Abstract
Introduction and Objectives:
Robot-assisted pyeloplasty results are comparable to those of open pyeloplasty, the standard option for ureteropelvic junction obstruction (UPJO), and it shows a less steep learning curve in comparison with laparoscopy. After nine transperitoneal standard retrocolic procedure, the video shows our first approach with a transmesocolic robot-assisted left dismembered pyeloplasty.
Material and Methods:
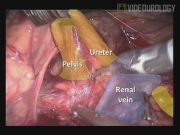
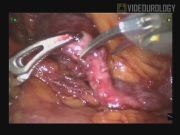
A 22-year-old man presented a bilateral UPJO. The symptoms and the worst grade of obstruction made the left side as first choice of correction. With a lombotomic (45°) position the robot da Vinci was placed on the back side of patient. Pneumoperitoneum was obtained with Verres needle and five transperitoneal trocar (three robotic and two laparoscopic for assistant) were inserted. After exposition of the left mesentero-colic space, and incision of the peritoneum, the ureter were identified and dissected. Identification and free dissection of the renal pelvis to obtain an adequate length to perform a tension free-repair. The renal pelvis was transected above the ureteropelvic junction (UPJ). The redundant renal pelvis was cut and the UPJ removed. After a lateral ureteral spatulation the excess pyelotomy was closed in running suture. A Double-J stent was antegradly inserted. The anastomosis was performed in multiple running 4/0 Monocryl suture.
Results:
Operative time was 115 minutes, blood loss <25 mL; catheter removal postoperative day 1; drain removal in postoperative day 2, discharge postoperative day 3; Double-J stent removal after 20 days. After 6 months in absence of left obstruction, we performed a contralateral right robot-assisted retrocolic pyeloplasty. At 2 years the diuretic scintigraphy showed absence of obstruction.
Conclusions:
Our initial results show that the transmesocolic robot-assisted pyeloplasty is safe and feasible. The direct approach to the left UPJ provides a good operative field and lower bowel manipulation. The robotic system makes easier reconstructive and suturing time and raises surgeon capabilities to work in a narrow space as the transmesocolic window. Larger series could confirm our first impression of effective operative time reduction.
No competing financial interests exist.
Runtime of video: 5 mins 52 secs
Keywords
Get full access to this article
View all access options for this article.
