Abstract
Introduction:
Bladder cancer represents 3% of all cancers and 7% of cancer deaths in the United States. 1 A majority of bladder cancer is treatable at an early stage. 1 However, radical cystectomy with urinary diversion is required for muscle invasive disease. 1 Traditionally, an ileal conduit is used; however, this has significant quality-of-life (QOL) changes. A neobladder can spare some of the QOL changes. All neobladders must use detubularization, double folding, creation of a spheroid shape, and efficient evacuation. 2 Pure intracorporeal robot-assisted laparoscopic technique has been recently developed with a select number of high-volume centers utilizing various operative and neobladder techniques. 3 –5 Recently, the robotic Ves.Pa neobladder was described in a human pelvic model. 6 We present our step-by-step process of the robot-modified Ves.Pa neobladder.
Materials and Methods:
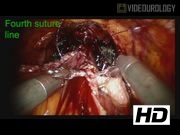
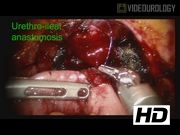
The modified robotic Ves.Pa neobladder was completed using the da Vinci SI surgical system. Cystoprostatectomy was completed as described previously. 7 A 45-cm segment of bowel 20 cm from the ileocecal valve was selected for the neobladder. The urethro-ileal anastomosis was completed 15 cm from the distal edge. Detubularization was performed. The other edge of bowel is then rotated and anastomosed to the edge at the location of the urethro-ileal anastomosis. All suture lines are completed with 3-0 V-loc suture into the final modified Ves.Pa formation. A suprapubic tube is not routinely placed due to the inability to anchor it to the abdominal wall when the abdomen is distended with the pneumoperitoneum, and this raises the possibility of an intraperitoneal urine leak occurring at the time of its removal. Uretero-ileal anastomosis were performed using a 4-0 monofilament absorbable suture on an RB-1 needle in a continuous manner as described by Bricker. 8 We chose not to place ureteral stents as there is minimal dissection of the ureters and no crossover of the left ureter under the sigmoid mesentery, which preserves vascular integrity of the ureter and, we feel, reduces the risk of stricture.
Results:
We reviewed the patients' characteristics, operative details, and perioperative courses in the two patients who have undergone robot-assisted laparoscopic radical cystectomy with pure intracorporeal modified Ves.Pa neobladder. These results were compared with other contemporary robotic neobladder series. 9 We demonstrate technical success with similar operative and perioperative results with the modified Ves.Pa neobladder. The mean operative time was 542 minutes. Patients were ambulating by postoperative day (POD) 1, advanced to a general diet by POD 2–3, and discharged by POD 4–5. No immediate postoperative complications were encountered. One patient had a urine leak at home due to an occluded catheter from mucous plugging. This was successfully managed with percutaneous drainage. All patients are currently voiding well.
Conclusion:
The robotic pure intracorporeal modified Ves.Pa neobladder is a technically feasible operation and may be easier to perform compared with other neobladders. Initial experience suggests operative time, and perioperative outcomes are similar to other robotic techniques.
No competing financial interests exist.
Runtime of video: 10 mins

Get full access to this article
View all access options for this article.
