Abstract
Abstract
Introduction:
Pheochromocytomas are catecholamine secreting neuroendocrine tumors most often arising from the adrenal medulla. They can often present with symptoms such as anxiety/panic attacks, headaches, palpitations, and hypertension. For a functional tumor, biochemical confirmation can be completed with plasma or urine fractionated metanephrines. 1 Imaging findings consistent with pheochromocytoma include heterogeneous lesions containing cystic or hemorrhagic changes with variable size. The nodules are often rounded, well circumscribed, and often contain internal necrosis. Importantly, pheochromocytomas will have high Hounsfield units (>40) on CT scans, unlike other benign adrenal tumors that have Hounsfield units <10. 2 Patients who are young, have positive family history, or suspicion for multifocal or malignant disease should undergo genetic testing. Before surgery, it is essential to begin preoperative alpha blockade to prevent intraoperative hypertensive crisis. Beta blockers may be added after adequate alpha blockade has been established to control tachycardia. Laparoscopic adrenalectomy is standard of care for the treatment of benign functional and nonfunctional masses. The retroperitoneal approach has been developed as a more direct approach to the adrenal gland with the added benefit of avoiding the abdominal cavity.3,4 We describe a left retroperitoneoscopic adrenalectomy for a 5 cm pheochromocytoma.
Materials and Methods:
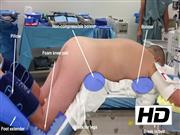
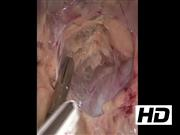
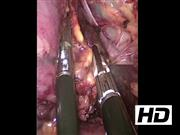
The patient is placed in the prone position with noncompressible bolsters supporting the hip and chest, which allows the abdominal contents to fall forward to develop the retroperitoneal working space. The back should be as flat as possible to prevent the hip from interfering with the laparoscopic instruments. The anatomical land marks are identified including the spine, the lateral border of the paraspinous muscle, and the inferior border of the 12th rib. The retroperitoneal approach requires higher insufflation pressure to achieve an adequate working space. Pressures up to 30 mm Hg are often used. The retroperitoneal fat is taken down from the posterior abdominal wall using a combination of blunt dissection and an electrothermal vessel-sealing bipolar device. The superior pole of the kidney should be identified and a plane developed to separate the adrenal gland from the kidney. Identification of the inferior phrenic vein can allude to the location of the adrenal vein on the left side. The adrenal gland should be handled carefully to avoid grasping the gland and tumor directly, but rather to grasp the periadrenal fat. This will help avoid disrupting the tumor capsule, which can lead to tumor spillage and recurrence. The adrenal vein is ligated with the electrothermal vessel sealing device (hemoclips are not routinely used in our practice). The tumor is removed through an encatchment bag and carefully morcellated to prevent tumor spillage. The surgical field is inspected with decreasing insufflation pressure to ensure hemostasis.
Conclusions:
Adrenalectomy through a minimally invasive retroperitoneal approach is a safe and effective method for treatment of large pheochromocytomas.
No competing financial interests exist involving the authors. We do not endorse the Ligasure device, but in our practice, we prefer to use a vessel sealing bipolar device in lieu of clips given the theoretical complication of clip displacement postoperatively.
Runtime of video: 7 mins 20 secs
Get full access to this article
View all access options for this article.
