Abstract

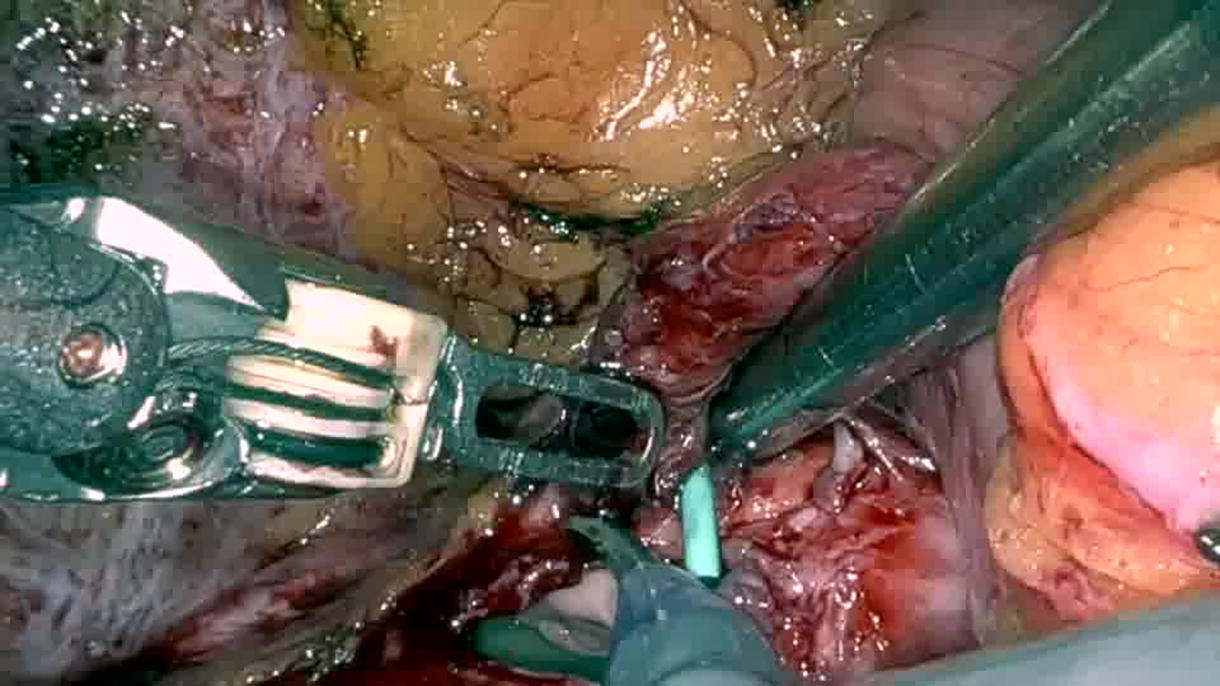
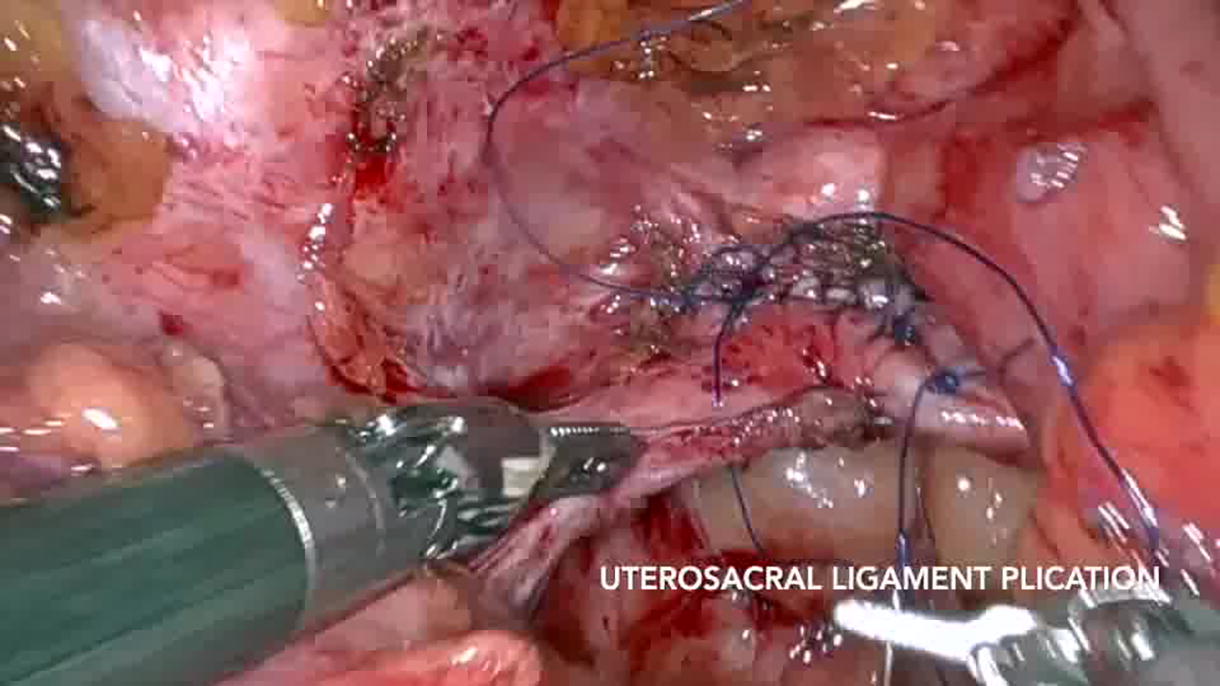
Neobladder-vaginal fistula (NVF) poses a complex surgical challenge due to the thin and less vascular neobladder wall. We present the case of a 37-year-old woman who developed a 2 cm NVF 3 weeks post robot-assisted radical cystectomy with intracorporeal orthotopic neobladder. Utilizing robotic assistance, meticulous dissection and repair were performed, employing a double-layer closure with omental interposition. The patient showed successful postoperative recovery with no recurrence of leakage at follow-up. This case underscores the efficacy of robot-assisted surgery in managing NVF, highlighting its benefits in reducing morbidity and improving surgical outcomes in complex cases.
Introduction:
Vesicovaginal fistula repair has steadily moved to minimally invasive approaches, namely laparoscopy and robot-assisted surgery. Robot-assisted surgery has revolutionized VVF repair by reducing the morbidity of the procedure, allowing for early recovery, minimal blood loss and better visualization of surgical planes. 1 Neobladder-vaginal fistula is a complex situation encountered in 2.7%–6.0% of women following neobladder formation. 2 While the principles of repair remain similar to VVF with an intact bladder, repair can be challenging as the neobladder wall is much thinner and less vascular than the walls of a normal bladder.
Materials and methods:
We share our experience of robot-assisted NVF repair in a 37-year-old lady following robot-assisted radical cystectomy with intracorporeal orthotopic neobladder.
Three weeks after the robot-assisted radical cystectomy, our patient presented with a continuous urine leak per vagina. CT urogram and flexible cystoscopy confirmed the presence of a 2 cm low-lying fistula between the neobladder (close to the urethrovesical anastomosis) and the vagina.
Results:
Because of a narrow and long vagina and the possibility of disrupting the neobladder integrity, we decided to proceed with robot-assisted repair. The fistula was looped with a ureteric catheter to enable intraoperative identification. Careful adhesiolysis and meticulous dissection aided by the articulating robotic hands helped us to carefully free the neobladder from the vagina and preserve the urethrovesical anastomosis. We performed a double-layer bladder and vaginal wall repair with omental interposition. A drain was placed that was removed on postoperative day 7. Foley catheter removal on postoperative day 21 with no leak on cystogram confirmed successful repair. The patient continues to remain completely dry on follow-up.
Conclusion:
Robot-assisted repair is becoming the gold standard approach for VVF repair. The benefits of robot-assisted surgery are even more pronounced in complex cases such as neobladder vaginal fistula by significantly reducing the morbidity associated with such a complex procedure and the results are equally good as an open approach.
The accompanying article provides a structured text breakdown.
We have ensured the video content aligns with the reviewed and accepted article. In addition, all narration is in English, and written informed consent for video publication has been obtained from each patient.
Conflicts of Interest Statement:
No conflicts of interest as signed by all authors. Form enclosed as separate attachment.
The video component details are as below.
Runtime of video: 7 min 41 sec.
Format: P4 playable on Windows PC.
Keywords
Get full access to this article
View all access options for this article.
