Abstract
Introduction:
Robot-assisted laparoscopic partial nephrectomy (RPN) is a safe and effective minimal invasive approach to nephron-sparing surgery (NSS). 1 –3 In an effort to preserve functional renal outcomes, techniques have been developed to minimize ischemia time during NSS. These include zero ischemia technique with hypotension 4 and selective arterial clamping, 5 but both are technically demanding and complex. To facilitate selective clamping during robotic NSS, we utilized the daVinci fluorescence video system (Intuitive Surgical Inc.) to assist in identifying target arterial branches and assess tissue perfusion of target areas for resection. Herein, we report our technique and initial experience with video fluorescence angiography and its application in selective arterial clamping during RPN.
Materials and Methods:
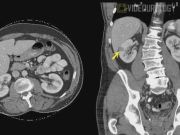
Included in this video are two cases in which we utilized the daVinci video fluorescence system with real-time indocyanine green (ICG) angiography during RPN. ICG is an optical contrast agent that emits fluorescence when excited by light at near-infrared wavelengths. Case 1 was via a retroperitoneal approach for a right posterior upper pole tumor measuring 1 cm. Case 2 was via a transperitoneal approach for a 2-cm tumor located in the lateral interpolar region of the right kidney. ICG (5 mg) was injected intravenously after selective clamping to assess renal perfusion and ischemia to target areas of resection.
Results:
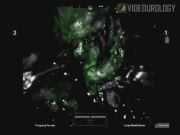
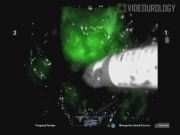
Case 1 demonstrates selective ischemia as a result of clamping only the apical segmental branch. This was verified with ICG angiography showing lack of perfusion and fluorescence at the target area. Reinjection of ICG after resection showed reperfusion of the tissue adjacent to the resection site. Preoperative and 2-week postoperative creatinine was unchanged at 0.90 mg/dL (glomerular filtration rate [GFR] > 60). In Case 2, ICG fluorescence revealed incomplete ischemia to the target area after selective clamping. This necessitated additional selective clamping of additional arterial branches supplying the resection bed. Preoperative creatinine was 1.0 mg/dL and 2-week postoperative creatinine was 0.9 mg/dL, signifying no change in GFR (>60). In both cases, tumor was excised in a near bloodless field with estimated blood loss of 25 and 100 mL, respectively, and total arterial clamp time of 9 and 19 minutes, respectively. In both cases, pathology revealed pT1a renal cell carcinomas with negative margins. There were no intraoperative or postoperative complications, and both patients were discharged on postoperative day 2.
Conclusion:
Integrated real-time video fluorescence and ICG angiography are key tools for selective arterial clamping during RPN. This novel technique contributes to selective clamping by allowing the surgeon to accurately and reproducibly confirm ischemia to target areas for resection. When applied, tumor excision can be carried out in a near bloodless field while keeping the remaining healthy renal parenchyma perfused. These initial results are promising, but further study is needed to assess patient selection and outcomes, including potential complications. Lastly, we acknowledge that dissection of renal arterial distal branches can be technically challenging, thus limiting this application to experienced renal surgeons.
Joseph Feliciano, M.D., and Yichun Chiu, M.D., have no competing financial interests. Michael Stifelman, M.D., is a consultant for Philadelphia Urology Associates and Vascular Technology, Inc., and a speaker for Intuitive Surgical, Inc., and Baxter Inc.
Runtime of video: 6 mins 52 secs
Get full access to this article
View all access options for this article.
