Abstract
Traumatic brain injury (TBI) is a significant cause of disability, but little is known about sex and gender differences after TBI. We aimed to analyze the association between sex/gender, and the broad range of care pathways, treatment characteristics, and outcomes following mild and moderate/severe TBI. We performed mixed-effects regression analyses in the prospective multi-center Collaborative European NeuroTrauma Effectiveness Research in Traumatic Brain Injury (CENTER-TBI) study, stratified for injury severity and age, and adjusted for baseline characteristics. Outcomes were various care pathway and treatment variables, and 6-month measures of functional outcome, health-related quality of life (HRQoL), post-concussion symptoms (PCS), and mental health symptoms. The study included 2862 adults (36% women) with mild (mTBI; Glasgow Coma Scale [GCS] score 13–15), and 1333 adults (26% women) with moderate/severe TBI (GCS score 3–12). Women were less likely to be admitted to the intensive care unit (ICU; odds ratios [OR] 0.6, 95% confidence interval [CI]: 0.4-0.8) following mTBI. Following moderate/severe TBI, women had a shorter median hospital stay (OR 0.7, 95% CI: 0.5-1.0). Following mTBI, women had poorer outcomes; lower Glasgow Outcome Scale Extended (GOSE; OR 1.4, 95% CI: 1.2-1.6), lower generic and disease-specific HRQoL, and more severe PCS, depression, and anxiety. Among them, women under age 45 and above age 65 years showed worse 6-month outcomes compared with men of the same age. Following moderate/severe TBI, there was no difference in GOSE (OR 0.9, 95% CI: 0.7-1.2), but women reported more severe PCS (OR 1.7, 95% CI: 1.1-2.6). Men and women differ in care pathways and outcomes following TBI. Women generally report worse 6-month outcomes, but the size of differences depend on TBI severity and age. Future studies should examine factors that explain these differences.
Introduction
Traumatic brain injury (TBI) is a major public health concern and a leading cause of mortality and disability. 1 Many persons who have experienced a TBI show long-term disturbances in physical, cognitive, emotional, and overall functioning. 1 –5 Nevertheless, sex and gender differences in health care and outcomes after TBI are still insufficiently investigated.
Sex refers to biological characteristics and it can be defined according to genetics, and morphology, whereas gender refers to sociocultural behaviors and attitudes. Although the terms are distinct, “sex” and “gender” are usually used interchangeably in the field of neurotrauma. 6 –8 Nevertheless, they highly interact in humans, and differences in the context of health outcomes in humans are rarely the product of exclusively sex or gender. 9,10 To emphasize that it is difficult to disentangle biological and sociocultural components in TBI, and that sex and gender probably have a combined impact, we will use the term “sex/gender” to refer to differences between men and women.
TBI was traditionally considered a “male problem” and associated with risk-taking behaviors and male-dominated professions. 7,11 Generally, men have more than a two-fold risk for sustaining a TBI and tend to acquire TBIs at a younger age. 12 Women, however, catch up in older age with a high proportion of fall-related TBIs. 13,14 In addition, increased participation of women in the military and contact sports has led to higher TBI rates among women. 1,13,15,16 Moreover, a substantial percentage of women experience repetitive TBIs as a result of intimate partner violence. 17 –20
Current scientific guidelines strongly advise considering sex and gender in analyzing and reporting outcomes and treatment effects. 21 –23 Some studies have shown that women have less access and lower rates of direct transfers to trauma centers 6,24 and fewer admissions to intensive care 25 after traumatic injuries. Following TBI, adherence to guidelines for performing computed tomography (CT) seem to be lower for women. 26,27 Further, there is evidence from other medical fields that can potentially be translated to the field of neurotrauma, such as men being provided with more aggressive treatments in cardiovascular medicine. 28 However, studies on differences in care specifically for patients with TBI remain limited, and TBI researchers are encouraged to investigate sex/gender difference in admission and referral from the emergency room (ER), and in outcome measures. 29
Sex/gender differences in outcomes following TBI have been investigated more frequently, but often with inconsistent results, 29 even for important outcomes such as mortality. 6,7,30 Generally, systematic reviews and syntheses of studies found worse outcomes in women, 8,30,31 particularly following mild TBI (mTBI) and when cognitive and psychological symptoms after several months were analyzed as outcomes. 8 In the moderate to severe spectrum of TBI, in which functional outcome and mortality were mostly analyzed as outcomes, a larger proportion of studies showed similar 32,33 outcomes in men and women, or better outcomes 8 in women.
Besides outcome measures and TBI severity, there are other personal and clinical factors that could impact the results of sex/gender-based analyses such as extracranial injuries or medical history, but these are often not included. 8,31 For instance, stratified analyses on both age and sex have shown that certain subgroups are at higher risk for developing poor outcomes following TBI, such as young women for post-traumatic stress disorder (PTSD), 34 women in “child-bearing years” for post-concussion symptoms (PCS), 35 and older women for mortality after isolated TBI. 36
Nevertheless, sex/gender differences in treatment and outcomes after TBI remain inconclusive. Therefore, the aim of this study was to determine the association between sex/gender and a broad range of care pathway and treatment characteristics, and outcomes following mTBI and moderate/severe TBI.
Methods
Patient population
The study population consisted of patients from the prospective multi-center longitudinal observational Collaborative European NeuroTrauma Effectiveness Research in Traumatic Brain Injury (CENTER-TBI) study. 1 For this article, the CENTER-TBI core data set, 37 version 2.0 was used. Data were collected from December 2014 to December 2017 in 63 European centers and in accordance with all relevant laws and regulations. Patients were included if they had a clinical diagnosis of TBI and were presented to a study center within 24 h of injury either to the ER, admission ward (ADM), or intensive care unit (ICU); had an indication for CT scanning; and provided informed consent. Participants were excluded if they had any severe pre-existing neurological disorder that could confound outcome assessments.
Participants with a baseline Glasgow Coma Scale (GCS) score between 13 and 15 were classified as mild, and with a baseline GCS score between 3 and 12 as moderate/severe. Sex/gender was defined based on medical records. Sociodemographic variables, medical history, and clinical and injury characteristics were assessed at admission. CT scanning was performed within 24 h after injury. The 6-month outcomes were measured 6 months post-injury (range 5–8 months).
Ethical approval
The CENTER-TBI study (European Commission [EC] grant 602150) has been conducted in accordance with all relevant laws of the European Union (EU) if directly applicable or of direct effect and all relevant laws of the country where the recruiting sites were located, including but not limited to, the relevant privacy and data protection laws and regulations (the “Privacy Law”), the relevant laws and regulations on the use of human materials, and all relevant guidance relating to clinical studies from time to time in force including, but not limited to, the International Conference on Harmonisation (ICH) Harmonised Tripartite Guideline for Good Clinical Practice (CPMP/ICH/135/95; “ICH GCP”) and the World Medical Association Declaration of Helsinki entitled “Ethical Principles for Medical Research Involving Human Subjects.” Informed consent by the patients and/or the legal representative/next of kin was obtained, accordingly to the local legislations, for all patients recruited in the core data set of CENTER-TBI and documented in the e-CRF. Ethical approval was obtained for each recruiting site. The list of sites, ethical committees, approval numbers, and approval dates can be found on the study website (
Treatment: Care pathway and treatment characteristics
We analyzed the following care pathway variables: Secondary referral: defined as transfer from another hospital to the study center (vs. primary referral = direct transfer to the study hospital). Time to study center: defined as the time from injury to arrival to study center. It was dichotomized at the group median and analyzed only for patients with primary referral. Discharge home: defined as discharge after the ER versus discharge to other facility, hospital, high care unit, or ICU and was analyzed only for patients with mTBI. Admission to the ICU after the ER versus discharge home, discharge to other facility, admission to the hospital or a high care unit was analyzed for all patients and separately for hospitalized patients with mTBI. Discharge to a high care unit or other ICU: versus discharge to general ward, other hospital, rehabilitation, home, and nursing home, after being admitted to ICU, and it was analyzed only for moderate/severe patients. Length of stay (LOS): dichotomized at the group median of hospital stay, and it was analyzed for all patients and for patients who survived until the discharge. Final discharge home: as final discharge location, based on discharge from the ER, ICU, and hospital (vs. rehabilitation, nursing home, or other hospital). Final discharge to rehabilitation: as final discharge location, based on discharge from the ER, ICU, and hospital (vs. home, nursing home, or other hospital). Final discharge was analyzed for patients who survived until the discharge.
As treatment characteristics, we analyzed:
Pre-hospital intubation: defined as an intubated airway upon arrival to the study hospital and was analyzed for patients with moderate/severe TBI.
Time to CT: defined as time from injury to first CT scanning and was dichotomized at the group median.
Intracranial pressure (ICP) monitoring: analyzed only for patients with moderate/severe TBI.
Cranial and extra-cranial surgery: performed during stay in the study hospital.
In-hospital outcome measures
In-hospital mortality: based on registered death at the ER, hospital, and ICU discharge.
Functional outcome measures at 6 months
Glasgow Outcome Scale Extended (GOSE)
The GOSE 38 is a structured interview that measures global outcome following TBI. It provides eight ordinal categories of outcome: dead (1); vegetative state (2); lower severe disability (3); upper severe disability (4); lower moderate disability (5); upper moderate disability (6); lower good recovery (7); and upper good recovery (8). GOSE was measured at 6 months by either a postal questionnaire or a telephone interview. Approximately 7% of responses were by a proxy alone, and 9% by a patient and proxy together. The categories “vegetative state (GOSE 2)” and “lower severe disability (GOSE 3)” were combined, resulting in a 7-point ordinal scale.
Return to work
Return to work is assessed by a follow-up questionnaire. Return to work represented post-injury return to the previous job or school activity at the same or increased level or hours. Not returning to work represented return to the previous job or school activity at reduced level, sheltered employment, or inability to work/go to school. Answers reflecting changing or searching for a job/school or being retired were not included.
Post-concussion and mental health symptoms at 6 months
Rivermead Post-Concussion Symptoms Questionnaire (RPQ)
The RPQ 39 measures cognitive, somatic, and emotional symptoms that are compared with the pre-injury level. It contains 16 items that can be answered with 0 = not experienced, 1 = no more of a problem (than before the injury), 2 = mild problem, 3 = moderate problem, or 4 = severe problem. Total score ≥12 (treating ratings “no more of a problem” as 0) 40 was considered indicative of having increased PCS.
Patient Health Questionnaire (PHQ-9)
The PHQ-941 measures depression severity. It contains nine items using a 4-point Likert scale (from 0 = not at all to 3 = nearly every day), and it can have a score range of 0–27. Cutoffs of 5, 10, and 15 indicate mild, moderate, and moderately severe to severe depressive symptoms, respectively. 42 The score was analyzed as an ordinal variable with four levels: none, mild, moderate, and moderately severe/severe.
Generalized Anxiety Disorder 7-item scale (GAD-7)
GAD-743 measures severity of anxiety. It comprises seven items that can be answered from 0 = not at all to 3 = nearly every day, and it can have a score range of 0–21. Cutoffs 5, 10, and 15 indicate mild, moderate, and severe anxiety, respectively. 43 The score was analyzed as an ordinal variable with four levels: none, mild, moderate, and severe.
Post-Traumatic Stress Disorder (PTSD) Checklist for DSM-5 (PCL-5)
44 PCL-5 measures symptoms of PTSD according to DSM-5 criteria. 45 It consists of 20 items that can be answered with 0 = not at all to 5 = extremely, and it can have a score range of 0–80. A score ≥33 was considered indicative of clinically relevant PSTD. 46,47
Health-related quality of life (HRQoL) measures at 6 months
Quality of Life after Brain Injury-Overall Scale (QOLIBRI-OS)
The QOLIBRI-OS 48 is a brief TBI-specific index of HRQoL that has a scale range of 0–100. Approximately 3% of questionnaires were filled by a proxy alone, and 10% by a patient and proxy together. A score <52 on QOLIBRI-OS was considered indicative of impaired disease-specific quality of life. 37,49
Short Form Health Surveys (SF-12v2; SF-36v2)
SF-12v250 with 12 items and SF-36v2 with 36 items are self-reported and generic measures of HRQoL. The results can be summarized as mental and physical component scores ranging from 0 to 100. Mental and physical component scores were based on a SF-12v2 score, and when there was no available SF-12v2 score, the score was derived using SF-36v2 (when available). 37 Approximately 3% of questionnaires were filled by a proxy alone, and 10% by a patient and proxy together. Mental and physical component scores < 40 were considered indicative for impaired mental and physical HRQoL, respectively. 37,49
Statistical analysis
Descriptive statistics
Descriptive statistics for TBI characteristics, and treatment, and outcome variables were presented separately for men and women using percentages for categorical variables and median with interquartile range for continuous outcomes. Differences were tested using non-parametric tests (e.g., chi-square and Mann-Whitney U test) (Table 1; Supplementary Table S1). All analyses were performed separately for mTBI and moderate/severe TBI.
Baseline Characteristics of Men and Women with Traumatic Brain Injury in the CENTER-TBI Data
Small subcategories merged for regression analyses.
ASA PS, American Society of Anesthesiologists Physical Status; CT, computed tomography; GCS, Glasgow Coma Scale; ISS, Injury Severity Score; MVA, motor vehicle accident; TBI, traumatic brain injury.
Mixed effects regression analyses
The association with multiple treatment characteristics and outcomes following TBI was analyzed with univariable and multi-variable mixed effects regression analyses with a random intercept for study center. In multi-variable analyses, we adjusted for age, baseline GCS score, pupillary reactivity, hypotension and hypoxia before arrival/at admission, CT abnormalities (CT Marshall Classification), traumatic subarachnoid hemorrhage (tSAH), epidural hematoma, Injury Severity Score (ISS), pre-injury medical situation (American Society of Anesthesiologists Physical Status [ASA PS] Classification), pre-injury psychiatric disorder, and cause of injury (fall/motor vehicle accident [MVA]/violence/other), which represent important predictors of outcome in TBI and/or can be associated with sex/gender. 3,46,51 –53 Analyses of pre-hospital and early hospital measures (secondary referral, time to study center, pre-hospital intubation, time to CT) were not adjusted for CT Marshall Classification, tSah, and epidural hematoma.
The multi-variable regression analyses were performed in a completed data set, in which missing values in potential confounders were imputed based on an imputation model with all baseline characteristics, all outcomes, and auxiliary variables (sociodemographic variables, other indicators of medical history, and CT abnormalities). The percentage of imputed missing values (Table 1) ranged from <1% (age, GCS score, ISS) to 16% (Marshall CT for moderate/severe). Further, when the outcome GOSE was assessed outside the time window (range 5–8 months), it was imputed based on GOSE measurements at other time-points. 37 Other outcome variables were not imputed.
Logistic mixed effects regression models were fitted for dichotomized outcomes (e.g., treatment variables and mortality), whereas ordinal mixed effects regression models were fitted for ordinal outcomes (GOSE, depression and anxiety severity). The results were presented in forest plots of ORs for women versus men. For mTBI, forest plots were also stratified by different age groups: 16–45 years, 45–65 years, and 65 years and older (when there were ≥100 outcome events in logistic regression). For moderate/severe TBI, stratified plots were only shown for GOSE because of smaller subsamples.
To check the sensitivity of the results to imputation of missing values, and dichotomization of continuous 6-month outcomes, we performed complete-case and linear regression analyses, respectively (Supplementary Tables S2 and S3).
Analyses were carried out in R 54 (version 5.3) using lme4, 55 ordinal, 56 mice, 57 tableone, 58 and forestplot 59 packages.
Results
Patient characteristics in men and women in the CENTER-TBI study
The study included 2862 adults (36% women) categorized as having mTBI, and 1333 adults (26% women) categorized as having moderate to severe TBI (Table 1).
Men were younger than women when they suffered a TBI (p < 0.001). Falls were the most common cause of mTBI for both men and women, but the proportion of falls was higher in women (p < 0.001). The most frequent cause of moderate/severe TBI was an MVA in men and women, but women had more moderate/severe TBIs due to falls, and men due to violence and other reasons (p < 0.05). Men with mTBI had higher ISS (p < 0.001), lower GCS score (p < 0.05), and higher percentage of epidural hematoma (p < 0.001). There were more women who sustained a moderate TBI, and men who sustained a severe TBI (p < 0.05). Women had a higher proportion of psychiatric disorders prior to mTBI and moderate/severe TBI (p < 0.001), and worse physical health prior to mTBI (p < 0.001; Table 1).
The association between sex/gender and care pathway and treatment characteristics
Following mTBI, women had different care pathways, with a lower proportion of referrals from another hospital (12% vs. 16%) and admissions to the ICU (14% vs. 23%), more discharge home (34% vs. 25%), and shorter hospital stay (46% vs. 52% higher than median stay). Regarding treatment characteristics, women had longer time to CT scan (53% vs. 48% higher than median; Table 2; Supplementary Fig. S1).
Descriptive Statistics for Care Pathway and Treatment Characteristics for Men and Women with Traumatic Brain Injury
CT, computed tomography; ICP, intracranial pressure; ICU, intensive care unit; LOS, length of stay.
Following moderate/severe TBI, men and women had similar care pathway and treatment characteristics. Women, however, had shorter hospital stays (44% vs. 52% for all, 34% vs. 43% above the median of LOS), and had fewer pre-hospital intubations (51% vs. 58%, Table 2; Supplementary Fig. S2).
In mixed-effect multi-variable analyses (Fig. 1), there were no significant differences between men and women with mTBI in the majority of care pathway and treatment characteristics. Women who sustained an mTBI were less likely to have a secondary referral (odds ratio [OR] 0.7, 95% confidence interval [CI]: 0.6-0.95). Moreover, women were more likely to be discharged home after presenting to the ER (OR 1.4, 95% CI: 1.0-1.8); and less likely to be admitted to the ICU (OR 0.6, 95% CI: 0.4-0.8), in the total mTBI sample and among hospitalized mTBI patients.
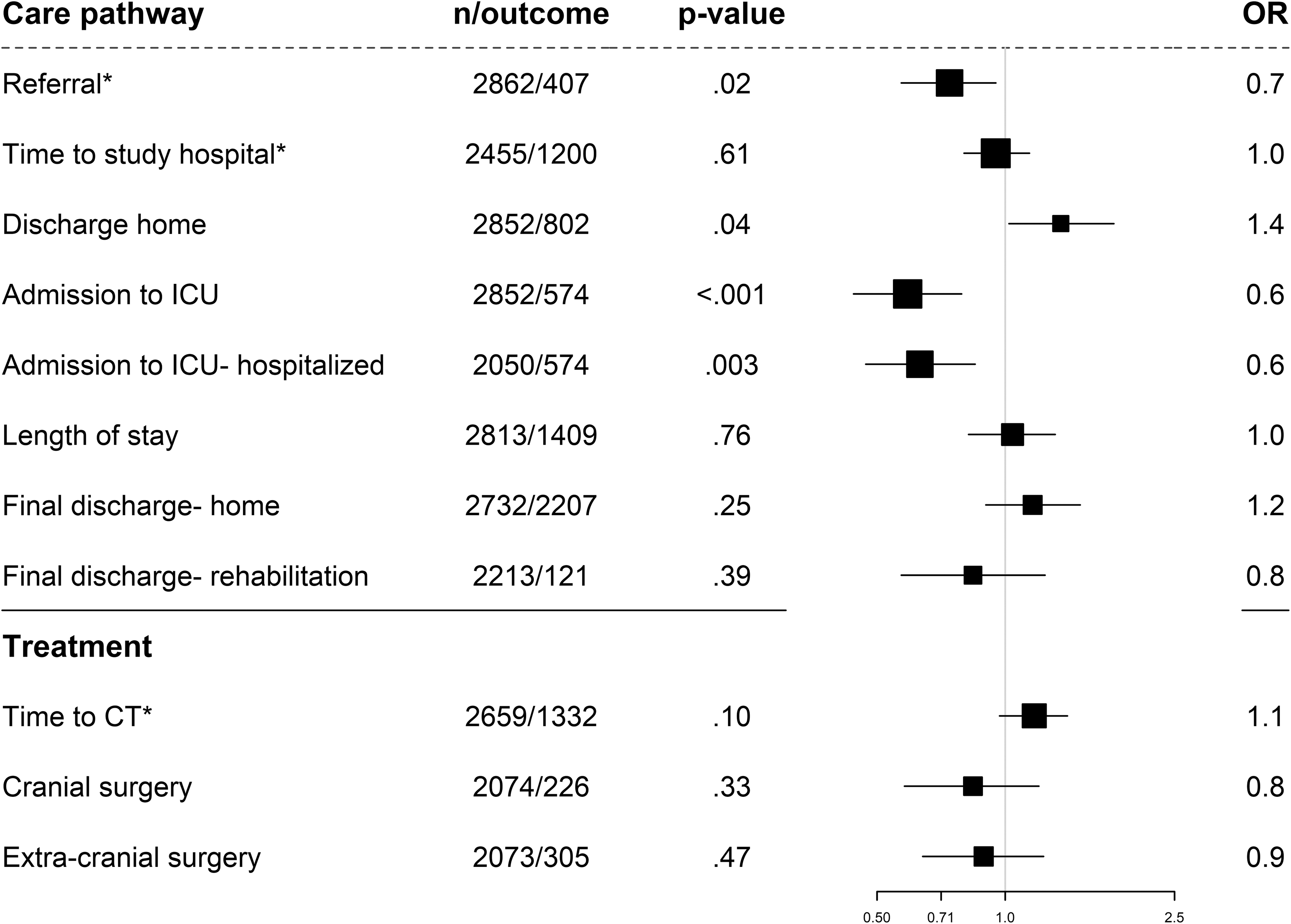
Forest plot with adjusted odds ratios (ORs) for women with mild traumatic brain injury: care pathway and treatment characteristics. The ORs are adjusted for age, baseline Glasgow Coma Scale score, pupillary reactivity, hypotension and hypoxia before arrival/at admission, Marshall Classification, traumatic subarachnoid hemorrhage (tSAH), epidural hematoma; Injury Severity Score (ISS), pre-injury medical situation (ASA PS Classification), pre-injury psychiatric disorder, and cause of injury. *Not adjusted for CT Marshall Classification, tSAH, and epidural hematoma. ASA PS, American Society of Anesthesiologists Physical Status; CT, computed tomography; ICU, intensive care unit; n/outcome, number of patients/number of patients with outcome.
Men and women with moderate or severe TBI did not differ in the majority of care pathway and treatment characteristics (Fig. 2). Among patients with primary referral (direct transfer to study hospital), women were somewhat less likely to have longer time to study hospital (OR 0.8, 95% CI: 0.6-1.1). Further, women were more likely to have a rehabilitation as the final discharge location (OR 1.5, 95% CI: 1.0-2.1), but less likely to stay in the hospital longer than a median of 22 days (patients who survived until discharge; OR 0.7, 95% CI: 0.5-1.0), and to have pre-hospital intubation (OR 0.8, 95% CI: 0.6-1.1).
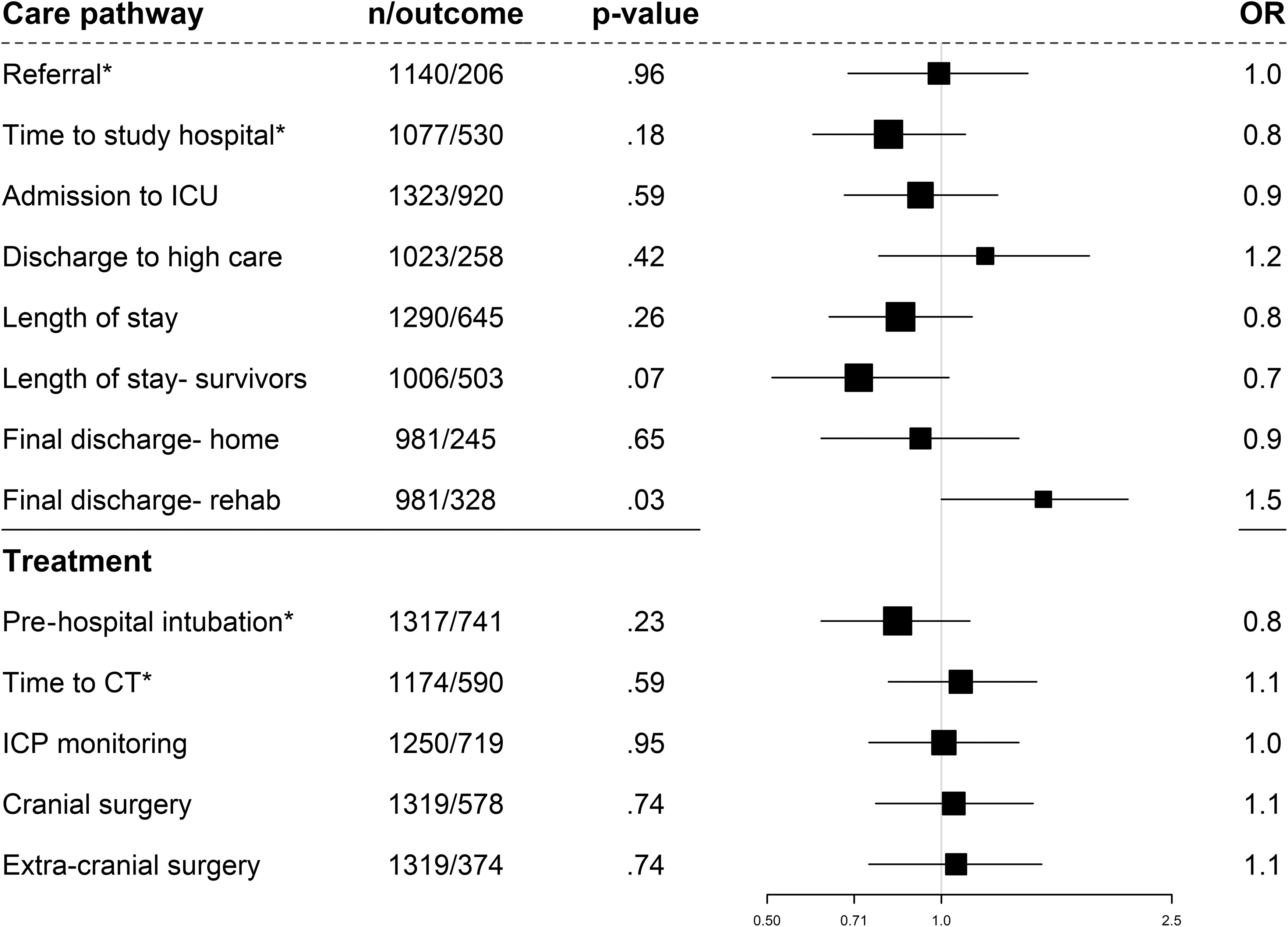
Forest plot with adjusted odds ratios (ORs) for women with moderate/severe traumatic brain injury: care pathway and treatment characteristics. The ORs are adjusted for age, baseline Glasgow Coma Scale score, pupillary reactivity, hypotension and hypoxia before arrival/at admission, Marshall Classification, traumatic subarachnoid hemorrhage (tSAH), epidural hematoma, Injury Severity Score (ISS), pre-injury medical situation (ASA PS Classification), pre-injury psychiatric disorder, and cause of injury. ASA PS, American Society of Anesthesiologists Physical Status; CT, computed tomography; ICP, intracranial pressure; ICU, intensive care unit; n/outcome, number of patients/number of patients with outcome.
The association between sex/gender, and in-hospital mortality and 6-month outcomes
For mTBI, the proportion of missing values in 6-month outcomes varied from 17% for GOSE to 40–45% for other outcomes. For moderate or severe TBI, the proportion of missing values varied from 1% for in-hospital mortality, 13% for GOSE, to about 60% for other outcomes (Supplementary Table S1). However, 26% of patients with moderate/severe TBI did not survive until 6 months.
Following mTBI, women had a higher percentage of unfavorable outcomes (lower GOSE), lower generic and disease-specific HRQoL, and more severe PCS, depression, anxiety, and PTSD (Table 3; Supplementary Table S1; Supplementary Fig. S3). There was no difference in probable PTSD diagnosis. Following moderate/severe TBI, women had more severe PCS (Table 3; Supplementary Table S1; Supplementary Fig. S4). Mental health measures were somewhat poorer in men, but the differences were insignificant (Table 3; Supplementary Table S1, Supplementary Fig. S4).
Distributions of Outcome Variables for Men and Women with Mild and Moderate or Severe Traumatic Brain Injury
GAD-7, Generalized Anxiety Disorder 7-item scale; GOSE, Glasgow Outcome Scale Extended; PCL-5, Post-Traumatic Stress Disorder Checklist for DSM-5; PHQ-9, Patient Health Questionnaire 9-item; QOLIBRI-OS, Quality of Life after Brain Injury-Overall Scale; RPQ, Rivermead Post-Concussion Symptoms Questionnaire; SF12, Short Form Health Survey 12 item; TBI, traumatic brain injury.
In multi-variable analyses of patients with mTBI (Fig. 3), women were more likely to have a poor global outcome (OR 1.4, 95% CI: 1.2-1.6 for ordinal GOSE), and not to return to work (OR 1.4, 95% CI: 1.0-1.9). Moreover, women were more likely to experience more severe PCS (OR 1.7, 95% CI: 1.3-2.1), depression (OR 1.6, 95% CI: 1.3-2.0), anxiety (OR 1.6, 95% CI: 1.2-2.0), and to report impaired disease-specific (OR 1.8, 95% CI: 1.4-2.3), mental (OR 1.6, 95% CI: 1.3-2.1) and physical (OR 1.8, 95% CI: 1.4-2.3) generic HRQoL. There was no association between sex/gender and probable PTSD diagnosis (OR 1.1, 95% CI: 0.7-1.6) present in smaller percentage of patients, but women showed higher PTSD symptoms in linear analysis (beta = 1.88, p = 0.01; Supplementary Table S3).
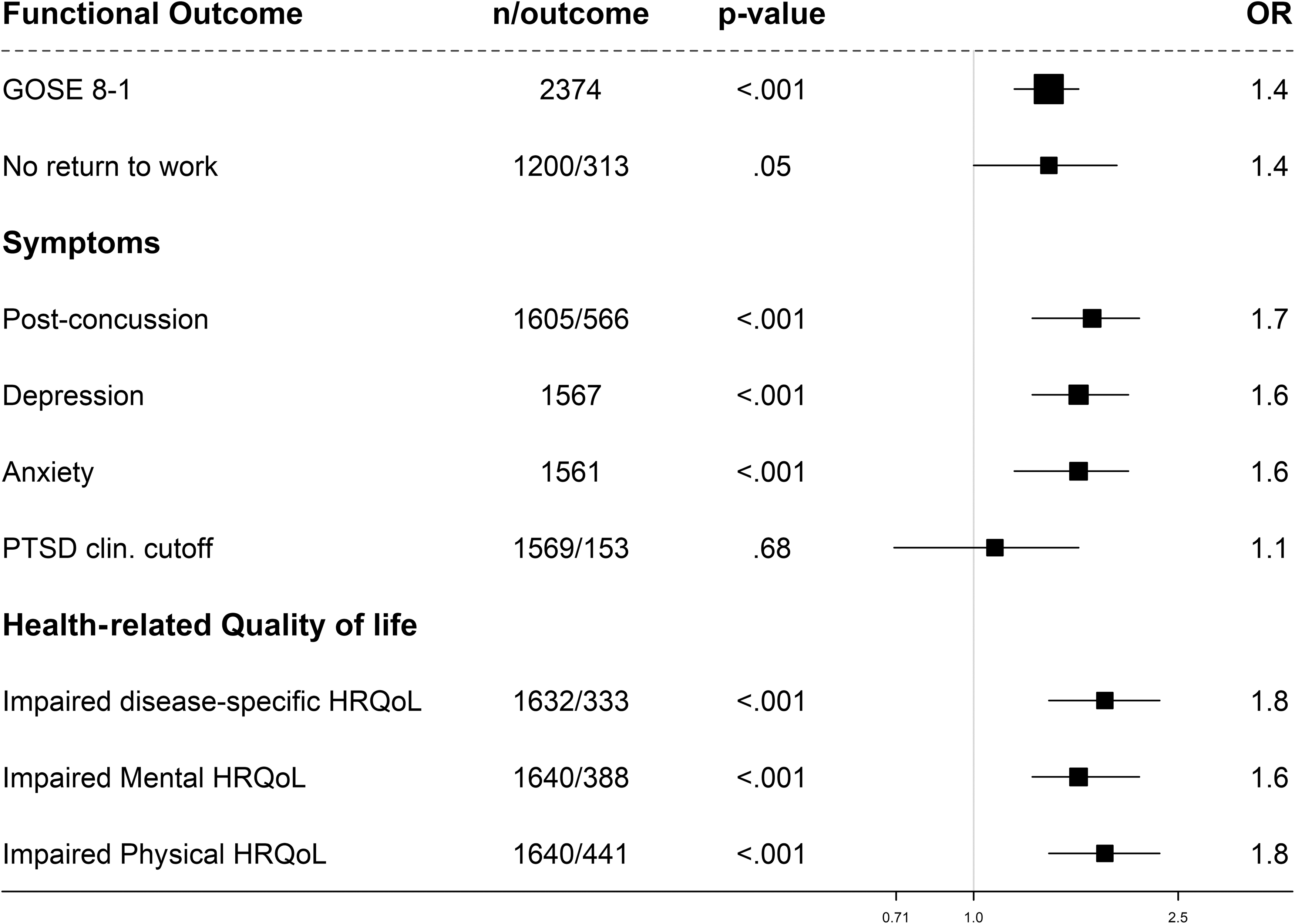
Forest plot with adjusted odds ratios (ORs) for women with mild traumatic brain injury: 6-month outcomes. The ORs are adjusted for age, baseline Glasgow Coma Scale score, pupillary reactivity, hypotension and hypoxia before arrival/at admission, Marshall Classification, traumatic subarachnoid hemorrhage (tSAH), epidural hematoma, Injury Severity Score (ISS), pre-injury medical situation (ASA PS Classification), pre-injury psychiatric disorder, and cause of injury. ASA PS, American Society of Anesthesiologists Physical Status; GOSE, Glasgow Outcome Scale Extended; PTSD, post-traumatic stress disorder; n/outcome, number of patients/number of patients with outcome.
Following moderate or severe TBI, multi-variable analyses (Fig. 4) showed somewhat lower, but insignificant, ORs for women for in-hospital mortality (OR 0.8, 95% CI: 0.5-1.2) and mortality at 6 months (OR 0.7, 95% CI: 0.5-1.0). No (substantial) differences were found in 6-month ordinal GOSE (OR 0.9, 95% CI: 0.7-1.2), return to work (OR 1.2, 95% CI: 0.7-2.1), or impaired physical HRQoL (OR 1.2, 95% CI: 0.7-1.2). Adjusted linear analyses showed no differences in brain-injury-specific and physical HRQoL (Supplementary Table S3).
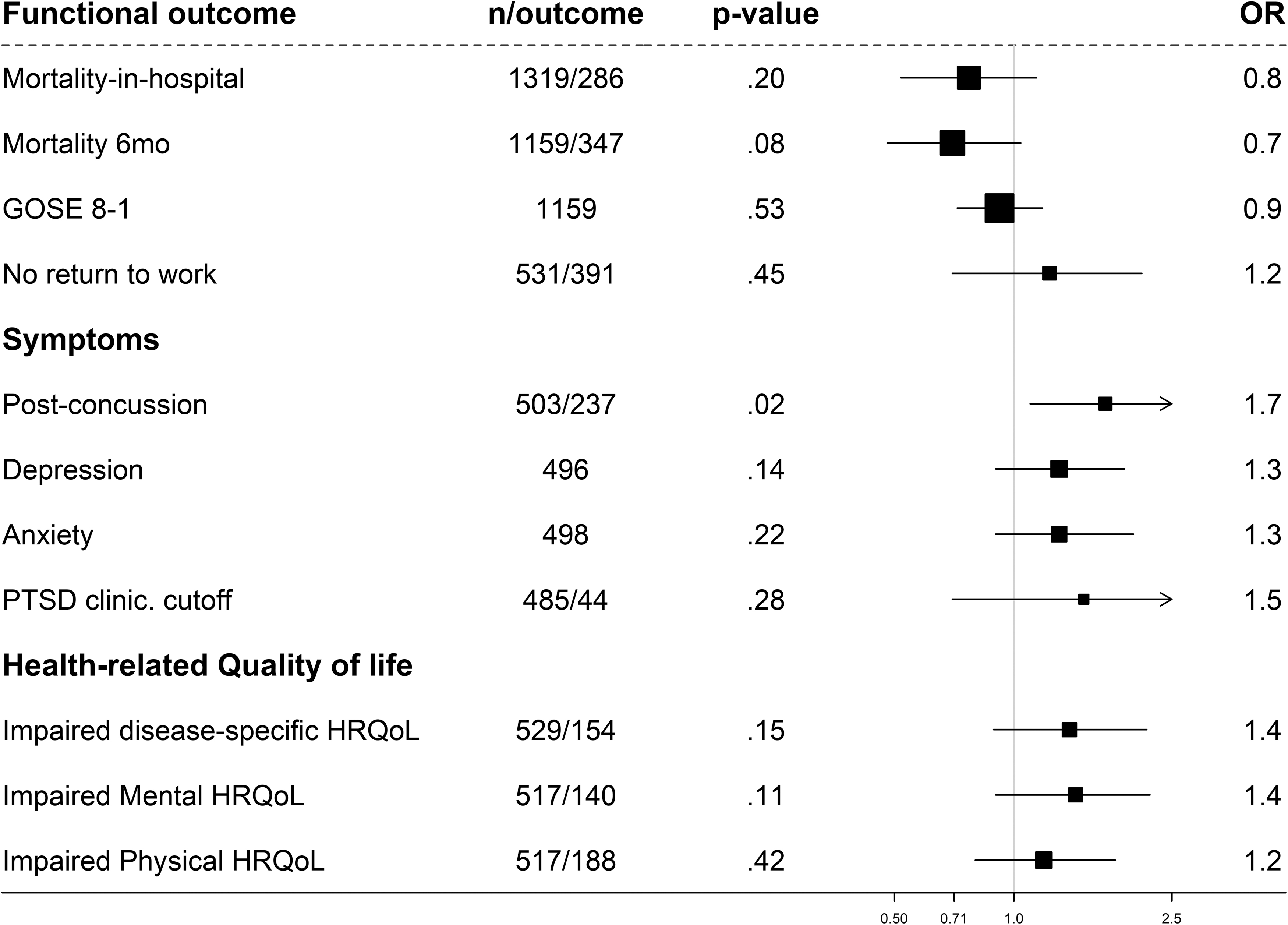
Forest plot with adjusted odds ratios (ORs) for women with moderate/severe traumatic brain injury: in-hospital mortality and 6-month outcomes. The ORs are adjusted for age, baseline Glasgow Coma Scale score, pupillary reactivity, hypotension and hypoxia before arrival/at admission, Marshall Classification, traumatic subarachnoid hemorrhage (tSAH), epidural hematoma, Injury Severity Score (ISS), pre-injury medical situation (ASA PS Classification), pre-injury psychiatric disorder, and cause of injury. ASA PS, American Society of Anesthesiologists Physical Status; GOSE, Glasgow Outcome Scale Extended; PTSD, post-traumatic stress disorder; n/outcome, number of patients/number of patients with outcome.
However, women were more likely to experience more severe PCS (OR 1.7, 95% CI: 1.1-3.0). The likelihood for depression severity (OR 1.3, 95% CI: 0.9-1.9), anxiety severity (OR 1.3, 95% CI: 0.9-2.0), probable PTSD diagnosis (OR 1.5, 95% CI: 0.7-3.3), impaired mental (OR 1.4, 95% CI: 0.9-2.2) and impaired disease-specific HRQoL (OR 1.4, 95% CI: 0.9-2.1) assessed with the QOLIBRI-OS was somewhat higher in women, but precision was limited and CIs included the null.
The association between sex/gender and 6-month outcomes in different age groups
Sex/gender differences in different age groups of mTBI patients varied between outcomes (Fig. 5; Supplementary Fig. S5). There was, however, no outcome or age group where men had worse outcomes, only the lack of differences or worse functioning of women were observed. The biggest sex/gender difference for GOSE (OR 1.9, 95% CI: 1.4-2.5), not returning to work (OR 1.6, 95% CI: 0.9-2.8), and PCS (OR 2.5, 95% CI: 1.5-3.8) were found in patients younger than age 45 years.
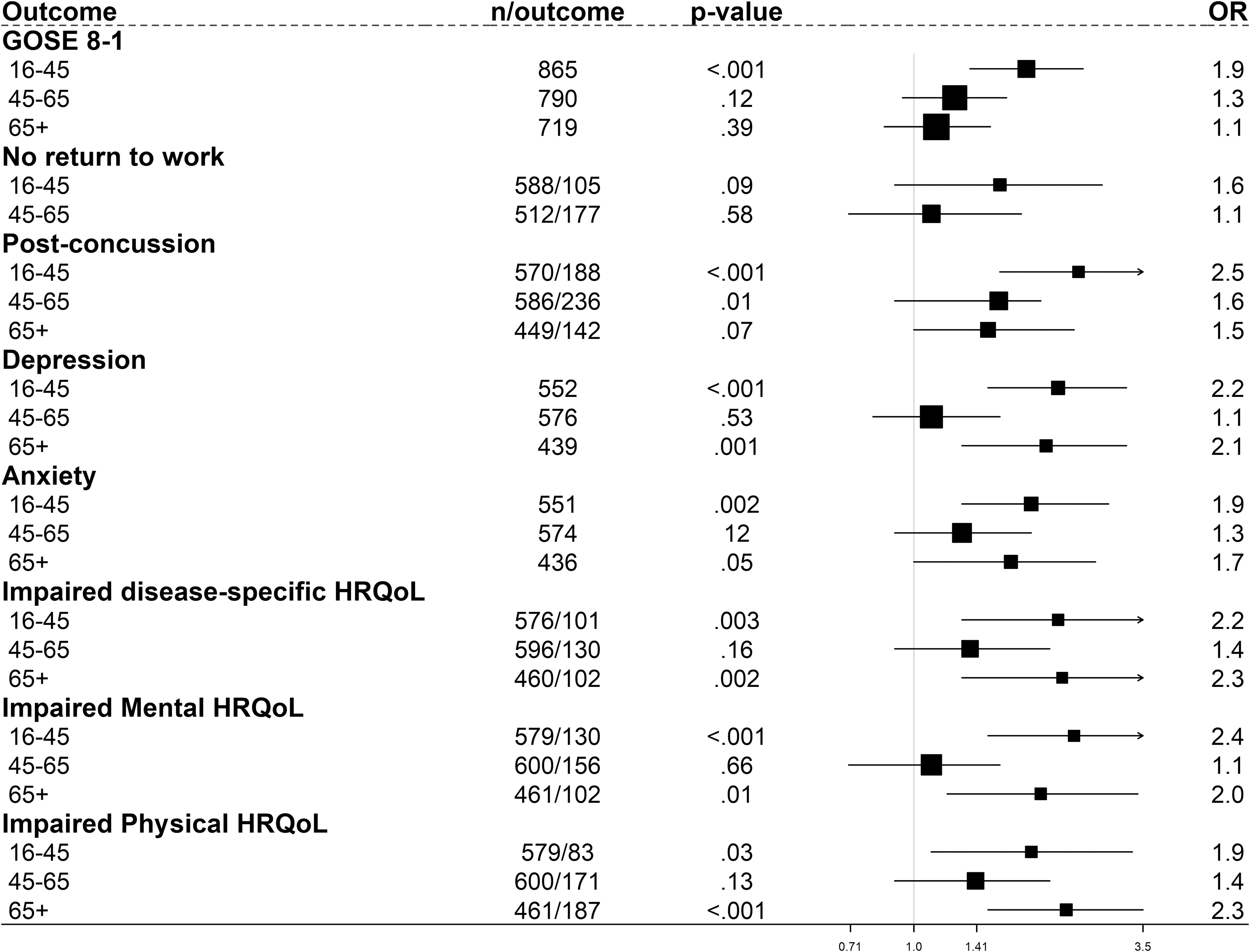
Forest plot with adjusted odds ratios (ORs) for women in different age groups: outcomes following mild traumatic brain injury. The ORs are adjusted for age, baseline Glasgow Coma Scale score, pupillary reactivity, hypotension and hypoxia before arrival/at admission, Marshall Classification, traumatic subarachnoid hemorrhage (tSAH), epidural hematoma, Injury Severity Score (ISS), pre-injury medical situation (ASA PS Classification), pre-injury psychiatric disorder, and cause of injury. ASA PS, American Society of Anesthesiologists Physical Status; GOSE, Glasgow Outcome Scale Extended ;n/outcome, number of patients/number of patients with outcome.
The difference was most pronounced in patients younger than age 45 years and older than 65 years for mental health and HRQoL: depression (OR 2.2, 95% CI: 1.5-3.2; OR 2.1, 95% CI: 1.3-3.2, respectively); anxiety (OR 1.9, 95% CI: 1.3-2.9; OR 1.7, 95% CI: 1.0-2.7), impaired mental (OR 2.4, 95% CI: 1.5-3.8; OR 2.0, 95% CI: 1.2-3.4), physical (OR 1.9, 95% CI: 1.1-3.3; OR 2.3, 95% CI: 1.5-3.5), and disease-specific HRQoL (OR 2.2, 95% CI: 1.3-3.6; OR 2.3, 95% CI: 1.3-3.8).
Following moderate/severe TBI (Fig. 6; Supplementary Fig. S6), women over age 65 years had a lower likelihood of poor functional outcome (GOSE) than men (OR 0.6, 95% CI: 0.3-0.96), whereas women under age 65 years had similar (or slightly worse) global functioning as men (OR 1.2, 95% CI: 0.8-1.7) under 45 years; (OR 1.0, 95% CI: 0.6-1.5; 45–65).
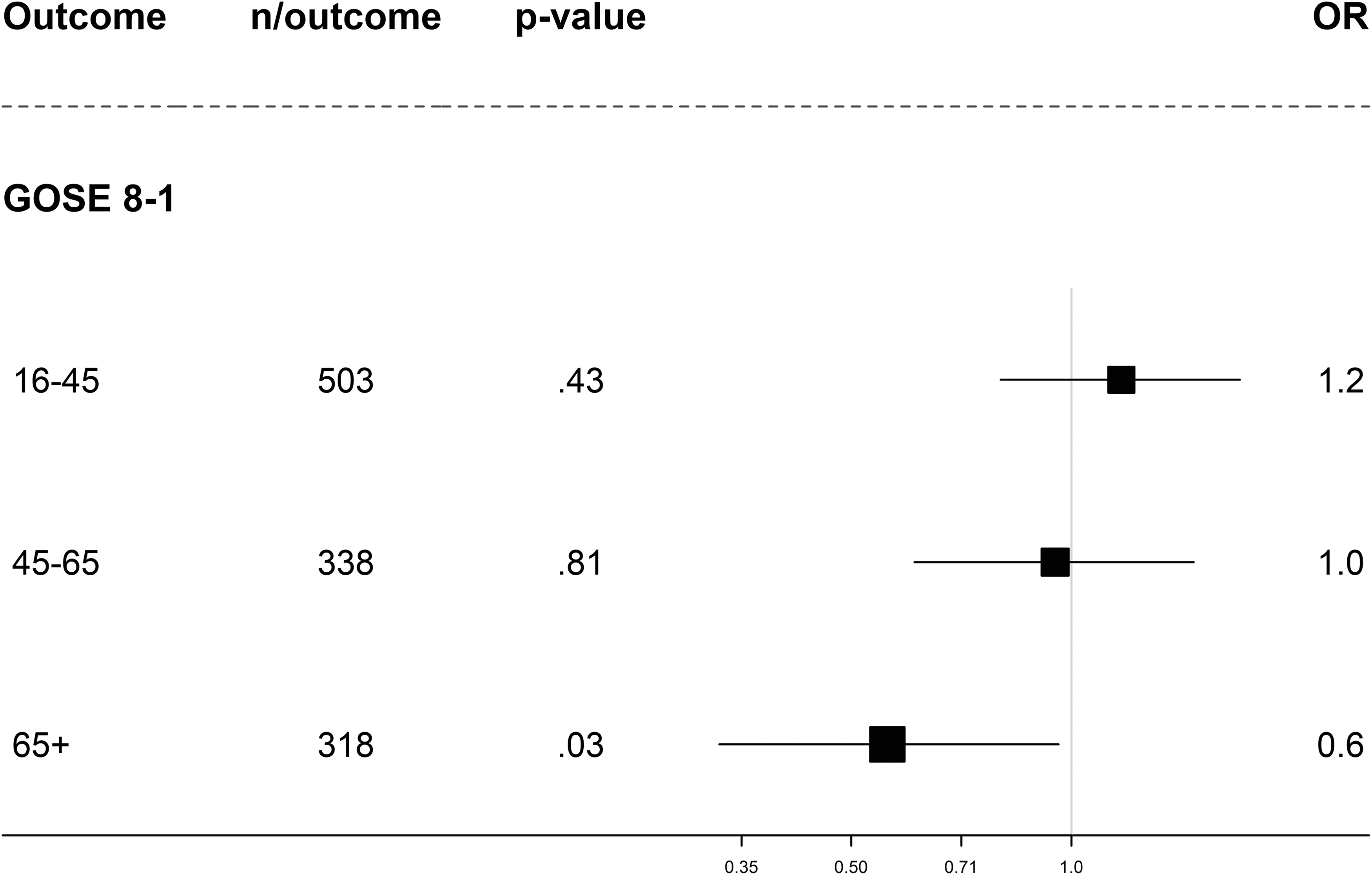
Forest plot with adjusted odds ratios (ORs) for women in different age groups: Glasgow Coma Scale Extended score following moderate to severe traumatic brain injury. The ORs are adjusted for age, baseline Glasgow Coma Scale score, pupillary reactivity, hypotension and hypoxia before arrival/at admission, Marshall Classification traumatic subarachnoid hemorrhage (tSAH), epidural hematoma, Injury Severity Score (ISS), pre-injury medical situation (ASA PS Classification), pre-injury psychiatric disorder, and cause of injury. ASA PS, American Society of Anesthesiologists Physical Status; GOSE, Glasgow Outcome Scale Extended; n/outcome, number of patients/number of patients with outcome.
Discussion
We examined sex/gender differences in various care pathway and treatment characteristics and outcomes following mTBI and moderate/ severe TBI. Men and women did not substantially differ in treatment characteristics, but some differences in care pathway, particularly discharge destinations following mTBI, were found. Women generally reported worse 6-month outcomes, but the differences with men depended on TBI severity and age. Sex/gender differences were more pronounced following mTBI, particularly under 45 and above 65 years of age.
We did not find strong association between sex/gender and most of the care pathway and treatment variables. Following mTBI, women were less likely to be referred from another hospital to a study center, and to be admitted to the ICU, and were more likely to be discharged home. Apart from that, some differences were observed with limited precision: men had a longer hospital stay and less discharge to rehabilitation following moderate/severe TBI. Similar studies are limited in the field of TBI, and observed differences are partially consistent with other studies in trauma and critical care.
Contrary to our results of women's more direct transfers and thus decreased time to study center, some previous studies have identified less access for women in general trauma care. 6,60 For example, in a large Canadian retrospective cohort study, women had a lower likelihood of direct transfer to trauma centers by both emergency service triage and the physicians. 24 Consistent with our result of fewer ICU admissions following mTBI (but not moderate/severe), some other studies have found less access to intensive care after traumatic injuries in women. 25,61 –64 Similarly, women are shown to receive fewer aggressive treatments in other medical fields. 28,65
Lower rates of intensive care in women, as well as their shorter hospital stay, are usually attributed to women's lower injury severity, different injury mechanisms, and better recovery. 25,33,61 Even though we adjusted for baseline characteristics in our analyses, residual confounding remains possible. Therefore, the observed differences can be also the result of insufficient adjustment for differences in clinical needs. 64,65 Nevertheless, obtaining differences in trauma care pathway after adjustment for relevant variables cannot completely rule out gender bias as a possible explanation. 30,62,66,67 For better insight in patterns of care pathways, more studies on sex/gender differences in health care are necessary in the field of neurotrauma. In any case, discussing the importance of gender in context of health, and potential bias related to gender (and other aspects of identity) should be universally and systematically incorporated in training of health care providers.
The study results are in line with some previous findings of worse outcomes in women several months after injury. 8,30 Women reported more severe mental health and post-concussion symptoms compared with men, particularly following mTBI, where women reported worse outcomes across all domains. Differences following moderate/severe TBI were generally smaller and less precise. The differences in self-report, particularly in the mental domain, might not be specifically related to the experience of TBI. Women generally tend to self-report more symptoms, and to seek medical help when needed. 68 –70 Mental health disturbances from the depressive and anxiety spectrum are generally higher in women than men, particularly in the young age. 71 –74
In addition, biological factors can interact with the general gender differences and contribute to more symptoms in women. For instance, disruption in hypothalamic-pituitary axis (HPA) and hypopituitarism seem to occur in more than one-quarter of patients after TBI, and even in 15% of patients with complicated mTBI, 75 which may affect outcomes and stress levels in a sex-specific manner. A recent study found differential dysregulation of HPA and, consequently, stress response, following mTBI in female compared with male mice. 76
Conversely, a neuroprotective role of the hormones estrogen and progesterone after TBI was found in animal studies and speculated in human studies, but the findings in human studies have been mixed. 8,77,78 Thus, differences in mortality after TBI were inconsistent in previous studies, 6,7,30,79 and they stayed unclear in our study with an insignificant lower likelihood of dying in the hospital or by 6 months for women. Further, we found a pattern of more disadvantage of women (vs. men) in global functioning in reproductive age than other age groups, which is not in line with explanations based on neuroprotection of sex steroids. 78 Some authors explain this pattern by post-TBI disruption in production of sex steroids in pre-menopausal women, which results in the reduction of the neuroprotection. 35,80
In this study, women under 45 years of age, and over 65 years for some outcomes, showed particularly worse 6-month outcomes following mTBI compared with men of the same age. Besides hormonal differences, men and women under age 45 years may face different challenges in everyday life. Women report struggling with expectations of managing the household, and balancing domestic duties and childcare with rehabilitation when recovering from acquired brain injury. 81,82 A substantial number of young adult women have to combine the role of the primary caregiver of underage children with the work role. In that way, gender norms can create an extra burden for women under age 45 years, and negatively impact their quality of life and mental health following TBI. 35,83 In contrast, men may have the pressure to return to work and normal functioning more quickly, because they still prevail as primary wage earners, 35,83 which could lead to better global functional outcome. At older age, women tend to outlive their partners, and they are more likely to live alone following TBI. 84 In addition, generally lower economic resources and power in the society can reduce (older) women's ability to adequately cope with a condition such as brain injury. 7,70,85,86
Sex/gender differences in subjective measures were, however, more pronounced in the mild versus moderate/severe TBI group. Difference in functioning following moderate or severe injuries may be more closely related to injury-related, physical and neurological disabilities. 3,43 In contrast, functioning after milder injuries may be under a greater influence of differences in self-report, perceived stress, and socioeconomic factors, which are associated with sex and gender. Thus, taking sex/gender into account could be particularly beneficial in scheduling follow-up appointments and organizing rehabilitation following mTBI. Further, treatment differences could also impact outcomes after several months. For instance, direct transfer and short time to trauma care generally contribute to better outcomes. The potential impact of the admission to the ICU after mTBI is unclear. A substantial proportion of ICU admissions following mTBIs seem to be unnecessary 87 and admission can be associated with negative psychological consequences, 88 but some patients do benefit from intensive monitoring.
This study has some limitations. First, the proportion of missing values was high for some 6-month outcomes, particularly in the moderate/severe group. Men had larger proportions of missing values in 6-month mental health and quality-of-life outcomes; however, the proportions were comparable between men and women who survived until 6 months. Further, due to testing for multiple end-points, which can increase the probability of false-positive findings, it is possible that some differences were found due to chance. On the other hand, analyses of patients with moderate/severe TBI and age groups could be underpowered to find sex/gender differences. Moreover, although we adjusted the analyses with numerous relevant variables, we might have missed some important confounders for specific analyses. Additionally, sex was based on medical records and therefore may be incorrect for some patients, or not correctly matched to the gender identity (being a woman or a man). We recognize that there is a notable minority of both intersex and cisgender persons, who were not adequately captured by this dichotomy. Future TBI studies could profit from including more detailed measures of gender.
Further, this study included hospital centers across Europe (and Israel), with the majority being academic hospitals located in urban areas in West and North Europe. 37,89 Between and within European countries, there is variability in health care and care pathways following TBI, 37,90 but also in gender equality in access to health care and unmet medical needs. 91 Generally, areas with more traditional and restrictive gender norms, and with less implemented strategies to reduce gender bias in health systems, tend to have larger gender inequalities in health care. 92,93 Following TBI, we hypothesize that in those areas men are offered more aggressive treatments, and women have less access to care, particularly in case of violence. In addition, differences in intention to self-report symptoms following TBI may be greater in the context of more traditional gender norms. 94 A reliable sex/gender analyses stratified by country or region would require a higher sample and better representation of East and South Europe, and smaller hospital centers. Moreover, the ability to generalize the findings of a European study to other geopolitical and cultural settings is limited.
A strength of the study is the use of a large data set of representative contemporary patients from different countries and with different injury severity. Importantly, there is a lack of studies on treatment and care pathway in the context of sex/gender and TBI, and this study provides an overview of a range of important characteristics. For 6-month functioning, a broad battery of different outcomes was used to cover various domains. The analyses were adjusted for study center and important personal and injury characteristics, which was a limitation of many previous studies.
In conclusion, men and women differ in care pathway and outcomes, depending on injury severity and age group. Future studies should continue investigating sex and gender differences in health care after TBI. In addition, underlying factors of the differences in outcomes, particularly following mTBI, should be explored by disentangling the influence of socioeconomic, biological, and treatment differences. Finally, differences should also be discussed in the context of provision and organization of care, such as incorporating gender considerations into the training of health care providers, and monitoring and rehabilitation of patients at risk for poorer outcomes following TBI.
Footnotes
Acknowledgments
We are grateful to all patients and investigators who participated in the CENTER-TBI study.
The CENTER-TBI Participants and Investigators
Cecilia Åkerlund, Karolinska Institutet, Stockholm, Sweden; Krisztina Amrein, University of Pécs, Pécs, Hungary, Nada Andelic, Oslo University Hospital and University of Oslo, Oslo, Norway; Lasse Andreassen, University Hospital Northern Norway, Tromso, Norway; Audny Anke, University Hospital Northern Norway, Tromso, Norway; Anna Antoni, Medical University Vienna, Vienna, Austria; Gérard Audibert, University Hospital Nancy, Nancy, France, University Hospital Nancy, Nancy, France; Philippe Azouvi, Raymond Poincare Hospital, Assistance Publique – Hopitaux de Paris, Paris, France; Maria Luisa Azzolini, S. Raffaele University Hospital, Milan, Italy; Ronald Bartels, Radboud University Medical Center, Nijmegen, The Netherlands; Pál Barzó, University of Szeged, Szeged, Hungary; Romuald Beauvais, ARTTIC, Munchen, Germany; Ronny Beer, Medical University of Innsbruck, Innsbruck, Austria; Bo-Michael Bellander, Karolinska University Hospital, Stockholm, Sweden; Antonio Belli, NIHR Surgical Reconstruction and Microbiology Research Centre, Birmingham, UK; Habib Benali, Assistance Publique – Hopitaux de Paris, Paris, France; Maurizio Berardino, AOU Città della Salute e della Scienza di Torino - Orthopedic and Trauma Center, Torino, Italy; Luigi Beretta, S. Raffaele University Hospital, Milan, Italy; Morten Blaabjerg, Odense University Hospital, Odense, Denmark; Peter Bragge, Monash University, Victoria, Australia; Alexandra Brazinova, Trnava University, Trnava, Slovakia; Vibeke Brinck, Quesgen Systems Inc., Burlingame, California, USA; Joanne Brooker, Monash University, Melbourne, Australia; Camilla Brorsson, Umeå University, Umeå, Sweden; Andras Buki, University of Pécs, Hungary; Monika Bullinger, Universitätsklinikum Hamburg-Eppendorf, Hamburg, Germany; Manuel Cabeleira, University of Cambridge, Addenbrooke's Hospital, Cambridge, UK; Alessio Caccioppola, Fondazione IRCCS Cà Granda Ospedale Maggiore Policlinico, Milan, Italy; Emiliana Calappi, Fondazione IRCCS Cà Granda Ospedale Maggiore Policlinico, Milan, Italy; Maria Rosa Calvi, S. Raffaele University Hospital, Milan, Italy; Peter Cameron, Monash University, Melbourne, Victoria, Australia; Guillermo Carbayo Lozano, Hospital of Cruces, Bilbao, Spain; Marco Carbonara, Fondazione IRCCS Cà Granda Ospedale Maggiore Policlinico, Milan, Italy; Ana M. Castaño-León, Hospital Universitario 12 de Octubre, Madrid, Spain; Simona Cavallo, AOU Città della Salute e della Scienza di Torino - Orthopedic and Trauma Center, Torino, Italy; Giorgio Chevallard, Niguarda Hospital, Milan, Italy; Arturo Chieregato, Niguarda Hospital, Milan, Italy; Giuseppe Citerio, Università Milano Bicocca, Milano, Italy and ASST di Monza, Monza, Italy; Iris Ceyisakar, Erasmus Medical Center-University Medical Center, Rotterdam, The Netherlands; Hans Clusmann, Aachen University, Aachen, Germany; Mark Coburn, University Hospital of Aachen, Aachen, Germany; Jonathan Coles, Cambridge University Hospital NHS Foundation Trust, Cambridge, UK; Jamie D. Cooper, Monash University and The Alfred Hospital, Melbourne, Victoria, Australia; Marta Correia, MRC Cognition and Brain Sciences Unit, Cambridge, UK; Amra Čović, Universitätsmedizin Göttingen, Göttingen, Germany; Nicola Curry, Oxford University Hospitals NHS Trust, Oxford, UK; Endre Czeiter, University of Pécs, Hungary; Marek Czosnyka, University of Cambridge, Addenbrooke's Hospital, Cambridge, UK; Claire Dahyot-Fizelier, CHU Poitiers, Potiers, France; Paul Dark, Salford Royal Hospital NHS Foundation Trust, Salford, UK; Helen Dawes, Oxford Brookes University, Oxford, UK; Véronique De Keyser, Antwerp University Hospital and University of Antwerp, Edegem, Belgium; Vincent Degos, Assistance Publique – Hopitaux de Paris, Paris, France; Francesco Della Corte, Maggiore Della Carità Hospital, Novara, Italy; Hugo den Boogert, Radboud University Medical Center, Nijmegen, The Netherlands; Bart Depreitere, University Hospitals Leuven, Leuven, Belgium; Đula Đilvesi, University of Novi Sad, Novi Sad, Serbia; Abhishek Dixit, University of Cambridge, Addenbrooke's Hospital, Cambridge, UK; Emma Donoghue, Monash University, Melbourne, Australia; Jens Dreier, Charité – Universitätsmedizin Berlin, Berlin, Germany; Guy-Loup Dulière, CHR Citadelle, Liège, Belgium; Ari Ercole, University of Cambridge, Addenbrooke's Hospital, Cambridge, UK; Patrick Esser, Oxford Brookes University, Oxford, UK; Erzsébet Ezer, University of Pécs, Pécs, Hungary; Martin Fabricius, Region Hovedstaden Rigshospitalet, Copenhagen, Denmark; Valery L. Feigin, Auckland University of Technology, Auckland, New Zealand; Kelly Foks, Erasmus MC, Rotterdam, the Netherlands; Shirin Frisvold, University Hospital Northern Norway, Tromso, Norway; Alex Furmanov, Hadassah-Hebrew University Medical Center, Jerusalem, Israel; Pablo Gagliardo, Fundación Instituto Valenciano de Neurorrehabilitación (FIVAN), Valencia, Spain; Damien Galanaud, Assistance Publique – Hopitaux de Paris, Paris, France; Dashiell Gantner, Monash University, Melbourne, Victoria, Australia; Guoyi Gao, Shanghai Renji Hospital, Shanghai Jiaotong University/School of Medicine, Shanghai, China; Pradeep George, Karolinska Institutet, Stockholm, Sweden; Alexandre Ghuysen, CHU, Liège, Belgium; Lelde Giga, Pauls Stradins Clinical University Hospital, Riga, Latvia; Ben Glocker, Imperial College London, London, UK; Jagoš Golubovic, University of Novi Sad, Novi Sad, Serbia; Pedro A. Gomez, Hospital Universitario 12 de Octubre, Madrid, Spain; Johannes Gratz, Medical University of Vienna, Austria; Benjamin Gravesteijn, Erasmus Medical Center-University Medical Center, Rotterdam, The Netherlands; Francesca Grossi, Maggiore Della Carità Hospital, Novara, Italy; Russell L. Gruen, Medical University of Vienna, Austria; Deepak Gupta, All India Institute of Medical Sciences, New Delhi, India; Juanita A. Haagsma, Erasmus Medical Center-University Medical Center, Rotterdam, The Netherlands; Iain Haitsma, Erasmus MC, Rotterdam, The Netherlands; Raimund Helbok, Medical University of Innsbruck, Innsbruck, Austria; Eirik Helseth, Oslo University Hospital, Oslo, Norway; Lindsay Horton, University of Stirling, Stirling, UK; Jilske Huijben, Erasmus Medical Center-University Medical Center, Rotterdam, The Netherlands; Peter J. Hutchinson, Addenbrooke's Hospital and University of Cambridge, Cambridge, UK; Bram Jacobs, University of Groningen, University Medical Center Groningen, Groningen, The Netherlands; Stefan Jankowski, Sheffield Teaching Hospitals NHS Foundation Trust, Sheffield, UK; Mike Jarrett, Quesgen Systems Inc., Burlingame, California, USA; Ji-yao Jiang, Shanghai Renji Hospital, Shanghai Jiaotong University/School of Medicine, Shanghai, China; Faye Johnson, Salford Royal Hospital NHS Foundation Trust, Salford, UK; Kelly Jones, Auckland University of Technology, Auckland, New Zealand; Mladen Karan, University of Novi Sad, Novi Sad, Serbia; Angelos G. Kolias, Addenbrooke's Hospital and University of Cambridge, Cambridge, UK; Erwin Kompanje, Erasmus Medical Center, Rotterdam, The Netherlands; Daniel Kondziella, Region Hovedstaden Rigshospitalet, Copenhagen, Denmark; Evgenios Koraropoulos, University of Cambridge, Addenbrooke's Hospital, Cambridge, UK; Lars-Owe Koskinen, Umeå University, Umeå, Sweden; Noémi Kovács, University of Pécs, Pécs, Hungary; Ana Kowark, University Hospital of Aachen, Aachen, Germany; Alfonso Lagares, Hospital Universitario 12 de Octubre, Madrid, Spain; Linda Lanyon, Karolinska Institutet, Stockholm, Sweden; Steven Laureys, University of Liège, Liège, Belgium; Fiona Lecky, University of Sheffield, Sheffield, UK, and Salford Royal Hospital, Salford UK; Didier Ledoux, University of Liège, Liège, Belgium; Rolf Lefering, Witten/Herdecke University, Cologne, Germany; Valerie Legrand, ICON, Paris, France; Aurelie Lejeune, Lille University Hospital, Lille, France; Leon Levi, Rambam Medical Center, Haifa, Israel; Roger Lightfoot, University Hospitals Southhampton NHS Trust, Southhampton, UK; Hester Lingsma, Erasmus Medical Center-University Medical Center, Rotterdam, The Netherlands; Andrew I.R. Maas, Antwerp University Hospital and University of Antwerp, Edegem, Belgium; Marc Maegele, Cologne-Merheim Medical Center (CMMC), Witten/Herdecke University, Cologne, Germany; Marek Majdan, Trnava University, Trnava, Slovakia; Alex Manara, Southmead Hospital, Bristol, Bristol, UK; Geoffrey Manley, University of California, San Francisco, California, USA; Costanza Martino, M. Bufalini Hospital, Cesena, Italy; Hugues Maréchal, CHR Citadelle, Liège, Belgium; Julia Mattern, University Hospital Heidelberg, Heidelberg, Germany; Catherine McMahon, The Walton Centre NHS Foundation Trust, Liverpool, UK; Béla Melegh, University of Pécs, Pécs, Hungary; David Menon, University of Cambridge, Addenbrooke's Hospital, Cambridge, UK; Tomas Menovsky, Antwerp University Hospital and University of Antwerp, Edegem, Belgium; Ana Mikolic, Erasmus Medical Center-University Medical Center, Rotterdam, The Netherlands; Benoit Misset, University of Liège, Liège, Belgium; Visakh Muraleedharan, Karolinska Institutet, Stockholm, Sweden; Lynnette Murray, Monash University, Melbourne, Victoria, Australia; Ancuta Negru, Emergency County Hospital Timisoara, Timisoara, Romania; David Nelson, Karolinska Institutet, Stockholm, Sweden; Virginia Newcombe, University of Cambridge, Addenbrooke's Hospital, Cambridge, UK; Daan Nieboer, Erasmus Medical Center-University Medical Center, Rotterdam, The Netherlands; József Nyirádi, University of Pécs, Pécs, Hungary; Otesile Olubukola, University of Sheffield, Sheffield, UK; Matej Oresic, Örebro University, Örebro, Sweden; Fabrizio Ortolano, Fondazione IRCCS Cà Granda Ospedale Maggiore Policlinico, Milan, Italy; Aarno Palotie, University of Helsinki, Helsinki, Finland, Massachusetts General Hospital, Boston, MA, USA, and The Broad Institute of MIT and Harvard, Cambridge, MA, USA; Paul M. Parizel, University Hospital of Grenoble, Grenoble, France; Jean-François Payen, University Hospital of Grenoble, Grenoble, France; Natascha Perera, ARTTIC, Munchen, Germany; Vincent Perlbarg, Assistance Publique – Hopitaux de Paris, Paris, France; Paolo Persona, Azienda Ospedaliera Università di Padova, Padova, Italy; Wilco Peul, Leiden University Medical Center, Leiden, The Netherlands and Medical Center Haaglanden, The Hague, The Netherlands. Anna Piippo-Karjalainen, Helsinki University Central Hospital; Matti Pirinen, University of Helsinki, Helsinki, Finland; Horia Ples, Emergency County Hospital Timisoara, Timisoara, Romania; Suzanne Polinder, Erasmus Medical Center-University Medical Center, Rotterdam, The Netherlands; Inigo Pomposo, Hospital of Cruces, Bilbao, Spain; Jussi P. Posti, Turku University Hospital and University of Turku, Turku, Finland; Louis Puybasset, Pitié -Salpêtrière Teaching Hospital, Assistance Publique, Hôpitaux de Paris and University Pierre et Marie Curie, Paris, France; Andreea Radoi, Vall d'Hebron Research Institute, Barcelona, Spain; Arminas Ragauskas, Kaunas University of Technology and Vilnius University, Vilnius, Lithuania; Rahul Raj, Helsinki University Central Hospital; Malinka Rambadagalla, Rezekne Hospital, Latvia; Jonathan Rhodes, NHS Lothian and University of Edinburg, Edinburgh, UK; Sylvia Richardson, Cambridge Institute of Public Health, Cambridge, UK; Sophie Richter, University of Cambridge, Addenbrooke's Hospital, Cambridge, UK; Samuli Ripatti, University of Helsinki, Helsinki, Finland; Saulius Rocka, Kaunas University of Technology and Vilnius University, Vilnius, Lithuania; Cecilie Roe, Oslo University Hospital/University of Oslo, Oslo, Norway; Olav Roise, Oslo University Hospital, Oslo, Norway; Jonathan Rosand, The Broad Institute, Cambridge MA Harvard Medical School and Massachusetts General Hospital, Boston MA, USA; Jeffrey V. Rosenfeld, The Alfred Hospital, Monash University, Melbourne, Victoria, Australia; Christina Rosenlund, Odense University Hospital, Odense, Denmark; Guy Rosenthal, Hadassah-Hebrew University Medical Center, Jerusalem, Israel; Rolf Rossaint, University Hospital of Aachen, Aachen, Germany; Sandra Rossi, Azienda Ospedaliera Università di Padova, Padova, Italy; Daniel Rueckert, Imperial College London, London, UK; Martin Rusnák, International Neurotrauma Research Organisation, Vienna, Austria; Juan Sahuquillo, Vall d'Hebron Research Institute, Barcelona, Spain; Oliver Sakowitz, University Hospital Heidelberg, Heidelberg, Germany and Klinik für Neurochirurgie, Klinikum Ludwigsburg, Ludwigsburg, Germany; Renan Sanchez-Porras, Klinik für Neurochirurgie, Klinikum Ludwigsburg, Ludwigsburg, Germany; Janos Sandor, University of Debrecen, Debrecen, Hungary; Nadine Schäfer, Witten/Herdecke University, Cologne, Germany; Silke Schmidt, University Greifswald, Greifswald, Germany; Herbert Schoechl, AUVA Trauma Hospital, Salzburg, Austria; Guus Schoonman, Elisabeth-Twee Steden Ziekenhuis, Tilburg, The Netherlands; Rico Frederik Schou, Odense University Hospital, Odense, Denmark; Elisabeth Schwendenwein, Medical University Vienna, Vienna, Austria; Charlie Sewalt, Erasmus Medical Center-University Medical Center, Rotterdam, The Netherlands; Toril Skandsen, Norwegian University of Science and Technology, NTNU and St. Olavs Hospital, Trondheim University Hospital, Trondheim, Norway; Peter Smielewski, University of Cambridge, Addenbrooke's Hospital, Cambridge, UK; Abayomi Sorinola, University of Pécs, Pécs, Hungary; Emmanuel Stamatakis, University of Cambridge, Addenbrooke's Hospital, Cambridge, UK; Simon Stanworth, Oxford University Hospitals NHS Trust, Oxford, UK; Robert Stevens, Johns Hopkins University School of Medicine, Baltimore, Maryland, USA; William Stewart, Queen Elizabeth University Hospital and University of Glasgow, Glasgow, UK; Ewout W. Steyerberg, Erasmus Medical Center-University Medical Center, Rotterdam, The Netherlands and Leiden University Medical Center, Leiden, The Netherlands; Nino Stocchetti, Milan University, and Fondazione IRCCS Cà Granda Ospedale Maggiore Policlinico, Milano, Italy; Nina Sundström, Umeå University, Umeå, Sweden; Anneliese Synnot, Monash University, Melbourne, Australia and La Trobe University, Melbourne, Australia; Riikka Takala, Turku University Hospital and University of Turku, Turku, Finland; Viktória Tamás, University of Pécs, Pécs, Hungary; Tomas Tamosuitis, Kaunas University of Health Sciences, Kaunas, Lithuania; Mark Steven Taylor, Trnava University, Trnava, Slovakia; Braden Te Ao, Auckland University of Technology, Auckland, New Zealand; Olli Tenovuo, Turku University Hospital and University of Turku, Turku, Finland; Alice Theadom, Auckland University of Technology, Auckland, New Zealand; Matt Thomas, Southmead Hospital, Bristol, Bristol, UK; Dick Tibboel, Erasmus Medical Center, Sophia Children's Hospital, Rotterdam, The Netherlands; Marjolein Timmers, Erasmus Medical Center, Rotterdam, The Netherlands; Christos Tolias, Kings College London, London, UK; Tony Trapani, Monash University, Melbourne, Victoria, Australia; Cristina Maria Tudora, Emergency County Hospital Timisoara , Timisoara, Romania; Peter Vajkoczy, Charité – Universitätsmedizin Berlin, Berlin, Germany; Shirley Vallance, Monash University, Melbourne, Victoria, Australia; Egils Valeinis, Pauls Stradins Clinical University Hospital, Riga, Latvia; Zoltán Vámos, University of Pécs, Pécs, Hungary; Mathieu van der Jagt, Erasmus MC – University Medical Center Rotterdam, Rotterdam, The Netherlands; Gregory Van der Steen, Antwerp University Hospital and University of Antwerp, Edegem, Belgium; Joukje van der Naalt, University of Groningen, University Medical Center Groningen, Groningen, The Netherlands; Jeroen T.J.M. van Dijck, Leiden University Medical Center, Leiden, The Netherlands and Medical Center Haaglanden, The Hague, The Netherlands; Thomas A. van Essen, Leiden University Medical Center, Leiden, The Netherlands and Medical Center Haaglanden, The Hague, The Netherlands; Wim Van Hecke, icoMetrix NV, Leuven, Belgium; Caroline van Heugten, Oxford Brookes University, Oxford, UK; Dominique Van Praag, Antwerp University Hospital, Edegem, Belgium; Thijs Vande Vyvere, icoMetrix NV, Leuven, Belgium; Roel P.J. van Wijk, Leiden University Medical Center, Leiden, The Netherlands and Medical Center Haaglanden, The Hague, The Netherlands; Alessia Vargiolu, ASST di Monza, Monza, Italy; Emmanuel Vega, Lille University Hospital, Lille, France; Kimberley Velt, Erasmus Medical Center-University Medical Center, Rotterdam, The Netherlands; Jan Verheyden, icoMetrix NV, Leuven, Belgium; Paul M. Vespa, University of California, Los Angeles, Los Angeles, California, USA; Anne Vik, Norwegian University of Science and Technology, NTNU, Trondheim, Norway and St. Olavs Hospital, Trondheim University Hospital, Trondheim, Norway; Rimantas Vilcinis, Kaunas University of Health Sciences, Kaunas, Lithuania; Victor Volovici, Erasmus MC, Rotterdam, The Netherlands; Nicole von Steinbüchel, Universitätsmedizin Göttingen, Göttingen, Germany; Daphne Voormolen, Erasmus Medical Center-University Medical Center, Rotterdam, The Netherlands; Petar Vulekovic, University of Novi Sad, Novi Sad, Serbia; Kevin K.W. Wang, University of Florida, Gainesville, Florida, USA; Eveline Wiegers, Erasmus Medical Center-University Medical Center, Rotterdam, The Netherlands; Guy Williams, University of Cambridge, Addenbrooke's Hospital, Cambridge, UK; Lindsay Wilson, University of Stirling, Stirling, UK; Stefan Winzeck, University of Cambridge, Addenbrooke's Hospital, Cambridge, UK; Stefan Wolf, Charité – Universitätsmedizin Berlin, Berlin, Germany; Zhihui Yang, University of Florida, Gainesville, Florida, USA; Peter Ylén, VTT Technical Research Centre, Tampere, Finland; Alexander Younsi, University Hospital Heidelberg, Heidelberg, Germany; Frederick A. Zeiler, University of Cambridge, Addenbrooke's Hospital, Cambridge, UK and University of Manitoba, Winnipeg, MB, Canada; Veronika Zelinkova, Trnava University, Trnava, Slovakia; Agate Ziverte, Pauls Stradins Clinical University Hospital, Riga, Latvia; and Tommaso Zoerle, Fondazione IRCCS Cà Granda Ospedale Maggiore Policlinico, Milan, Italy.
Funding Information
This study was supported by The Netherlands Organisation for Health Research and Development (ZonMw). The authors A. Mikolic, S. Polinder, A.I.R. Maas, N. von Steinbuechel, M. Zeldovich, E.J.A. Wiegers, and H.F. Lingsma were supported by the European Union 7th Framework Programme (EC grant 602150). Additional support was obtained from the Hannelore Kohl Stiftung (Germany), OneMind (USA), Integra LifeSciences Corporation (USA), and Neurotrauma Sciences (USA).
Author Disclosure Statement
No competing financial interests exist.
Supplementary Material
Supplementary Figure S1
Supplementary Figure S2
Supplementary Figure S3
Supplementary Figure S4
Supplementary Figure S5
Supplementary Figure S6
Supplementary Table S1
Supplementary Table S2
Supplementary Table S3
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
