Abstract
Introduction:
Placement of an artificial urinary sphincter is the gold standard for treatment of male stress urinary incontinence (SUI) with a high degree of patient satisfaction. 1 However, sphincter placement may be unattractive to patients because of potential infection, mechanical failure, and the desire to avoid a mechanical device. 2 Since 2006, the transobturator male sling has offered a new and minimally invasive treatment. We present a video reviewing the technique of sling placement and a review of our initial experience. Run time is 7 minutes and 13 seconds.
Materials and Methods:
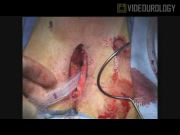
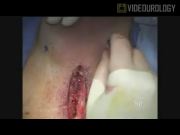
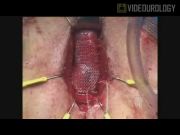
The video highlights important procedural points such as complete mobilization of the urethra from the perineal body to allow the urethra to be lifted proximally, marking the attachment of the perineal body to the urethra to mark the proximal location of the sling, passage of the needles to the apex of the intersection of the urethra and pubic arch, and tensioning of the sling under direct vision with cystoscopy for coaptation of the proximal bulbar urethra. A retrospective chart review was also performed of all transobturator male slings (AdVance Sling; AMS, Minnetonka, MN) placed from September 2008 to May 2010. All patients had preoperative confirmation of SUI by history and physical examination. Foley catheter was removed in the post-anesthesia care unit (PACU) after the procedure and was replaced for post-void residual (PVR) >200 cc. Patients with retention returned to the clinic in 3–5 days for a voiding trial. Success of the procedure was defined as resolution of leakage (no pads) or great improvement of leakage (rare or one pad) and lack of urinary leakage with stress maneuvers on postoperative physical examination. All other results were considered failures. Mean follow-up was 99 days.
Results:
Nineteen patients underwent sling placement. The average age was 68 years (45–85). Etiology of incontinence included 16 radical prostatectomies, 2 Holmium laser enucleations of the prostate, and 1 transurethral unroofing of a prostatic abscess. Mean pads used per day were 4 (1–8). Seventy-four percent (14/19) had success: 0 pads (8), 1 pad daily, or 1 safety pad occasionally (6). All patients went home on the day of surgery. Four failed the voiding trial and were discharged with a catheter. There were no occurrences of de novo irritative lower urinary tract symptoms, perineal pain, chronic urinary retention (>14 days), sling erosion, or sling extrusion.
Conclusion:
The transobturator male sling in the properly chosen patient provides a minimally invasive, low-risk, and successful procedure that can be performed with little difficultly as displayed in our video. Success of the procedure depends on proper patient selection, which includes documentation of SUI on physical examination or urodynamics, coaptation of the external urinary sphincter on cystoscopy, and mild to moderate urinary incontinence. In addition, surgical landmarks should be carefully utilized to ensure proper placement of the sling. Finally, patients must be counseled to refrain from heavy physical activity for the first 4–6 weeks to prevent sling loosening or dislodgement. Our experience has a short follow-up and a small sample size and, thus, further research into this area is warranted.
Gwen M. Grimsby: no disclosures; Christopher E. Wolter: meeting participant for Allergan and a lecturer for Coloplast.
Runtime of video: 7 mins 13 secs
Abstract was presented at AUA Western Section Meeting 2010, Big Island, Hawaii, October 2010.
Keywords
Get full access to this article
View all access options for this article.
