Abstract
Abstract
Introduction:
The management of necrotizing pancreatitis with secondary infection has evolved from traditional open necrosectomy to a minimally invasive step-up approach, when feasible.1,2 Although the disease continues to have significant morbidity and mortality rates, a conservative treatment strategy is associated with fewer major complications. 3 This video demonstrates a retroperitoneoscopic debridement of pancreatic necrosis in a patient with severe necrotizing pancreatitis after failed percutaneous drainage.
Materials and Methods:
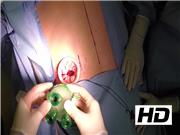
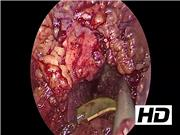
Under general anesthesia, the patient was placed in a prone position. A 2.5-cm incision was made inferior to the left 12th rib for insertion of a GelPOINT® Mini with two 5-mm trocars. An additional 5-mm trocar was placed laterally. The left kidney was mobilized and rotated medially, allowing access to the pancreatic necrosis anteriorly. After debridement of the necrosum, an additional large drain was placed.
Results:
The patient tolerated the procedure well without complication. Pathology report confirmed no viable tissue in the specimen. Postoperative CT scan showed a significant improvement in the infected collection. The patient's sepsis resolved without need for further debridement.
Conclusions:
Retroperitoneoscopic debridement is a viable strategy for treating infected pancreatic necrosis when percutaneous drainage has failed, and may result in decreased morbidity compared with traditional open necrosectomy.
The authors have no conflicts of interest to report
.
Runtime of video: 6 mins 5 secs
Get full access to this article
View all access options for this article.
