Abstract
Abstract
Introduction:
Ectopic parathyroid adenomas may occur in up to 25% of patients with primary hyperparathyroidism (PHPT), and in most of the cases can be excised by conventional neck exploration. However, 1–2% of these can present with “major ectopia” in the mediastinum, use to be responsible for persistent PHPT, and are very often not amenable to be excised by conventional approach. Parathyroid tissue at the aortopulmonary window (AoPW) is a rare condition (2.3% of all the mediastinal lesions) and the glands involved are usually inferior or supernumerary. Video-assisted thoracoscopic surgery (VATS) has evolved as a minimally invasive approach to solve these cases, avoiding the morbidity associated to classical approaches as sternotomy or anterior thoracotomy.
Materials and Methods:
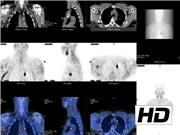
In this study, we present a patient with symptomatic PHPT in which the workup showed ectopic adenoma placed at the AoPW. VATS was used to successfully remove the diseased gland.
Results:
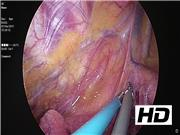
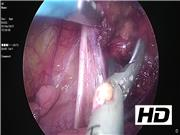
Management consisted on parathyroidectomy through VATS. Frozen section confirmed parathyroid adenoma (size 11 mm, weight 803 mg). Ten minutes after removing the adenoma, the intraoperative parathyroid hormone assay showed a 73.5% decay when compared with its previous pre-excision highest value, thus confirming the success of the procedure. One year after surgery, the patient is in good condition and remains with normal calcium levels.
Discussion:
Appropriate preoperative workup is mandatory to avoid persistent disease in primary hyperparathyroidism cases. For years, the classical approach to major ectopia used to be invasive (sternotomy or anterolateral thoracotomy) with a high rate of associated complications (29%). Later on, new and more conservative techniques were described as transcervical approach using the Cooper's retractor, 1 the Chamberlain's approach 2 that resected the chondral portion of the rib, and the subxiphoid approach. 3 Recently, Moreno et al. 4 described intercostal video-assisted mediastinal surgery to remove ectopic glands placed low in the anterior mediastinum. However, for those adenomas placed deep in the mediastinum, VATS has shown to be very safe and efficient. In the event of high complexity cases, we should use all the intraoperative tools at our disposal to perform a successful surgery.
Representation of any instrumentation within the video does not indicate any endorsement of the product and/or company by the publisher, the American Thyroid Association, or the authors. The authors have no disclosure.
Runtime of video: 6 mins 37 secs
Get full access to this article
View all access options for this article.
