Abstract
Inroduction:
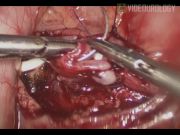
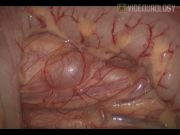
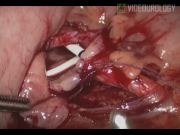
Laparoscopic dismembered pyeloplasty is considered as the gold standard for the management of pelviureteric junction obstruction. Conventional laparoscopic pyeloplasty through a transperitoneal approach mandates colonic mobilization for access to the pathological segment. In selected individuals (with minimal mesenteric fat), a transmesocolic approach may be attempted and colonic handling can be avoided. The transmesocolic approach offers several advantages. Colonic mobilization may be attended with a prolonged procedural duration, increased blood loss, possibility of iatrogenic insults, and delayed recovery. 1,2 With the transmesocolic approach, these problems can be reduced. We present a video demonstration of laparoscopic transmesocolic pyeloplasty. Port positions are depicted in the illustration. After achieving the pneumoperitoneum, the left renal pelvis and upper ureter were clearly visible through the mesocolon in this patient. This motivated us to embark on the transmesocolic approach. A transmesocolic window was created with selective generation of electrocautery. The ureter was dissected and traced upto the pelviureteric confluence. Periureteric and peripelvic adhesiolysis was performed using cold scissors, refraining from overvigorus usage of electrocautery. After delineation of the pathological segment, dismemberment was undertaken and pyelotomy was conducted. Ureter was adequately spatulated posterolaterally to ensure a wide anastomosis. Tension-free pelviureteric approxamibility was ascertained. Pelviuretreic approximation was undertaken using 4-0 polyglactin. The corner stitch was taken incorporating the apex of the spatulated ureter and the most dependent part of the pelvis. The opposite corner was approximated next followed by completion of the anterior layer of closure. The suture line was then upturned and attention directed to the posterior layer of pelviureteric approximation. A stent was inserted in an antegrade fashion. The redundant pelvis was excised and the posterior layer closure was completed by approximating the edges of the remaining pelvis. Hemostasis was achieved and a drain was inserted. The mesocolic window was closed.
Materials and Methods:
A 3-year-old male child was diagnosed with left pelviureteric junction obstruction after detailed evaluation. Retrograde dye delineation confirmed short segment left pelviureteric narrowing. Laparoscopic dismembered pyeloplasty through the transperitoneal route was contemplated. Operative and postoperative details were recorded. Patient was followed up at regular intervals. We analyzed the perioperative and long-term functional outcome of all patients who underwent transmesocolic pyeloplasty at our center.
Results and Conclusion:
Totally 41 patients underwent transmesocolic dismembered pyeloplasty at our institution. Thirty patients were of the pediatric age group and remaining were adults. The mean stricture length was 1.2 cm and a crossing vessel was present in seven patients. The mean duration of surgery was 70 minutes, mean blood loss was 100 mL. The mean time to start orals was 12 hours, mean duration of hospital stay was 36 hours, mean duration of follow up was 45 months. The success rate was 97.5%. Transmesocolic dismembered pyeloplasty is a safe and feasible procedure with less morbidity and satisfactory functional outcome. However, the transmesocolic approach may be practiced in individuals with short segment pelviureteric narrowing as the mesocolic window does not allow wide mobilization of the pelvis and upper ureter. Additionally, this approach is applicable in individuals with minimal mesocolic fat, which is typically encountered in children or thin individuals.
No competing financial interests exist.
Runtime of video: 4 mins 55 secs
Keywords
Get full access to this article
View all access options for this article.
