole hydronephrosis preoperatively, one patient had an ipsilateral multicystic dysplastic kidney. No patient had vesicoureteral reflux (VUR) into the ipsilateral upper pole, three patients (37.5%) had VUR into the ipsilateral lower pole, and two (25%) patients had VUR into the contralateral renal unit at presentation. On postoperative imaging, all of the ureteroceles were completely decompressed. After unroofing, the ipsilateral hydronephrosis resolved in one patient, decreased in three patients, and remained stable in three patients. Of the three patients with pre-existing VUR (average grade = 4.2), reflux persisted but was downgraded (average grade 2.7). One patient developed contralateral de novo VUR (grade 3/4) and three patients developed ipsilateral upper pole de novo VUR (grades 2, 3, and 4). Contralateral VUR resolved in one patient. Two patient's VCUGs are pending. No perioperative complications have been noted.
Conclusions:
Ureterocele puncture can be performed in many ways: cold knife, Bugbee electrode, YAG:Holmium laser, one puncture, or multiple punctures. The SUuRE technique provides another highly effective, even safer tool in the armamentarium of ureterocele treatment.
No competing financial interests exist.
Authors have received and archived patient consent for video recording/publication in advance of video recording of procedure.
Runtime of video: 2 mins 44 secs

Get full access to this article
View all access options for this article.
