Abstract
Abstract
Introduction:
Paraganglioma (PGL) are rare neuroendocrine tumors arising from neural crest-derived chromaffin cells of the sympathetic and parasympathetic ganglia. Most abdominal PGL arise from sympathetic ganglia and are usually located adjacent to the aorta. Even if abdominal PGL are predominantly functional and hypersecrete catecholamines, causing secondary hypertension or typically paroxysmal hypertensive spikes, about 30% are nonsecreting.1,2 Surgery is the mainstay of treatment for abdominal PGL and represents the only chance of cure. Minimally invasive endoscopic techniques are currently the preferred surgical approaches in experienced hands, when it is anatomically feasible. 3
Materials and Methods:
We present a case of laparoscopic excision of a para-aortic PGL en bloc with partial adrenalectomy by transperitoneal approach in lateral position.
Results:
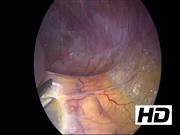
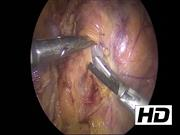
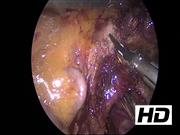
A 53-year-old woman underwent CT scan for right abdominal quadrants pain; a left para-aortic retroperitoneal solid hypodense 21-mm sized mass with significant enhancement and washout of contrast medium was incidentally discovered. The lesion was located between the left renal vein and the origin of the superior mesenteric artery, adjacent to the left adrenal gland. The arterial blood pressure was normal, and no symptoms such as facial flushing, excessive sweating, nausea/vomiting, or blurred vision were reported. Because of the radiologic suspicion of retroperitoneal PGL, a proper hormonal screening was performed; plasma neuron specific enolase (NSE), Chromogranin A, urinary 24-hour excretion of metanephrines, catecholamines, dopamine, and 3-methoxytyramine were in the normal range. An 18F-DOPA-PET MRI and 18F-FDG-PET CT scan showed a significant uptake of the mass for both radiotracers (SUV MAX 7.19 and 5.86, respectively). The genetic screening revealed absence of pathognomonic germline mutations in the genes responsible for hereditary pheochromocytoma and PGL syndromes. The video shows the main steps of the operation, starting from the mobilization of the left colonic flexure and the dissection of splenorenal ligament, allowing the fall of the spleen and pancreas tail medially. The plane separating the adrenal gland and the kidney from the tail of the pancreas was opened, allowing the view of the mass located between the left adrenal gland, the renal vein at the entrance of the inferior adrenal vein, adjacent to the superior mesenteric artery. The lesion was carefully dissected and removed en bloc with a partial adrenalectomy after the section of the adrenal vein, given the tight connection of these structures to the mass. During the procedure, some hypertensive spikes occurred.
Conclusions:
The procedure was finally uneventful; pathology report revealed a well-differentiated extra-adrenal pheochromocytoma (PASS score 1). At a 2 years follow-up, the patient is cured with absence of clinical, biochemical, and radiologic signs of recurrent disease.
Acknowledgments:
Authors have received and archived patient consent for video recording/publication in advance of video recording of procedure.
No competing financial interests exist
.
Runtime of video: 7 mins 56 secs
Get full access to this article
View all access options for this article.
