Abstract
Introduction:
Bladder paragangliomas (BP) (also commonly called bladder pheochromocytomas) account for 0.06% of bladder tumors, but may occur more frequently with familial syndromes, including the von Hippel-Lindau (VHL) syndrome and succinate dehydrogenase B (SDHB) mutations. Treatment is by surgical excision. Options include transurethral resection of bladder tumor (TURBT), partial cystectomy, and radical cystectomy. Therapy is dictated by the tumor size and location. We present a robotic-assisted partial cystectomy for treatment of a BP. We also performed a retrospective review of all cases of BP treated by the Urologic Oncology Branch at the National Institutes of Health (NIH) Clinical Center from 1989 to 2013.
Materials and Methods:
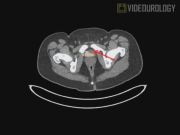
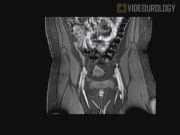
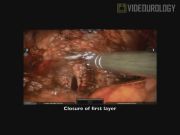
Our patient is a 14-year-old male with a history of VHL. He presented with a history of headaches upon micturition and night sweats. Previous surgeries were a robotic left partial adrenalectomy 8 years earlier and a right partial followed by right radical adrenalectomies 6 years earlier, all for pheochromocytoma. The presence of a bladder mass was confirmed by MRI and 123-iodine methyliodobenzylguanidine, and flexible cystoscopy revealed a submucosal left-sided bladder mass. Preoperative blockade was achieved with phenoxybenzamine and metyrosine. A robotic-assisted partial cystectomy was performed using a six-port transperitoneal setup. Following minimal lysis of adhesions, the bladder was taken down from the anterior abdominal wall. A flexible cystoscope was then advanced into the bladder and transmural illumination was used to aid in localizing the lesion. The mass was dissected circumferentially using electrocautery, and then sharply dissected off of the submucosa. Examination of the excision site was performed and leak testing using a cystoscope confirmed proper closure.
Results:
The patient had an uneventful recovery with complete resolution of symptoms. The Foley catheter was removed on the fourth postoperative day. Postoperative follow-up at 3 months demonstrated normal labwork and imaging. Review of previous cases of BP treated at our institution revealed eight patients diagnosed with BP during the study period. The mean age of diagnosis was 21.6 years (range 6–42 years). Five of the cases (62.5%) had VHL or SDHB. Familial BP tended to be smaller than sporadic cases (mean 4 cm3 [cc] vs. 33 cc tumor volume). BP detected in pediatric patients (<18 years old) were generally small (9.8 cc vs. 17.7cc for patients >18 years old). All patients with suspected BP received preoperative blockade. TURBT was sufficient for management in three of the patients (mean tumor volume 2.2 cc), partial cystectomy for four of the patients (mean tumor volume 11.6 cc), and a radical cystectomy was performed in one patient (tumor volume 63 cc).
Conclusions:
Surgical management of BPs include TURBT, partial cystectomy, and radical cystectomy and is largely dictated by the extent of disease. Robot-assisted partial cystectomy with cystoscopic lesion localization is an option in patients with small tumors, including pediatric patients. Regular follow-up is important in these patients as both local and distant recurrences can occur.
No competing financial interests exist.
Runtime of video: 7 mins 58 secs
Acknowledgment:
This research was made possible through the Intramural Research Program of National Institutes of Health (NIH), National Cancer Institute, Center for Cancer Research and NIH Medical Research Scholars Program, a public-private partnership supported jointly by NIH and generous contributions to the Foundation for NIH from Pfizer Inc., The Leona M. and Harry B. Helmsley Charitable Trust, and the Howard Hughes Medical Institute, as well as other private donors. For a complete list, please visit the Foundation website at
Keywords
Get full access to this article
View all access options for this article.
