Abstract
Introduction:
Robotic surgery has revolutionized the field of urology. The use of robotics in urology is not limited to prostate surgery, and it is now being employed in renal surgery, reconstructive surgery, and even transplantation. Recently, we have seen the emergence of robotic and laparoscopic single-site surgery. We report on our technique and early outcomes of robotic laparoendoscopic single site (R-LESS) sacrocolpopexy.
Methods:
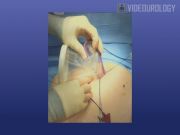
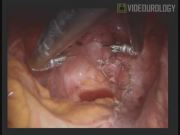
We queried our institutional review board–approved pelvic organ prolapse database for patients who underwent R-LESS sacrocolpopexy, and retrospectively reviewed the data. Preoperative evaluation consisting of a quantified pelvic examination using the Pelvic Organ Prolapse Quantification (POP-Q) system, standing voiding cystourethrogram, urodynamic testing, and demographic information were recorded. Perioperative data included surgical time, blood loss, conversion to standard robotic or open sacrocolpopexy, and length of stay. Key technical aspects include the following: (1) a single 4-cm peri-umbilical incision and insertion of the GelPoint laparoscopic system; (2) configuration of robotic ports in the GelPoint system to facilitate movement of robotic arms intracorporally; (3) end-to-end anastamosis clamp placed in the vagina at the start of the procedure and moved around by the assistant; (4) to allow maneuvering between robotic side ports a 30-degree up scope is necessary for this procedure; however, compared to standard robotic approach, this limits the field of view during promontory dissection; identification of the promontory is facilitated by tactile feedback from the suction tip introduced in the assistant port; (5) observation of the pelvis is enhanced by retraction of the small and large intestines away from the pelvic cavity, and temporarily tacked to the pelvic side-wall using a hem-o-lok® clip; (6) the marlex mesh, which has been measured, trimmed, and already secured with 2/0 Vicryl sutures on the back table, is introduced via the assistant port; (7) mesh fixation with absorbable sutures (2-0 Vicryl) that incorporate strong bites into the vaginal wall and occasionally the levator muscles; (8) mesh is secured to the anterior spinous ligament with 2/0 Ethibond nonabsorbable sutures; (9) to restore proper vaginal cuff support and avoid vaginal distortion, we do not place the mesh under tension but simply ensure that the mesh lays along the concavity of the sacrum in its prepared groove; (10) the peritoneum is closed over the mesh with a running V-loc suture; this peritoneal closure ensures prevention of bowel adhesions to the mesh; and (11) cystoscopy with administration of IV indigo carmine is performed to ensure no bladder or ureteric injuries.
Results:
From March 1, 2011 to September 1, 2011, four R-LESS sacrocolpopexies have been performed at our institution for advanced prolapse in thin patients (body mass index ≤25). In two patients, the pelvic exposure for one and the promontory access for the other failed, forcing a conversion to a five-port robotic procedure. All four patients were discharged home on postoperative day 1. Mean duration of follow-up since surgery was 6 months (3 to 9). No prolapse recurrence has been noted and significant improvement in POP-Q points was observed along with restoration of better quality of life for each patient.
Conclusion:
Although technically more challenging than the traditional robotic approach, R-LESS sacrocolpopexy is feasible when strict patient selection criteria are applied. Whether there is a strong cosmetic or pain advantage for this technique remains to be determined.
Benjamin E. Dillon: No competing financial interests exist.
Jeffrey A. Cadeddu: Ethicon Endosurgery: Consultant, advisory board, patent holder, sponsored research. Applied Medical: Speaker.
Philippe E. Zimmern: No competing financial interests exist.
Runtime of video: 4 mins 35 secs
Get full access to this article
View all access options for this article.
