Abstract
Abstract
Introduction:
Takotsubo cardiomyopathy (TC) is an acute reversible heart failure syndrome characterized by regional systolic dysfunction of the left ventricular (LV) apex and mid-ventricle. The cause is unknown, but it is well recognized that it is precipitated by stressful situations. 1 The clinical presentation is similar to an acute coronary syndrome but with normal coronary artery anatomy.1,2 Cardiac ventriculogram shows a characteristic ballooning of the apex of the left ventricle. 2 The pathophysiology of TC remains unknown; spontaneous multivessel coronary spasm, microcirculatory dysfunction, oxidative stress, and contractile dysfunction from catecholamine excess have been hypothesized as causes for TC.1–3 Although thyroid hormones (TH) have important chronotropic and inotropic cardiac effects, hyperthyroidism is a rare cause of TC, and to the best of our knowledge, only 13 cases have been reported in the literature. 4 TH regulate the number and affinity of myocardial β-adrenergic receptors (AR) and the activity of the adenylate cyclase system. 5 During hyperthyroidism, the number of cardiac β1-AR increases and the expression of inhibitory G-proteins decreases, resulting in cyclic adenosine monophosphate accumulation and subsequently tachycardia. 6 These effects of TH on myocardial β-adrenergic system may contribute to TC in predisposed subjects.
Case:
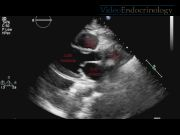
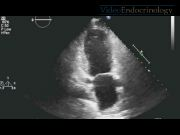
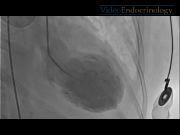
We present a case of a 61-year-old female patient with thyrotoxicosis complicated with TC. She consulted to the emergency department with a 1-week history of palpitations, shortness of breath, chest pain, nervousness, and weight loss of 4 kg. She had been recently diagnosed with hyperthyroidism but was not taking any medication. She denied any recent stressful event in her life. She was found to have an irregular pulse with heart rate of 205 bpm. Her initial laboratory values were significant for serum troponin T: 0.12 ng/mL (n: 0.01–0.03 ng/mL), CKMB: 6.0 ng/mL (n: 0.1–2.9 ng/mL), TSH: 0.01 mcIntUnit/mL (n: 0.27–4.2 mcIntUnit/mL), free T4: 6.10 ng/dL (n: 0.93–1.70 ng/dL), free T3: 12.86 pg/mL (n: 2.3–4.2 pg/mL), and TSI: 593% (n: <140%). An initial electrocardiogram (EKG) showed atrial fibrillation with rapid ventricular response; repeat EKG after rate control with propranolol showed sinus rhythm with heart rate of 95 bpm, nonspecific ST segment changes, and T-wave inversion in anterior leads. A transthoracic echocardiogram showed normal LV wall thickness and chamber size, LV ejection fraction of 35%–39%, abnormal diastolic function, and akinesia of septal and apical wall. The patient underwent cardiac angiogram for suspected non-ST segment elevation myocardial infarction. No coronary artery disease was found, but ballooning of the LV apex was noted. She was diagnosed with TC secondary to thyrotoxicosis and was started on digoxin, methimazole, dexamethasone, and propranolol. However, she remained symptomatic with severe dyspnea; total thyroidectomy was performed with remarkable improvement in her clinical symptoms. The patient was discharged home on thyroid replacement therapy. A transthoracic echocardiogram performed 10 weeks after the surgery was unremarkable.
All authors listed above have contributed sufficiently to the article to be included as authors. We state that this video has not been submitted elsewhere; it is not under review and has not been published previously. Authors identified no conflicts of interest. No competing financial interests exist. All authors are aware of and approve the manuscript being submitted at this journal.
Running time of video: 7 mins, 1 sec
Get full access to this article
View all access options for this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
